Clear Sky Science · en
Potential gonadal-beneficial effect of sitagliptin against paclitaxel-induced testicular dysfunction via mediating PERK/CHOP/NLRP3/Sestrin2 signaling pathway
Why this study matters for cancer patients
Chemotherapy saves lives but can quietly damage fertility, especially in men. One widely used cancer drug, paclitaxel, is known to harm the testes and lower sperm quality. This study in rats asks a practical question with clear human relevance: can an already-approved diabetes pill, sitagliptin, be repurposed to shield the male reproductive system from paclitaxel’s side effects without interfering with its cancer-fighting role?
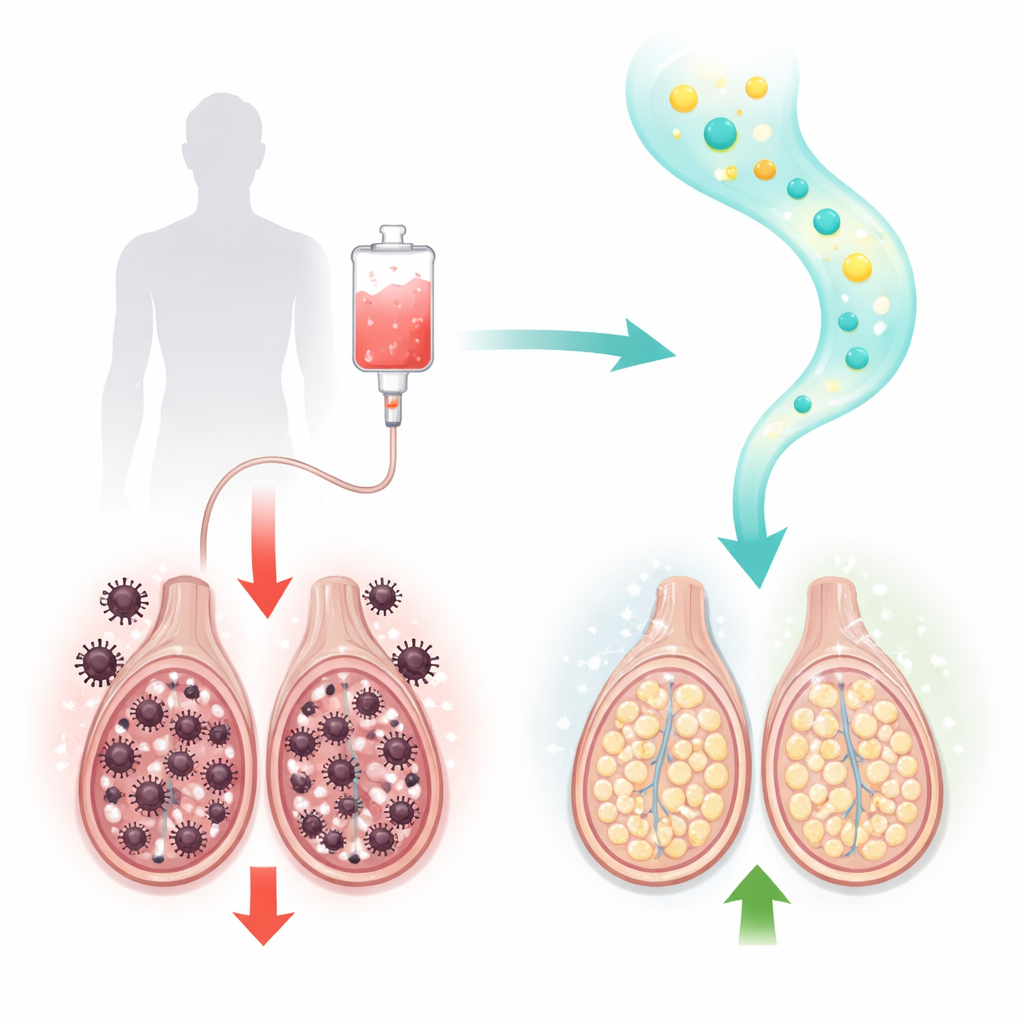
A common cancer drug with a hidden cost
Paclitaxel is a mainstay treatment for breast, ovarian, lung, and other solid tumors. It works by freezing the cell division machinery of fast-growing cancer cells. Unfortunately, dividing cells in healthy organs are also vulnerable. In male rats, paclitaxel treatment led to classic signs of testicular injury: sperm counts, motility, and viability all dropped sharply, while misshapen sperm increased. Under the microscope, the researchers saw damaged seminiferous tubules (where sperm are made) and injured hormone-producing Leydig cells, along with shrunken tissue layers. Blood tests confirmed that testosterone and a key enzyme needed to make it, 17β-hydroxysteroid dehydrogenase, were greatly reduced.
A diabetes drug as an unexpected protector
Sitagliptin is widely prescribed to control blood sugar in people with type 2 diabetes. Earlier work hinted that, beyond its metabolic effects, sitagliptin can dampen harmful oxidative stress, inflammation, and cell death in organs such as the liver, kidney, and brain. Building on this, the researchers divided male rats into four groups: untreated controls, a paclitaxel-only group, and two groups that received paclitaxel plus either a lower or higher dose of sitagliptin for two weeks. They then compared sperm quality, hormone levels, tissue structure, and a set of molecular “alarm systems” inside the testes that sense stress and trigger inflammation and cell suicide.
How sitagliptin calmed cellular stress and inflammation
Paclitaxel pushed the testes into a state of oxidative and internal stress: levels of damaging by-products (measured as malondialdehyde) rose, while natural defenses such as reduced glutathione and the enzyme catalase fell. Deep inside cells, the protein-folding factory known as the endoplasmic reticulum switched on a danger pathway called PERK–CHOP, a signal that prolonged stress is tipping cells toward death. At the same time, an inflammatory protein complex (NLRP3) became highly active, driving up inflammatory messengers like interleukin‑1β and activating a cascade of cell-death proteins, including cytochrome c and caspase‑3. Sitagliptin reversed much of this. Both doses reduced oxidative damage and restored antioxidant defenses. They markedly lowered activation of the PERK–CHOP stress route and curbed NLRP3-driven inflammation and apoptosis. A protective protein called Sestrin2, which helps clear reactive molecules and has been linked to healthier sperm, was boosted by sitagliptin at both the gene and protein level.
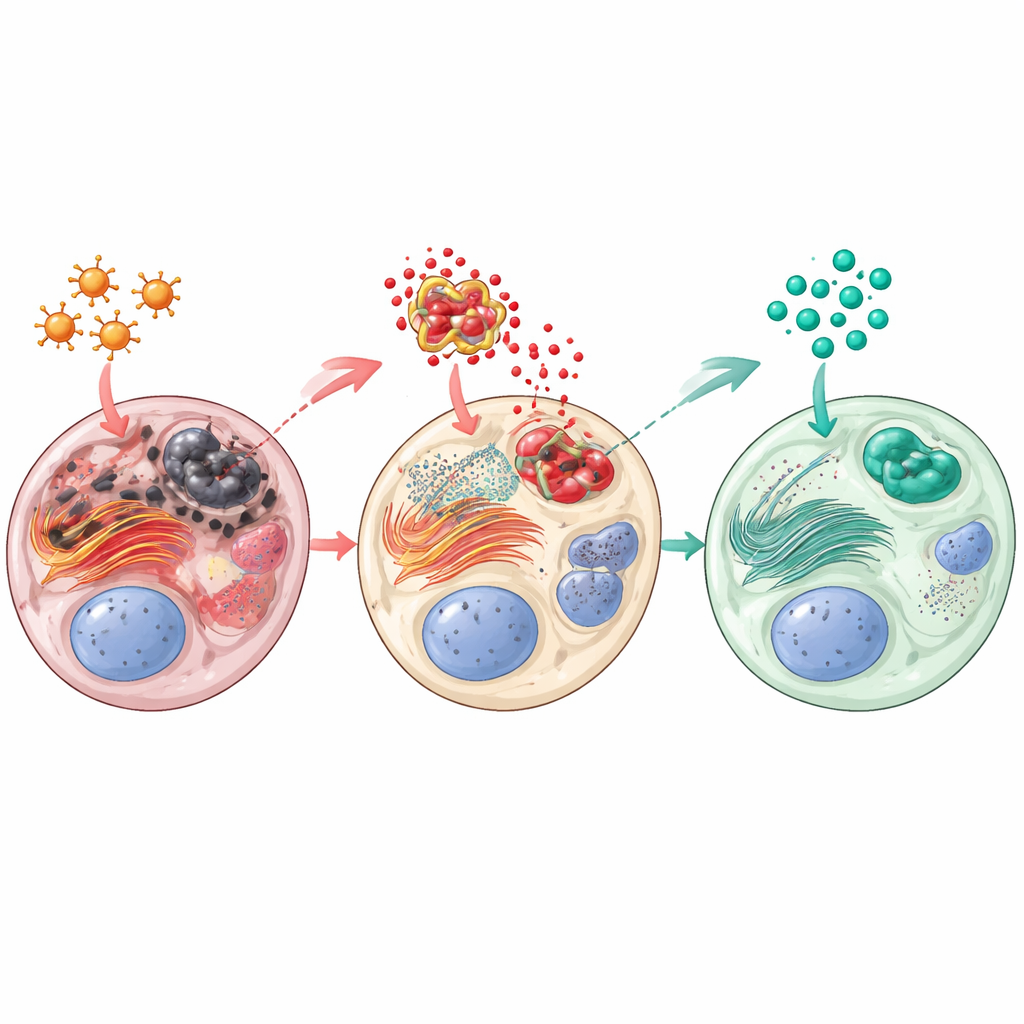
Better sperm, healthier tissue, stronger hormones
The biochemical improvements translated into tangible functional benefits. Rats given sitagliptin after paclitaxel had higher sperm counts, better motility, and fewer abnormal sperm than animals that received paclitaxel alone, with the higher sitagliptin dose coming closest to normal. Testosterone and 17β‑hydroxysteroid dehydrogenase rebounded, suggesting that steroid hormone production by Leydig cells was recovering. Under both light and electron microscopes, sitagliptin-treated testes showed more orderly seminiferous tubules, more Leydig cells, thicker and healthier cell layers, and fewer structural distortions. Overall, the drug helped preserve the architecture and function needed for ongoing sperm production.
What this could mean for men undergoing chemotherapy
This animal work suggests that sitagliptin can significantly blunt paclitaxel-induced damage to the testes by quieting a network of harmful signals—oxidative stress, internal protein-folding stress, inflammation, and programmed cell death—largely through boosting Sestrin2 and dialing down the PERK/CHOP/NLRP3 axis. Because sitagliptin is already used in the clinic for diabetes, it stands out as a realistic candidate to test as a fertility-protective add‑on in men receiving paclitaxel, particularly those who are also diabetic. The authors emphasize that human studies are still needed, but their findings raise a hopeful possibility: a familiar pill might one day help cancer patients keep not only their lives but also their chances of fathering children.
Citation: El-Beheiry, K.M., El-Shitany, N.A., El-Sayad, M.ES. et al. Potential gonadal-beneficial effect of sitagliptin against paclitaxel-induced testicular dysfunction via mediating PERK/CHOP/NLRP3/Sestrin2 signaling pathway. Sci Rep 16, 9090 (2026). https://doi.org/10.1038/s41598-026-40511-9
Keywords: paclitaxel, sitagliptin, male fertility, oxidative stress, testicular toxicity