Clear Sky Science · en
Spinal cord involvement and cardiovascular autonomic dysfunction in Parkinson’s disease
Why this matters for everyday health
People often think of Parkinson’s disease as a condition that only affects movement—tremor, stiffness, and slowness. But many patients also struggle with dizziness when standing up and fainting spells caused by drops in blood pressure. This study asks a simple but important question: are tiny changes in the upper spinal cord helping to drive these dangerous blood pressure problems, and could advanced MRI scans reveal them early?
Looking beyond the brain
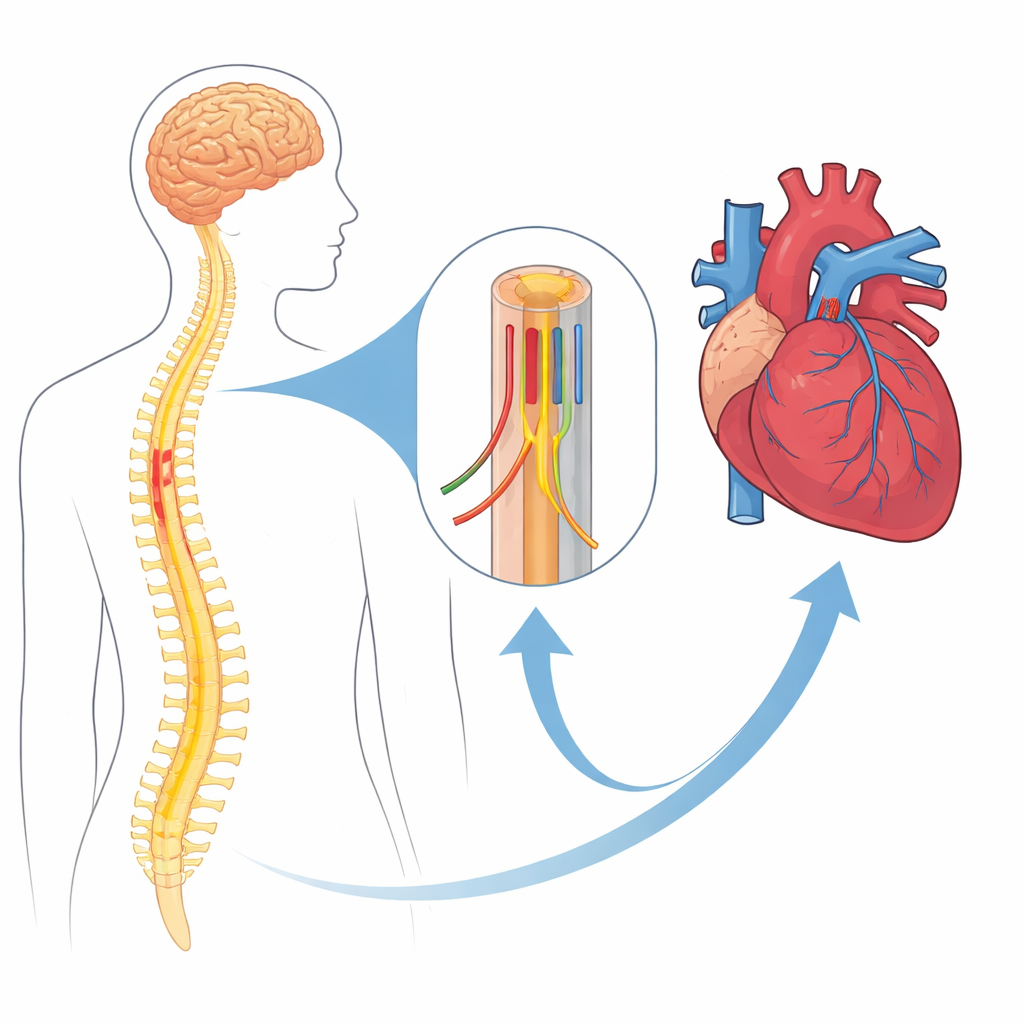
Parkinson’s disease is now understood to involve the entire nervous system, not just the brain. Nerve cells that automatically regulate the heart and blood vessels run through the upper chest portion of the spinal cord before reaching the heart. Damage here could disrupt the body’s ability to keep blood pressure steady when a person stands up, leading to a condition called orthostatic hypotension. The researchers focused on this key spinal region to see whether its structure, measured with advanced MRI techniques, relates to blood pressure problems in people with Parkinson’s disease.
Who was studied and how
The team examined 26 people with Parkinson’s disease and 22 healthy volunteers of similar age and sex. Among the patients, they separated those who also had REM sleep behavior disorder—a condition where people act out their dreams—from those who did not, because prior work suggests this sleep problem may signal a form of Parkinson’s with earlier and more severe autonomic issues. All participants underwent detailed MRI scans of the neck and upper chest spinal cord. The scans measured subtle tissue properties that can hint at nerve fiber health and myelin (the insulation around nerves). The researchers then compared these measurements across the three groups and linked them to blood pressure changes when participants went from lying down to standing, both at the time of scanning and over a five-year follow-up.
What the scans did—and did not—show
When the scientists looked at each MRI measurement on its own, they did not find strong, clear-cut structural differences in the spinal cord between Parkinson’s patients and healthy volunteers, or between the two Parkinson’s subgroups. However, when they combined many MRI features at once using a multivariate machine-learning method, the patterns in the spinal cord data could distinguish healthy people from patients, and also separate the two Parkinson’s subtypes fairly well. This suggests that while individual measurements may look normal, their overall pattern carries meaningful information about disease-related changes.
Links between spinal changes and blood pressure
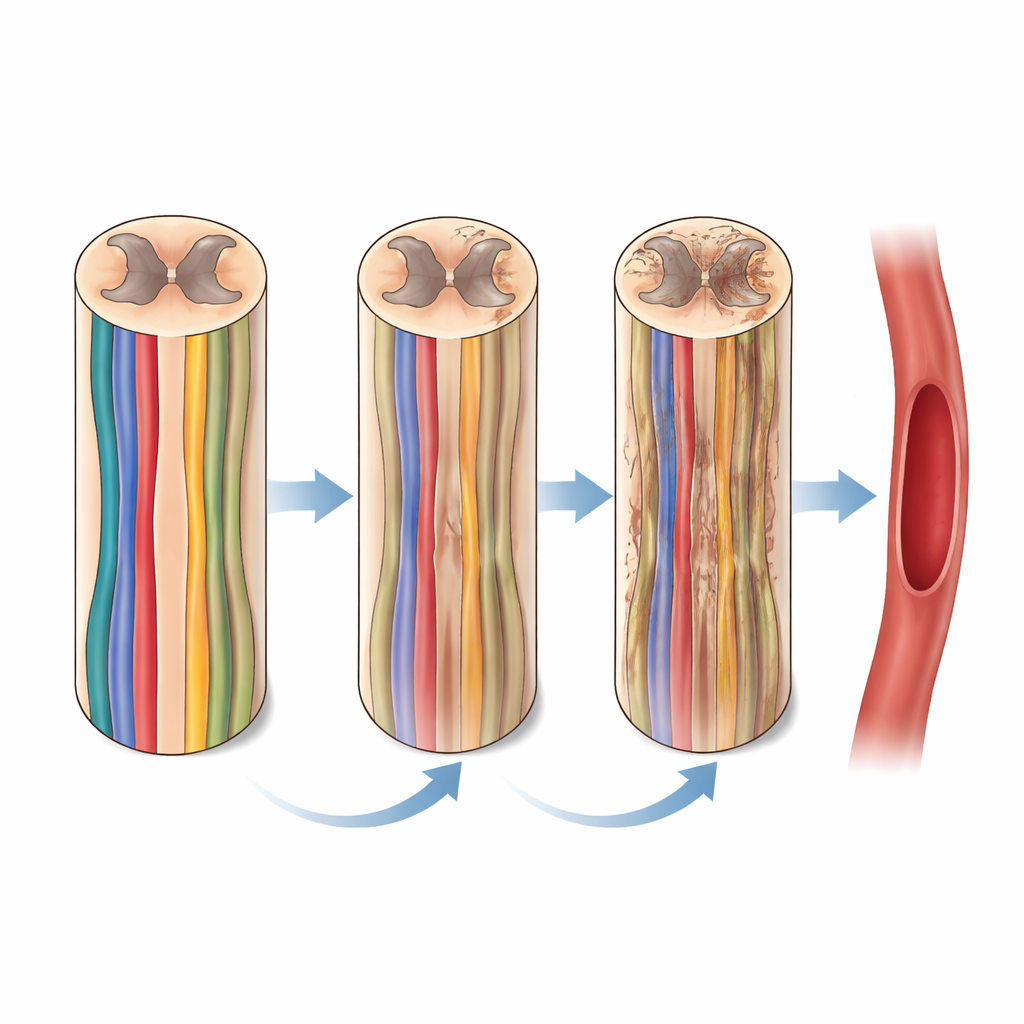
The most striking findings emerged when the team zoomed in on the junction between the lower neck and upper chest, where crucial blood pressure control centers sit. In patients with both Parkinson’s disease and REM sleep behavior disorder, larger drops in blood pressure on standing were tied to specific MRI signs of altered microstructure in the nerve tracts and gray matter of this region. Moreover, these MRI features predicted how blood pressure responses would change over five years, even after accounting for age, sex, and initial blood pressure. These associations were not seen in patients without the sleep disorder or when all Parkinson’s patients were grouped together, hinting that spinal cord involvement may be especially important in this higher-risk subtype.
What this means going forward
For non-specialists, the takeaway is that Parkinson’s disease appears to reach beyond the brain into the spinal cord in ways that may quietly disturb the body’s automatic control of blood pressure. While this small study did not prove overt structural damage that clearly separates all patients from healthy people, it suggests that sensitive MRI markers in a specific spinal region track with current and future blood pressure problems in a vulnerable subgroup. If confirmed in larger studies, such spinal cord imaging could one day help doctors identify which patients are at greatest risk of fainting and falls, allowing earlier monitoring and treatment of cardiovascular complications in Parkinson’s disease.
Citation: Chougar, L., Lejeune, FX., Cohen-Adad, J. et al. Spinal cord involvement and cardiovascular autonomic dysfunction in Parkinson’s disease. Sci Rep 16, 13831 (2026). https://doi.org/10.1038/s41598-026-38152-z
Keywords: Parkinson’s disease, spinal cord, autonomic dysfunction, orthostatic hypotension, quantitative MRI