Clear Sky Science · en
Haploidentical versus matched unrelated donor transplantation with post-transplant cyclophosphamide: a platform-dependent machine learning analysis of donor age
Why Donor Age Matters for Life-Saving Transplants
For adults with aggressive blood cancers like leukemia, a stem cell transplant from a healthy donor can be the difference between life and death. But when no perfectly matched sibling is available, doctors must choose between a partially matched family member and a fully matched stranger from a registry. These two options often come with very different donor ages. This study asks a simple but crucial question: how much does the donor’s age really matter, and does it matter differently depending on which transplant route is chosen?
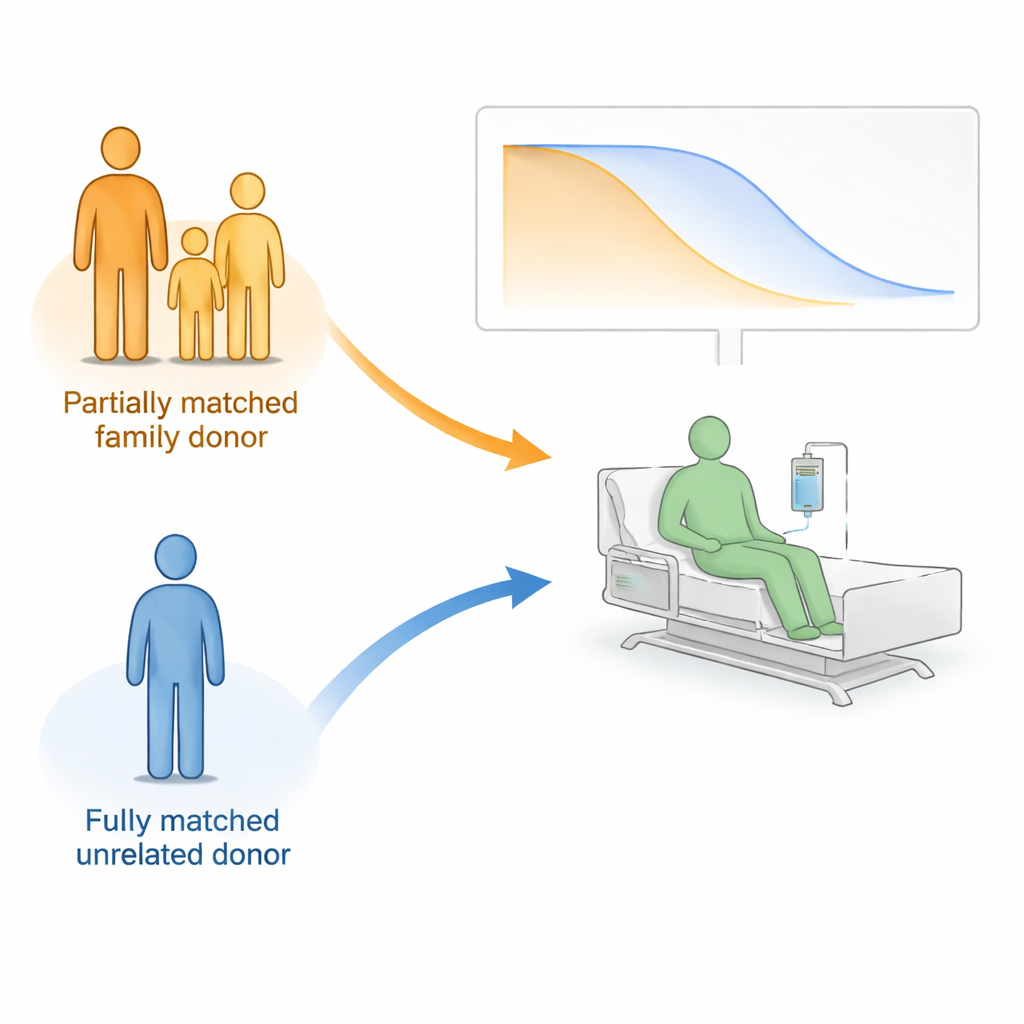
The Two Main Paths to a Donor
Modern transplants increasingly rely on a drug called post-transplant cyclophosphamide (PTCy) to control dangerous immune reactions after the graft. In this PTCy era, patients usually face two main donor choices. One is a “haploidentical” donor—typically a parent, child, or sibling who is only a half-match genetically but often easy to find quickly in the family. The other is a fully matched unrelated donor found through international registries. The trade-off is clear: the family donor is often older and only partly matched, while the registry donor may be younger but harder to locate in time, especially for patients from minority backgrounds.
How the Researchers Studied Risk
The researchers analyzed records from 4,258 adults with acute leukemia who received their first transplant between 2017 and 2021, all using PTCy. Over 3,000 received a haploidentical transplant, and about 1,100 received a fully matched unrelated donor transplant. Instead of relying only on traditional statistics, the team used machine learning methods—random survival forests and deep neural networks—to explore how donor age shapes survival in a flexible, data-driven way. They then cross-checked these results with several robust regression techniques designed to balance differences between the two donor groups, such as disease risk and patient health status at the time of transplant.
Donor Age Affects Each Pathway Differently
The central finding is that donor age does not behave the same way in both transplant approaches. In the haploidentical group, the risk of death steadily climbed as donor age increased. The models showed that using a donor in the late 30s already crossed a meaningful risk threshold: for every 100 patients switched from an 18-year-old donor to such an older haploidentical donor, about one extra patient would be expected to die within two years. As donor age moved into the 40s and beyond, this penalty grew faster, costing more survival time. By contrast, the fully matched unrelated donor platform appeared strikingly resilient. The added risk from donor aging stayed minimal for donors up to about 50 years old, with survival curves remaining almost flat over this range.
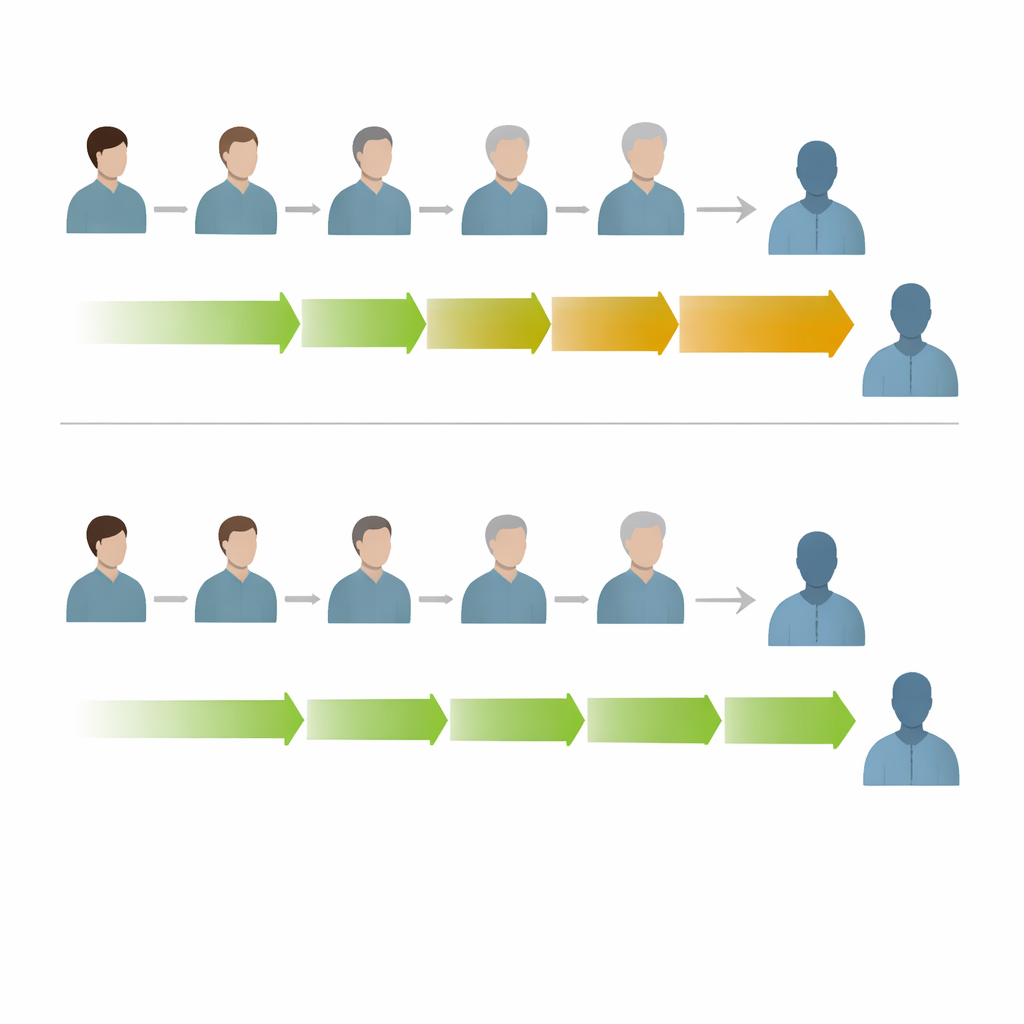
Turning Complex Models into Practical Choices
To make these patterns clinically useful, the team translated model outputs into numbers doctors can act on. They calculated “number needed to harm” (how many patients would have to receive an older donor to cause one extra death) and “restricted mean survival time” (how many days of life are lost over two years). In haploidentical transplants, donor age beyond the mid-30s quickly reduced average survival by days to weeks, especially when the donor was much older than the ideal young reference. Yet the authors also stress that small age differences—say, a few years between candidate family donors—are unlikely to matter much. Heatmaps that combined both patient and donor ages showed that, across most age pairings, fully matched unrelated donors offered a modest but consistent survival edge, largely driven by less chronic graft-versus-host disease and lower non-relapse mortality.
What This Means for Patients and Policy
To a layperson, the takeaway is that a well-matched stranger’s cells hold up surprisingly well to the wear and tear of aging—at least into the late 40s—when modern PTCy protection is used. Haploidentical family donors, while vital and often the only option, become more risky as they age, particularly once they reach their late 30s and 40s. Overall, the study supports choosing a fully matched unrelated donor whenever feasible, even if that donor is not especially young, and suggests that current rules that reject older registry donors may be overly strict. By quantifying exactly how donor age and donor type interact, this work offers doctors and patients a clearer, more personalized roadmap for making one of the most important treatment decisions they will ever face.
Citation: Mehta, R.S., Kanakry, C.G., Nawas, M. et al. Haploidentical versus matched unrelated donor transplantation with post-transplant cyclophosphamide: a platform-dependent machine learning analysis of donor age. Leukemia 40, 1009–1017 (2026). https://doi.org/10.1038/s41375-026-02903-8
Keywords: stem cell transplantation, donor age, haploidentical donors, matched unrelated donors, machine learning in medicine