Clear Sky Science · en
The role of applying radiological modifiers to the Letournel classification and its clinical implications
Why hip socket injuries need a clearer picture
When the ball-and-socket joint of the hip is broken, surgeons must quickly decide how to put it back together so patients can walk again without pain. For decades, doctors have relied on a classic map of hip socket (acetabular) fractures called the Letournel classification. But real-world injuries are often messier than the textbook patterns. This study shows that adding extra CT and X‑ray details—called radiological modifiers—to the traditional system can give surgeons a more complete roadmap, helping them choose safer, more effective operations.
How doctors currently sort hip socket breaks
The hip socket is a deep cup of bone in the pelvis that carries most of the body’s weight. When it breaks, usually in car crashes or falls, the pattern of the fracture strongly influences which operation will work best and how well the joint will function years later. The Letournel classification, introduced in the 1960s, divides acetabular fractures into a set of "elementary" and "associated" types based mainly on the main crack lines. Although this system is widely used and considered the gold standard, many fractures do not fit neatly into its categories, and it often ignores smaller but critical details—such as impacted cartilage, loose fragments, or subtle extensions into nearby structures—that can make surgery more difficult and outcomes worse.
Adding fine print to the fracture map
The authors reviewed CT scans and X‑rays from 236 acetabular fractures treated at their institution over a two‑year period. Two experienced surgeons looked for a predefined list of radiological modifiers—extra features that describe the true nature of the injury beyond the main fracture pattern. These included different types of bone impaction in the weight‑bearing roof and the femoral head, loose fragments inside the joint, preoperative dislocation of the hip, severe fragmentation of the joint surface, involvement of the pelvic ring, damage to the quadrilateral plate (a thin inner wall of the socket), and additional breaks of the posterior wall that are not recognized in the classic scheme. The team then examined how often each modifier appeared, how they related to patient age, and which fracture patterns they tended to accompany.
What the added details revealed
The modifiers turned out to be common and informative. Nearly half of patients had a dislocated hip, around one in five had a highly fragmented joint surface, and one in six had loose pieces of bone floating inside the socket. Several modifiers appeared more often in older patients, including fractures or impaction of the femoral head, roof impaction, and quadrilateral plate involvement—features often associated with weaker, osteopenic bone. Certain fracture types tended to travel with specific modifiers; for example, classic posterior wall fractures were frequently paired with hip dislocation, loose fragments, and severe comminution, while T‑shaped fractures often showed roof and head impaction. Importantly, 22 fractures (about 9%) could not be classified by the Letournel system alone. By tagging quadrilateral plate damage and “hidden” posterior wall fragments as modifiers, 20 of these 22 could be re‑described in a structured way, reducing the unclassified group by about 90%.
Changing the surgeon’s game plan
These extra imaging details were not just academic. They directly influenced surgical choices. Certain modifiers—especially femoral head fractures, roof impaction, and intra‑articular fragments—prompted surgeons to use a demanding but powerful technique called surgical hip dislocation in nearly 9% of cases, giving them 360‑degree access to the joint to restore the damaged surfaces. When the quadrilateral plate was involved, surgeons more often used infrapectineal plating through an approach that better buttresses the inner wall and prevents the femoral head from drifting inward. Every case with pelvic ring involvement required an additional plan to stabilize the ring, and added posterior wall fragments in complex fracture types led surgeons to include a posterior approach. The study also showed that different observers could reliably agree on the presence of nearly all modifiers, meaning they are practical to use in routine care.
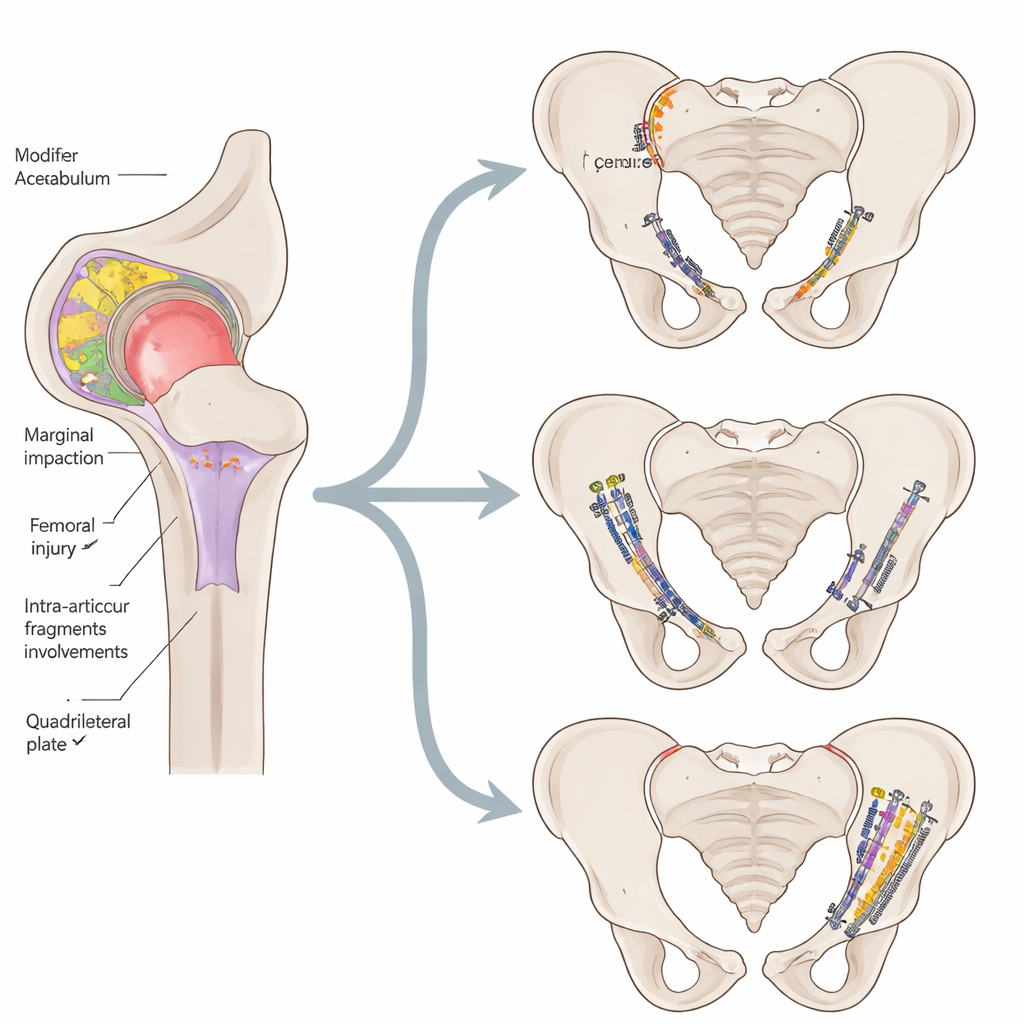
From rigid labels to a full fracture identity
The authors argue that the “identity” of an acetabular fracture should go beyond a single label. By pairing the Letournel type with a checklist of modifiers—summarized in an “Acetabular Fracture Identification Sheet”—surgeons gain a richer description of what is actually broken, where the joint surface is damaged, and which surrounding structures are threatened. This, in turn, can highlight injuries with a poorer prognosis, flag the need for advanced techniques, and make it easier to compare cases across hospitals and studies. While the classic classification remains the backbone, incorporating radiological modifiers makes it more inclusive and clinically useful, bringing the picture of a broken hip socket closer to the complex reality surgeons face in the operating room.
Citation: Abdelnasser, M.K., Thabet, M.A., Ibrahim, B. et al. The role of applying radiological modifiers to the Letournel classification and its clinical implications. Sci Rep 16, 11616 (2026). https://doi.org/10.1038/s41598-026-42515-x
Keywords: acetabular fractures, hip surgery, fracture classification, radiological modifiers, pelvic trauma