Clear Sky Science · en
FTY-720 pre-treatment attenuates acute lung injury following bilateral renal ischemia/reperfusion but not bilateral nephrectomy
When Failing Kidneys Threaten the Lungs
People in intensive care often face more than one organ failing at a time. Doctors have long noticed that when the kidneys suddenly stop working, the lungs frequently become leaky and stiff, making breathing difficult and raising the risk of death. This study, carried out in rats, asks a deceptively simple question with big implications: does a particular group of immune cells called lymphocytes drive this dangerous kidney–lung connection, and can an approved drug that traps these cells protect the lungs?
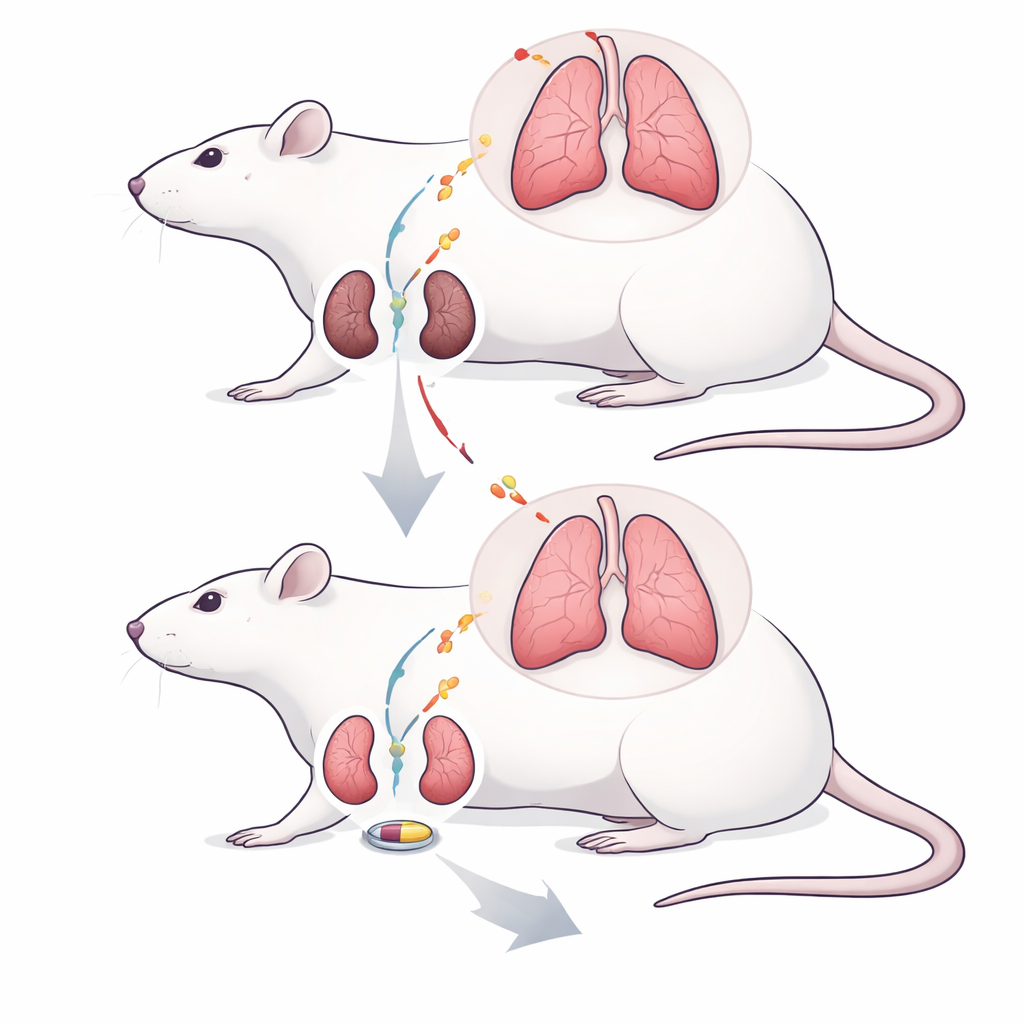
A Closer Look at Kidney and Lung Damage
The researchers focused on acute kidney injury, a rapid loss of kidney function that commonly occurs after major surgery, severe infection, or kidney transplantation. In this condition, waste products and salts quickly build up in the blood, and the injured kidneys release a storm of reactive molecules and inflammatory signals. These substances can travel through the bloodstream and damage distant organs, especially the lungs, which receive the entire cardiac output. The team used well-established rat models that either temporarily cut off blood flow to both kidneys (ischemia/reperfusion) or completely removed both kidneys (nephrectomy) to mimic different routes to sudden kidney failure.
Testing an Immune-Targeting Drug
To probe the role of lymphocytes, the scientists turned to FTY-720 (fingolimod), a drug already approved for multiple sclerosis. Fingolimod works by causing lymphocytes to remain trapped in lymph nodes, leading to a sharp drop in their numbers in the bloodstream. Rats were divided into five groups: a sham surgery group; a group with temporary kidney blood-flow blockage; a group with both kidneys removed; and two additional groups that received fingolimod before either ischemia or nephrectomy. Over the next 24 hours, the team monitored kidney function, blood chemistry, lung structure, lung fluid leakage, and gas exchange, as well as how many white blood cells, including lymphocytes, were circulating.
Protection Only When Kidneys Are Injured by Ischemia
Blocking blood flow to the kidneys for one hour and then restoring it caused severe kidney damage: blood flow through the kidneys fell, filtering capacity plunged, and the kidneys lost their ability to finely control salt, water, and urine concentration. Waste products such as creatinine and urea, as well as potassium and acid, rose sharply in the blood, together with markers of oxidative stress. The lungs of these animals showed swollen walls, bleeding, excess fluid, and heavy infiltration of inflammatory cells, along with poor oxygen transfer. Remarkably, rats pretreated with fingolimod before ischemia had much healthier kidney tissue, better kidney blood flow and filtration, lower levels of waste products and oxidative markers in the blood, and far less structural and functional lung injury.
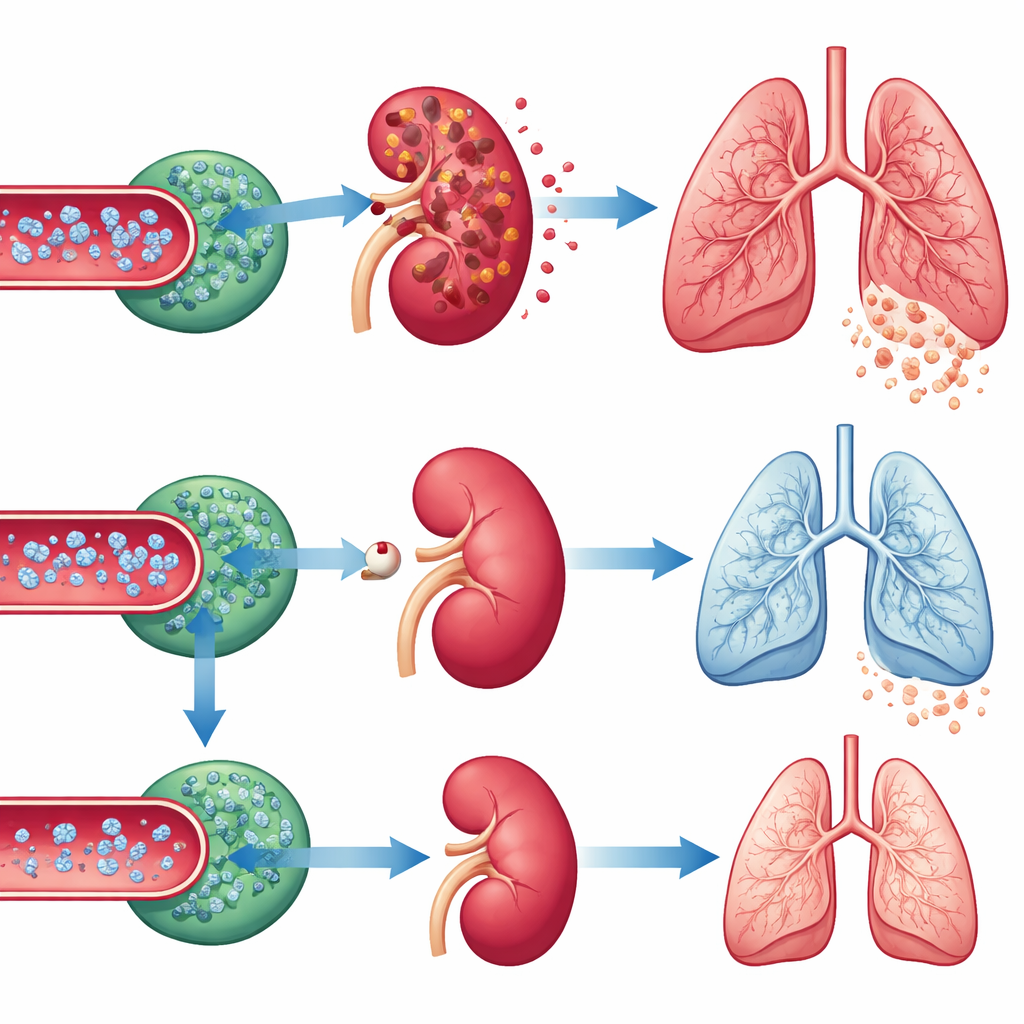
When Kidneys Are Removed, the Story Changes
Removing both kidneys also produced strong rises in blood waste products and salts and led to clear signs of lung injury and fluid buildup. Fingolimod pretreatment in this setting did what it was supposed to do in the blood—it caused a profound drop in circulating lymphocytes. Yet despite this lymphocyte depletion, the severity of lung injury after nephrectomy was essentially unchanged. Lung leakiness, swelling, and oxygen transfer were no better in drug-treated animals than in untreated ones. This contrast—strong lung protection in the ischemia model but no benefit in the nephrectomy model—was key to interpreting the results.
What This Means for Patients
The study shows that fingolimod can strongly protect the lungs, but only when it first protects the kidneys from ischemic damage. When the kidneys are absent altogether, lowering lymphocyte numbers does not help the lungs, even though lung injury still occurs. To a lay reader, this means that lymphocytes alone are unlikely to be the main messengers that carry injury from the kidneys to the lungs. Instead, the drug’s benefit seems to come from keeping the kidneys themselves healthier, which in turn reduces the harmful substances that spill into the bloodstream and damage the lungs. While these findings come from rats and from a preventive treatment strategy, they sharpen the search for the true culprits in kidney–lung cross-talk and suggest that future therapies may need to focus on directly limiting kidney damage and the toxic signals it releases.
Citation: Alebrahimdehkordi, N., Karimi, Z., Owji, S.M. et al. FTY-720 pre-treatment attenuates acute lung injury following bilateral renal ischemia/reperfusion but not bilateral nephrectomy. Sci Rep 16, 10373 (2026). https://doi.org/10.1038/s41598-026-38140-3
Keywords: acute kidney injury, acute lung injury, fingolimod, organ crosstalk, ischemia reperfusion