Clear Sky Science · en
Polystyrene nanoparticles promote endometrial cancer development through the ACSS2-mediated reprogramming of arachidonic acid metabolism
Why tiny plastics in our bodies matter
Plastic has quietly seeped into nearly every corner of modern life—and now, into our bodies. Scientists are increasingly finding microscopic plastic particles in human blood, lungs, and even in the tissue lining the womb. This study asks a pressing question with real-world consequences for women’s health: can these invisible plastic fragments help drive endometrial cancer, one of the most common cancers of the uterus? By tracing what happens when polystyrene nanoplastics encounter womb cancer cells, the authors uncover a step‑by‑step chain of events that links everyday pollution to tumor growth.
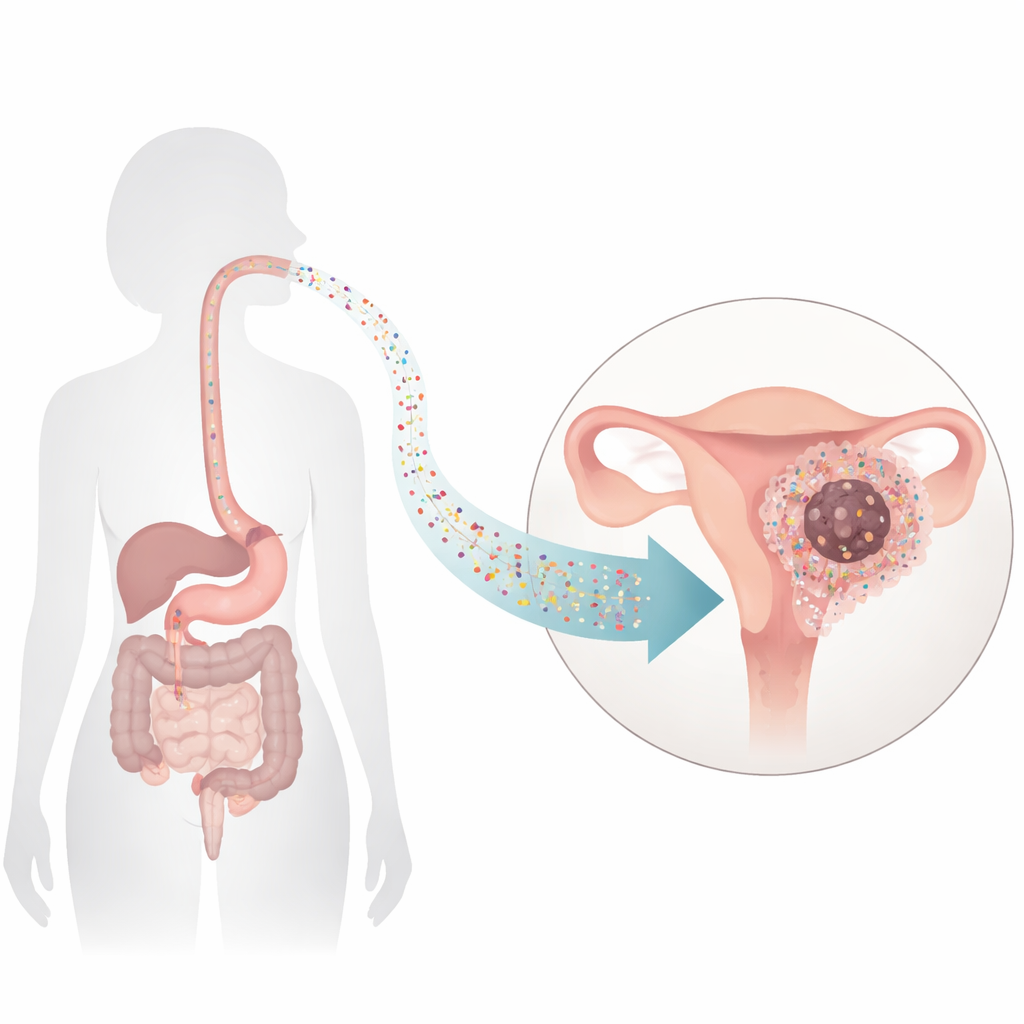
From daily exposure to hidden buildup
We encounter micro- and nanoplastics through food, water, air, and even household dust. Because nanoplastics are so small, they can slip through biological barriers and lodge in organs. Earlier work had already detected microscopic plastics in human endometrial tissue, but no one knew whether they simply sat there or actively fueled disease. In this study, researchers focused on polystyrene nanoplastics—a common type used in packaging and many consumer goods—and exposed human endometrial cancer cells and patient-derived “mini-tumors” (organoids) to them in the lab. Using fluorescent tags, they watched these particles steadily accumulate around and inside the cancer cells over hours and days, confirming that the cells can readily take them up.
Plastic particles push cancer cells into overdrive
Once inside, the nanoplastics did not remain harmless passengers. Long-term exposure made endometrial cancer cells divide faster, move more easily, and invade surrounding tissue more aggressively. Organoids grown from patient tumors also expanded more quickly when bathed in nanoplastics. To see whether the same held true in a living body, the team gave mice drinking water containing polystyrene nanoplastics. Over several weeks, mice with implanted endometrial tumors developed substantially larger and heavier tumors than control animals. The tumors from exposed mice contained more actively dividing cells, highlighting that the plastic particles were not just present, but were helping tumors grow.
A molecular chain reaction inside tumor cells
Digging deeper, the scientists mapped the internal changes triggered by nanoplastic exposure. They found that the particles increase reactive oxygen species—highly reactive molecules that signal cellular stress. This, in turn, activates a protein called AMPK, a kind of metabolic switch. When switched on, AMPK physically interacts with another enzyme, ACSS2, and helps move it into the cell’s nucleus. There, ACSS2 boosts the chemical “loosening” of DNA-packaging proteins, a form of epigenetic change that makes certain genes easier to turn on. One such gene is PLA2G3, which produces an enzyme that clips fatty molecules in cell membranes to release arachidonic acid, a key building block for inflammatory and growth-promoting signals.
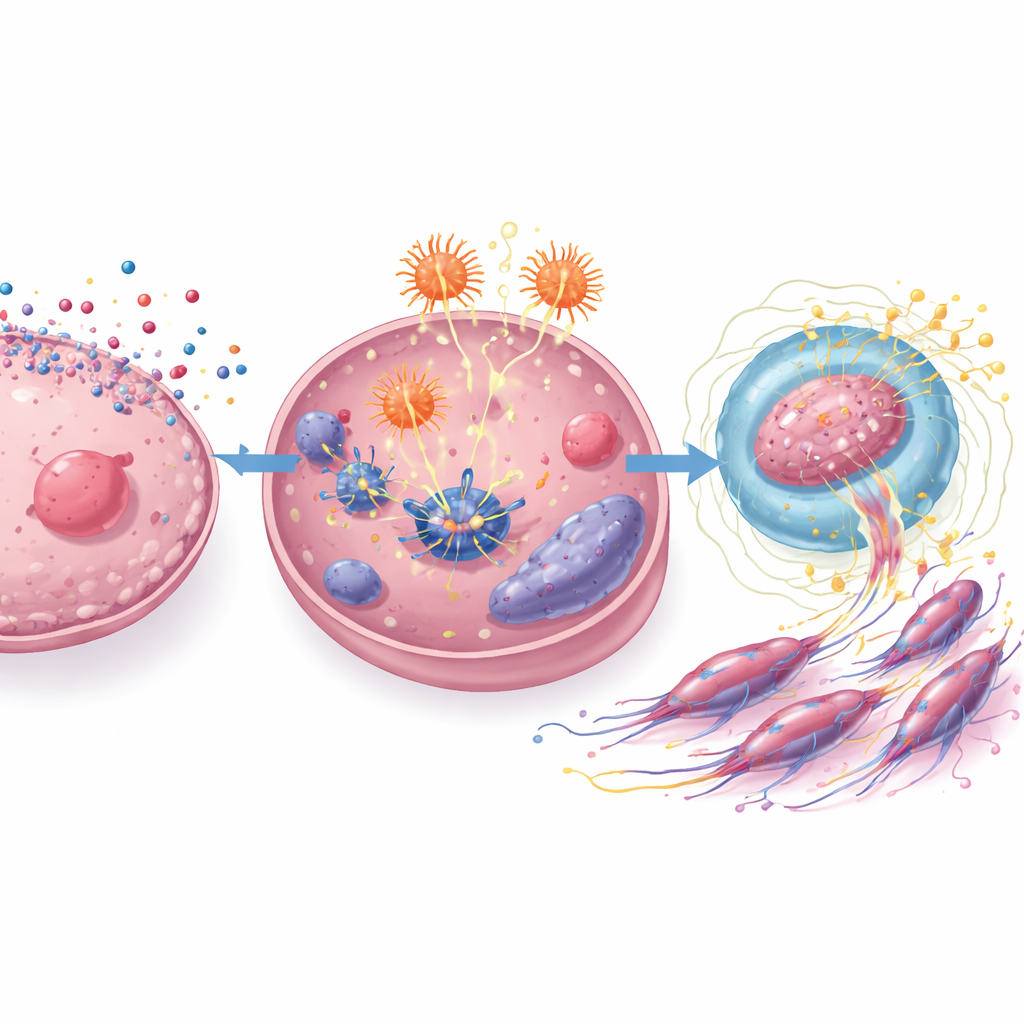
Rewiring fat chemistry to fuel invasion
By combining gene-activity data and targeted measurements of cellular fats, the researchers showed that nanoplastic-exposed cells ramp up PLA2G3 and produce more arachidonic acid. This shift in fat chemistry goes hand in hand with a classic transformation seen in dangerous tumors: epithelial–mesenchymal transition, or EMT. During EMT, cancer cells lose traits that keep them anchored in place and gain features that allow them to move and spread. In the study, plastic-exposed cells lost E-cadherin, a “Velcro-like” protein that helps cells stick together, and gained markers associated with mobility and tissue invasion. Blocking ACSS2 or PLA2G3 reversed many of these changes, reduced arachidonic acid levels, and curbed the cells’ ability to grow, migrate, and invade, underscoring this pathway as a critical link between nanoplastics and tumor aggressiveness.
What this means for everyday health
Taken together, the findings outline a clear story: polystyrene nanoplastics can enter endometrial cancer cells, build up inside them, and set off a stress-driven cascade that rewires fat metabolism and nudges tumors toward faster growth and greater invasiveness. Although this work was done in cancer models, not in healthy uterine tissue, it raises important concerns about chronic exposure to microscopic plastics in the environment. The study also points to potential early-warning markers and drug targets—such as ACSS2, PLA2G3, and arachidonic acid–related changes—that might one day help doctors identify or blunt plastic-related risks in endometrial cancer. For now, it offers some of the clearest evidence yet that the “Age of Plastics” may carry hidden costs for women’s reproductive health.
Citation: Huang, X., Xu, L., Wang, J. et al. Polystyrene nanoparticles promote endometrial cancer development through the ACSS2-mediated reprogramming of arachidonic acid metabolism. Cell Death Discov. 12, 189 (2026). https://doi.org/10.1038/s41420-026-03071-5
Keywords: microplastics, endometrial cancer, nanoplastics, lipid metabolism, uterine health