Clear Sky Science · en
Trehalose ameliorates severe acute pancreatitis by modulating gut microbial metabolism
Why a Sweet Molecule Matters for a Dangerous Disease
Severe acute pancreatitis is a sudden, painful inflammation of the pancreas that can lead to organ failure and death, yet doctors still lack targeted drugs to treat it. This study explores an unexpected ally: trehalose, a simple sugar already used as a food additive and medical excipient. By following how trehalose interacts with gut microbes and their chemical by-products, the researchers show that this sugar can rebalance intestinal metabolism, calm inflammation, and limit pancreatic damage in mice—offering a fresh angle on treating a life-threatening condition.
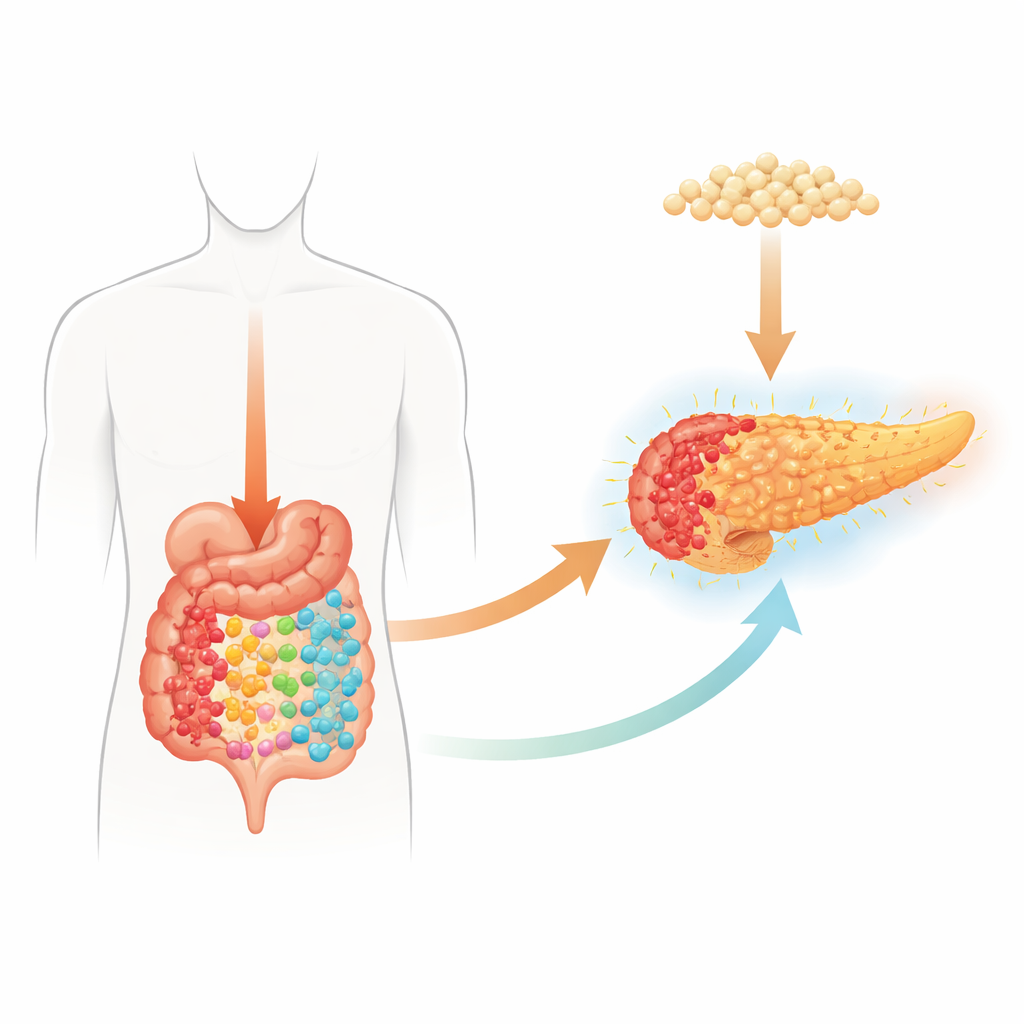
A Delicate Organ Under Siege
The pancreas helps digest food and control blood sugar, but when its enzymes activate too early, the organ begins to digest itself, triggering severe acute pancreatitis. About a third of patients develop a dangerous form that can damage multiple organs, and current care focuses mainly on supportive measures such as fluids and nutrition. Mounting evidence suggests that the trillions of microbes living in our intestines—and the chemicals they produce—play a central role in how bad pancreatitis becomes. Some patients and animal models with severe disease show major shifts in gut bacteria and their metabolic products, hinting at a hidden communication channel between microbes, the gut, and the pancreas.
When Gut Microbes and Their Chemistry Go Off Balance
In mice with severe acute pancreatitis, the team found that both the makeup of gut bacteria and their metabolic activity were profoundly disrupted. Microbes that normally support a healthy intestine declined, while others expanded. At the same time, the chemical fingerprints in the gut shifted: substances linked to fat metabolism surged, whereas products of carbohydrate and amino acid metabolism dropped. When the researchers wiped out most gut bacteria with a broad antibiotic cocktail, pancreatic injury, blood fats, and inflammatory molecules in the bloodstream decreased. Strikingly, this microbial depletion also caused a sharp rise in certain gut carbohydrates, especially trehalose, suggesting that specific sugars might be tied to protection.
A Safe Sugar that Reprograms the Gut
To test whether trehalose itself could help, the scientists added it to the drinking water of mice before triggering pancreatitis. At modest concentrations, trehalose markedly reduced pancreatic inflammation and tissue death, and lowered blood triglycerides and key inflammatory signals such as IL-6, IL-17A, and TNF-α. High doses, however, caused intestinal upset without extra benefit, underscoring that more is not always better. Detailed genetic and chemical profiling revealed that trehalose gently reshaped the gut ecosystem. It consistently boosted a bacterial family called Muribaculaceae and reduced Lactobacillaceae, while nudging microbial metabolism away from fat processing and toward carbohydrate use, particularly pathways related to galactose. These changes partially reversed the metabolic imbalance seen during severe disease.
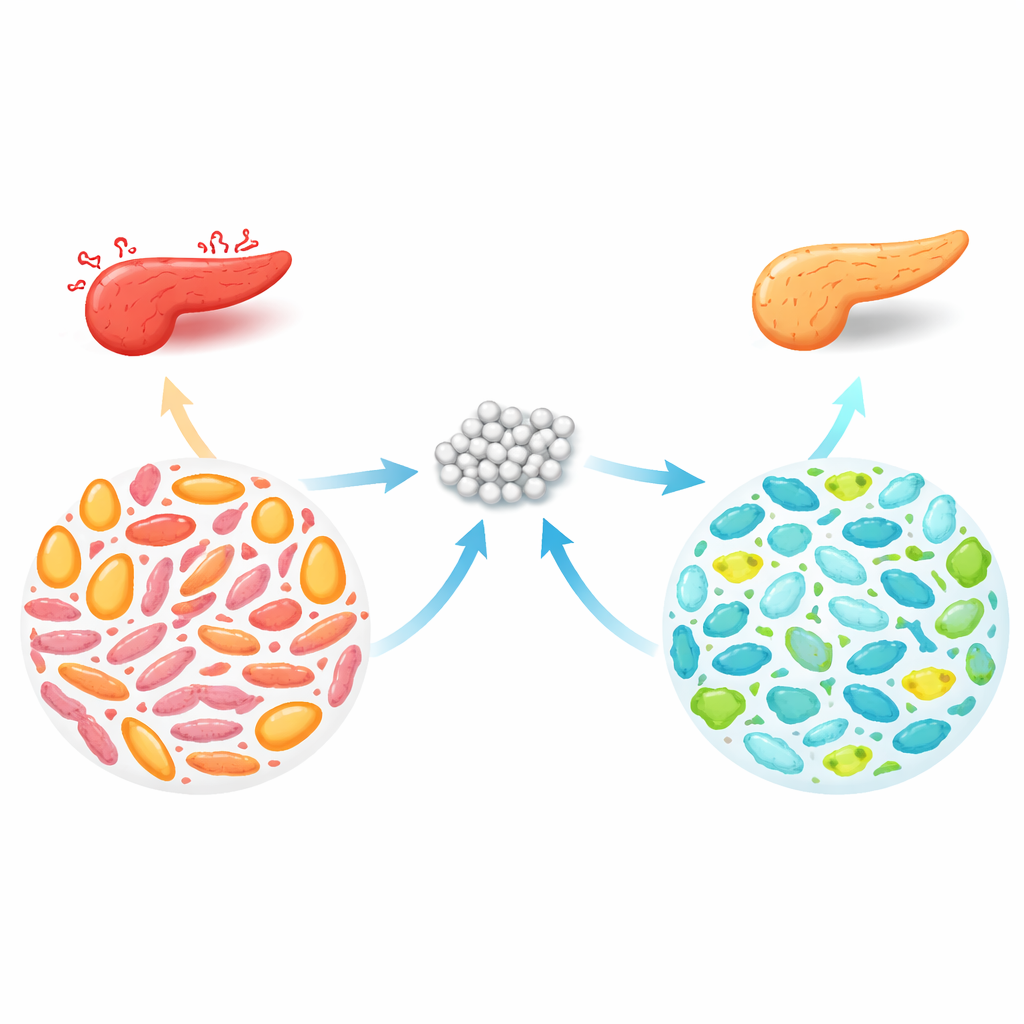
Microbe-Mediated Protection of the Pancreas
The protective effects of trehalose depended on the presence of gut microbes. In germ-free mice, which lack intestinal bacteria, trehalose no longer shielded the pancreas. But when these germ-free animals received fecal microbes from trehalose-treated donors, they gained protection: pancreatic injury and inflammatory markers fell, and blood fat levels improved. In both conventional and germ-free recipients, trehalose-linked microbial communities were marked by more Muribaculaceae and a metabolic signature of higher carbohydrate and lower fat processing. In the pancreas itself, trehalose and trehalose-trained microbiota reduced the infiltration of immune cells called macrophages and dampened activation of the cell-death enzyme caspase‑3, suggesting a direct impact on how much tissue is lost during an attack.
What This Means for Future Treatments
To a non-specialist, the core message is that a simple dietary sugar can instruct gut microbes to shift their chemistry in ways that protect a distant organ. By steering microbial metabolism toward burning more carbohydrates and fewer fats, trehalose helps quiet inflammation, curb harmful blood lipids, and limit cell death in the pancreas. The authors propose a "microbial metabolism–gut–pancreatic axis" in which diet, microbes, and their metabolites form a chain of cause and effect. While these experiments were done in mice and careful work is still needed to define safe doses and rule out unwanted effects in people, the findings raise the possibility that trehalose—or similar targeted dietary supplements—could one day complement standard care for severe acute pancreatitis by treating the gut to help heal the pancreas.
Citation: Hao, H., Du, D., Lin, H. et al. Trehalose ameliorates severe acute pancreatitis by modulating gut microbial metabolism. npj Biofilms Microbiomes 12, 81 (2026). https://doi.org/10.1038/s41522-026-00950-8
Keywords: severe acute pancreatitis, trehalose, gut microbiota, microbial metabolism, inflammation