Clear Sky Science · en
Gaps in recovery priorities between individuals with spinal cord injury and healthcare professionals
Why this study matters to everyday life
When someone has a spinal cord injury, it can change nearly every aspect of daily life, from using their hands to going to the bathroom. Doctors and therapists try to help people regain as much function as possible—but what if the goals they focus on are not the same ones their patients care about most? This study from Japan looked closely at what people living with spinal cord injury say they most want to recover, and compared that with what healthcare professionals think is most important. The findings reveal a quiet but important mismatch that can affect quality of life, independence, and satisfaction with care.
Different injuries, different daily struggles
The researchers surveyed 103 people in Japan living with spinal cord injury and 85 healthcare professionals who care for them. Among the people with injuries, some had tetraplegia (affecting the arms and legs) and others had paraplegia (mainly affecting the legs). The team asked everyone to choose and rank their top three recovery wishes from 14 everyday functions, such as arm and hand use, bladder and bowel control, walking, sexual function, and temperature regulation. This allowed the scientists to see clear patterns in what people valued most, and how those patterns shifted depending on the type of injury.
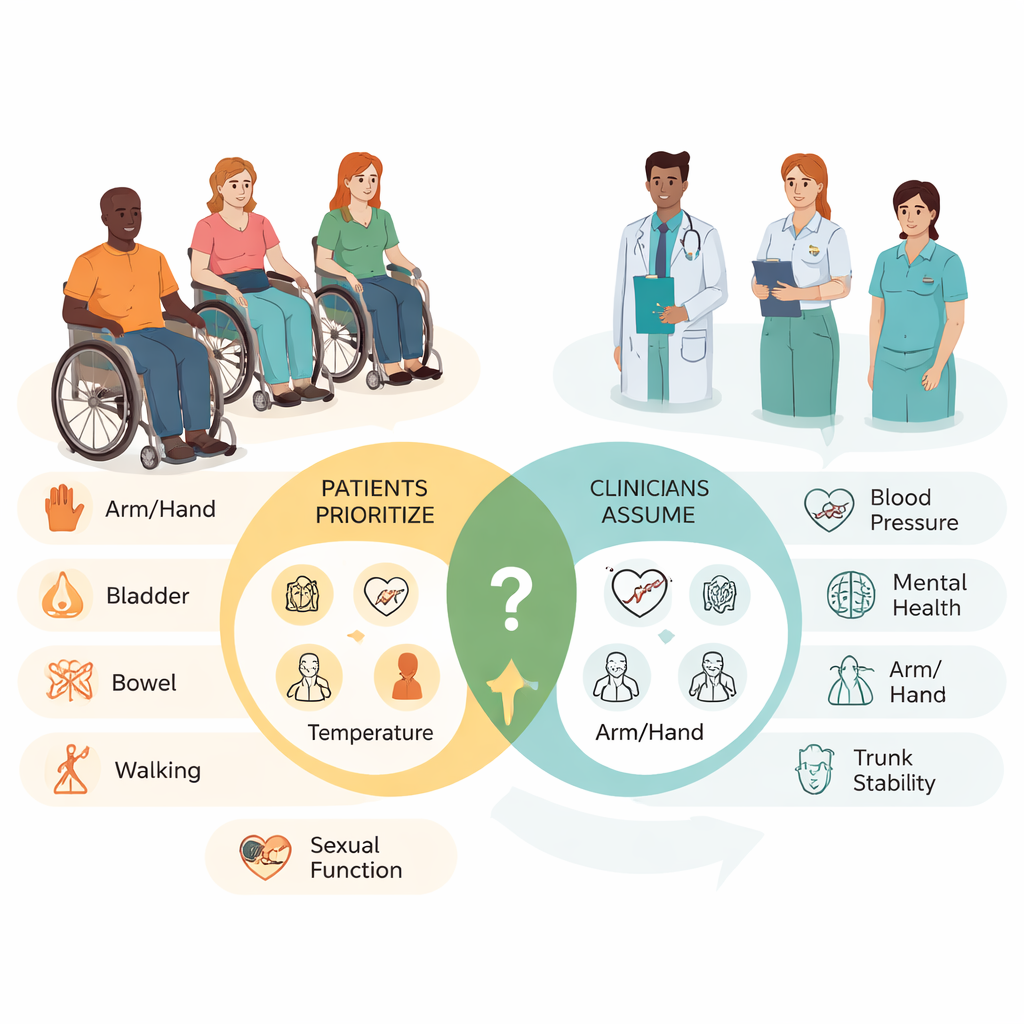
What people with spinal cord injury want most
For people with tetraplegia, being able to use their arms and hands again rose to the very top. That makes sense: reliable hand function can mean being able to feed oneself, use a phone, push a wheelchair, or manage personal care without constant help. For people with paraplegia, who usually retain arm and hand use, the top priority was different: bladder function. Many in both groups also placed high importance on bowel control, standing and walking, and managing body temperature. These choices reflect the exhausting reality of living with problems that are often invisible to others—such as having to plan life around long bathroom routines, worrying about leaks or infections, or feeling too hot or too cold because the body no longer regulates temperature well.
Unseen burdens of bladder and bowel problems
The study highlights how strongly bladder and bowel issues shape everyday life after spinal cord injury. Frequent urinary tract infections, fear of accidents in public, and the sheer time it takes to manage bladder and bowel care can limit work, relationships, and social activities. Many people with spinal cord injury report spending more than half an hour on each bowel routine and adjusting their schedules—and even their social lives—to avoid embarrassment. These challenges are not just medical problems; they touch dignity, independence, and the ability to participate fully in community life.
What healthcare professionals think is most important
When researchers turned to the healthcare professionals, they found a different set of priorities. Clinicians tended to emphasize blood pressure control, mental health and psychological well-being, and arm and hand function. These concerns partly reflect what they see most often in hospitals and rehabilitation units, such as dangerous blood pressure swings or emotional distress after injury. Many of the professionals surveyed were physical and occupational therapists working in acute or inpatient settings, where urgent medical issues demand attention. Yet their rankings showed that they generally placed less weight on bladder, bowel, sexual function, and temperature regulation than the people actually living with spinal cord injury.
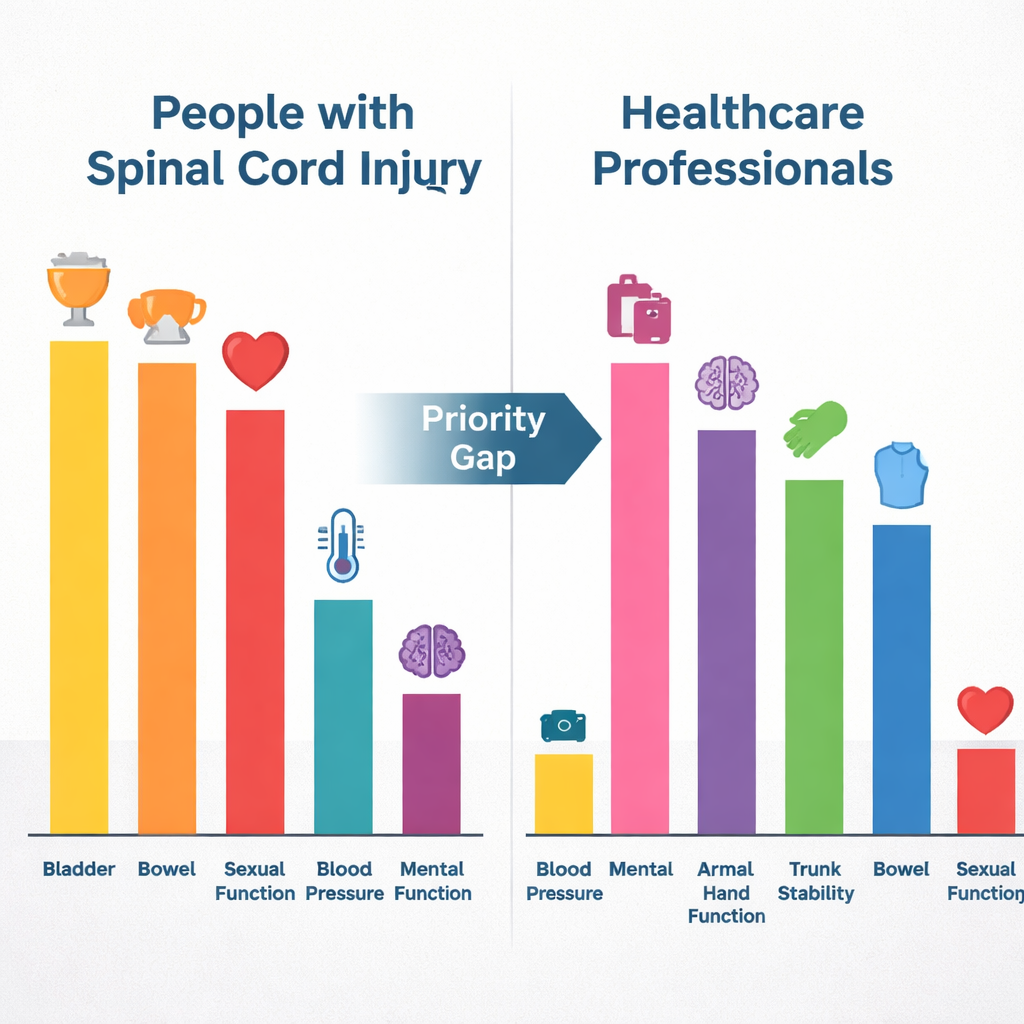
Closing the gap between medical care and real life
The contrast between the two groups reveals a crucial “priority gap”: people with spinal cord injury tend to place more importance on autonomic functions—those that control bladder, bowel, sexual function, skin, and body temperature—while healthcare professionals focus more on visible movement and immediate medical risks. The authors argue that to deliver truly person-centered rehabilitation, these invisible but deeply felt needs must be brought to the forefront. That means asking patients directly about their goals, teaching clinicians more about the day-to-day impact of bladder, bowel, and sexual problems, and weaving these topics into routine care plans. In simple terms, the study’s message is clear: recovery plans work best when they are built around what matters most to the people living with the injury, not just what looks most urgent on a medical chart.
Citation: Samejima, S., Miyashita, H., Yamashita, T. et al. Gaps in recovery priorities between individuals with spinal cord injury and healthcare professionals. npj Health Syst. 3, 19 (2026). https://doi.org/10.1038/s44401-026-00073-4
Keywords: spinal cord injury, rehabilitation priorities, quality of life, patient-centered care, bladder and bowel function