Clear Sky Science · en
Deep learning-enhanced dual-mode multiplexed optical sensor for point-of-care diagnostics of cardiovascular diseases
Why testing the heart quickly matters
When someone shows up with chest pain or trouble breathing, doctors have only a short window to tell whether the heart is having a crisis. Today, key blood tests for heart attack and heart failure are often slow, require large machines, and usually measure just one signal at a time. This paper describes a small, low-cost device that can sit near the patient, read several heart-related blood markers from a single tiny sample, and use artificial intelligence to turn faint optical signals into clear numbers that doctors can use.
Two common heart problems, one tangled story
Heart attacks and heart failure are among the leading killers worldwide and are closely linked. A heart attack suddenly cuts off blood to part of the heart muscle, while heart failure develops when the heart can no longer pump efficiently. Many patients suffer from both, which greatly increases their risk of death and repeat hospital visits. Doctors rely on three main blood markers to understand what is happening: cardiac troponin I, which signals damage to heart muscle cells; creatine kinase-MB, which helps spot a fresh or repeat injury; and NT-proBNP, which rises when the heart is stretched and struggling to pump. Measuring these three together gives a much fuller picture of a patient’s condition than any single test alone.
Limits of today’s lab and bedside tests
Current systems for measuring these markers are split between large central laboratories and smaller point-of-care devices. Big analyzers in hospital labs are sensitive and reliable, but they need skilled staff, separate cartridges and reagents for each marker, and relatively large blood volumes. Results can take hours, which clashes with the narrow treatment window for heart attacks and makes frequent follow-up testing burdensome, especially for people living far from major centers. Existing bedside devices are faster but typically test only one marker per cartridge, often lack the extreme sensitivity now recommended for troponin, and struggle to cover the very different concentration ranges of the three markers without interference or loss of accuracy.
A paper-based cartridge that sees in two ways
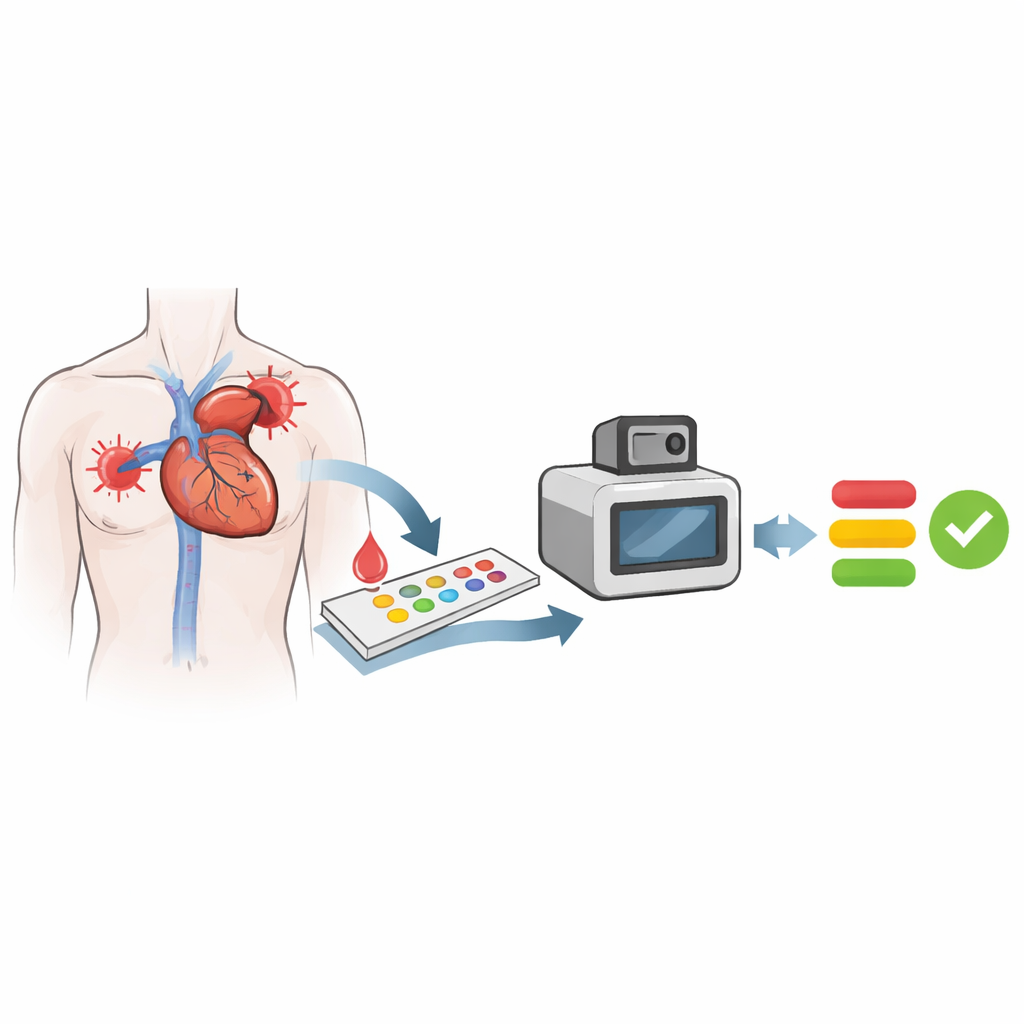
The researchers built a palm-sized optical sensor platform around a paper-based "vertical flow" cartridge. A drop of serum mixed with special nanoparticle-tagged antibodies is pulled straight down through a small membrane dotted with tiny reaction spots: some catch troponin, some catch NT-proBNP, some catch CK-MB, and others serve as built-in controls. The same cartridge is then read in two optical modes. In colorimetric mode, gold nanoparticles make certain spots darker under green light. In chemiluminescent mode, an added chemical makes enzyme-tagged complexes glow in the dark. By assigning low-abundance troponin to the glow mode and the higher-abundance markers mainly to the color mode, the device cleanly spans concentrations from less than a trillionth of a gram per milliliter to tens of billionths, all within one test that takes about 23 minutes and uses only 50 microliters of serum.
Teaching a small computer to read complex patterns
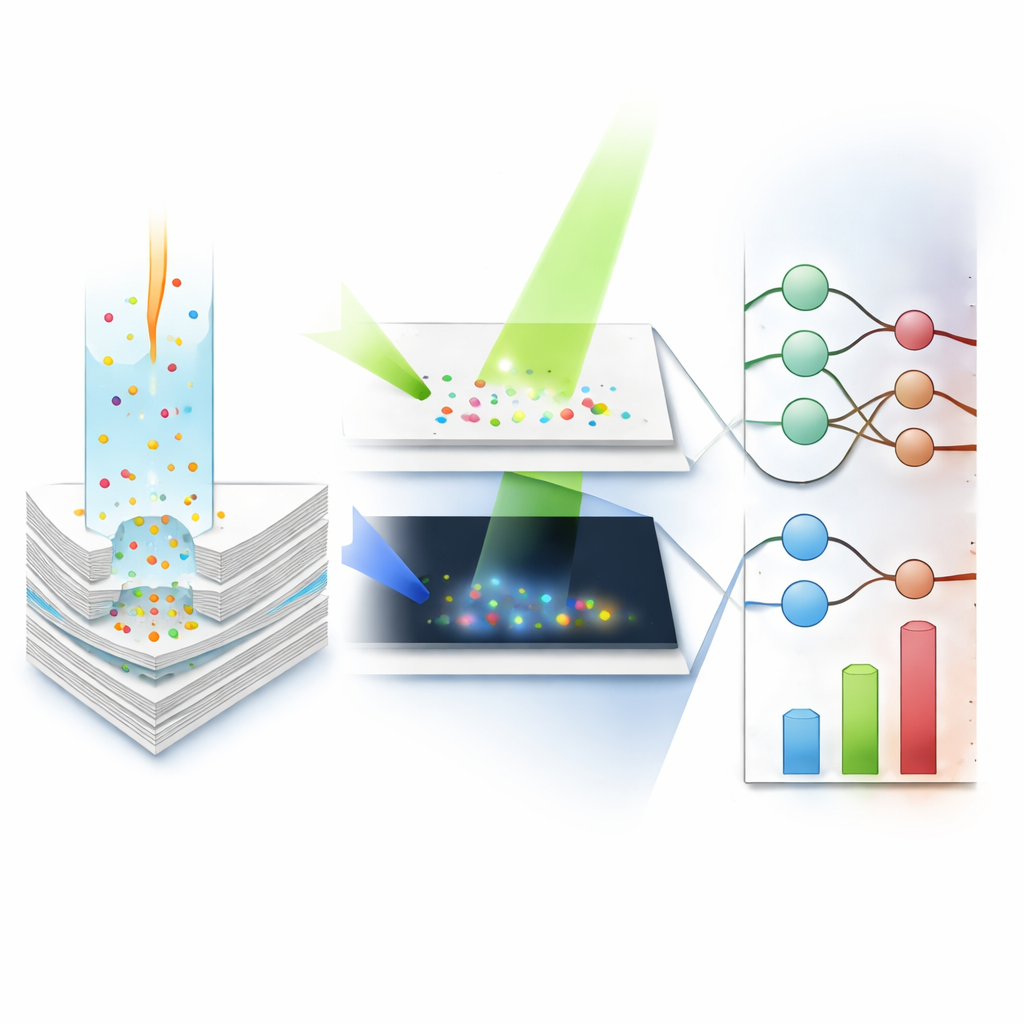
Because paper flow, sample composition, and other factors can subtly change the raw signals, the team turned to compact neural networks—software models inspired by brain circuitry—to interpret the images. A Raspberry Pi-based reader captures both color and glow images and extracts the brightness of each spot and control. For each marker, a first network quickly places the result into a broad range (for example, below or above a heart-failure threshold), and a second network then estimates the exact concentration within that range. The system cross-checks these steps; if the range and value disagree, the result is flagged as undetermined instead of silently reporting a suspect number. Trained and then tested on 92 real patient serum samples, the models’ outputs matched standard hospital assays very closely, with correlation values above 0.96 for all three markers.
What this could mean for everyday care
In practical terms, this work shows that a low-cost, handheld reader and disposable paper cartridge can deliver lab-grade, multi-marker heart testing at the bedside or in small clinics. The dual optical modes allow extremely low troponin levels and very high values to be measured within a single run, while the neural networks help correct for noise and variability that would otherwise weaken a simple one-signal-per-marker approach. Although further, larger clinical studies and whole-blood tests are still needed, this platform points toward a future where people at risk for heart attack or heart failure can be assessed, monitored, and triaged rapidly and affordably in many more settings than today.
Citation: Han, GR., Eryilmaz, M., Goncharov, A. et al. Deep learning-enhanced dual-mode multiplexed optical sensor for point-of-care diagnostics of cardiovascular diseases. Light Sci Appl 15, 190 (2026). https://doi.org/10.1038/s41377-026-02275-9
Keywords: cardiac biomarkers, point-of-care diagnostics, chemiluminescent sensors, deep learning, heart attack and heart failure