Clear Sky Science · en
Differential cardiovascular and autonomic responses to structurally distinct intermittent hypoxia paradigms in rats
Why the Pattern of Lost Breath Matters
People with obstructive sleep apnea repeatedly stop breathing for brief moments during the night. Doctors usually rate how severe this is by simply counting how many times breathing is interrupted per hour. But not all patients with the same "score" develop high blood pressure or memory problems. This study in rats asks a deceptively simple question: does it matter whether those nightly oxygen drops are many and short, or fewer and longer, even if the total time spent low on oxygen is the same?
Two Ways to Mimic Sleep Apnea
To explore this, researchers exposed rats to two different patterns of interrupted oxygen while they rested. One pattern used many short dips in oxygen—brief 5‑second drops happening 60 times an hour. The other used fewer, longer dips—10‑second drops occurring 30 times an hour. Over three weeks, the animals spent eight hours a day in these conditions, while a control group breathed normal air. Tiny wireless sensors continuously tracked blood pressure, heart activity, brain waves, sleep stages, and breathing. The team also tested the animals’ maze learning and examined brain tissue for signs of damage or inflammation. 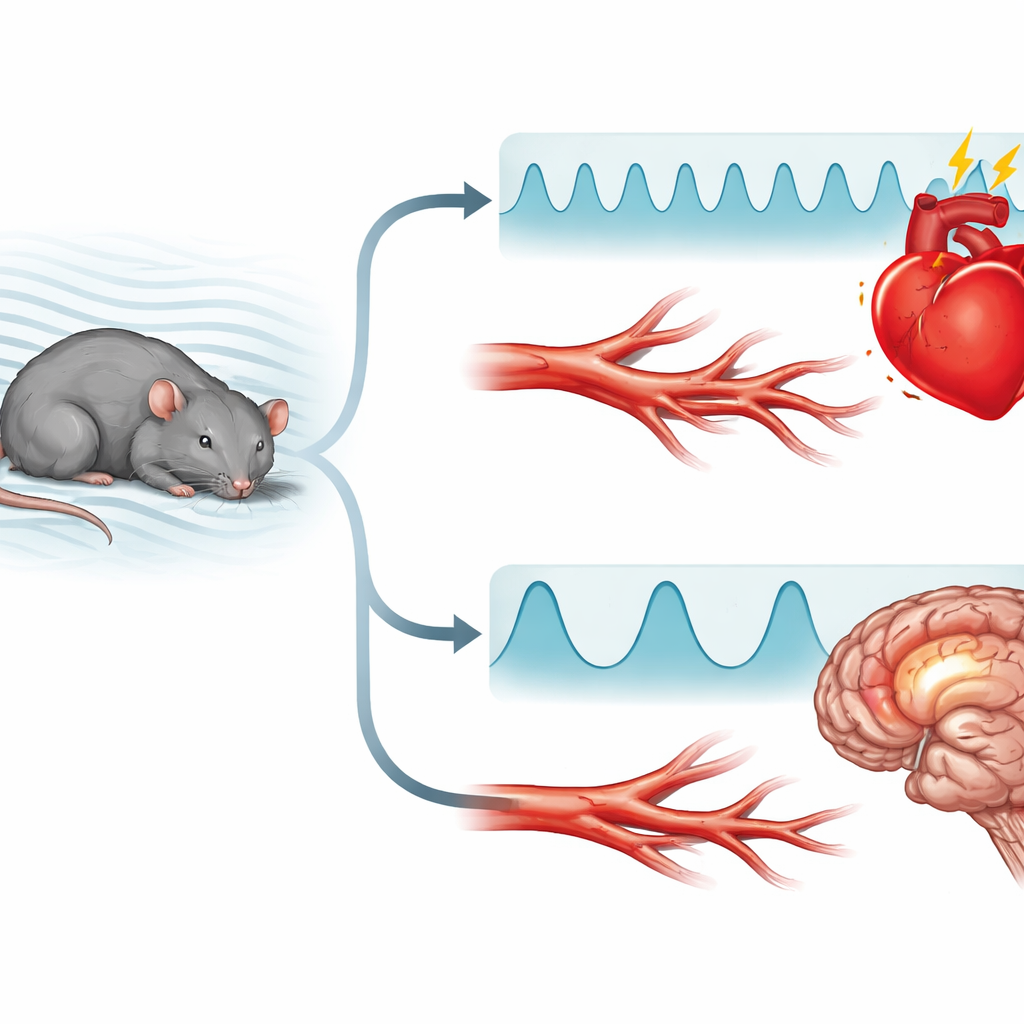
Short, Frequent Dips Strain the Heart and Vessels
Both abnormal breathing patterns raised blood pressure and tilted the automatic nervous system toward a more "fight‑or‑flight" state. But the many short dips produced a more troubling cardiovascular picture. Rats in this group showed more persistent high blood pressure that did not fall as much at night—a pattern known in people as "non‑dipping," which is linked to higher risk of heart disease and stroke. Measures of heart‑beat timing indicated ongoing over‑activity of the body’s stress nerves and weaker reflexes that normally buffer sudden changes in blood pressure. Their blood also showed thicker, more concentrated red cells, a change that can make blood harder to pump and further strain the circulation.
Fewer, Longer Dips Hit the Brain and Memory
The longer‑lasting oxygen drops told a different story. These rats did not keep their blood pressure elevated in the same sustained way, but they did show more disturbed sleep structure and a strong "rebound" of dream‑like sleep after the exposure ended, suggesting the brain was working harder to recover. In a spatial memory maze, these animals made more mistakes and wandered more than their peers, hinting at learning and memory problems. When the scientists examined the brain, especially the cortex and hippocampus—areas critical for thinking and memory—they found reduced levels of proteins that mark healthy nerve cells and increased markers of inflammation and stress. In other words, longer dips seemed to leave a deeper footprint on brain health.
Different Breathing Patterns, Different Sleep Brains
Brain‑wave recordings added another layer. During the oxygen‑drop periods, both hypoxia patterns reduced the slow, deep‑sleep waves and altered the rhythmic activity linked with dream sleep. Yet only the short, frequent pattern produced a lasting rise in fast "beta" brain activity during dream‑like sleep, a signal often associated with hyperarousal and a racing nervous system. This combination—restless brain activity plus stubbornly high blood pressure and blunted nighttime dipping—resembles a subset of sleep apnea patients whose bodies stay revved up even when they appear to be sleeping.
What This Means for People with Sleep Apnea
Overall, the study shows that not all interrupted‑breathing patterns are equal, even when the total time spent low on oxygen is matched. Many short, rapid drops mainly drove a cardiovascular stress profile: higher blood pressure, a more activated stress‑nerve system, and altered blood composition. Fewer, longer drops instead favored a brain‑vulnerability profile with greater inflammation, loss of nerve‑cell markers, and memory problems. 
Citation: She, SC., Lin, CW., Chen, CW. et al. Differential cardiovascular and autonomic responses to structurally distinct intermittent hypoxia paradigms in rats. Hypertens Res 49, 1659–1672 (2026). https://doi.org/10.1038/s41440-026-02588-7
Keywords: sleep apnea, intermittent hypoxia, blood pressure, autonomic nervous system, cognitive function