Clear Sky Science · en
Learning from multiple readings for axial spondyloarthritis classification of the sacroiliac joints
Why this matters for people with back pain
Chronic low back pain can be life-altering, and one important cause is a condition called axial spondyloarthritis, which often attacks the joints linking the spine to the pelvis. Doctors use magnetic resonance imaging (MRI) to spot early signs of damage in these sacroiliac joints, but reading hundreds or thousands of scans by eye is slow and sometimes inconsistent between experts. This study shows how a fully automated computer system can outline these joints and grade several kinds of damage on MRI with performance similar to human specialists, potentially speeding up care and making assessments more reliable.
Looking closely at a hard-to-see joint
The sacroiliac joints sit deep in the pelvis, where the base of the spine meets the hip bones. In axial spondyloarthritis, these joints can show swelling, scarring, erosion, and new bone growth, all of which appear as subtle patterns on MRI. Today, trained readers carefully scan each image and score these changes, but even experts often disagree with themselves on different days or with one another. The authors set out to tackle two linked problems: first, teaching a computer to find and trace the outline of each sacroiliac joint on MRI; and second, training it to detect five key lesion types that matter for diagnosis and monitoring. By automating both steps, they aim to reduce the workload on radiologists and rheumatologists while improving consistency across large clinical trials and, eventually, routine practice.
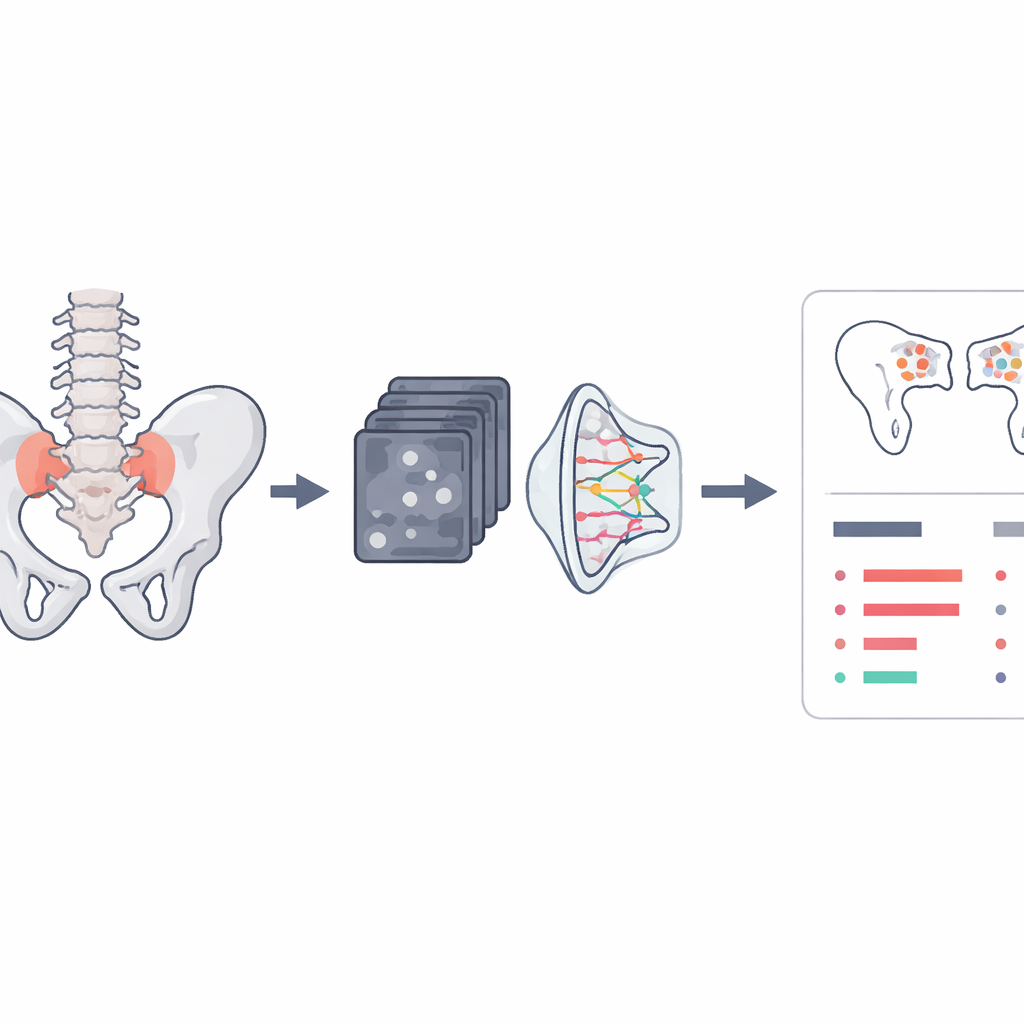
Teaching the computer to draw the joint
To find the sacroiliac joints, the team designed a method that does not just color in the joint as a solid block but instead learns the precise line of its boundary. They train a neural network to predict a “flow” of tiny arrows across each MRI slice, where arrows outside the joint point toward the nearest spot on the joint edge and arrows lying on the edge follow its direction like a path. The same network also predicts where the boundary should start and end. A virtual “walker” then follows the arrows from the start point to the end point, tracing an open curve that marks the joint. Tested on a large local dataset of nearly 17,000 images, this contour-following approach produced smoother and more accurate joint outlines than a simpler landmark-based method, with most errors smaller than a few millimeters—good enough to define a tight region of interest for later grading.
From clean outlines to detailed damage maps
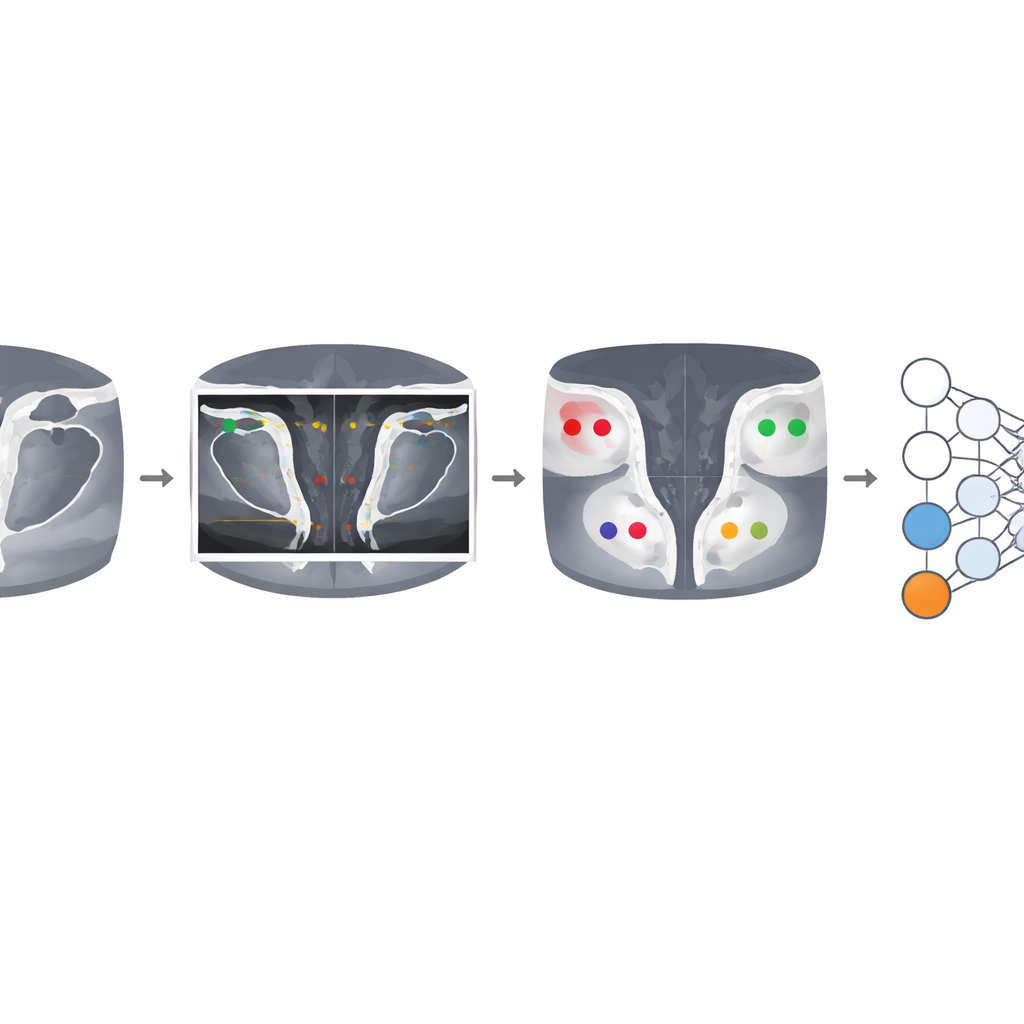
Once the joints are outlined, the system crops focused regions around the left and right sacroiliac joints from two types of MRI sequences that highlight different tissue features. Each joint is divided into four quadrants on the pelvis and spine sides. A deep learning model then examines the stack of slices and, for each quadrant and each whole joint, predicts whether five lesion types are present: bone marrow swelling, fatty change, surface erosion, hardening of bone, and fusion of the joint. A distinctive feature of this work is how it handles human disagreement. Instead of relying on a single score, the model is trained on multiple readings from several experts, learning how each reader tends to grade scans and how their opinions combine into a shared “consensus.” This allows the computer to mimic the collective judgment of specialists rather than any single observer.
Proving reliability across multiple clinical trials
The researchers trained their lesion classifier on MRI scans from a large ankylosing spondylitis trial and then tested it on two independent trials that were never used during training. Across these studies, the system showed strong ability to distinguish scans with and without lesions, with performance varying slightly by lesion type. It was especially accurate in detecting advanced changes like joint fusion and bony overgrowth, and somewhat less so for early, more subtle swelling signals—a challenge that also affects human readers. When model predictions were compared with consensus labels from multiple experts, its accuracy and discrimination were on par with, and in some cases close to, the agreement levels seen between human readers themselves.
What this means for patients and clinicians
In everyday terms, the study demonstrates that a computer can learn to trace the sacroiliac joints on MRI and flag important patterns of joint damage with skill comparable to human experts, even when those experts do not always agree with each other. While the system does not replace clinical judgment, it offers a way to standardize how sacroiliac joint MRIs are read in research and, with further validation, in clinics. That could lead to faster, more consistent diagnoses, better tracking of how disease responds to treatment, and more efficient large-scale studies of new therapies for people living with axial spondyloarthritis.
Citation: Jamaludin, A., Windsor, R., Ather, S. et al. Learning from multiple readings for axial spondyloarthritis classification of the sacroiliac joints. Sci Rep 16, 9866 (2026). https://doi.org/10.1038/s41598-026-39417-3
Keywords: axial spondyloarthritis, sacroiliac joint MRI, medical imaging AI, lesion classification, chronic back pain