Clear Sky Science · en
Histopathologic responses of the dental pulp to an experimental calcium aluminate–calcium silicate based capping material in comparison to mineral trioxide aggregate
Saving Teeth by Helping Them Heal Themselves
Modern dentistry is moving away from drilling and root canals toward gentler treatments that let teeth repair themselves. When the soft center of a tooth (the pulp) is accidentally exposed during decay removal or injury, dentists can sometimes protect it with a small “cap” instead of removing it. This study tested a new tooth-colored material, based on calcium-rich ceramics, to see whether it can protect and heal the pulp as well as a widely used product called mineral trioxide aggregate (MTA). The work, carried out in dogs whose teeth respond much like ours, asks a simple but important question: can this new material keep teeth alive and help them rebuild their own protective barrier?
Why the Soft Core of the Tooth Matters
Inside every tooth lies a living core of nerves, blood vessels, and repair cells. If this pulp is exposed, bacteria and irritation can lead to pain, infection, and eventually tooth loss. A procedure called direct pulp capping aims to avoid that outcome. The dentist gently covers the exposed spot with a protective material, then seals the tooth with a filling. The ideal cap soothes irritation, blocks germs, and encourages the tooth to grow a new layer of hard tissue—called a dentin bridge—over the wound. For years, MTA has been a leading option because it generally causes mild irritation and reliably triggers hard-tissue repair, but it is expensive, slow to set, and not easy to handle.
A New Candidate for Gentle Tooth Repair
The researchers developed an experimental material made from calcium aluminate and calcium silicate, with added calcium carbonate and mixed with a polyacrylic acid liquid. These ingredients were chosen because they set faster and more strongly than MTA and release calcium in a way that can stimulate hard-tissue formation. In the study, four healthy dogs provided 112 teeth, which were divided into four groups: teeth capped with the new material, teeth capped with MTA, exposed teeth restored without any capping material (a “worst case” positive control), and untouched, healthy teeth (a negative control). Small standardized cavities were created to expose the pulp, the different treatments were applied, and the teeth were then examined under the microscope after one month and again after three months.
What Happened Inside the Teeth
The team focused on two key signs of success: how much inflammation developed in the pulp and how well a dentin bridge formed over the exposure site. After one month, the new material caused more noticeable inflammation than MTA, and some samples showed disruption of the orderly cell layer lining the pulp. MTA-treated teeth mostly showed only enlarged blood vessels, a milder change. However, even at this early stage, both capping materials already showed signs of new mineral deposits at the wound, while the exposed teeth without any capping material developed severe inflammation and tissue death. The untouched teeth remained completely healthy.
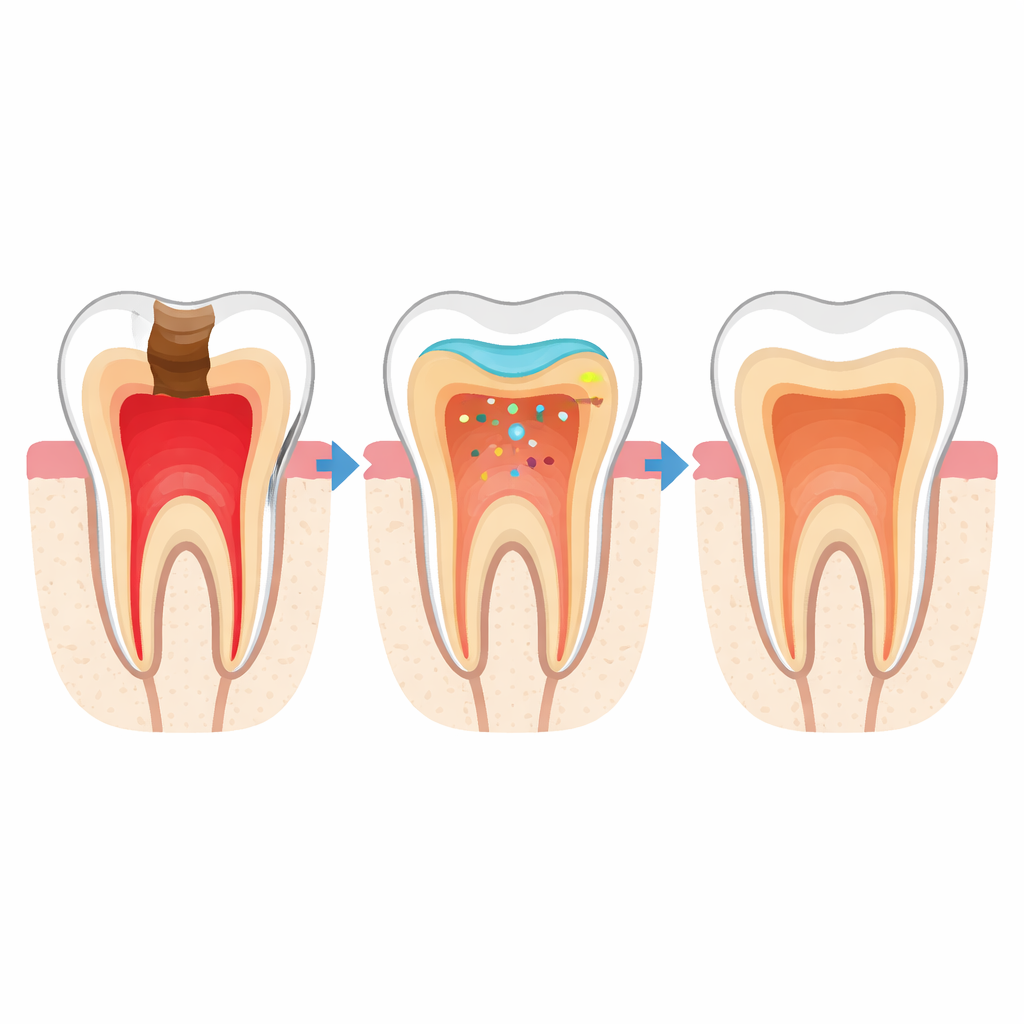
Healing Strengthens Over Time
By three months, the picture had changed. In both the new-material and the MTA groups, inflammation had dropped sharply, and the pulp tissue looked calm and organized. Under the microscope, the MTA-capped teeth displayed a thick, continuous dentin bridge sealing the exposure site. The teeth capped with the experimental material also showed clear bridge formation, although the new layer was generally somewhat thinner or less uniform. Statistically, there was no meaningful difference between MTA and the experimental material in either inflammation scores or in how often a partial or complete dentin bridge was present. In contrast, the exposed teeth without any capping still showed severe inflammation and no repair, highlighting the importance of using a suitable protective material.
What This Means for Future Dental Care
To a non-specialist, the main message is that this new calcium-based capping material helped teeth heal themselves almost as well as the current standard, MTA. Although it caused stronger irritation at first, the pulp settled down over time, and a hard, protective bridge formed in most treated teeth. Because the material is designed to be strong, less costly, and easier to work with, it could eventually give dentists another reliable option for saving teeth that might otherwise need root canal treatment. The authors emphasize that further, longer-term studies—especially in teeth with existing decay and inflammation—are needed before the material reaches everyday practice, but their results suggest it is a promising tool for more conservative, tooth-preserving dentistry.
Citation: Saleh, R.S., Elbattawy, E.A., Hamza, S. et al. Histopathologic responses of the dental pulp to an experimental calcium aluminate–calcium silicate based capping material in comparison to mineral trioxide aggregate. Sci Rep 16, 9670 (2026). https://doi.org/10.1038/s41598-026-41284-x
Keywords: vital pulp therapy, pulp capping materials, dentin bridge formation, calcium aluminate cement, mineral trioxide aggregate