Clear Sky Science · en
Traumatic brain injury among patients presenting from prison: a cohort study
Why this study matters
When someone in prison experiences a serious head injury, their chances of survival and recovery may not be the same as for someone in the general community. This study asks a stark question: for people with traumatic brain injury who come to the hospital from prison, are their outcomes worse, even when their injuries look similar on paper? The answer has important implications for fairness, medical ethics, and how we care for some of society’s most medically vulnerable people.
Who was studied
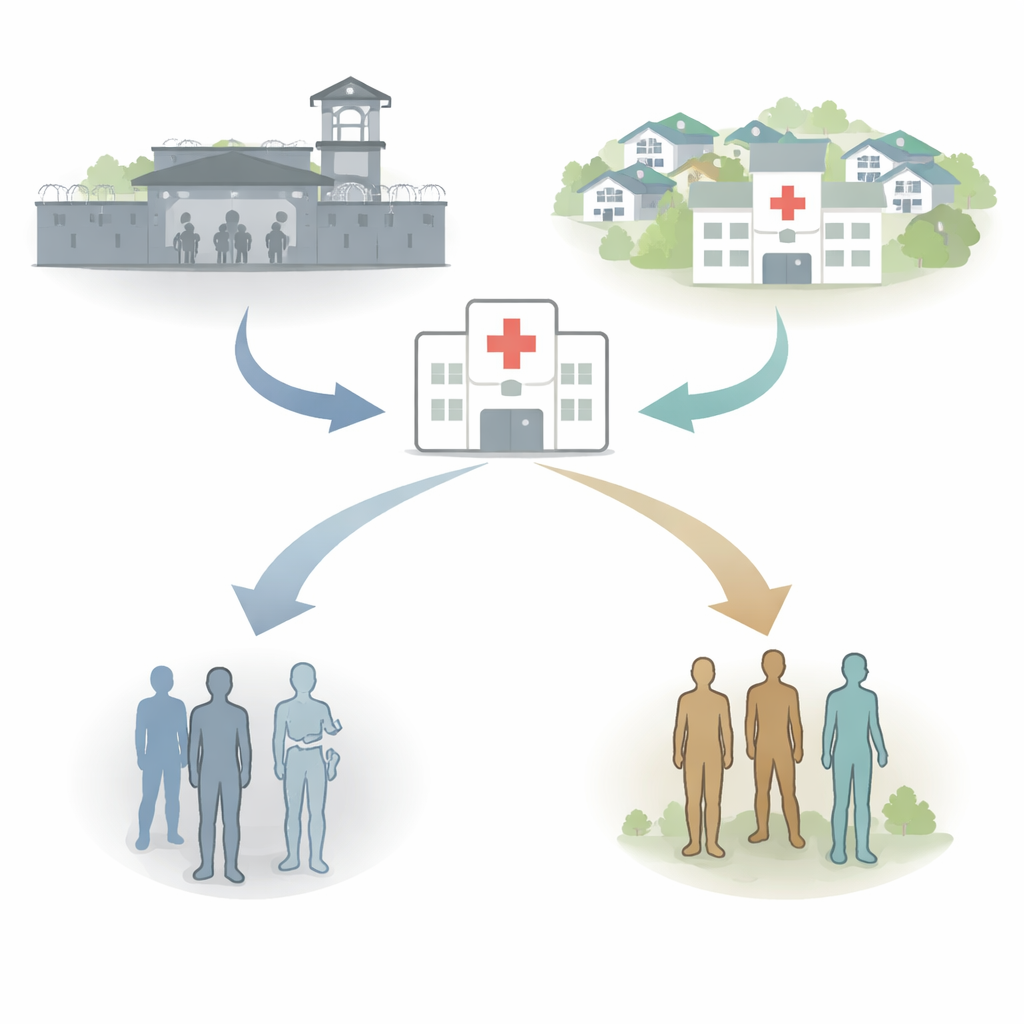
The researchers examined records from the National Trauma Data Bank, a large collection of cases from trauma centers across the United States, focusing on the years 2021 and 2022. They looked at adults with traumatic brain injury—damage to the brain caused by a blow or penetrating force to the head—and compared more than 4,600 patients whose injuries occurred in prison with over 500,000 whose injuries occurred in the community. To make a fair comparison, they used statistical matching to pair incarcerated patients with similar patients from the community based on age, sex, race, and key measures of how badly injured they were, including standard trauma and brain-injury scores.
Different ways people get hurt
The study found that people arriving from prison with head injuries looked quite different from those arriving from the community. Incarcerated patients were younger, overwhelmingly male, and more likely to be Black. They generally had fewer long-term health problems and somewhat less severe overall injuries. How they were injured also differed sharply. In prison, most head injuries came from assaults or being struck, while crashes involving cars, motorcycles, or pedestrians and firearm-related wounds were rare. In contrast, community patients were far more often injured unintentionally, especially in motor vehicle crashes, and were more likely to have multiple body regions severely injured.
What happened in the hospital
When the researchers compared patients whose injury severity and brain injury scores were closely matched, they found that key hospital treatments were used at similar rates. Incarcerated and community patients with comparable injuries were about equally likely to receive intensive interventions such as brain pressure monitoring or surgery to relieve pressure on the brain. Lengths of stay in the intensive care unit and overall hospital stay were also broadly similar. However, patients from prison were more often transferred between hospitals, raising questions about whether they were initially brought to the best-equipped facility.
Who survived and where they went next
The most troubling differences appeared in survival and what happened after the hospital stay. Overall, patients from prison with traumatic brain injury died in the hospital more often than matched patients from the community. Among those with the most severe brain injuries, coming from prison was linked to a 43% higher risk of death, even after adjusting for factors like age, race, and how extensive the injuries were. For survivors, pathways also diverged. Incarcerated patients were far less likely to be discharged to places that specialize in recovery, such as acute rehabilitation centers and skilled nursing facilities, and more likely to be sent back to correctional custody. This gap was especially large for older adults, who often need intensive support after a serious brain injury.
What this means for people and policy
To a lay observer, this study suggests that where a person lives at the time of injury—behind bars or in the community—may shape their odds of surviving a severe brain injury and accessing the rehabilitation care that supports long-term recovery. The injuries themselves were not more severe in the prison group, and measurable high-level treatments looked similar, yet outcomes were worse and access to post-hospital services more limited. The authors argue that structural barriers, such as delayed triage, complex decision-making processes for incapacitated patients, and limits on rehabilitation options for people who remain under correctional control, may be driving an invisible but important inequity. They call for deeper investigation and targeted reforms to ensure that people with traumatic brain injury receive equitable emergency care, intensive treatment, and long-term rehabilitation, regardless of incarceration status.
Citation: Feler, J., Schachman, N., Cielo, D. et al. Traumatic brain injury among patients presenting from prison: a cohort study. Sci Rep 16, 13388 (2026). https://doi.org/10.1038/s41598-026-37391-4
Keywords: traumatic brain injury, incarceration, health disparities, prison healthcare, rehabilitation access