Clear Sky Science · en
Temporal assessment of behavior in Parkinson’s visual hallucinations via a multidimensional analysis strategy
Why strange sights in Parkinson’s matter
Many people know Parkinson’s disease for its tremors and stiff movements, but up to a third of patients also see things that are not really there. These visual hallucinations can be deeply unsettling—shadowy figures, animals, or strangers in the room—and they often signal faster thinking problems and heavier care needs. Yet doctors still lack good ways to study these episodes in the lab or to measure whether new treatments actually ease them. This study introduces a new mouse model and a powerful behavior-tracking approach that together offer a more objective window into Parkinson’s visual hallucinations.
A mouse model for eerie visions
To approximate Parkinson’s disease in mice, the researchers first damaged dopamine-producing cells in a brain region that controls movement. These mice developed slower motion, weaker grip, and memory problems, much like human patients. The team then gave some of these mice a drug called benzhexol, an anticholinergic medicine sometimes prescribed for Parkinson’s tremor that is known, at high doses, to trigger hallucinations in people. In the treated mice, a curious pattern emerged: soon after each dose, they began to show abnormal head twitches and long, fixed stares, hinting at an altered internal experience.
Reading hidden signals in posture and motion
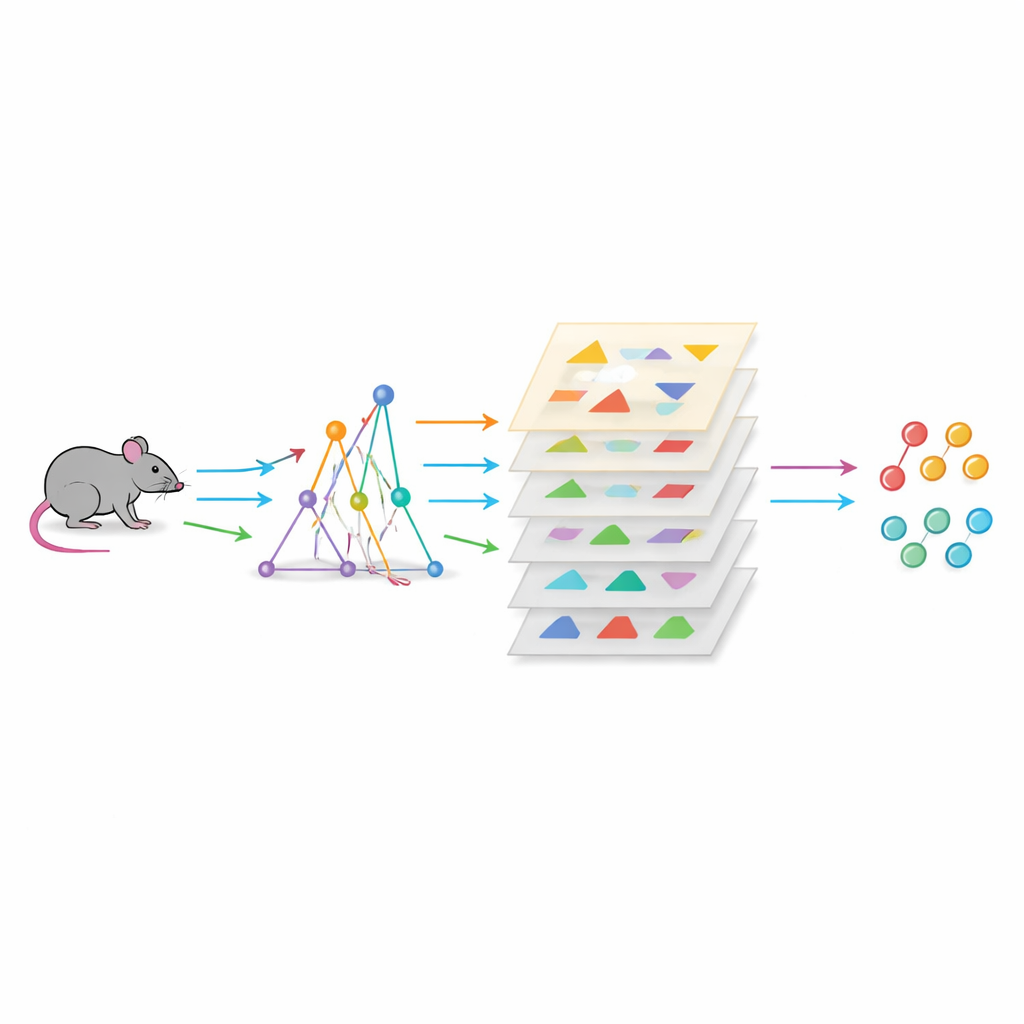
Rather than judging these behaviors by eye alone, the authors used a three-dimensional motion-capture system and machine learning to record every movement of freely moving mice over time. They decomposed the animals’ activity into dozens of repeatable movement “modules,” then asked which ones changed with Parkinson’s damage and with benzhexol. Two movement types stood out in the drug-treated animals: a sustained hunching posture paired with intense staring, and a similar hunching state peppered with rapid head twitches. Together, these formed what the team called a “hallucination-related hunching state,” a longer-lasting posture within which briefer twitch and stare events were embedded.

Behavior as a structured sequence, not random noise
Next, the researchers looked at how one behavior flowed into another, building maps of transition probabilities between the different movement types. The benzhexol-treated mice showed fewer shifts into routine “maintenance” behaviors, such as grooming, and more shifts into a kind of defensive stillness. Overall, their behavior patterns became more predictable and less random, as measured by information-theory tools. Simple counts of head twitches or stares could already distinguish “hallucinating” from non-hallucinating mice fairly well, but combining these with the transition patterns produced near-perfect separation. In other words, it was not just what the mice did, but when and in what order, that best captured the hallucinatory state.
Timing the rise and fall of an episode
To track how hallucination-like states evolved minute by minute, the authors divided each recording into 10‑second windows and measured how often the hunching states appeared in each slice. In benzhexol-treated mice, these episodes surged early after dosing and then waned in a consistent pattern; in untreated Parkinson’s mice, they were rare and irregular. By pairing behavior analysis with recordings of calcium activity—a proxy for firing—in specific prefrontal brain cells, the team found that longer hunching bouts were linked to reduced activity in these neurons. This suggests that the duration of a posture carries information about the underlying brain state, not just the presence or absence of a movement.
Matching brain changes and testing a real drug
The study went further to check whether the mouse model resembled human Parkinson’s hallucinations at the brain level. The benzhexol-treated mice showed increased activation in vision-related cortex and prefrontal regions, echoing imaging studies in patients who see vivid images. Single-cell RNA sequencing of mouse brain tissue revealed gene activity patterns that closely matched those seen in the midbrain of people with Parkinson’s hallucinations, and were distinct from patterns caused by the anesthetic ketamine, another hallucinogenic drug. Finally, when the researchers treated the mice with pimavanserin, a drug already approved for Parkinson’s psychosis, the hallmark hunching, staring, and twitching behaviors were markedly reduced, and the altered transition patterns moved back toward normal.
What this means for patients and future treatments
For people living with Parkinson’s, strange visions are more than a curiosity—they are a warning sign that the disease is affecting perception and thinking. This work offers a way to capture that invisible experience objectively in animals, by reading subtle changes in posture, gaze, and behavioral flow. By tying these patterns to specific brain circuits and gene programs, and by showing that a known antipsychotic drug can normalize them, the study lays groundwork for testing new therapies and for understanding why some Parkinson’s patients see ghosts in the shadows while others do not.
Citation: Zhang, QX., Zhang, YX., Jiang, CC. et al. Temporal assessment of behavior in Parkinson’s visual hallucinations via a multidimensional analysis strategy. Sig Transduct Target Ther 11, 146 (2026). https://doi.org/10.1038/s41392-026-02651-2
Keywords: Parkinson’s visual hallucinations, animal behavior analysis, anticholinergic drugs, pimavanserin, mouse models of psychosis