Clear Sky Science · en
Updates in the English Diabetic Eye Screening Programme
Why this matters for people with diabetes
For many people living with diabetes, losing eyesight is one of the most feared complications. The English Diabetic Eye Screening Programme (DESP), running since 2003, has already helped cut rates of blindness by catching damage early. But with the number of people with diabetes rising sharply and hospital eye clinics under pressure, the programme itself must evolve to stay effective and sustainable. This article explains how DESP is being updated so it can keep protecting vision while making better use of limited staff, time and technology.
From yearly checks to smarter timing
Until recently, everyone with type 1 or type 2 diabetes in England was invited for eye screening every year. At each visit, eye drops are used to widen the pupils and photographs are taken of the back of the eye. Trained graders then look for signs of diabetic retinopathy (damage to the light-sensitive retina) and maculopathy (changes near the central area needed for sharp vision). Studies involving hundreds of thousands of people have shown that those with completely normal eye results on two visits in a row have a very low chance—less than 1% over two years—of progressing to sight-threatening disease. Based on this evidence, DESP has begun moving some of these low-risk individuals to screening every two years rather than every year.
Balancing safety and fairness
Extending the gap between eye checks raises understandable worries about delayed diagnosis. Research from a more ethnically diverse screening programme suggested that, for some people—particularly those from Black and South Asian communities and younger individuals—a two-year recall could postpone the discovery of serious changes by a year. The article stresses that national and local programmes must monitor these groups closely to avoid widening health inequalities. Certain higher-risk situations are already excluded from the longer interval: pregnant women follow a separate, more frequent schedule, and people with type 1 diabetes starting insulin pumps remain on annual screening at first because rapid improvements in blood sugar control can temporarily worsen eye disease.
Sorting moderate from severe eye damage
Another key update is a more detailed splitting of one of the traditional grading steps used to describe the severity of retinopathy. Previously, a broad middle category called R2 covered a wide range of "pre-proliferative" changes—signs that blood vessels in the retina are becoming more damaged but have not yet grown the fragile new vessels linked to sudden sight loss. The new system divides this into low-risk (R2L) and high-risk (R2H). R2H corresponds to more extensive bleeding and vessel changes that carry almost a 50% chance of progressing to advanced disease within five years. People in this group are referred to hospital eye services for specialist review. Those with R2L, however, can stay within DESP, being followed more closely in special surveillance clinics rather than automatically swelling hospital waiting lists.
Using 3D scans to focus hospital referrals
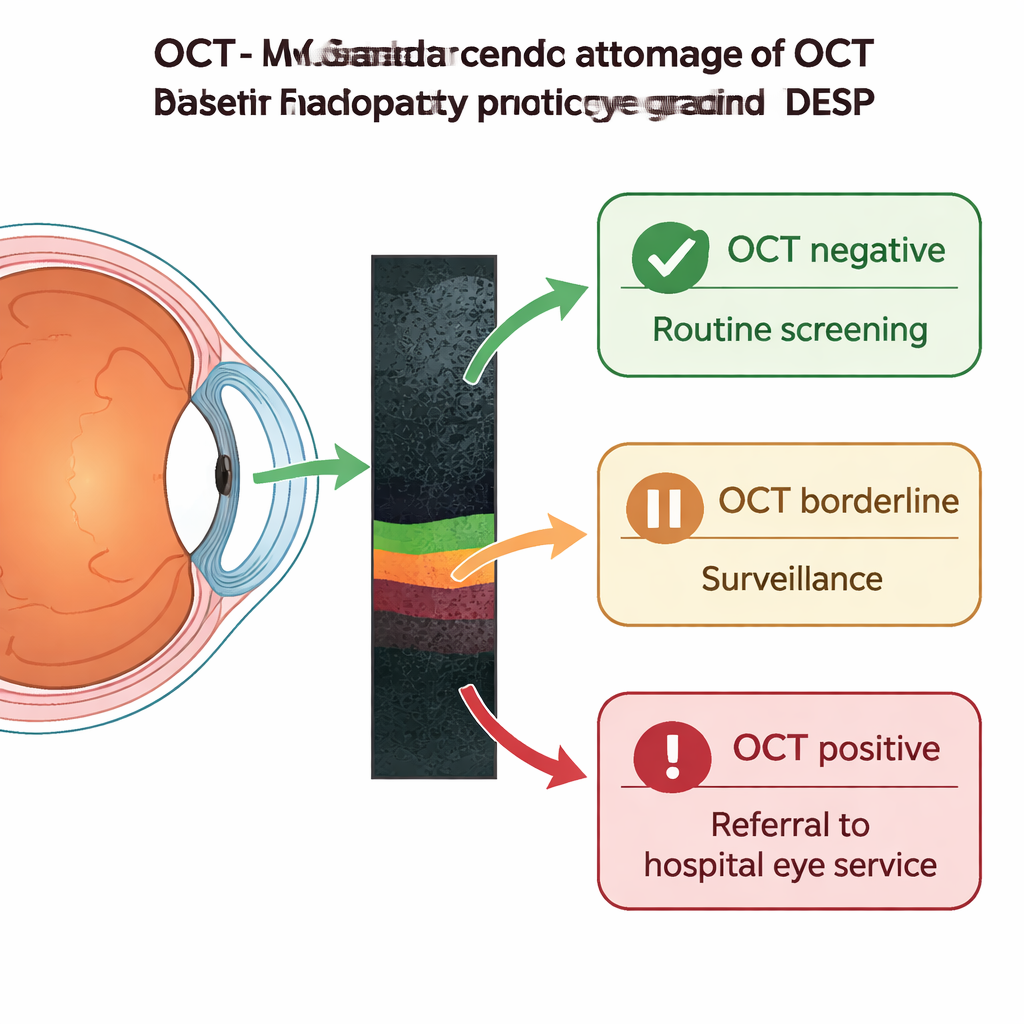
Changes around the eye’s central point of vision (the macula) have long been grouped into a single category called M1, which triggered referral to hospital even when the risk of sight loss was low. The article describes how new optical coherence tomography (OCT) scanning—essentially a painless, 3D cross-sectional image of the retina—is being built into DESP to refine this. Now, anyone given an M1 grade is routed to an OCT clinic within the screening service. The scan is then classified as OCT negative, borderline or positive. OCT-negative cases, where no meaningful thickening or cysts are seen, can safely return to routine digital screening. Borderline scans stay in the OCT surveillance pathway for repeat checks, while OCT-positive scans—showing significant swelling or shape changes at the centre of vision—are referred on to hospital eye clinics for possible laser or injection treatments. This triage also allows urgent non-diabetic problems spotted on OCT, such as age-related macular degeneration, to be fast-tracked.
What these changes mean going forward
Taken together, these updates aim to free up capacity where the risk is low and concentrate specialist attention where the risk of sight loss is highest. Two-yearly screening for people with repeatedly normal eyes reduces unnecessary visits, while refined grading and OCT-based pathways keep many moderate cases safely under the wing of the screening programme instead of overwhelming hospital clinics. At the same time, hospitals will increasingly see only patients with more advanced or complex disease, who need timely face-to-face care and treatment. The author notes that these improvements depend on proper training, quality checks and careful monitoring for unfair gaps in care. For people with diabetes, the message is clear: eye screening remains essential, but behind the scenes it is becoming smarter, more targeted and better equipped to protect sight in the long term.
Citation: Mann, S.S. Updates in the English Diabetic Eye Screening Programme. Eye Open 2, 7 (2026). https://doi.org/10.1038/s44440-026-00014-y
Keywords: diabetic eye screening, diabetic retinopathy, OCT imaging, vision loss prevention, public health programmes