Clear Sky Science · en
Prediction of Ki-67 expression in invasive breast cancer with dual-modality radiomics
Why this research matters to patients
For women facing a diagnosis of invasive breast cancer, one key question is how fast the tumor is likely to grow and spread. Doctors often rely on a protein called Ki-67 to estimate how quickly cancer cells are dividing, but measuring it usually requires taking tissue with a needle or surgery. This study explores whether information hidden in routine breast imaging—ultrasound and mammography—can be combined and analyzed by computer to predict Ki-67 levels without an extra invasive test, potentially helping tailor treatment with less discomfort and risk.
Seeing more than the eye can detect
Ultrasound and mammography are standard tools for detecting and characterizing breast tumors. Radiologists look at shape, borders, and other visible details, but each image also contains subtle patterns of brightness and texture far too complex for the human eye to fully interpret. Radiomics is a technique that converts these medical images into hundreds of measurable features, turning each tumor into a rich numerical fingerprint. The authors reasoned that these fingerprints might reflect how aggressively a tumor behaves, including whether its Ki-67 level is high or low.
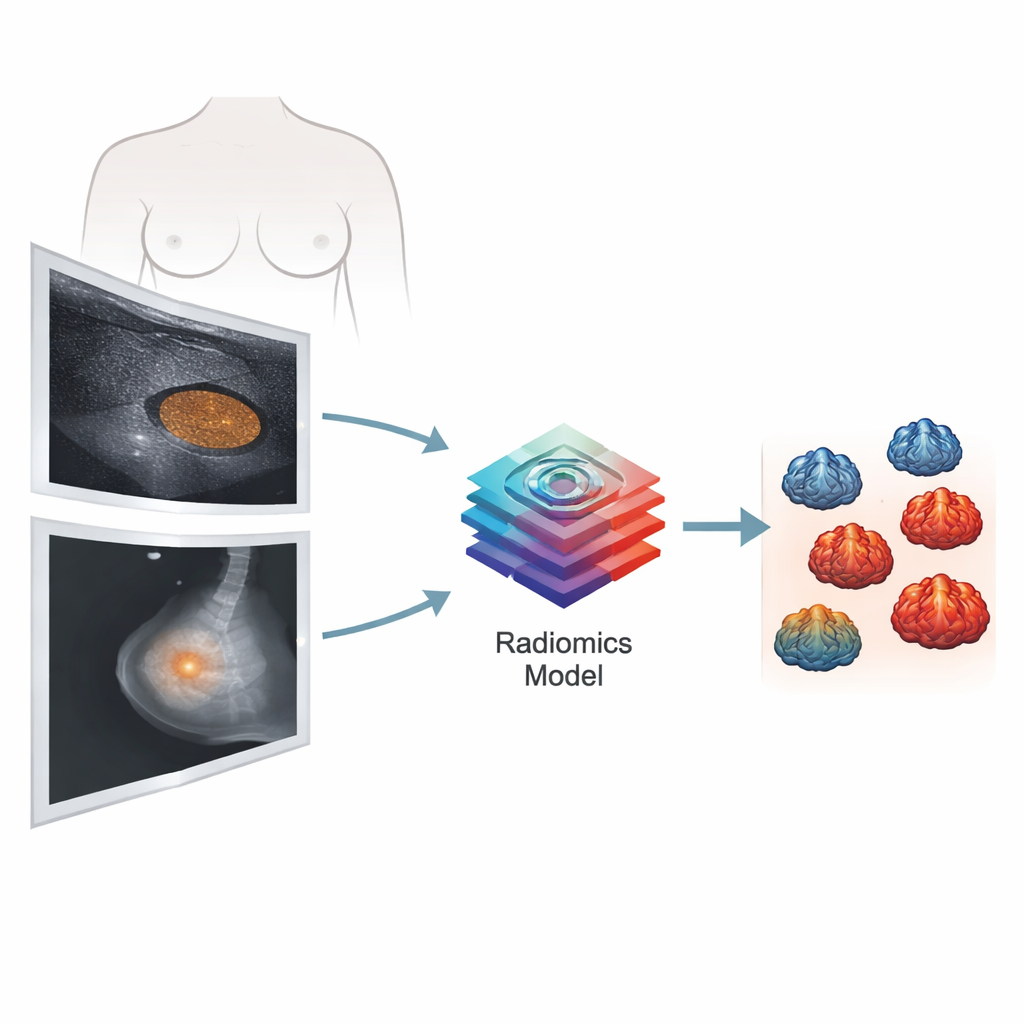
Combining two kinds of imaging
The research team studied 206 women with invasive breast cancer treated at a single hospital. All had clear preoperative ultrasound and mammography images, along with lab-based Ki-67 results. Tumors were grouped as low Ki-67 (20% or less) or high Ki-67 (above 20%), a commonly used cutoff. Specialists traced the outline of each tumor on the images, and computer software extracted over a thousand features from each imaging method. These features described basic brightness, tumor shape, and fine-grained texture patterns, both in the original images and after mathematical transformations designed to highlight hidden structures.
Teaching the computer to predict aggressiveness
Because not all features are equally useful, the researchers used a statistical method to whittle them down to a smaller set that carried the most predictive power. They then trained several types of machine learning models to distinguish high from low Ki-67 tumors, building three versions: one based only on ultrasound, one on mammography alone, and one that combined features from both. They rigorously tested the models using repeated cross-validation, a process that repeatedly reshuffles and splits the data into training and testing groups to check how well the results hold up on new cases.
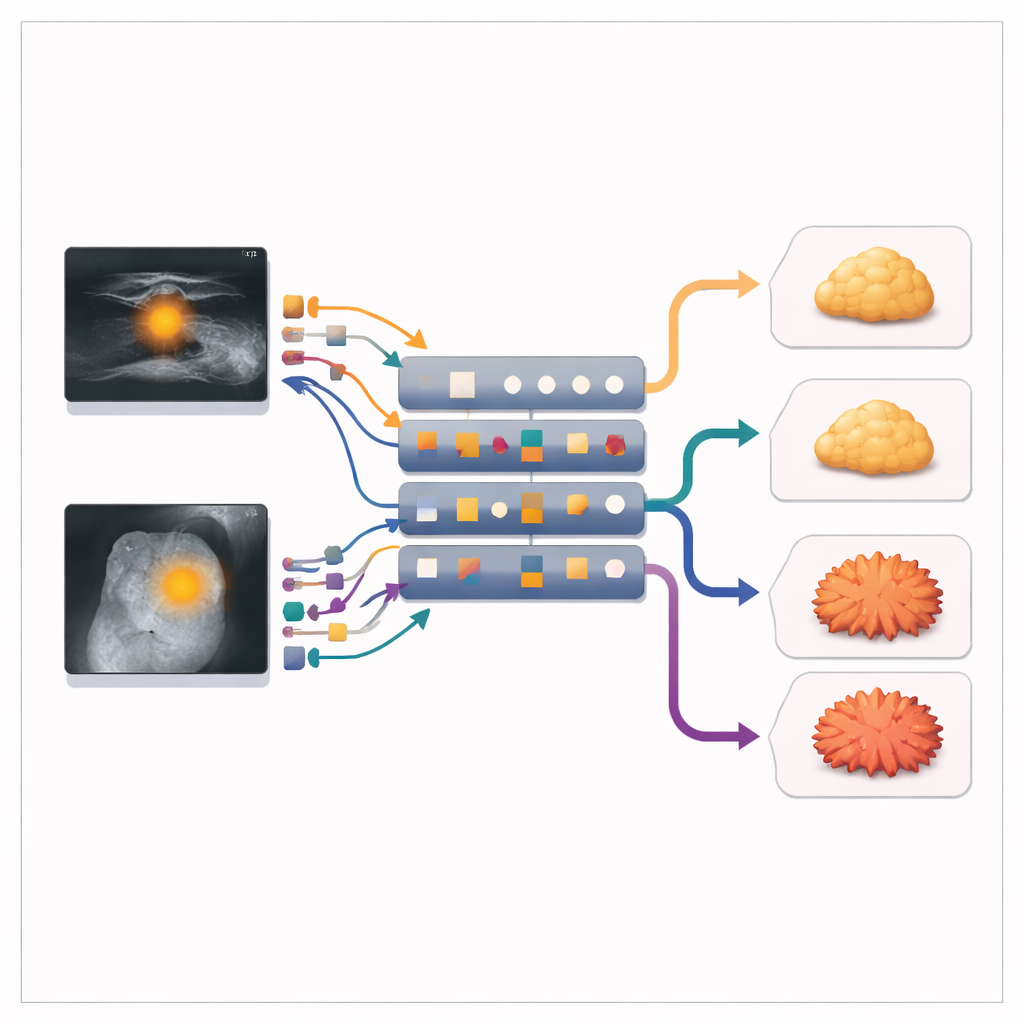
What the models learned from the images
The combined model clearly outperformed models based on a single imaging method. It reached an area under the curve of 0.882, meaning it correctly ranked high versus low Ki-67 tumors in nearly nine out of ten cases, with a good balance between sensitivity (catching aggressive tumors) and specificity (avoiding false alarms). Ultrasound alone and mammography alone were noticeably less accurate. Many of the most important features captured texture—how uniform or varied the gray levels were within the tumor—as well as aspects of tumor shape. Using an interpretation tool called SHAP, the authors showed which features most strongly pushed the model toward a high- or low-risk prediction, making its decisions more transparent.
Potential impact on care and next steps
The study suggests that by combining information from ultrasound and mammography, computers can estimate a tumor’s growth activity in a way that closely matches biopsy-based Ki-67 testing. In practice, such a tool could help doctors decide when to intensify treatment or monitor more closely, especially when a biopsy is hard to obtain or when repeated measurements are needed over time. However, the work was done in a single center and retrospectively, so it still needs to be tested in larger, diverse patient groups and in prospective trials. If confirmed, this dual-modality radiomics approach could become a valuable, non-invasive companion to traditional pathology in guiding personalized breast cancer treatment.
Citation: Xu, R., Lin, Q., Zheng, C. et al. Prediction of Ki-67 expression in invasive breast cancer with dual-modality radiomics. Sci Rep 16, 12129 (2026). https://doi.org/10.1038/s41598-026-42827-y
Keywords: breast cancer, Ki-67, radiomics, ultrasound, mammography