Clear Sky Science · en
Two-to-three-year effectiveness and safety of nurse-led accelerated corneal crosslinking for progressive keratoconus: The Birmingham and Midland Eye Centre Study
Protecting Sight in Young People
Keratoconus is a disease that makes the clear front window of the eye, the cornea, become thinner and bulge forward. This can blur and distort vision, often in teenagers and young adults who should otherwise have healthy eyes. The main treatment to stop this worsening is called corneal crosslinking, but demand for it is rising faster than doctors can keep up. This study from a major UK eye hospital asks a simple but important question: can specially trained nurses safely perform a faster version of this procedure and still protect patients’ sight over the long term?

When the Front Window of the Eye Warps
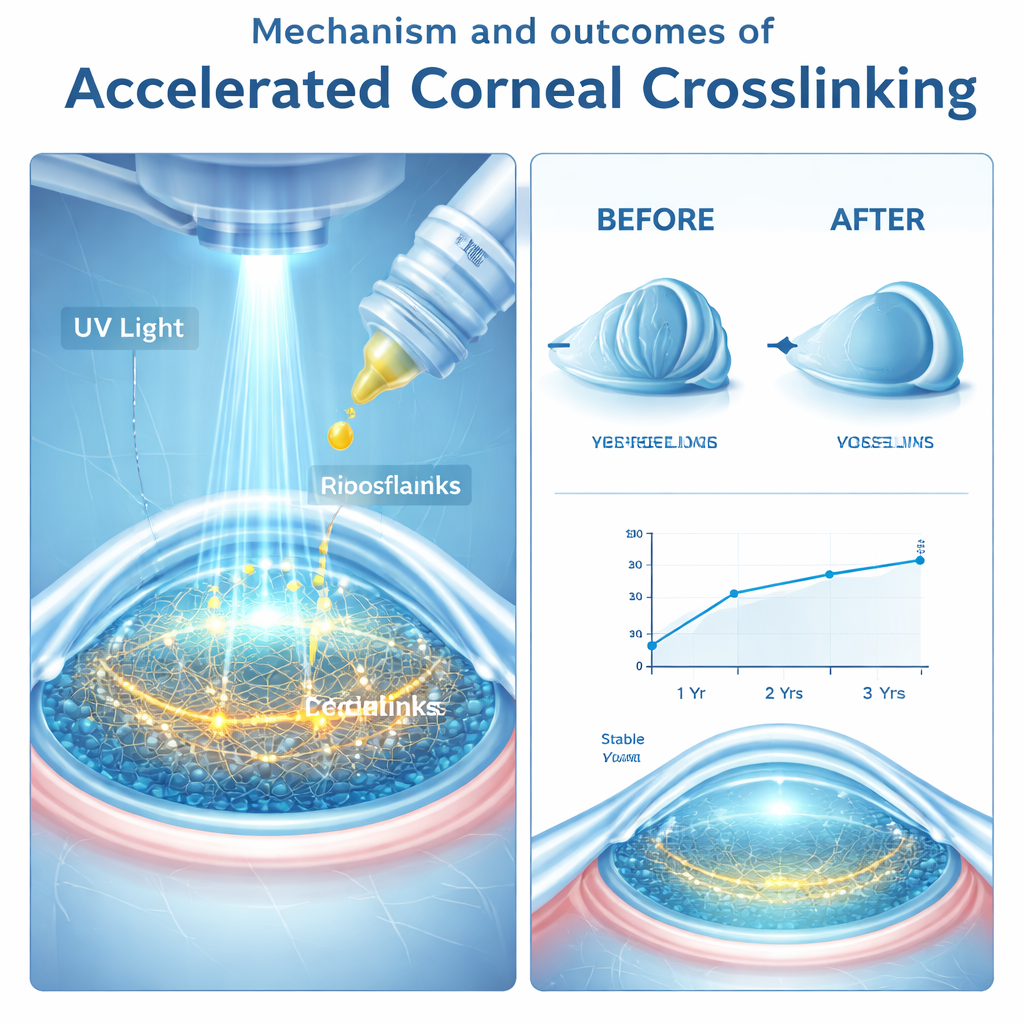
In keratoconus, the cornea gradually thins and becomes cone‑shaped instead of smoothly curved. As the cone steepens, people develop increasing short‑sightedness and irregular astigmatism, so glasses often no longer give clear vision. In the past, many of these patients eventually needed a corneal transplant. Crosslinking changed that story: by shining controlled ultraviolet (UV) light on the cornea after soaking it with vitamin B2 (riboflavin) drops, doctors can stiffen the corneal tissue and usually halt its further warping. Because this treatment works best when done early, long waiting lists can mean the difference between keeping good vision and living with permanent damage.
Sharing the Workload with Specialist Nurses
The Birmingham and Midland Eye Centre introduced a nurse‑led service to help meet the growing need for crosslinking. In this study, they looked back at 97 patients (97 eyes) with worsening keratoconus who had their procedure done by a single specially trained nurse using a standard “accelerated” protocol. Instead of a long 30‑minute light exposure, the team used a higher‑intensity UV light for 9 minutes after gently removing the surface layer of the cornea and applying riboflavin drops. All patients had at least two years of follow‑up, and about one‑third were tracked for three years. The researchers examined vision, corneal shape measurements, and any side effects to see how well this nurse‑led approach worked.
Vision Held Steady—and Often Improved
Over the first two years after treatment, patients’ vision generally improved and then stayed stable. On average, their best corrected distance vision got about one line better on the eye chart, and a larger share of patients achieved what most people would consider “everyday good” vision (roughly driving‑standard sight). A key measure of the cornea’s steepest point, called Kmax, flattened slightly rather than becoming steeper, showing that the cone was no longer progressing. These benefits were maintained in the group followed for three years, with further small improvements in the steepness measures and no meaningful loss of vision. Only a small minority of eyes showed signs of continued corneal change on scans, and even these did not lose lines of vision or need a repeat procedure during the study period.
Safety in Skilled Hands
Safety is crucial when shifting procedures from doctors to other health professionals. In nearly 100 eyes over up to three years, there were no serious complications such as corneal infections or tissue breakdown. Three patients developed noticeable but mild corneal haze in the first week after surgery; this cleared quickly with standard steroid drops and did not leave lasting problems. Overall, the pattern of side effects looked very similar to results reported when doctors perform the same accelerated crosslinking protocol. The researchers also searched for risk factors—such as age, starting vision, or corneal measurements—that might predict which patients would continue to worsen, but none stood out, possibly because relatively few eyes showed progression.
Freeing Up Clinics While Saving Vision
For a lay reader, the bottom line is reassuring: when properly trained and supervised, specialist nurses can safely deliver a quicker form of corneal crosslinking that effectively holds keratoconus in check for at least two to three years. Patients tended to see slightly better, their corneas stayed more stable, and serious harms were not seen. By expanding nurse‑led services, eye departments can shorten waiting times, offer timely treatment to more young people at risk of vision loss, and reserve doctors’ time for the most complex cases. In practical terms, this model could help many more patients keep their own clear cornea and avoid a transplant later in life.
Citation: Khan, M., Sahota, R., Hanson, J. et al. Two-to-three-year effectiveness and safety of nurse-led accelerated corneal crosslinking for progressive keratoconus: The Birmingham and Midland Eye Centre Study. Eye Open 2, 6 (2026). https://doi.org/10.1038/s44440-026-00013-z
Keywords: keratoconus, corneal crosslinking, nurse-led care, vision preservation, eye surgery