Clear Sky Science · en
A multimodal feature fusion with deep representation learning approach for polycystic ovary syndrome diagnosis using ultrasound images
Why this matters for women’s health
Polycystic ovary syndrome (PCOS) is one of the leading causes of infertility and hormonal problems in women of reproductive age, yet it is often hard to diagnose early. Today, specialists still inspect ultrasound scans of the ovaries by eye, counting tiny fluid‑filled sacs and judging their size and shape. This is time‑consuming, depends heavily on expert skill, and can miss early signs. The paper summarized here presents a new computer‑based method that reads ultrasound images automatically, aiming to spot PCOS more accurately and more quickly, which could help more women receive timely treatment and avoid long diagnostic odysseys.
A closer look at PCOS and current tests
PCOS affects roughly one in ten women before menopause. It is linked to elevated levels of male‑type hormones, irregular periods, and multiple small cysts in the ovaries. These changes can disrupt ovulation, making it harder to become pregnant, and are associated with weight gain, diabetes risk, and emotional distress. At present, doctors combine hormone blood tests, menstrual history, and ultrasound imaging to decide whether someone has PCOS. But no single test is definitive, and interpreting the swirl of bright and dark spots on an ultrasound image is a demanding visual task, especially for less‑experienced clinicians. As a result, diagnosis can be slow, inconsistent, and sometimes inaccurate.
Turning ultrasound scans into clearer signals
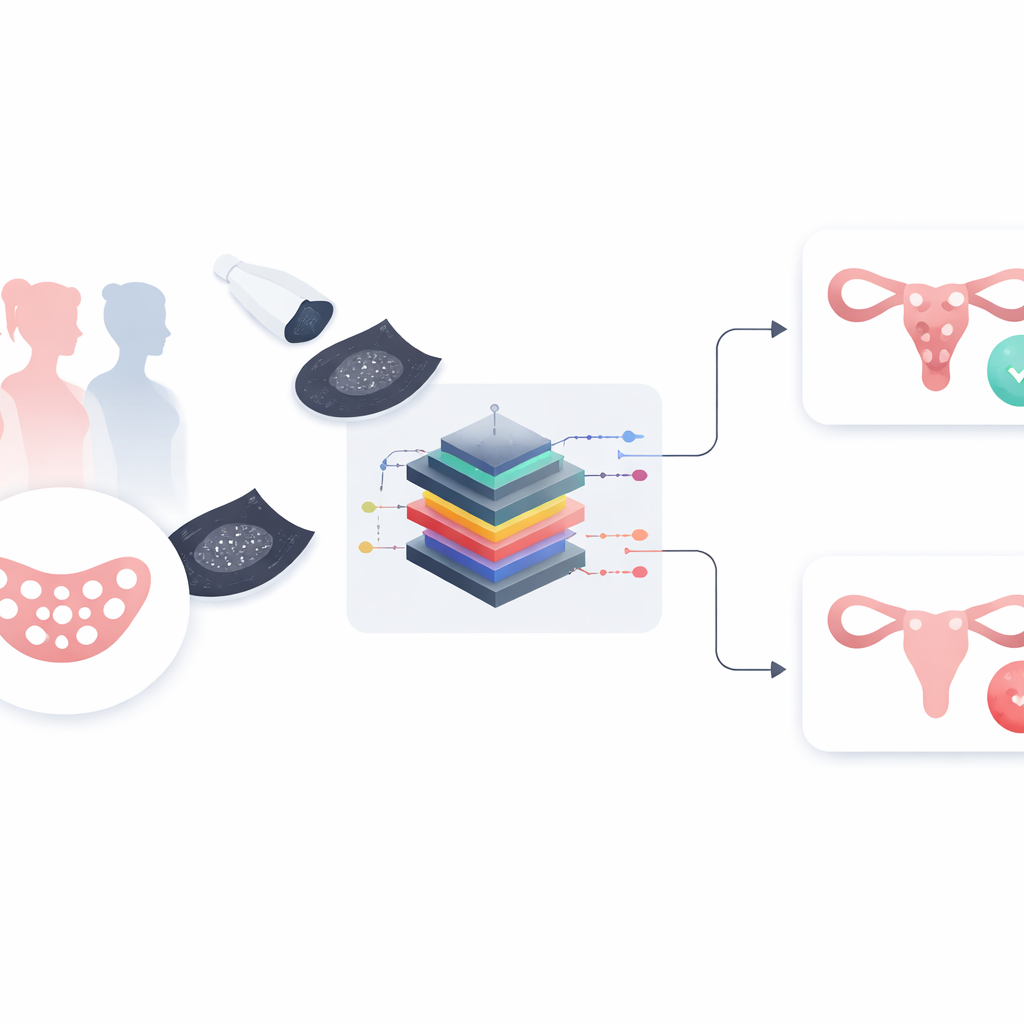
The researchers set out to build a smart image‑analysis system that could examine ovarian ultrasound scans and decide whether the ovary looks typical or shows signs of PCOS. Their approach, called MMFEDL‑DPCOS, begins by gently cleaning each scan using a process known as Gaussian filtering. In simple terms, this step smooths away random speckles and background noise while keeping important edges and details. The goal is to make the crucial structures in the ovary stand out more clearly so that the computer can focus on what matters, much like adjusting the focus and reducing grain in a photograph before inspecting it.
Many digital “eyes” working together
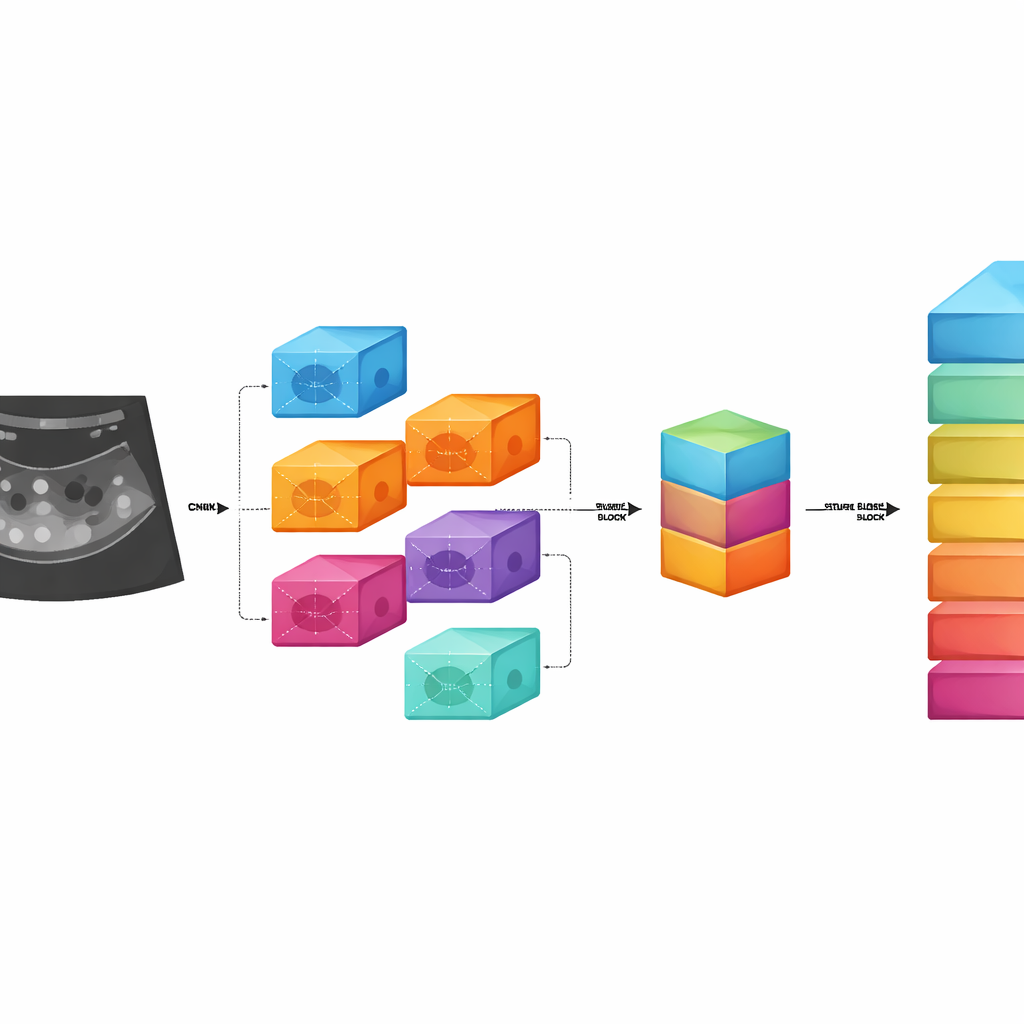
Instead of relying on a single pattern‑recognition method, the team combines five different deep learning image models—well‑known tools in computer vision that excel at spotting shapes and textures. Each model looks at the same ultrasound image but captures slightly different aspects, from fine‑grained details to broader structural patterns within the ovary. These five streams of information are then fused into a single, rich description of what the image contains. This fused representation is passed to a second learning module called a regularized stacked autoencoder, which distills the information further and learns to separate PCOS from non‑PCOS images while avoiding overfitting, a common pitfall where a model memorizes training data instead of learning general rules.
Putting the system to the test
To judge how well their method worked, the authors trained and evaluated it on a public collection of 9,000 ovarian ultrasound images, evenly split between women with PCOS and those without. They gradually refined the system through thousands of training cycles and monitored how accurately it labeled new, unseen images. The final version correctly distinguished PCOS‑affected from unaffected ovaries in about 99 out of 100 cases, and it did so faster than several other machine learning approaches, including traditional classifiers and single deep networks. When the researchers disabled parts of the system in “ablation” tests, performance consistently dropped, showing that combining multiple image models and the final autoencoder stage was crucial to its strong results.
What this could mean for patients
In everyday terms, this study demonstrates that a carefully designed artificial intelligence tool can read ovarian ultrasound images with very high accuracy, potentially matching or supporting experienced specialists while working far more quickly. Such a system could act as a second pair of eyes for radiologists and gynecologists, flagging concerning scans, reducing missed cases, and helping standardize PCOS diagnosis across clinics. The authors note that their work still relies on a single dataset and will need testing on more diverse images and patient groups. Even so, it offers a promising step toward more objective, early, and widely available PCOS screening, which could translate into earlier treatment options and better long‑term health for many women.
Citation: Kranthi, S., Sandeep, Y., Pranathi, K... et al. A multimodal feature fusion with deep representation learning approach for polycystic ovary syndrome diagnosis using ultrasound images. Sci Rep 16, 9977 (2026). https://doi.org/10.1038/s41598-026-40718-w
Keywords: polycystic ovary syndrome, ultrasound imaging, deep learning, medical diagnosis, women’s health