Clear Sky Science · en
Alzheimer’s Disease blood biomarkers measured through remote capillary sampling correlate with cognition in older adults
Checking Brain Health from Home
Alzheimer’s disease is often detected late, after memory and thinking problems have already taken a serious toll. Most people with early signs of trouble never reach a specialist clinic. This study explores a simple idea with big implications: could older adults check key Alzheimer’s-related signals with an easy finger-prick test at home, then mail the sample to a lab? If reliable, this kind of home test could help find people at higher risk much earlier and guide who needs a full clinical workup or closer monitoring.
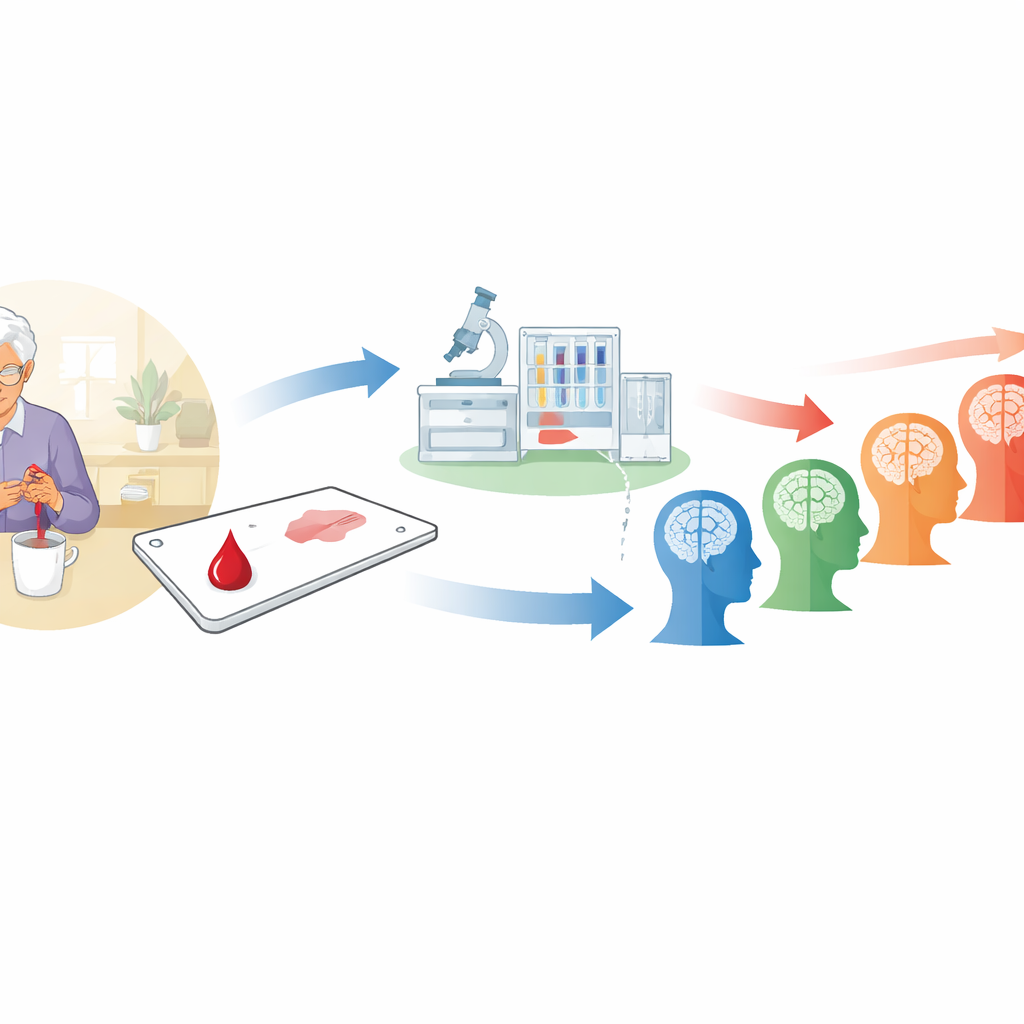
A Simple Finger-Prick Instead of a Hospital Visit
The researchers tested a new way to measure two blood markers linked to brain changes in Alzheimer’s and other forms of cognitive decline. Instead of drawing blood from a vein in a clinic, participants used a small device to prick a fingertip and placed a tiny amount of blood onto a special card at home. The card dries and preserves a plasma-like sample, which can be posted to a central laboratory without refrigeration. There, highly sensitive machines measure levels of two proteins in the blood: p-tau217, closely tied to Alzheimer’s disease changes in the brain, and GFAP, which reflects certain types of brain cell stress and inflammation. Alongside the blood test, participants completed online thinking and memory tests and answered questions about everyday functioning.
Blood Markers that Track Thinking Skills
Among 174 older adults who were either cognitively healthy, had mild cognitive problems, or had dementia, both p-tau217 and GFAP levels from finger-prick samples were linked to how well people performed on computer-based tests. Higher p-tau217 was associated with poorer episodic memory, attention, and executive skills such as planning and mental flexibility. GFAP was related to working memory and executive function. Both markers were also tied to how well people managed everyday activities like handling finances or shopping. When the team compared capillary finger-prick results with traditional venous blood samples in a subgroup, they found strong agreement, suggesting that the home-based method can capture the same biological signals as standard blood draws.
Sorting People into Risk Groups, Not Making a Diagnosis
The goal of this approach is not to diagnose Alzheimer’s from a single drop of blood, but to triage people by risk. Using statistical methods, the team chose cut-off values for p-tau217 and GFAP that favored high specificity: when the test flagged someone as above the threshold, they were quite likely to have meaningful cognitive or functional problems, even if sensitivity was modest. Participants above the p-tau217 cut-off performed substantially worse on thinking tests and daily function scales than those below it. By combining p-tau217 levels with memory scores, the researchers defined a high-risk group, a low-risk group, and an intermediate group. People in the high-risk corner of this scatter plot had clearly poorer performance across several thinking domains and daily functioning, while those in the low-risk corner did better than the rest of the cohort.
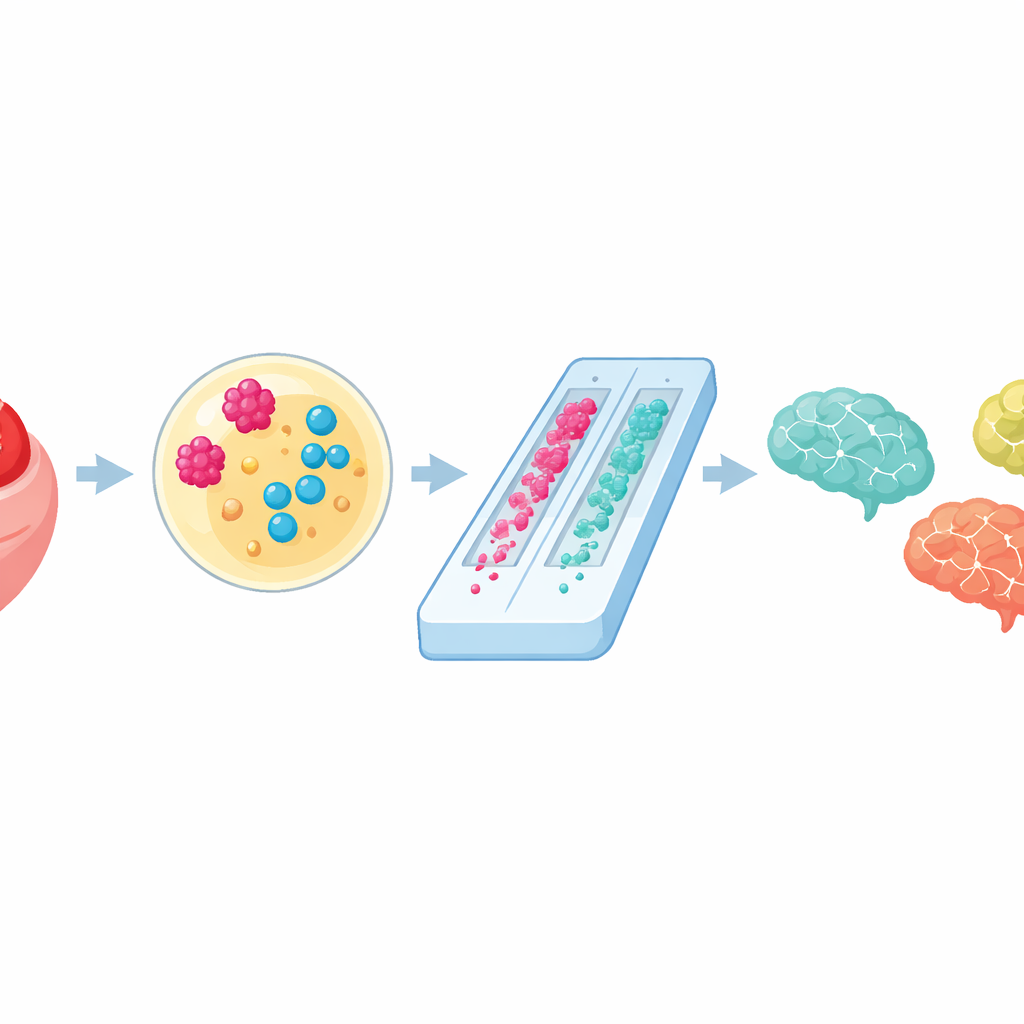
Different Markers, Different Clues
Interestingly, p-tau217 and GFAP did not flag the same people. Only a small fraction of participants were positive on both markers, suggesting that each captures somewhat different risk pathways. Further analysis showed that those with elevated GFAP were much more likely to report heart disease, and tended to have more attentional difficulties. In contrast, elevated p-tau217 did not track with heart disease or high blood pressure, fitting its role as a more Alzheimer-specific marker. This pattern hints that GFAP may highlight cognitive risk linked to blood vessel problems and brain inflammation, while p-tau217 may better reflect the classic Alzheimer’s process. Together, they may help clinicians identify people at risk for a range of progressive memory and thinking problems, not just Alzheimer’s alone.
A Step Toward Earlier and Easier Brain-Health Checks
Participants found the finger-prick kits acceptable and easy to use, with most completing the test on their own and many saying they would be willing to use such kits as part of routine healthcare. For now, these blood markers are best seen as a way to sort people into risk categories, guiding who should be invited for full assessment, further imaging, or closer monitoring over time. If confirmed in larger, long-term studies, at-home capillary blood testing combined with online cognitive assessments could offer a practical, scalable way to reach the many older adults who currently never see a specialist, allowing earlier support and more efficient recruitment into trials of new Alzheimer’s treatments.
Citation: Corbett, A., Sander-Long, M., Ashton, N.J. et al. Alzheimer’s Disease blood biomarkers measured through remote capillary sampling correlate with cognition in older adults. Nat Commun 17, 3699 (2026). https://doi.org/10.1038/s41467-026-71448-2
Keywords: Alzheimer’s screening, blood biomarkers, at-home testing, cognitive decline, early detection