Clear Sky Science · en
Patient-reported experiences with silicon-based prosthetic solutions and surgical options following thumb amputation
Living with a Missing Thumb
Most of us don’t think about our thumbs until something happens to them. Yet the thumb is central to opening jars, using a phone, and doing countless tasks at work. This study looks at what life is really like for people who have lost a thumb and received modern silicone-based prosthetic thumbs. Rather than focusing only on surgical techniques or mechanical details, the researchers listened closely to how patients themselves describe their daily lives, their jobs, and how they feel about their bodies after injury.
Why the Thumb Matters in Everyday Life
The thumb normally provides up to half of the hand’s usefulness, so losing it after an accident can be a major shock, physically and emotionally. Standard medical thinking emphasizes complex reconstruction surgeries or carefully crafted silicone thumbs to restore both appearance and function. But there has been little research on how people actually use these devices once they go home. This study followed 28 adults who had an isolated thumb amputation and were fitted with one of three main prosthetic options: a realistic silicone thumb, a brace-like device with a rigid thumb, or a small protective cap over the stump.
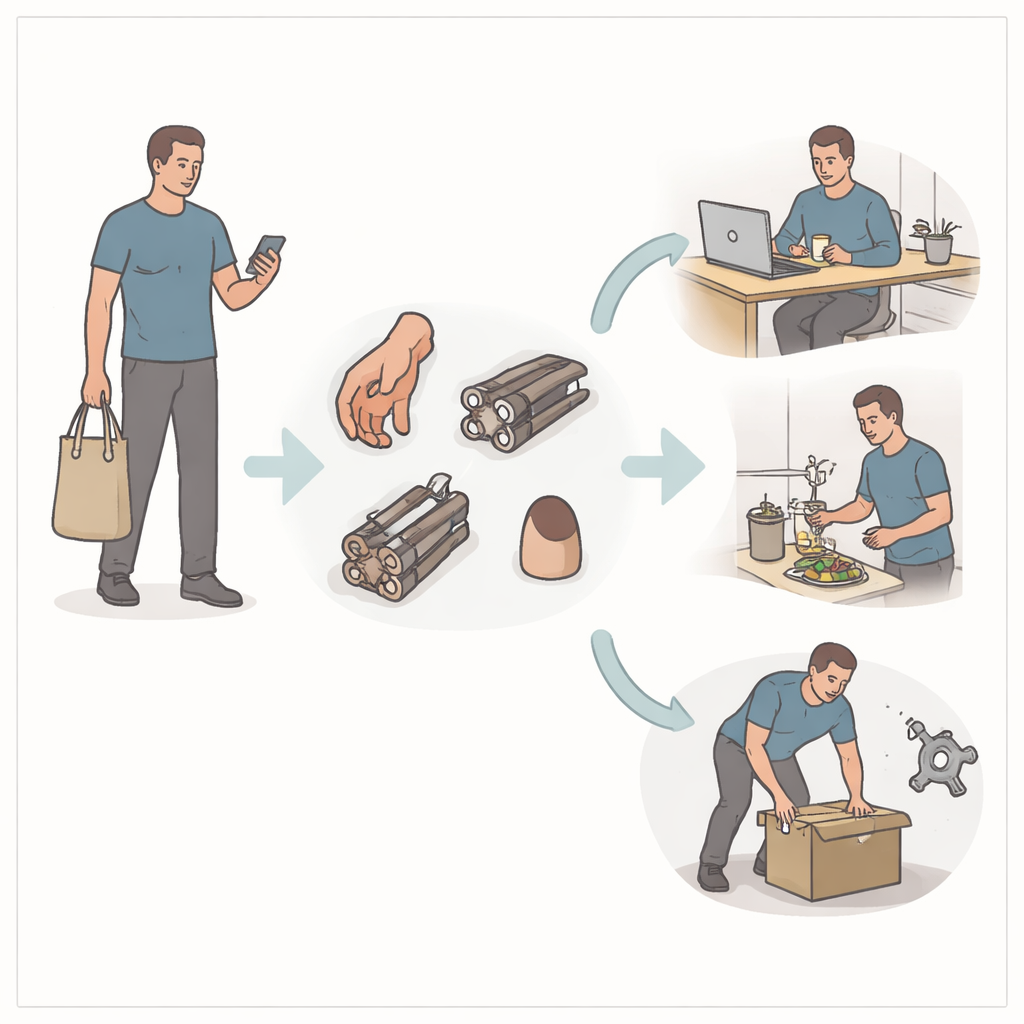
What Patients Say About Daily Tasks and Work
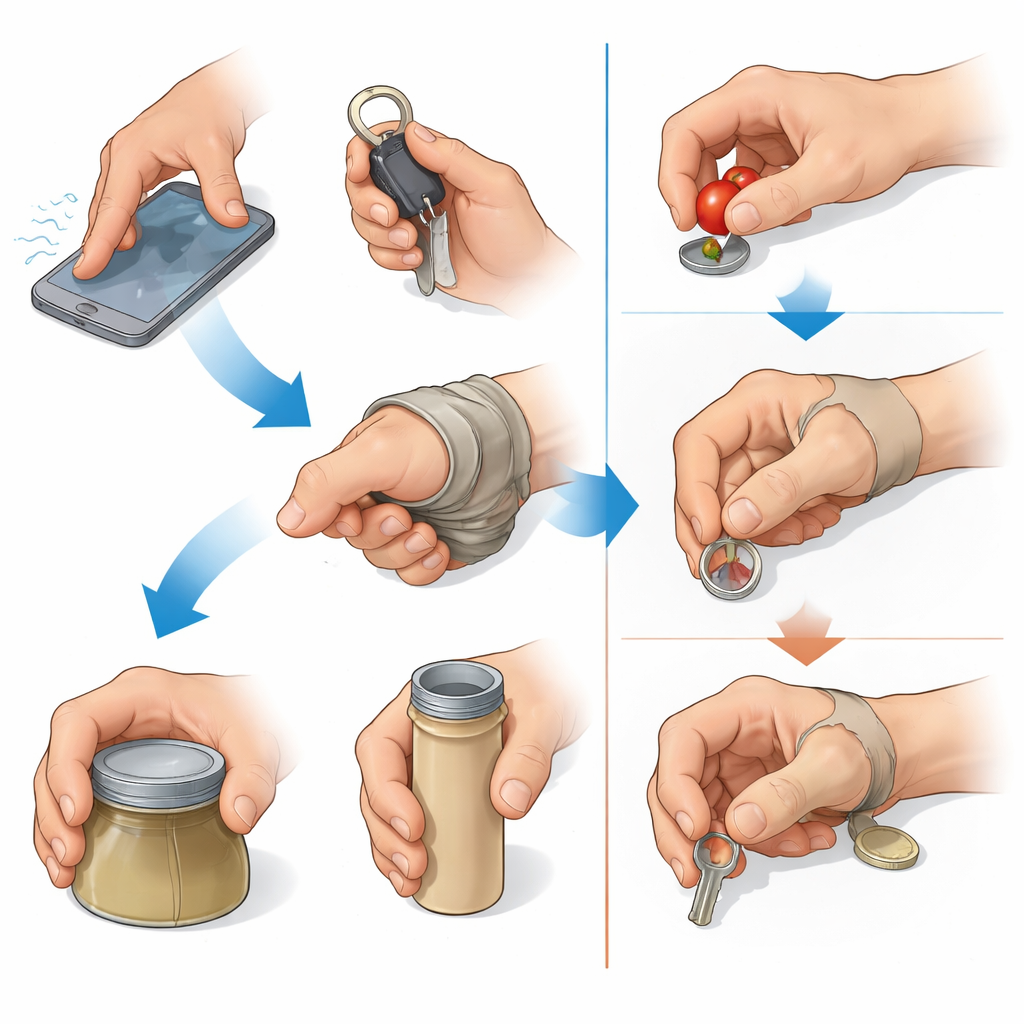
Surprisingly, most participants reported they could manage daily activities such as dressing, cooking, and using smartphones without regularly wearing a prosthesis. Nearly four out of five said they never used their device in everyday life, often explaining that the artificial thumb slipped, felt awkward, or took too long to put on. For many, the benefit was mostly cosmetic: they appreciated that the silicone thumb looked natural but did not feel it helped them actually grasp or hold objects better. In contrast, work life was much harder to adapt to. More than half of those in industrial or manual jobs could not return to their previous roles, even if they coped fairly well at home.
How Feelings, Pain, and Amputation Level Shape Choices
The researchers also explored how emotions, pain, and the exact location of the amputation influenced adaptation. People who lost only the tip or middle part of the thumb tended to adjust more quickly and were more likely to use a prosthesis at least sometimes. Those with more extensive loss closer to the hand often reported stronger emotional strain and were less inclined to wear a device. Many patients described a process of gradually accepting their changed hand, sometimes with the help of family support, while a sizeable minority struggled with worries about how others see them or disappointment about past surgeries. Pain levels varied: some lived with ongoing stump or phantom pain, but pain itself was rarely the main reason for not using a prosthesis.
Balancing Aesthetics, Function, and Further Surgery
Because silicone prostheses restore appearance but not sensation, some patients viewed them as more of a cosmetic glove than a true tool. A simple thumb cap, which protects the stump while preserving remaining feeling, was used more often than more elaborate silicone thumbs. When asked about additional surgery, such as advanced reconstructions or osseointegration (anchoring a prosthetic directly to bone), most people declined. They felt they had already adapted, feared new complications, or could not afford the time away from work. Still, among those whose injuries made them good candidates for bone-anchored prostheses, many were open to this idea, especially if it promised more stable and useful function than their current devices.
What This Means for Future Care
The study’s central message is that life after thumb loss is more complex than simply replacing what was removed. Patients often learn to handle everyday tasks without a prosthesis, yet still face serious limits at work. Silicone thumbs are valued mainly for how they look, not for how they work. As a result, many people leave them in a drawer. For a layperson, the takeaway is that successful care must look beyond technology alone. Future solutions need to be easier to use, more truly helpful in demanding jobs, and better aligned with how people feel about their bodies. Just as important, emotional support and counseling should be part of rehabilitation so that appearance, function, work demands, and self-image are all addressed together.
Citation: Prahm, C., Kefalianakis, L., Heinzel, J. et al. Patient-reported experiences with silicon-based prosthetic solutions and surgical options following thumb amputation. Humanit Soc Sci Commun 13, 328 (2026). https://doi.org/10.1057/s41599-026-06842-8
Keywords: thumb amputation, silicone prosthesis, patient experience, hand function, osseointegration