Clear Sky Science · en
Epimedin C attenuates airway inflammation and remodeling in Asthma by intervening M2 macrophage polarization via modulating the PI3K/Akt/mTOR signaling pathway
Why this study matters for people with asthma
Asthma affects hundreds of millions of people and, even with inhalers, many still live with lingering airway inflammation and long‑term damage to their lungs. This study explores whether Epimedin C, a natural compound from a traditional Chinese medicinal herb, can calm irritated airways and slow structural damage in asthma. By examining both whole animals and individual immune cells, the researchers look for a new way to control asthma that goes beyond standard steroids and bronchodilators.
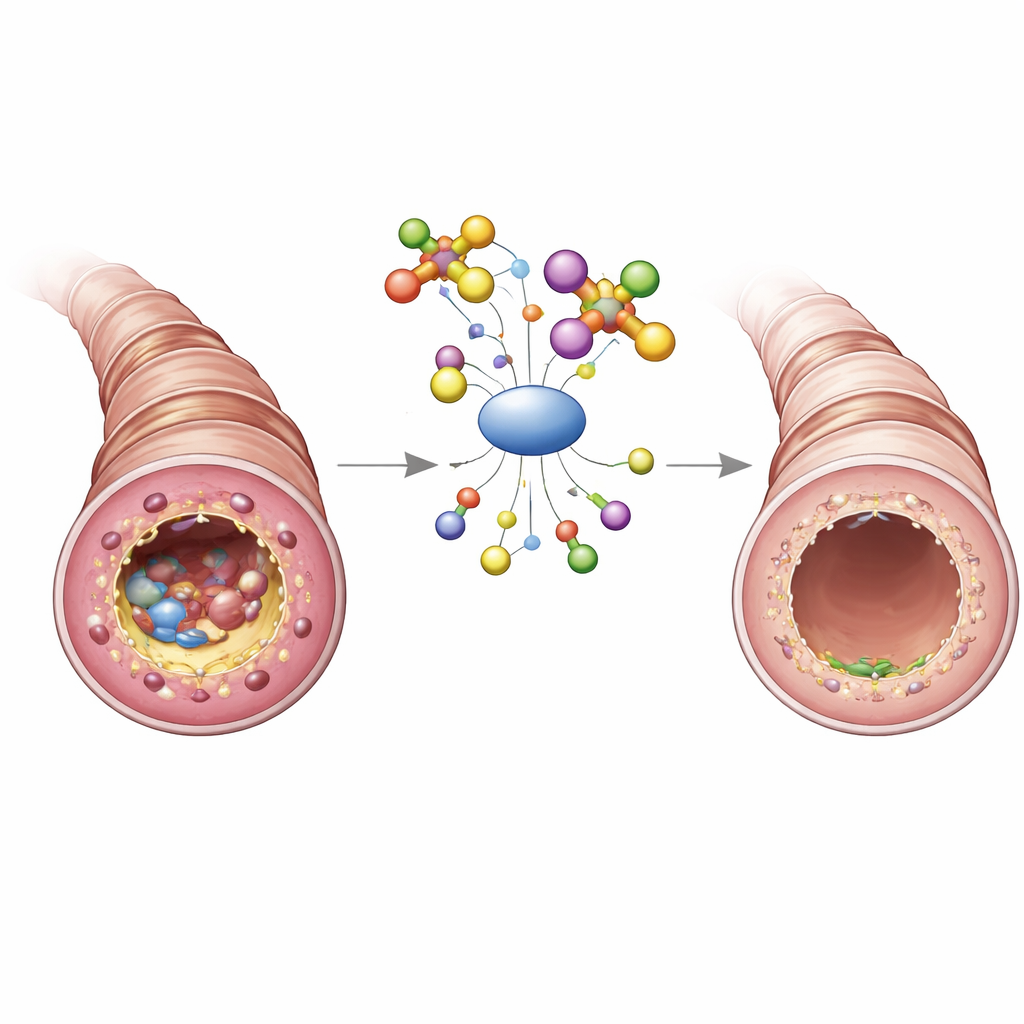
What goes wrong in the asthmatic airway
In asthma, the tubes that carry air in and out of the lungs become chronically inflamed. The airway walls thicken, fill with mucus, and gradually remodel, making it harder to breathe even between attacks. A key player in this process is a type of immune cell called the macrophage, which can adopt different “personalities.” One form, called the M2 type, is usually involved in healing, but in allergic asthma it can be pushed into overdrive. When that happens, M2 cells release substances that attract other immune cells, stimulate mucus production, and promote scarring of the airway wall.
A herbal molecule under the microscope
Epimedin C is a flavonoid—an active plant ingredient—abundantly found in Herba Epimedii, a herb long used in traditional Chinese medicine. Previous work suggested that mixtures containing this herb could ease asthma symptoms, but it was unclear which component was responsible or how it worked. The authors designed a set of experiments in mice with allergy‑induced asthma and in cultured mouse macrophages to test whether purified Epimedin C could improve breathing, reduce airway damage, and dial down the harmful M2 macrophage response.
Testing Epimedin C in an asthma model
First, the team created asthma‑like disease in mice by repeatedly exposing them to egg‑white protein, a standard method for provoking allergic airway inflammation. These mice showed hallmark signs of asthma: they reacted strongly to a bronchial irritant, had swollen, mucus‑filled airways, and displayed protein markers of tissue scarring. When the animals were treated by mouth with Epimedin C, especially at higher doses, their lung function improved and their airways looked more normal under the microscope. Levels of several key inflammatory molecules in lung fluid fell, and markers of structural remodeling in the airway wall declined, with effects comparable in many measures to the steroid drug dexamethasone.
How Epimedin C calms overactive immune cells
To understand how these improvements occur, the researchers focused on a central cell‑signaling route inside macrophages known as the PI3K/Akt/mTOR pathway, which acts like a control panel for cell growth and activation. In asthmatic mice, this pathway was highly switched on in lung tissue, and M2‑type macrophages were abundant. Epimedin C treatment lowered the activity of the pathway and reduced the proportion of M2 cells, tightly linking the two changes. In cell culture, the team pushed macrophages into the M2 state using the cytokine IL‑4. This increased pathway activity and the release of factors that drive inflammation and tissue remodeling. Blocking the pathway with a known chemical inhibitor, or adding Epimedin C, both prevented full M2 conversion and cut the production of these damaging factors. Combining Epimedin C with the inhibitor did not add much extra benefit, suggesting they act on the same control route.
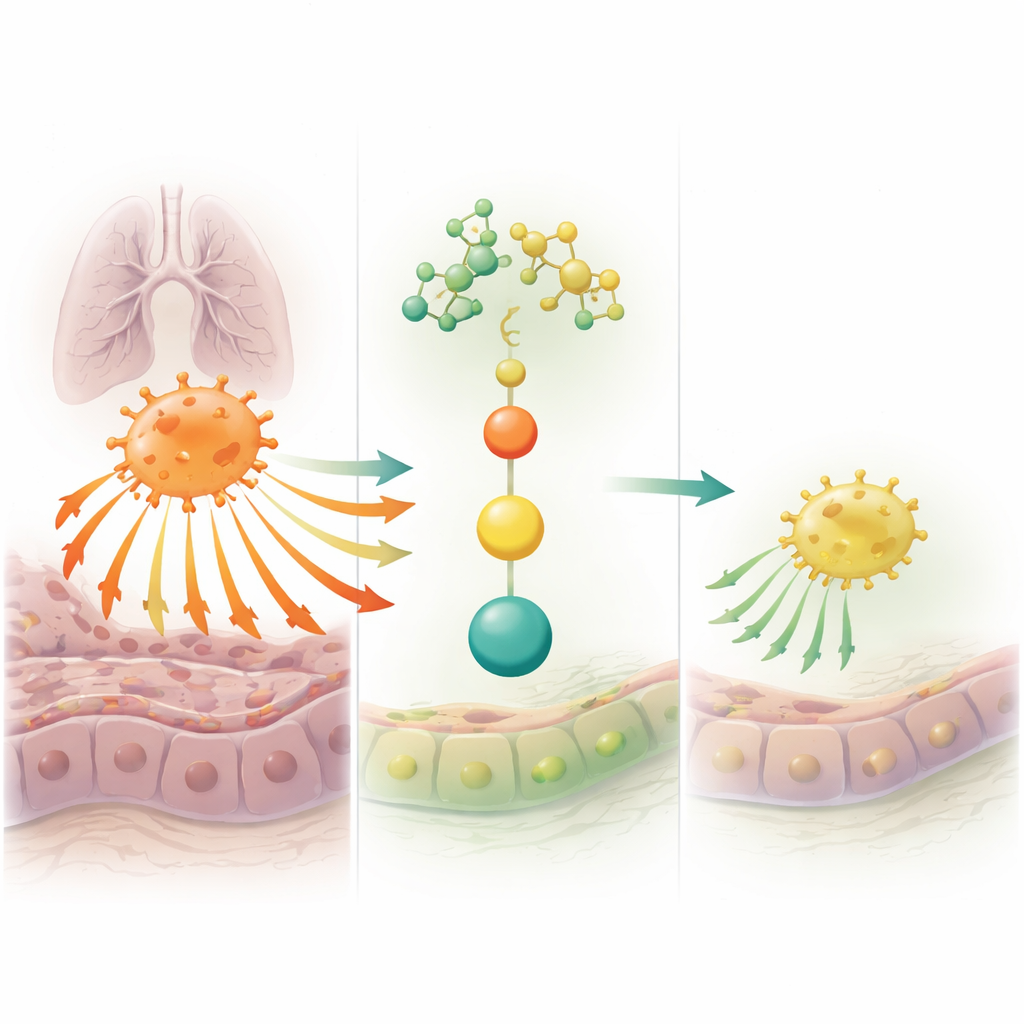
What this could mean for future asthma care
Altogether, the findings suggest that Epimedin C helps protect the lungs in asthma by turning down a key internal switch in macrophages, preventing them from becoming overly pro‑remodeling M2 cells and curbing the signals that thicken and scar the airways. While this work was done in mice and cell models and does not yet prove safety or effectiveness in humans, it offers a clear biological explanation for the compound’s benefits and identifies a specific pathway to target. In the long term, Epimedin C or similar molecules could complement existing inhalers, aiming not only to relieve symptoms but also to slow or prevent the underlying damage that makes asthma a chronic disease.
Citation: Zhang, Z., Cao, S., Qin, Z. et al. Epimedin C attenuates airway inflammation and remodeling in Asthma by intervening M2 macrophage polarization via modulating the PI3K/Akt/mTOR signaling pathway. Sci Rep 16, 13604 (2026). https://doi.org/10.1038/s41598-026-42160-4
Keywords: asthma, airway inflammation, macrophages, traditional Chinese medicine, cell signaling