Clear Sky Science · en
Vancomycin therapeutic drug monitoring is associated with reduced toxicity in ICU patients: a MIMIC-IV retrospective study
Why this matters for patients in intensive care
When people land in the intensive care unit with life threatening infections, doctors often reach for vancomycin, a powerful antibiotic. But this drug can quietly harm the kidneys, liver, and blood if the dose is not carefully tuned. This study asks a practical question that matters to patients and families alike: does regularly measuring vancomycin levels in the blood help keep critically ill patients safer and more likely to survive?
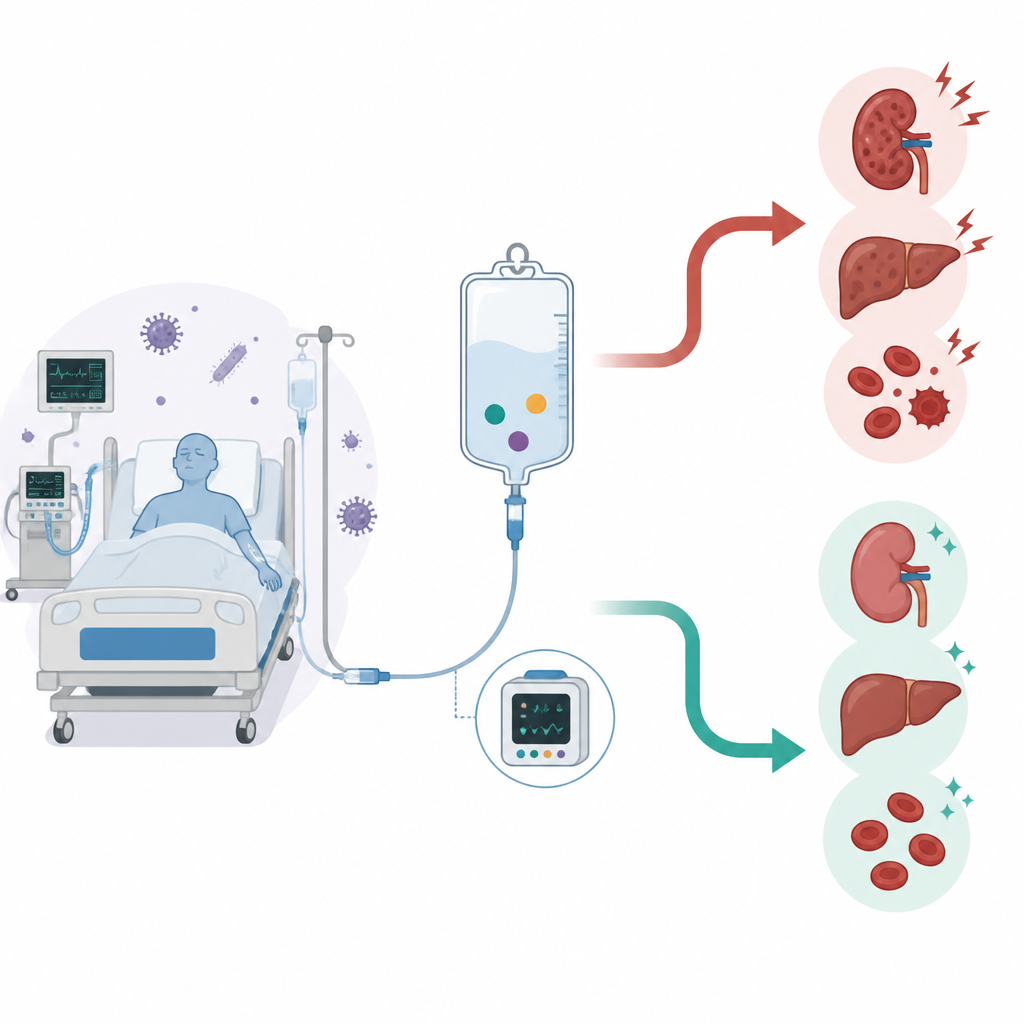
A closer look at a widely used hospital antibiotic
Vancomycin is a mainstay treatment for stubborn bacteria such as methicillin resistant Staphylococcus aureus, often called MRSA. It has saved countless lives over decades of use. At the same time, it has a narrow safety margin, meaning the helpful dose is not far from the harmful one. Too much vancomycin can injure the kidneys, irritate the liver, or disturb blood cell counts. To balance benefit and risk, many guidelines advise therapeutic drug monitoring, where blood samples are used to measure vancomycin levels and adjust dosing. Yet until now, large scale evidence in the sickest patients those in the ICU has been limited and sometimes conflicting.
How the researchers used real world ICU data
The team analyzed records from more than 28,000 adults in the MIMIC IV database, which collects detailed, anonymized information from ICU stays at a major US hospital. All included patients received vancomycin through a vein after arriving in intensive care. About one third had at least one vancomycin level measured, placing them in the monitoring group, while the rest formed the non monitoring group. Because doctors tend to monitor sicker patients more closely, the researchers used advanced statistical methods to make fair comparisons, matching patients with similar ages, illnesses, lab results, and other treatments before looking at outcomes.
What happened to organs and survival
Before adjusting for differences in how sick patients were, those who underwent monitoring appeared to have more kidney, liver, and blood problems. This was expected, because they started off in worse shape. After carefully matching similar patients and adjusting for dozens of health factors, the picture flipped. In the matched groups of nearly 10,000 pairs, patients whose vancomycin levels were monitored had lower rates of acute kidney injury and fewer blood related side effects such as low platelets or anemia. They also had somewhat fewer liver problems. Most importantly, monitored patients were less likely to die during their ICU stay or before leaving the hospital, and survival curves showed their advantage appearing early and persisting over time.
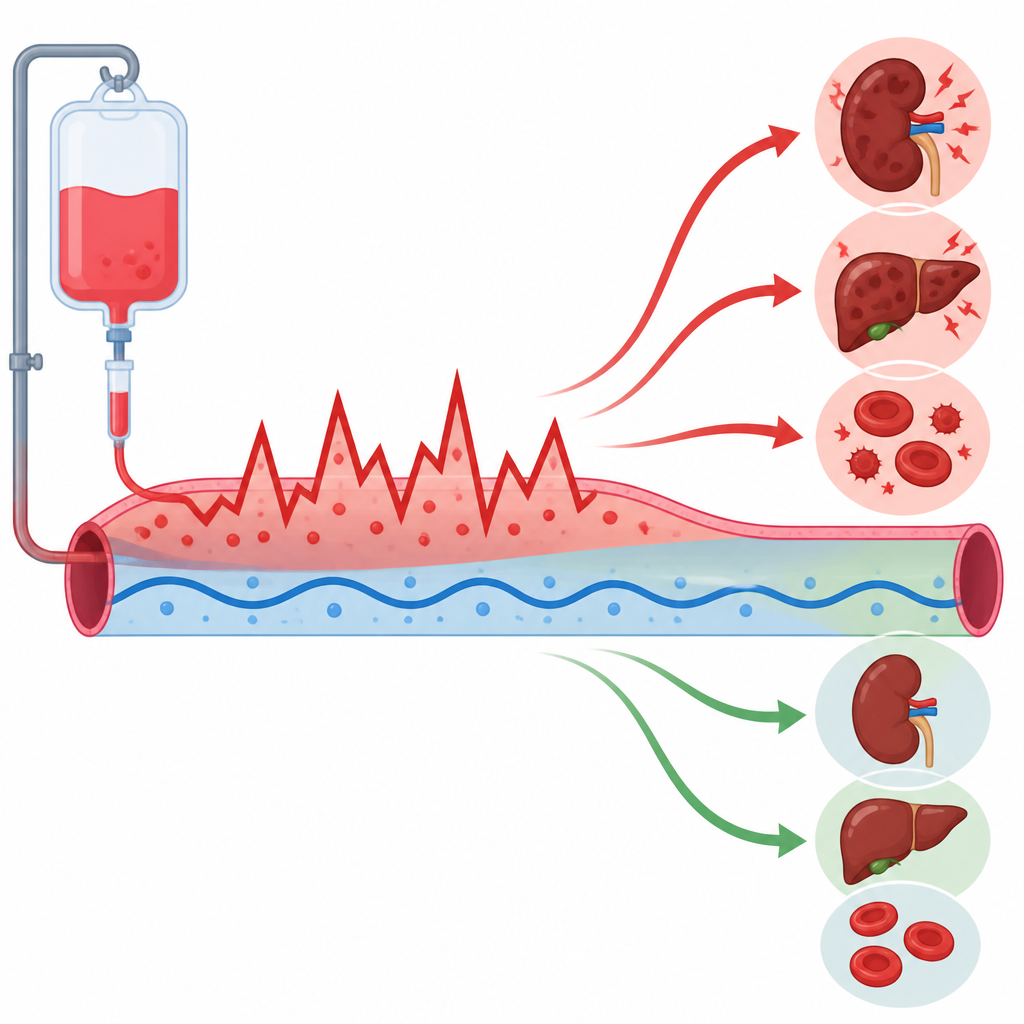
Who was at higher risk from treatment side effects
The study did more than compare monitoring with no monitoring. It also searched for conditions that made organ injury more likely. High blood pressure, type 2 diabetes, cancer, and bleeding in the brain were among the health issues linked to greater risk of kidney or blood toxicity while on vancomycin. Patients taking aspirin or other antibiotics at the same time also faced higher odds of problems in multiple organs. These patterns suggest that some ICU patients are especially fragile and might benefit even more from close tracking and dose adjustment.
What this means for everyday care in the ICU
The findings suggest that checking vancomycin levels during treatment is not just a lab exercise but a safety tool that can reduce organ damage and is associated with better chances of leaving the hospital alive. While this observational study cannot prove cause and effect, its large size, careful matching, and consistent results support the idea that routine vancomycin monitoring should be standard practice in intensive care, especially for patients with kidney strain or other risk factors.
Citation: Wang, J., Huang, C., Chen, Y. et al. Vancomycin therapeutic drug monitoring is associated with reduced toxicity in ICU patients: a MIMIC-IV retrospective study. Sci Rep 16, 15009 (2026). https://doi.org/10.1038/s41598-026-42395-1
Keywords: vancomycin, therapeutic drug monitoring, ICU patients, drug toxicity, acute kidney injury