Clear Sky Science · en
Surface CD81 supports leukemia stem cell function and reveals a therapeutic vulnerability in acute myeloid leukemia
Why some leukemias keep coming back
Many people with acute myeloid leukemia (AML) respond well to initial chemotherapy, only to face the shock of the disease returning months or years later. This relapse is usually what proves fatal. The study summarized here asks a simple but urgent question: what is it about certain leukemia cells that allows them to survive powerful drugs, hide in the bone marrow, and later restart the cancer? The researchers pinpoint a small surface protein called CD81 as a key helper of these relapse‑driving cells and show that it can be turned into a weakness that new treatments might exploit.
A small docking protein with big consequences
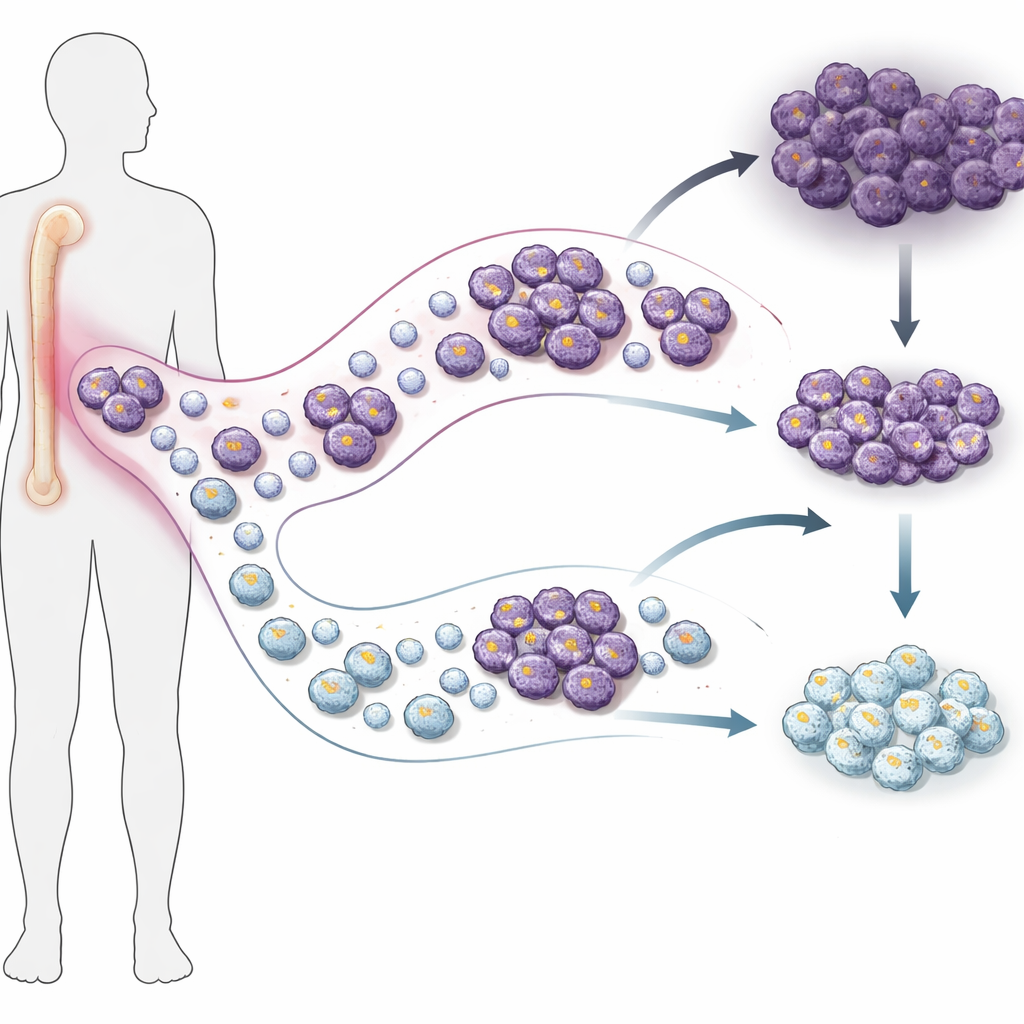
CD81 is a tiny protein that sits in clusters on the outer membrane of many immune cells, where it helps organize signaling and cell‑to‑cell contact. It has already drawn attention in some B‑cell cancers, but its role in AML was unclear. By analyzing bone marrow samples from more than 250 patients, the authors found that leukemia cells often carry much more CD81 on their surface than healthy bone marrow cells. Patients whose leukemia cells had especially high CD81 levels at diagnosis were more likely to relapse and had shorter overall survival, even when standard genetic risk factors were taken into account. This pattern held across several independent patient cohorts and was particularly striking in forms of AML that are otherwise considered to have a relatively good outlook.
How CD81 toughens leukemia cells
To move beyond correlation, the team engineered leukemia cell lines to either increase or decrease CD81 on their surface. Cells forced to overproduce CD81 became harder to kill with standard chemotherapy drugs such as daunorubicin and cytarabine, while cells in which CD81 was silenced became more sensitive. When these altered cells were injected into immunodeficient mice, high‑CD81 cells homed to the bone marrow more efficiently, spread more widely, and killed the animals faster. Low‑CD81 cells showed weaker engraftment, less tissue invasion, and allowed mice to live longer. Microscopy revealed that CD81‑rich leukemia cells extended more thin, finger‑like projections that help cells crawl, stick, and interact with their surroundings, suggesting that CD81 strengthens their grip on the protective niches of the bone marrow.
The hidden shelter of leukemia stem cells
Relapse in AML is thought to arise from a small population of leukemia stem cells—rare cells with the capacity to regenerate the disease after treatment. The researchers examined these stem‑like cells in detail using flow cytometry and single‑cell RNA sequencing. In healthy bone marrow, early blood‑forming cells displayed little CD81, but in AML, stem‑like cells and closely related progenitors showed uniformly high CD81 levels. The proportion of CD81‑positive leukemia stem cells was higher at relapse than at diagnosis and predicted both a greater risk of relapse and shorter survival. In mouse transplant experiments using patients’ leukemia samples, those with higher CD81 not only engrafted more readily but also produced larger spleens filled with leukemia cells—another sign of aggressive behavior. Molecular analyses linked CD81 to a gene called LAPTM4B and to activation of the STAT3 signaling pathway, both associated with stem‑cell programs, migration, and drug resistance.
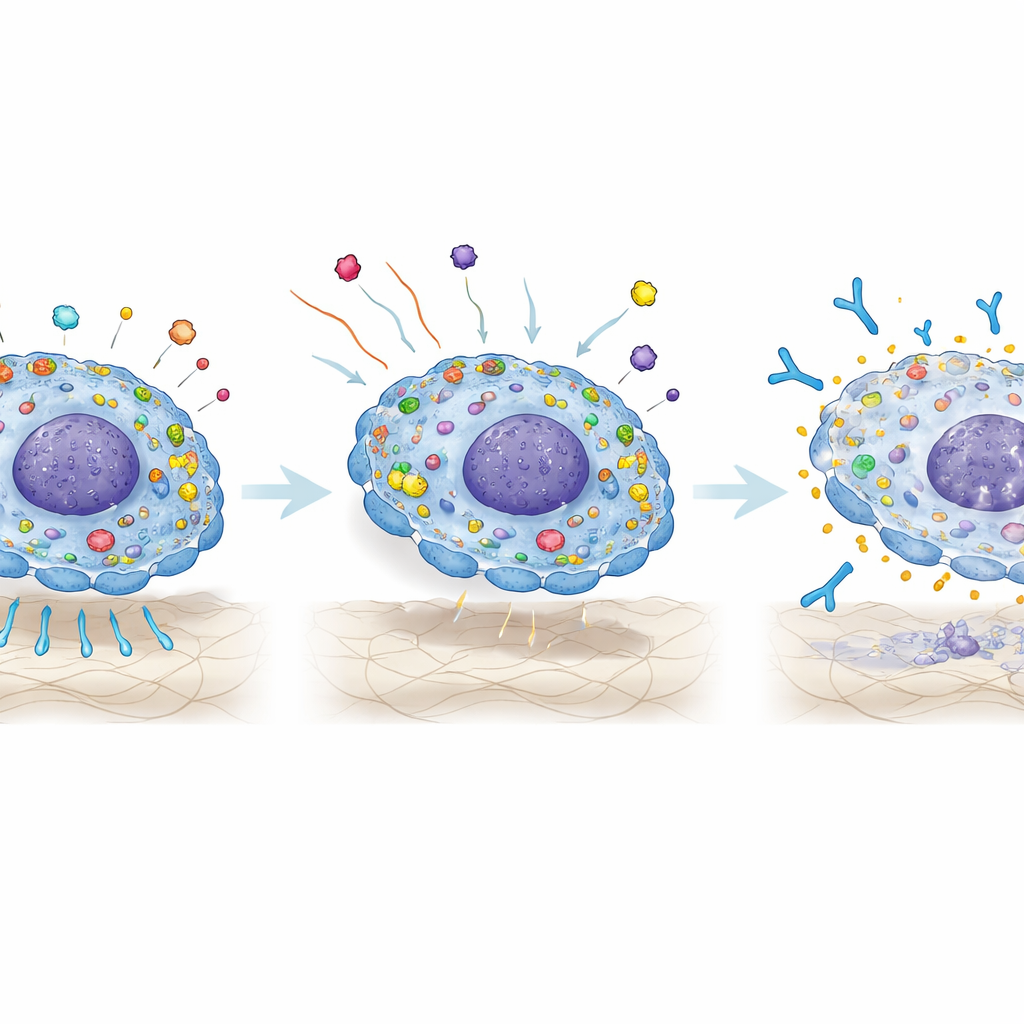
Turning a strength into a weak point
Because CD81 sits on the cell surface, it can in principle be targeted by therapeutic antibodies. The team tested an anti‑CD81 antibody in several preclinical models. Treating leukemia cell lines with this antibody reduced their ability to engraft in mice and made them more vulnerable to chemotherapy. In mouse models already bearing leukemia, combining the anti‑CD81 antibody with standard chemotherapy led to deeper remissions, fewer relapses, and longer survival than chemotherapy alone. Importantly, exposing healthy donor bone marrow cells to the antibody did not impair their survival, cell cycle, or ability to form colonies in culture, suggesting that the treatment might spare normal blood‑forming stem cells.
What this could mean for patients
Taken together, the work paints CD81 as both a marker and a driver of the most dangerous leukemia cells—the ones that seed relapse and resist treatment. By helping leukemia stem cells cling to protective bone marrow niches and activate survival pathways, CD81 makes standard drugs less effective. Yet the same surface location that makes CD81 useful to the leukemia also makes it accessible to antibody‑based therapies. While further studies are needed to confirm safety and test combinations in people, this research identifies CD81‑dependent signaling as a promising new vulnerability. Targeting it could one day improve the chances that a first successful treatment for AML is also the last.
Citation: Gonzales, F., Peyrouze, P., Laurent, D. et al. Surface CD81 supports leukemia stem cell function and reveals a therapeutic vulnerability in acute myeloid leukemia. Sig Transduct Target Ther 11, 145 (2026). https://doi.org/10.1038/s41392-026-02697-2
Keywords: acute myeloid leukemia, leukemia stem cells, CD81, chemoresistance, antibody therapy