Clear Sky Science · en
Adipocyte-specific NR5A2 deficiency ameliorates diet-induced metabolic syndrome by suppressing adipose tissue inflammation
Why fat cells matter for whole-body health
Obesity is often portrayed as a simple problem of extra weight, but the real danger lies in what happens inside fat tissue. When fat cells grow too large, they can become inflamed and send out distress signals that disrupt blood sugar control, strain the liver, and raise the risk of type 2 diabetes. This study explores a little-known molecular switch inside fat cells called NR5A2 and shows that turning it off in mice can protect against many of the harmful effects of a high-fat diet.
A molecular switch in fat
The researchers began by asking a basic question: does NR5A2, a protein that helps control gene activity, behave differently in obesity? They found that in mice fed a rich, high-fat diet and in genetically obese mice, fat tissue ramped up production of NR5A2. Both the deep belly fat and the fat under the skin showed higher levels of this protein, and its activity also rose when precursor cells were turning into mature fat cells in the lab. These patterns suggested that NR5A2 might be closely tied to the way fat tissue expands and responds to calorie overload.
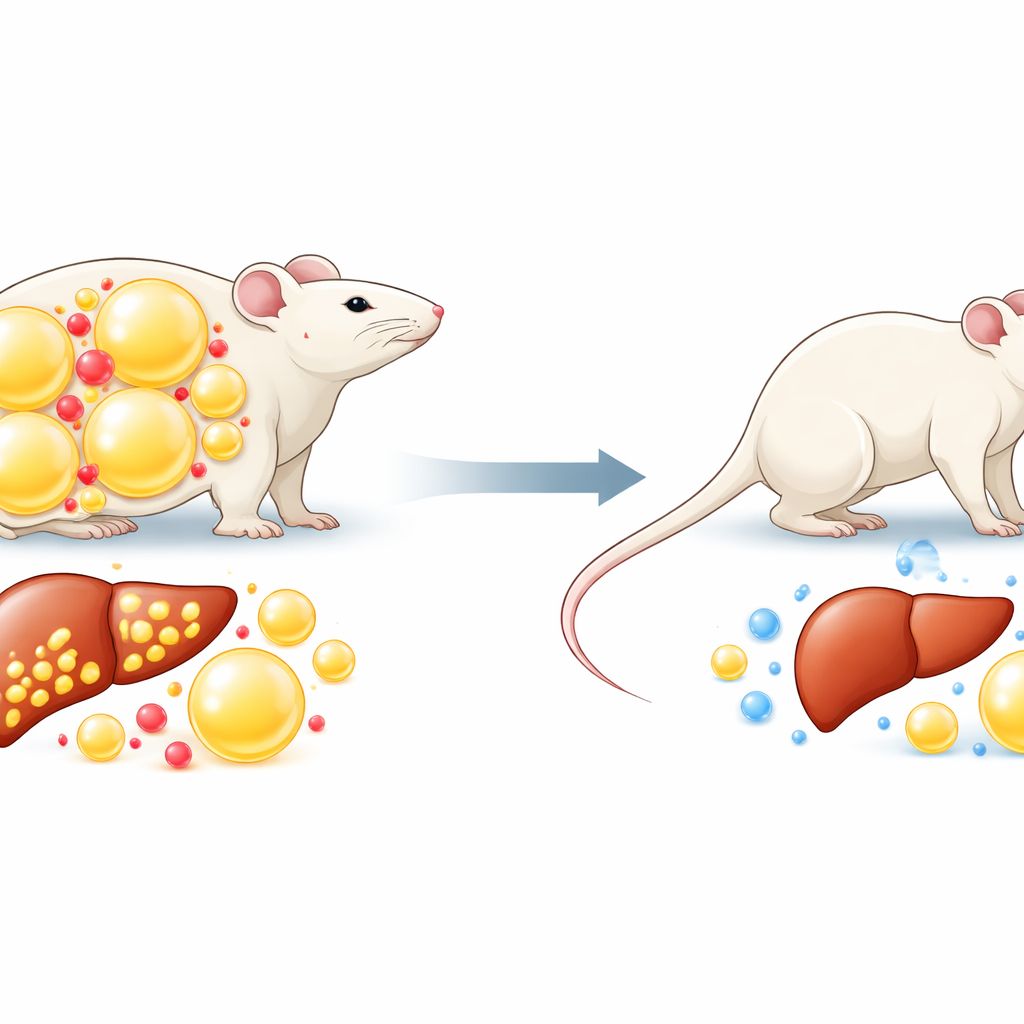
Switching off NR5A2 in fat cells
To test NR5A2’s role directly, the team engineered mice in which NR5A2 was removed only from fat cells, leaving other organs untouched. Under normal chow, these mice looked much like their littermates. But when both groups were fed a high-fat diet, the difference was striking. Mice lacking NR5A2 in fat cells gained less weight, accumulated less body fat, and their individual fat cells remained smaller. Importantly, they ate and drank just as much as the control mice, suggesting that the protection did not come from dieting behavior but from how their fat tissue handled excess calories.
Better blood sugar and less liver fat
These leaner fat cells translated into healthier metabolism. Mice without NR5A2 in their fat cells cleared sugar from the bloodstream more efficiently and responded better to insulin, a hormone that keeps blood sugar in check. Their fasting blood sugar and insulin levels were lower, indicating that their bodies did not have to work as hard to manage glucose. The high-fat diet typically causes fat buildup in the liver, a condition known as fatty liver, but in the modified mice the liver stayed lighter and contained less fat. Blood fats, including triglycerides and cholesterol, were also reduced, pointing to broad improvements in how the body processed and stored lipids.
Quieter inflammation and more energy burning
Obese fat tissue often becomes a hub of chronic, low-grade inflammation, filled with immune cells that surround and clear dying fat cells. In the high-fat-fed mice with intact NR5A2, the researchers observed many such immune cell clusters and high levels of inflammatory molecules. In contrast, fat from NR5A2-deficient mice showed fewer invading immune cells and lower levels of inflammatory signals. At the same time, these animals burned more energy, as shown by increased oxygen use, carbon dioxide production, and heat output, even though their activity levels and diet were similar. In laboratory experiments, cells lacking NR5A2 were less able to mature into large, fat-storing adipocytes, hinting that this protein normally promotes fat cell growth and storage.
What this could mean for future treatments
Taken together, the findings paint NR5A2 as a key driver linking overfed fat cells to inflammation, fatty liver, and poor blood sugar control. In mice, blocking NR5A2 only in fat cells made those cells smaller and calmer, reduced harmful signals to the rest of the body, and boosted energy use, all of which eased signs of metabolic syndrome. While much work remains to translate this to people and to understand the exact pathways involved, the study suggests that carefully targeting NR5A2 in fat tissue could become a novel strategy to combat obesity-related diseases without simply relying on eating less.
Citation: Yuan, W., He, S., Zang, Y. et al. Adipocyte-specific NR5A2 deficiency ameliorates diet-induced metabolic syndrome by suppressing adipose tissue inflammation. Sci Rep 16, 11864 (2026). https://doi.org/10.1038/s41598-026-40395-9
Keywords: obesity, adipose inflammation, insulin resistance, fatty liver, energy expenditure