Clear Sky Science · en
Rapid peptide analysis in dried bloodspots to identify novel markers for newborn screening for congenital hypothyroidism
Why This Matters for Newborns
Congenital hypothyroidism is a hormone problem present at birth that, if missed, can quietly damage a baby’s brain and growth. Around the world, including in Thailand, every newborn is screened with a simple heel‑prick blood test. Yet the standard test can sometimes say a healthy baby is sick, or worse, miss a child who truly needs treatment. This study explores a new way to read tiny chemical fingerprints in a dried drop of blood, aiming for faster, more reliable screening that could help protect babies’ brains with greater precision.
The Current Test and Its Blind Spots
Today’s newborn screening for congenital hypothyroidism typically measures a single hormone, thyroid‑stimulating hormone (TSH), in a dried blood spot collected a couple of days after birth. High TSH suggests the baby’s thyroid gland is not making enough hormone. But many real‑world factors disturb this signal: blood taken too early, iodine in disinfectants, the mother’s iodine status, low birth weight, twins, severe illness, or transfusions. These influences can push the TSH level up or down, creating both false alarms and missed cases. Adjusting the cutoff value helps one side of the problem but worsens the other, so researchers are searching for smarter, complementary ways to screen.
Turning a Blood Spot into a Molecular Barcode
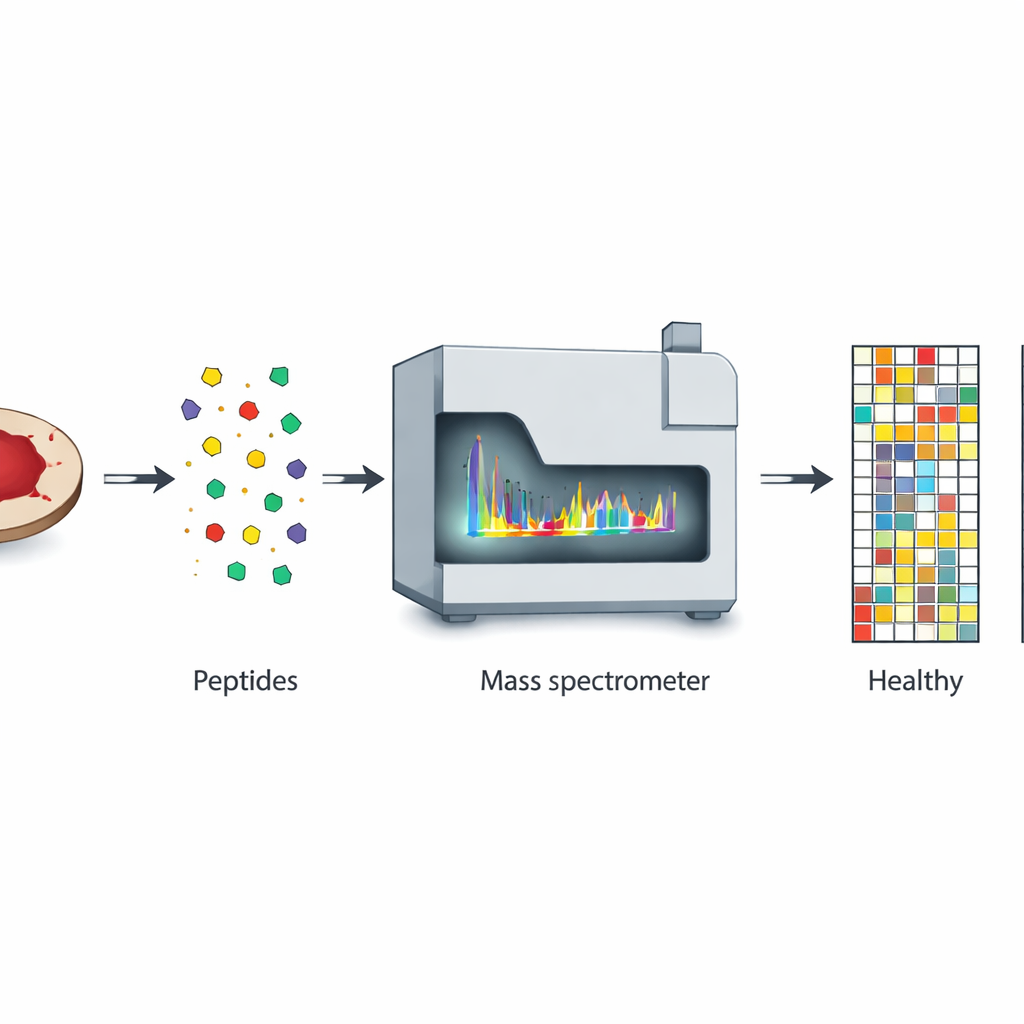
The team behind this study focused on the same dried blood spots already used in national screening programs, but instead of looking only at TSH, they examined many tiny pieces of proteins called peptides. Using a technique known as MALDI‑TOF mass spectrometry, they rapidly scanned 470 leftover samples from Thai newborns: 400 who ultimately proved healthy and 70 confirmed to have congenital hypothyroidism. Each sample produced a complex pattern of peptide signals across a specific mass range, like a barcode unique to the baby’s underlying biology. Sophisticated statistical tools showed that the patterns from affected and unaffected infants separated cleanly, hinting that these barcodes contain a strong disease signature.
Finding Signature Peptides Linked to Disease
From more than 1,400 peptide signals, the researchers narrowed down a subset that best distinguished sick from healthy babies. They combined different types of analysis—looking at how strongly each peptide differed between groups, and how much it contributed to accurate classification. This yielded 15 promising peptide features, including six that appeared exclusively in newborns with congenital hypothyroidism and never in the healthy group. To understand these signals more deeply, the team used a second, more detailed method (LC‑MS/MS) to read peptide sequences and traced them back to their parent proteins. Across this deeper scan they identified over 11,000 peptides and, through layers of comparison and correlation, distilled a final panel of 37 candidates that consistently appeared only in affected infants.
Connecting Peptides to the Body’s Thyroid Circuit
Finding a distinct pattern is only part of the story; it also matters how those molecules fit into the body’s hormone network. The researchers used a database that maps known links between proteins and small chemicals to see how their peptide‑related proteins might interact with key thyroid players such as thyroxine (T4), the active hormone T3, and the TSH receptor. Twelve of the candidate peptides connected, either directly or indirectly, to this hormonal circuit. One protein, UGT2B10, showed direct ties to thyroid hormones, while others were linked through broader signaling and regulatory pathways. These connections suggest that the peptide barcodes are not random; they likely reflect real shifts in how the thyroid system and related processes are working in babies with congenital hypothyroidism.
What This Could Mean for Future Screening
This work does not replace current screening yet, but it offers a powerful proof of concept. By reading detailed peptide barcodes from a single dried drop of blood, laboratories could add a rapid, high‑throughput layer of information on top of the standard hormone test. In practice, that might mean fewer families recalled unnecessarily and fewer affected infants slipping through unnoticed. The authors emphasize that larger, multi‑center studies are still needed before these peptide markers become routine. Still, their approach points toward a future in which newborn screening is not based on a single number, but on a richer molecular fingerprint that supports earlier, more personalized care for babies at risk of lifelong thyroid‑related problems.
Citation: Phoungphosop, J., Arpornsuwan, T., Jaresitthikunchai, J. et al. Rapid peptide analysis in dried bloodspots to identify novel markers for newborn screening for congenital hypothyroidism. Sci Rep 16, 12955 (2026). https://doi.org/10.1038/s41598-026-42578-w
Keywords: newborn screening, congenital hypothyroidism, dried blood spots, peptide biomarkers, mass spectrometry