Clear Sky Science · en
AI-assisted diagnosis of cervical dysplasia from cervicography images
Why this matters for women’s health
Cervical cancer is one of the most preventable cancers, yet many women in low-resource regions still lack access to advanced screening tools. This study explores how artificial intelligence can turn simple cervical photographs, taken after a vinegar-like solution is applied, into a powerful aid for spotting early precancerous changes. By doing so, it aims to bring more accurate diagnosis to clinics that do not have expensive equipment or specialists, helping catch disease earlier and potentially saving lives.
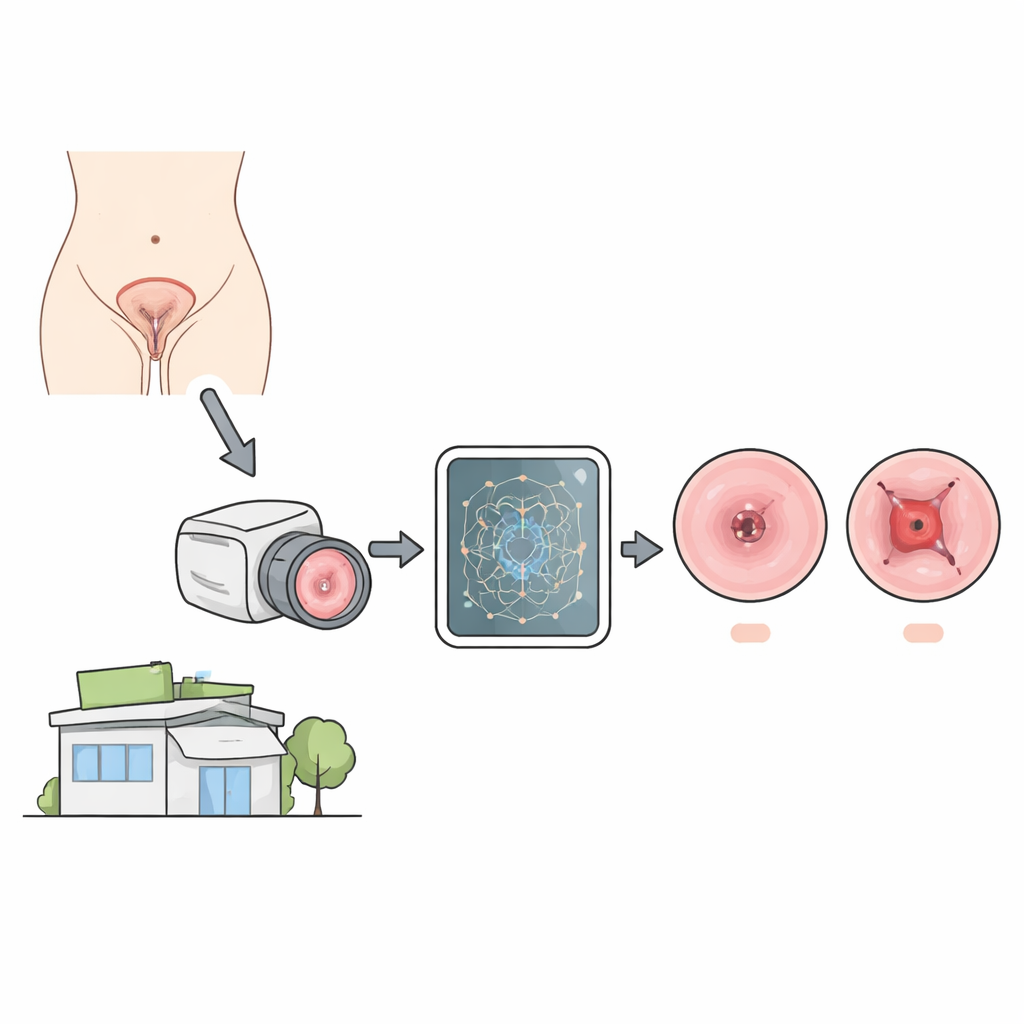
From simple photos to smarter screening
In many high-income hospitals, doctors use a magnifying device called a colposcope to closely inspect the cervix and decide whether suspicious areas should be biopsied. In poorer or rural settings, this tool is often unavailable, so nurses rely on Visual Inspection with Acetic Acid (VIA): they apply diluted acetic acid, look for white patches, and may take a photo (cervicography). VIA is good at flagging that something might be wrong, but it is much less reliable at judging how serious the abnormality is. The key clinical decision is whether a lesion is mild and can be monitored, or severe and needs immediate treatment. The researchers set out to teach a computer to make this distinction directly from cervicography images.
Teaching computers to read subtle visual cues
The team built a two-stage system around a modern image-analysis model known as YOLOv11, chosen for its ability to find objects quickly and run on modest hardware. First, the system checks if a VIA image contains a suspicious lesion at all, based on medical rules about how the white areas should appear and where they should lie on the cervix. If a lesion is present, the second stage examines four visual features that colposcopy experts rely on: how white the area becomes after acid, how smooth or rough its surface looks, how much of the transformation zone it covers, and how many of four cervical quadrants are involved. Each feature is analyzed either by the AI model or by simple geometric rules, and together they provide a richer picture of disease severity than color alone.
Making more data from few patients
A major obstacle was that high-quality, biopsy-confirmed images, especially of early mild disease, are rare. To overcome this, the researchers used a type of generative AI (StyleGAN-2 with adaptive augmentation) to create realistic synthetic cervix images that mimicked underrepresented patterns. These artificial images were used only for training and validation, never for final testing. The real data came from several sources, including large international datasets with colposcopy images and Swede Score labels, a smaller but highly reliable set with histopathology confirmation, and external collections from Indonesian hospitals and mobile-phone-based screening programs. This blend allowed the model to learn from both expert grading and gold-standard tissue diagnoses.
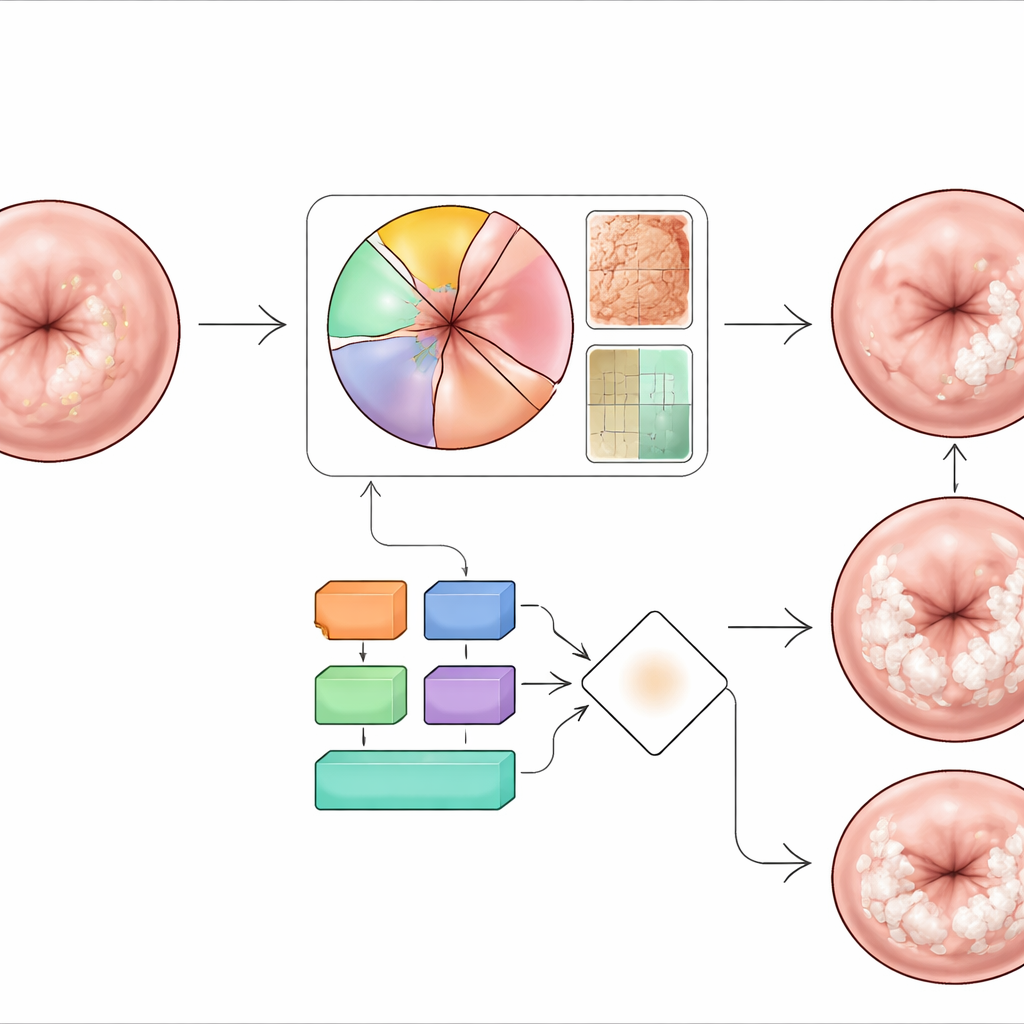
Blending multiple opinions into one decision
Once the four key features were extracted from each image, the system used an ensemble approach—essentially a structured “vote” among different feature-specific classifiers—to label each case as mild or severe dysplasia. Early experiments without advanced augmentation reached only about 62% accuracy, showing how difficult the task is when data are scarce and imbalanced. After adding GAN-generated training images and carefully tuning the ensemble, the best configuration achieved around 95% overall accuracy on an independent biopsy-confirmed test set. It correctly identified more than 95% of severe cases and over 80% of mild ones, while keeping the overall misclassification rate below 8%. The model also performed consistently on a separate hospital dataset, suggesting it can handle variations in equipment and local practice, though performance did dip when confronted with brightly lit mobile-phone images.
What this means for everyday care
For non-specialist clinics that already perform VIA screening, this work shows that ordinary cervicography images could be turned into a much more informative tool. An AI system that highlights lesions, estimates how far they have spread, and indicates whether they look mild or severe could help frontline providers decide who needs urgent referral and who can be safely monitored. The authors caution that their model still has limits: it relies partly on synthetic data, was trained mostly on colposcopy rather than real-world phone images, and has been tested on relatively small biopsy-confirmed sets. Larger, more diverse studies are needed before such a system can guide treatment on its own. Nonetheless, the results demonstrate that combining affordable imaging with carefully designed AI could strengthen cervical cancer prevention in exactly the places that need it most.
Citation: Nurmaini, S., Rachmatullah, M.N., Agustiansyah, P. et al. AI-assisted diagnosis of cervical dysplasia from cervicography images. Sci Rep 16, 9920 (2026). https://doi.org/10.1038/s41598-026-39192-1
Keywords: cervical cancer screening, cervicography, medical AI, deep learning, dysplasia grading