Clear Sky Science · en
SERBP1 is required for efficient HR repair and cisplatin chemoresistance in lung adenocarcinoma
Why this matters for cancer patients
Cisplatin, a decades-old chemotherapy drug, remains a mainstay treatment for lung adenocarcinoma, the most common form of lung cancer. Yet many tumors initially shrink and then learn to survive the drug, leaving patients with fewer options and poorer outcomes. This study uncovers a previously underappreciated molecular player, a protein called SERBP1, that helps lung tumors repair the DNA damage caused by cisplatin and thus escape its lethal effects. Understanding this escape route may open new ways to make existing treatments work better and longer.
A stubborn cancer and a fading weapon
Lung cancer is the leading cause of cancer-related death worldwide, and about 85 percent of cases are grouped under non-small cell lung cancer. Lung adenocarcinoma is the most frequent subtype. Even with advances in targeted drugs and immunotherapy, many patients still rely on cisplatin-based chemotherapy. Cisplatin works by latching onto DNA in rapidly dividing cells, creating cross-links that stall DNA copying and ultimately trigger cell death. However, tumors often become less responsive over time, a process known as chemoresistance. Until now, the detailed reasons why some lung tumors resist cisplatin while others remain vulnerable have been only partly understood.
Spotlighting a helper of hard-to-kill tumors
The researchers began by comparing lung tumor samples and nearby noncancerous tissue from patients, as well as several lung cancer cell lines and normal airway cells. They consistently found higher levels of a protein called SERBP1 in tumors, and especially in cisplatin-resistant cancer cells. Patients with more SERBP1 in their tumors tended to have shorter survival and more advanced disease, including greater spread to lymph nodes. When the team artificially lowered SERBP1 levels in resistant lung cancer cells grown in the lab, those cells became more sensitive to cisplatin, formed fewer colonies, and underwent more programmed cell death. In contrast, boosting SERBP1 in previously sensitive cells made them harder to kill with cisplatin and increased their growth, even in the drug’s presence.
A hidden lifeline for damaged DNA
Diving deeper, the scientists focused on how SERBP1 affects the cell’s ability to fix broken DNA. Cisplatin often causes double-strand breaks, the most dangerous kind of DNA damage. Cells can repair these breaks through a precise process called homologous recombination, which relies on key proteins such as BRCA1 and RAD51. The team showed that high SERBP1 levels led to more BRCA1 and RAD51 activity and fewer signs of unrepaired damage, whereas removing SERBP1 had the opposite effect. They discovered that SERBP1 physically binds to the messenger RNA that encodes BRCA1, protecting this RNA from being degraded. As a result, more BRCA1 protein is produced, which then helps recruit RAD51 to broken DNA and patch it up. In essence, SERBP1 acts as a stabilizing chaperone that strengthens the cell’s DNA repair crew just when cisplatin is trying to overwhelm it.
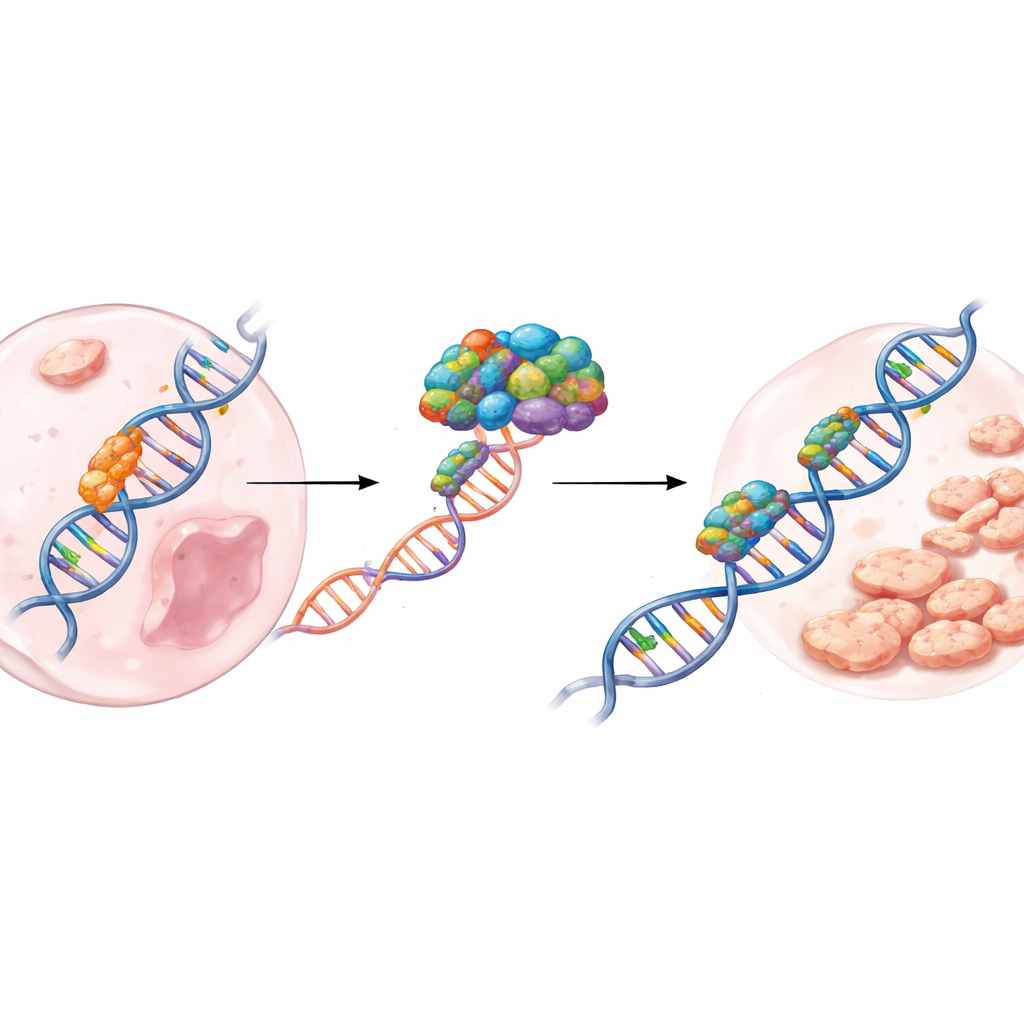
Putting the mechanism to the test in living tumors
To confirm that this pathway matters beyond cell dishes, the researchers implanted human lung cancer cells into mice. Tumors engineered to produce extra SERBP1 grew larger and were less affected by cisplatin injections than control tumors. Crucially, when they simultaneously reduced BRCA1 in these SERBP1-rich tumors, the resistance largely disappeared: the tumors shrank more, showed higher levels of DNA damage, and had fewer markers of active DNA repair. These in vivo experiments reinforced the idea that a SERBP1–BRCA1–RAD51 chain forms a central axis that allows lung adenocarcinoma cells to withstand cisplatin treatment.
What this could mean for future treatments
This work reveals SERBP1 as a key enabler of cisplatin resistance in lung adenocarcinoma by stabilizing BRCA1 RNA and boosting a powerful DNA repair pathway. For patients, the implication is twofold: SERBP1 levels might help predict which tumors will respond poorly to platinum-based chemotherapy, and drugs that block SERBP1 or disrupt its grip on BRCA1 RNA could re-sensitize resistant cancers to cisplatin. While such targeted inhibitors do not yet exist, the study provides a clear blueprint for designing therapies that disable this molecular lifeline and restore the potency of a long-standing cancer drug.
Citation: Xie, Y., Chen, Q., Tang, N. et al. SERBP1 is required for efficient HR repair and cisplatin chemoresistance in lung adenocarcinoma. Cell Death Discov. 12, 162 (2026). https://doi.org/10.1038/s41420-026-03017-x
Keywords: cisplatin resistance, lung adenocarcinoma, DNA repair, SERBP1, BRCA1