Clear Sky Science · en
Mesothelioma location influences the tumour microenvironment and immune checkpoint therapy response in preclinical models
Where a Cancer Grows Can Change Its Behavior
Mesothelioma is a rare cancer linked to asbestos exposure that usually forms in the thin linings around the lungs or the abdomen. Doctors now use immune-based drugs called checkpoint therapies for some patients, but it is unclear whether results from tumors in the chest can be applied to those in the belly. This study in mice shows that simply changing where the cancer grows inside the body can alter how it interacts with the immune system and how well it responds to modern immunotherapy.
Different Places, Different Tumors
To explore this, researchers implanted the same mesothelioma cells into three locations in mice: under the skin, inside the chest lining, and inside the abdominal lining. Although the cancer cells were identical, the resulting tumors did not behave the same. Tumors in the chest and abdomen invaded nearby organs, while those under the skin stayed more contained. The team also observed distinct patterns of immune cells gathering around the tumors, hinting that local surroundings strongly shape how the disease develops.
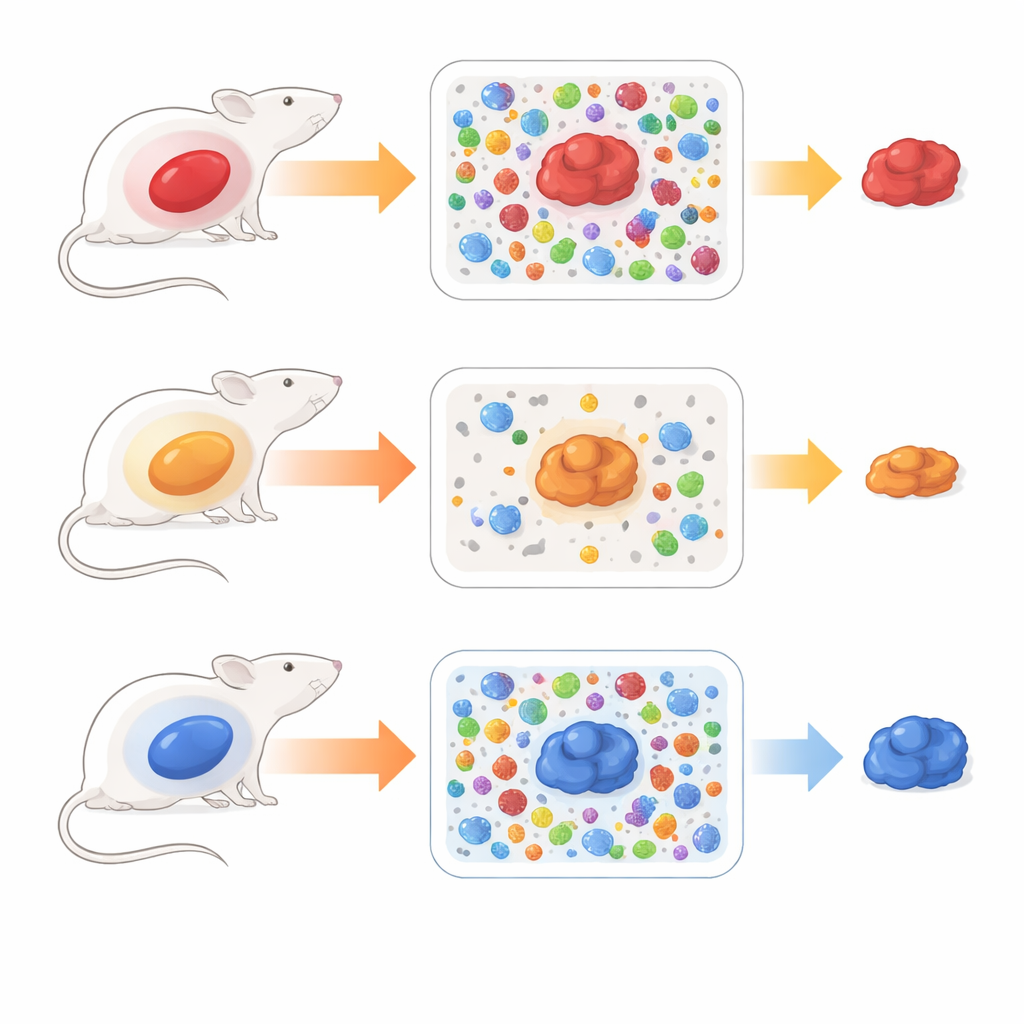
Local Immune Neighborhoods Shape Inflammation
The scientists next looked at gene activity in whole tumors using RNA sequencing, which reveals which biological pathways are switched on. Tumors growing under the skin and in the chest showed strong signs of inflammation, including activation of interferon and other immune-related signals that are usually linked with better responses to immunotherapy. In contrast, abdominal tumors had a much more subdued inflammatory profile, with weaker engagement of these immune pathways and a shift toward cell growth programs. This suggested that the abdominal cavity creates a calmer, more suppressive immune neighborhood around the cancer.
Who Shows Up to the Fight
By combining computational analyses with detailed cell staining, the team mapped which immune cells were present in each setting. Chest tumors were rich in T cells, the key foot soldiers that can directly attack cancer cells, while under-the-skin tumors had more natural killer cells and other inflammatory cells clustered around their edges. Abdominal tumors, however, were dominated by macrophages and B cells and had relatively few T cells and natural killer cells. Even the macrophages appeared less activated, based on their surface markers. These differences indicate that tumors in the abdomen may be surrounded by cells that are less ready, or even less able, to mount an effective anti-cancer attack.
Same Drugs, Different Outcomes
The researchers then asked how these location-dependent immune environments affected treatment with immune checkpoint therapy, which works by releasing natural brakes on T cells. When treated with a combination of two checkpoint-blocking antibodies, most under-the-skin tumors shrank dramatically or disappeared, regardless of how the drugs were delivered. In earlier work, the same approach also worked well in chest tumors. In sharp contrast, abdominal tumors rarely vanished. Some shrank temporarily and survival improved, but complete cures were not seen. These results held even when drugs were injected directly into the abdomen, implying that the local biology of that space, not drug access, limits the benefit.
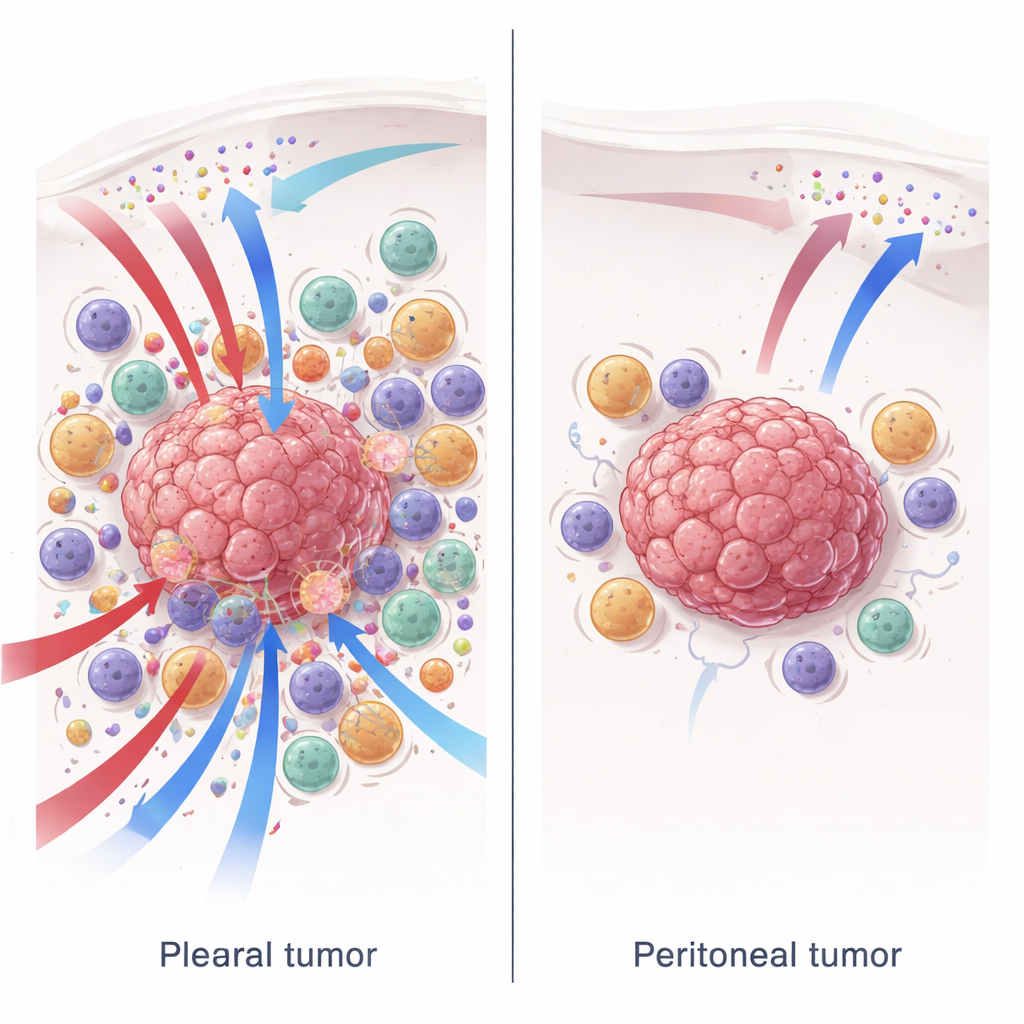
Why This Matters for Patients
Overall, the study shows that the same mesothelioma cells can behave very differently depending on where they grow, because each body compartment provides a distinct immune setting. Tumors in more inflamed environments, such as the chest lining or under the skin, are more likely to respond strongly to current immunotherapies. Tumors in the abdominal lining instead sit in a cooler, more suppressive neighborhood that blunts these treatments. For patients, this means results from clinical trials in pleural (chest) mesothelioma may not automatically apply to peritoneal (abdominal) mesothelioma. Future therapies for abdominal disease may need to first reprogram local immune cells—especially macrophages and B cells—to turn a quiet neighborhood into one where checkpoint drugs can work much more effectively.
Citation: Orozco Morales, M.L., Lansley, S.M., Chin, W.L. et al. Mesothelioma location influences the tumour microenvironment and immune checkpoint therapy response in preclinical models. Sci Rep 16, 10473 (2026). https://doi.org/10.1038/s41598-026-41431-4
Keywords: mesothelioma, tumor microenvironment, immunotherapy, immune checkpoint blockade, peritoneal cancer