Clear Sky Science · en
AI-guided surgical decision support system for corneal laceration repair: a prospective, non-randomized controlled feasibility study
Why Smarter Eye Surgery Matters
When the clear front window of the eye—the cornea—is cut by an accident, vision can be permanently damaged even after emergency surgery. Tiny stitches must be placed just right to close the wound, smooth the corneal surface, and prevent distorted vision. This study explores whether an artificial intelligence (AI) system can help eye surgeons decide exactly where to place those stitches, with the goal of giving patients sharper, more comfortable sight after serious eye injuries.
Eye Injuries and the Challenge of Repair
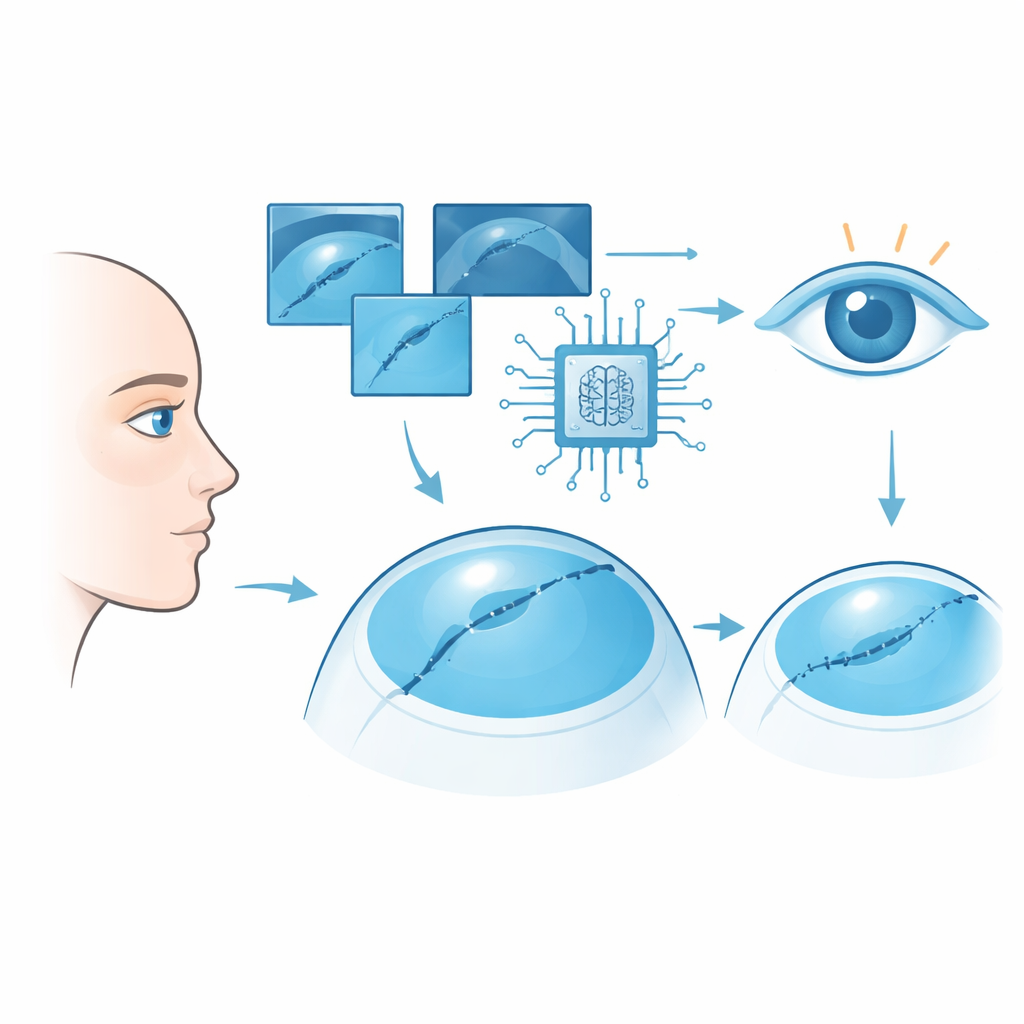
Corneal lacerations are urgent injuries that threaten both the shape of the eye and the ability to see clearly. Surgeons must close the wound quickly, but the cut edges are often irregular and hard to align perfectly. If the stitches are too tight, uneven, or crowded, the cornea can heal with scars and strong astigmatism—a warping of the eye’s surface that bends light unevenly and blurs vision. Outcomes vary widely from one surgeon to another, especially in rushed emergency settings. The authors of this study asked whether a computer system, trained on thousands of images, could offer objective guidance to make stitching more precise and more consistent.
How the AI Learns from Images
The team first built a computer vision system using deep learning, a technique that allows software to “learn” patterns from large image datasets. They trained their model on 2,400 images of pig eyes with corneal cuts, which closely resemble human corneas. The AI learned to outline the wound edges in each photo, essentially tracing the true shape and location of the laceration. Then, using transfer learning, the model was fine-tuned on 300 human corneal injury images that had been carefully outlined by experienced eye doctors. The final system could reliably highlight the wound on a new corneal image and use that outline to calculate how many stitches were needed and exactly where each one should go along the wound.
Turning Image Analysis into Stitch-by-Stitch Advice
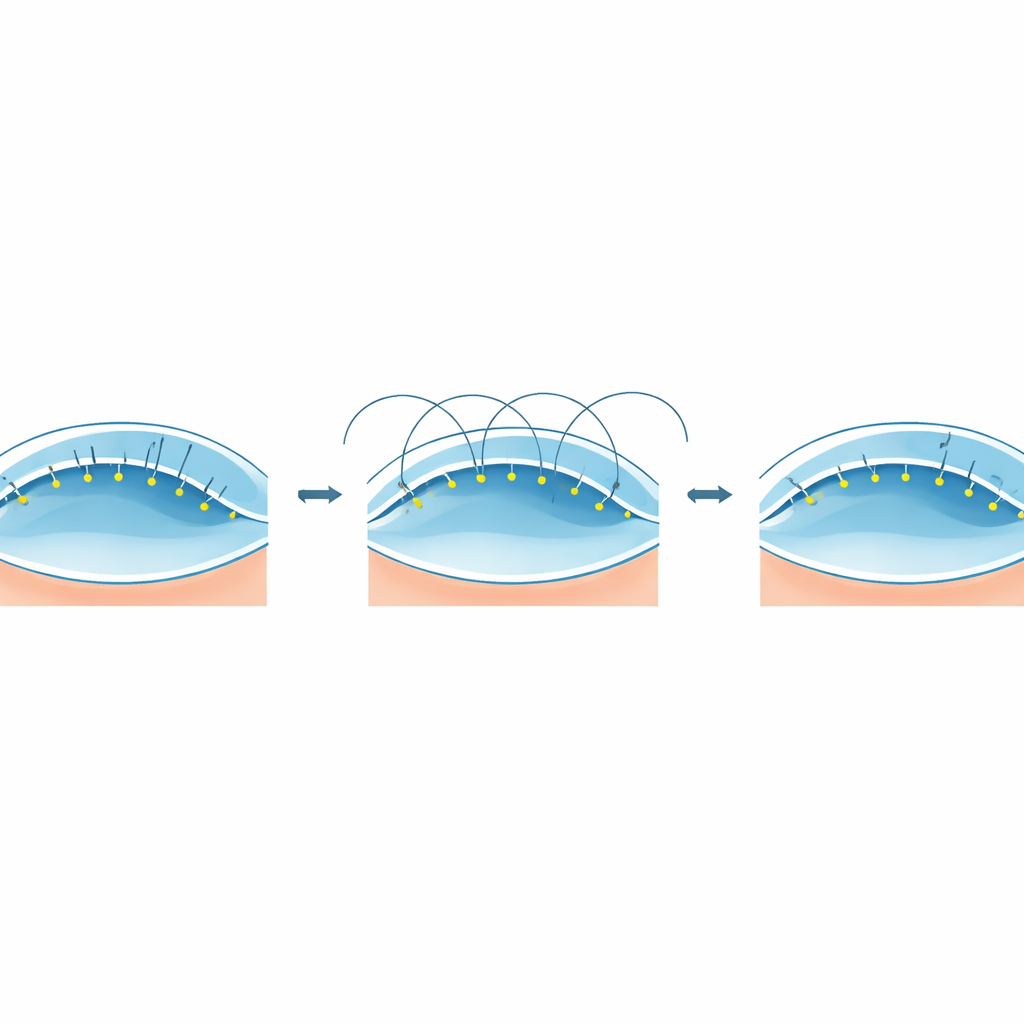
Building on its wound outline, the AI estimated how much healthy tissue surrounded the cut and suggested an appropriate number of sutures and spacing between them. It did this by drawing a center line along the wound, marking reference points at fixed distances, and then projecting short lines outward into the surrounding cornea to choose precise suture entry spots. These computer-chosen points were compared with expert surgeons’ preferred locations and matched within about a tenth of a millimeter, indicating near-human precision. During surgery, doctors in the AI-guided group viewed the system’s suggested stitch pattern and followed roughly 92% of its recommendations while still retaining final control in the operating room.
Testing AI Guidance in Real Patients
To see whether this planning actually helped patients, the researchers conducted a prospective study of 25 people with full-thickness corneal lacerations. Fourteen were treated with standard suturing based solely on the surgeon’s judgment, while eleven had their stitches planned with AI support. All patients were followed for at least six months, and their vision and corneal shape were measured after the stitches were removed. Those whose surgery was guided by AI had better best-corrected visual acuity and less astigmatism than those treated conventionally. Measures of how smooth and symmetric the corneal surface was after healing also favored the AI group, and none of the AI-guided cases needed re-suturing for leaks.
What This Could Mean for Future Eye Care
To a lay reader, the main message is that an AI “co-pilot” in the operating room can help surgeons place stitches more evenly and efficiently after serious eye injuries, leading to clearer vision and fewer complications. This was a small, non-randomized feasibility study, so larger and more rigorous trials are still needed. The system also has limits—it was built for acute, linear trauma cuts and does not yet handle more complex wounds or provide depth information. Even so, the findings suggest that combining a surgeon’s skill with a data-driven stitching plan could make emergency eye repair more precise and more predictable, improving the odds that patients regain useful, comfortable sight after devastating corneal injuries.
Citation: Zheng, J., Lu, H., Chen, Y. et al. AI-guided surgical decision support system for corneal laceration repair: a prospective, non-randomized controlled feasibility study. Sci Rep 16, 12431 (2026). https://doi.org/10.1038/s41598-026-42805-4
Keywords: corneal injury, eye surgery, artificial intelligence, surgical planning, astigmatism