Clear Sky Science · en
Modifiable PEDOT:PSS-based flexible diagnostic and therapeutic dressings for personalized wound management
Smart Bandages for Faster Healing
Chronic and hard‑to‑heal wounds are a growing problem worldwide, especially for people with diabetes, poor circulation, or repeated infections. Traditional gauze and ointments protect the skin, but they cannot “see” what is happening underneath or actively guide the healing process. This study introduces a new kind of flexible smart bandage that not only watches key signals from a wound but also gently treats it with electricity and light, speeding up repair in animal tests.
Why Wounds Need Smarter Care
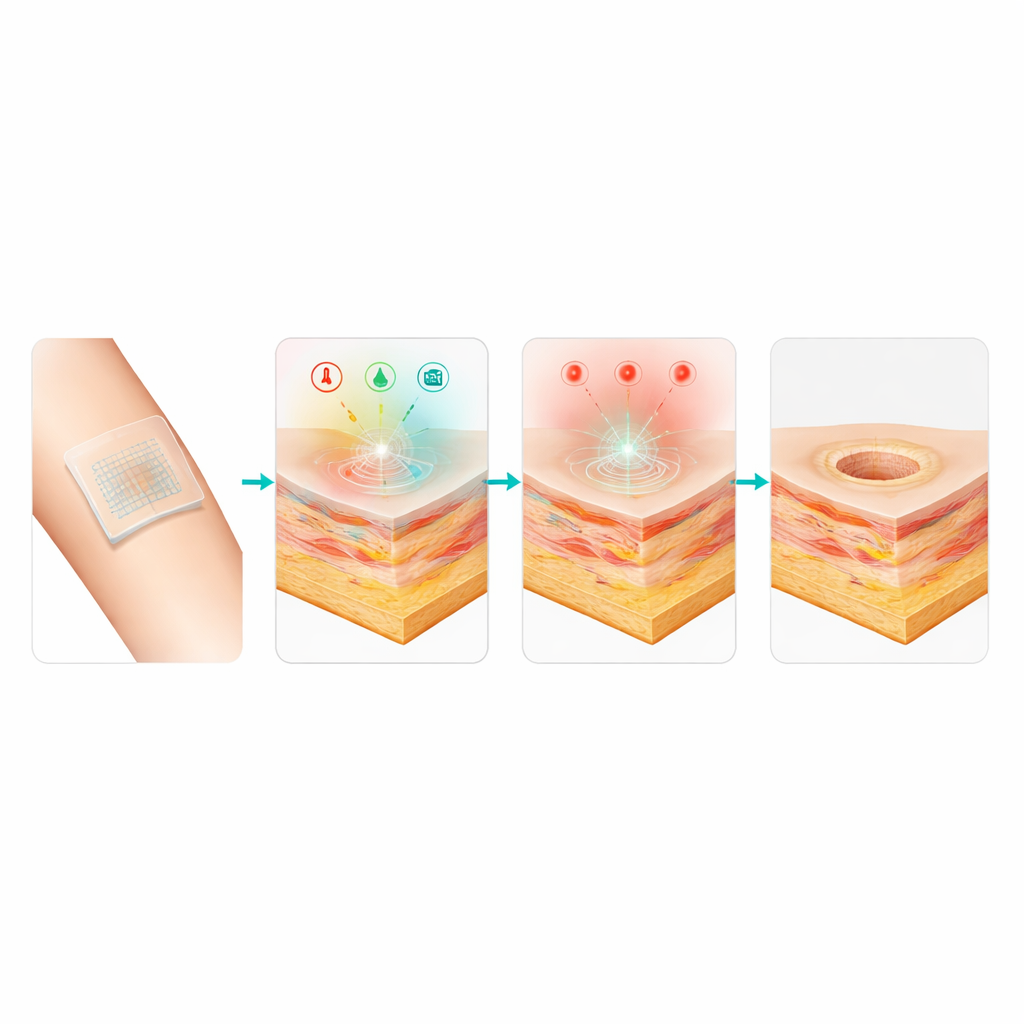
Healthy skin repairs itself through a careful sequence of inflammation, tissue growth, and remodeling. In difficult wounds, this sequence can stall because of infection, imbalanced chemistry, or poor blood supply. Three simple clues can reveal how well a wound is doing: temperature, moisture, and acidity. A hotter wound may signal infection; changes in electrical resistance can reflect how wet or dry the tissue is; and a shift from mildly acidic toward alkaline often accompanies chronic inflammation. At the same time, gentle electric fields and red light are already known, separately, to help cells move, divide, and form new blood vessels. The challenge has been to combine continuous monitoring with these physical therapies in a soft, comfortable dressing that conforms to moving skin.
A Single Soft Film That Does It All
The team solved this by building the entire electronic layer of the dressing from a tunable plastic conductor called PEDOT:PSS. By adding specific additives in two steps, they could adjust how well this thin film carries electricity over a very wide range while keeping it flexible and skin‑friendly. Lower‑conductivity regions serve as sensitive temperature elements, while higher‑conductivity regions form electrodes and connections for measuring moisture and acidity and delivering electrical stimulation. A tiny red light source for phototherapy is embedded alongside these structures. All of this is sandwiched between breathable medical tape layers with a total thickness of only about 60 micrometers—thinner than a human hair—so it bends and twists easily with the body.
Listening to the Wound in Real Time
Inside this soft stack, three kinds of sensors continuously track the wound environment. One traces resistance changes as skin warms or cools, allowing small shifts in temperature to be detected. A second pair of electrodes senses how easily current flows through a moist sponge‑like layer that mimics wound fluid; this reflects changing moisture levels as the wound weeps and then dries. A third sensor, coated with a pH‑responsive layer, reads out acidity as an electrical signal. In tests, all three sensors responded in a straight‑line, predictable way across medically important ranges, and their readings were stable over repeated cycles. The dressing is powered wirelessly by a thin receiving coil and tiny rechargeable battery, and it sends data by Bluetooth, so animals wearing it could move freely while their wounds were monitored.
Guiding Skin Repair with Electricity and Light
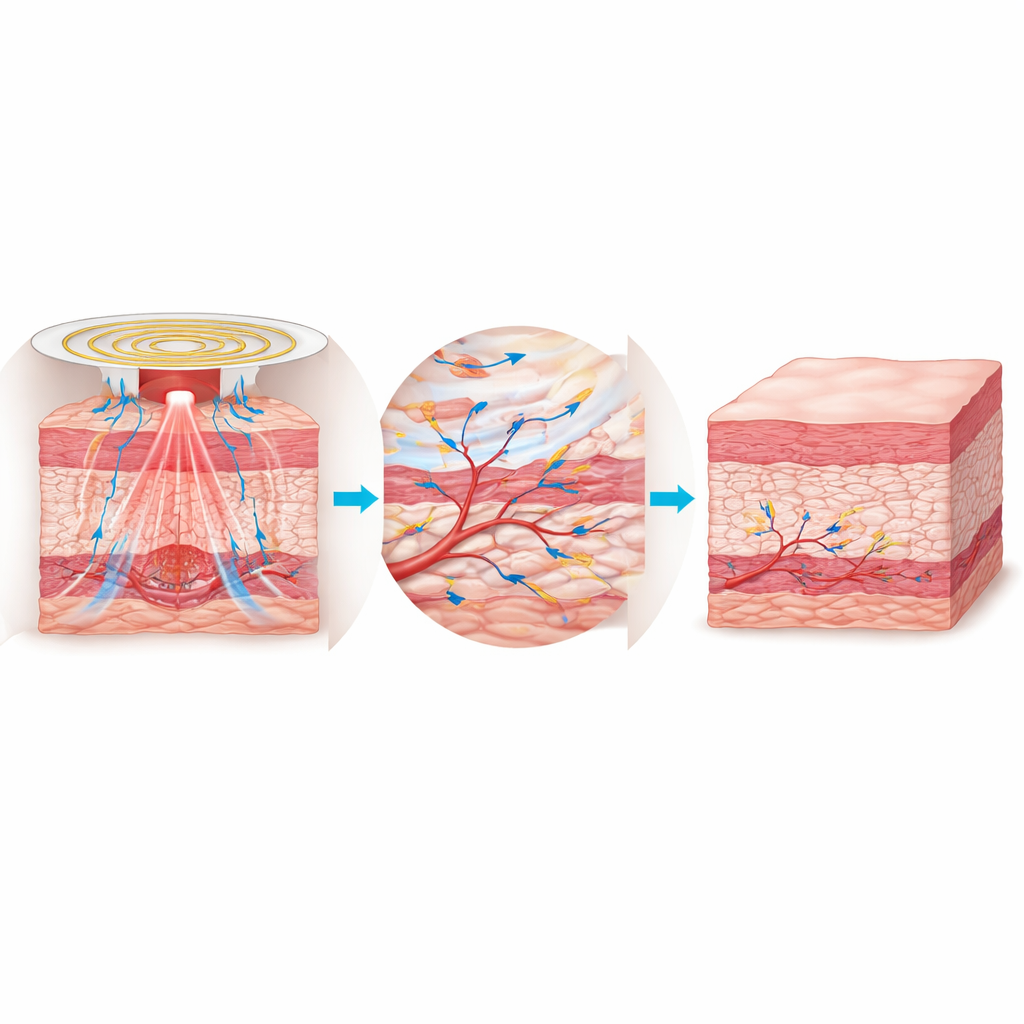
Beyond monitoring, the dressing actively helps wounds to close. Concentric electrodes deliver low‑level electrical stimulation that imitates natural signals seen at the edges of skin injuries and encourages cells to migrate into the gap. At the same time, a small red light source shines into the tissue, boosting energy production in cell “power plants” and easing harmful oxidative stress. In rat models with square and circular full‑thickness wounds, daily one‑hour sessions with both treatments combined led to about 99% closure after eight days, clearly ahead of dressings that provided only electricity, only light, or no active treatment. Microscopic examination showed that the combined therapy group had more complete new skin layers, denser and better‑organized collagen fibers, and richer networks of tiny blood vessels.
From Laboratory Patch to Personalized Care
By uniting sensing and therapy in a single soft, metal‑free film, this smart bandage acts like a miniaturized clinic directly on the skin. It can watch over the temperature, moisture, and acidity of the wound in real time, then deliver finely tuned electrical and light stimulation that together spur cell growth, blood vessel formation, and tissue remodeling. While these results are still in animals, the work points toward future dressings that could automatically adjust treatment to each person’s wound, helping stubborn injuries heal faster and with fewer complications.
Citation: Wang, L., Yao, G., Cai, S. et al. Modifiable PEDOT:PSS-based flexible diagnostic and therapeutic dressings for personalized wound management. Microsyst Nanoeng 12, 148 (2026). https://doi.org/10.1038/s41378-026-01200-9
Keywords: smart wound dressing, flexible bioelectronics, electrical stimulation therapy, photobiomodulation, chronic wound healing