Clear Sky Science · en
A simulation framework for evaluating electronic order workflows in integrated health records
Why the Invisible Digital Paperwork Matters
Every time a doctor orders a lab test, an X-ray, or a specialist consult, that request travels through a maze inside the electronic health record (EHR). If that digital journey is slow or gets stuck, patients wait longer for care and staff lose time chasing status updates. This paper describes a new way to "test drive" those hidden electronic workflows using computer simulation, so hospitals can safely explore how changes in software, staffing, or demand might affect delays and backlogs before patients feel the impact.
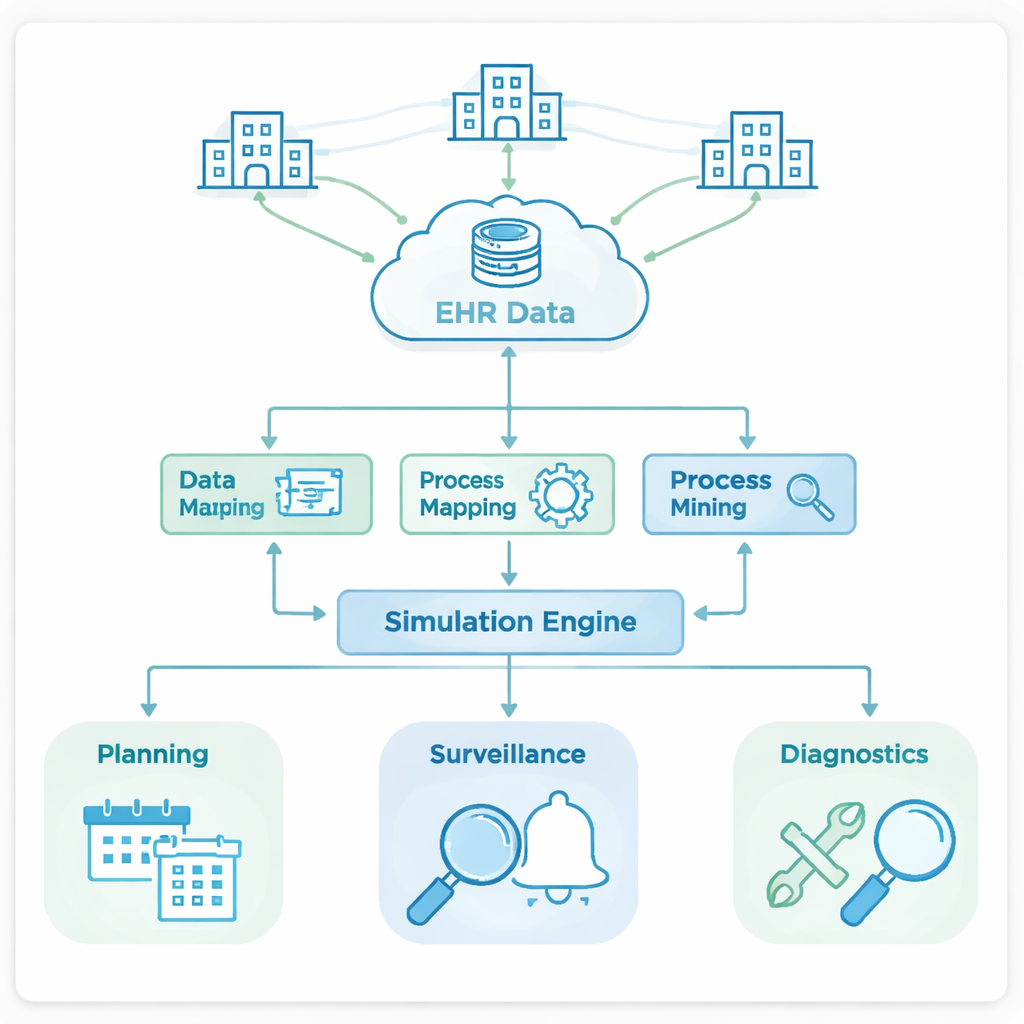
Turning Raw Clicks into a Clear Story
The authors focused on the Veterans Health Administration, the largest integrated health system in the United States. Its EHR records every step an electronic order takes, but the data are scattered across many technical tables and time stamps. The team first translated this jumble of events into a simple, universal set of states that any layperson could recognize in a process: an order is Created, made Ready, Reserved for action, moved InProgress, and finally Completed, or it may end in problem states like Failed, Exited, or Error. This mapping, based on an international standard for business workflows, turned messy logs into clean, comparable digital “tracks” that show how orders actually move through the system.
Building a Virtual Test Track for Orders
With these standardized tracks, the researchers built a discrete‑event simulation—a computer model that plays out thousands of orders as they move from state to state over time. They calibrated the model using real data from five Veterans hospitals, feeding in how often each transition happens and how long it typically takes, including rare but very long delays. They then checked how well the simulated “time in system” for orders matched history, using statistical tests and side‑by‑side plots. The simulated and real timelines agreed closely across facilities, especially for the typical cases, giving confidence that the virtual system behaves much like the real one and can be used for “what‑if” experiments.
Stress‑Testing the System Under Pressure
The team then used the model to ask practical questions: What happens if more orders arrive, or if key steps are limited by staff or equipment? In one set of experiments, they increased order volume and capped how many orders could be processed at crucial steps such as moving from Reserved to InProgress, or from InProgress to Completed. When there were no limits, the system absorbed higher demand with only modest growth in orders waiting. But once caps were introduced, backlogs swelled and the system struggled to reach a stable state, especially under heavier demand. In effect, modest resource limits turned a manageable surge into a tipping point where delays and unfinished orders rose sharply—insights that can guide staffing and capacity planning.
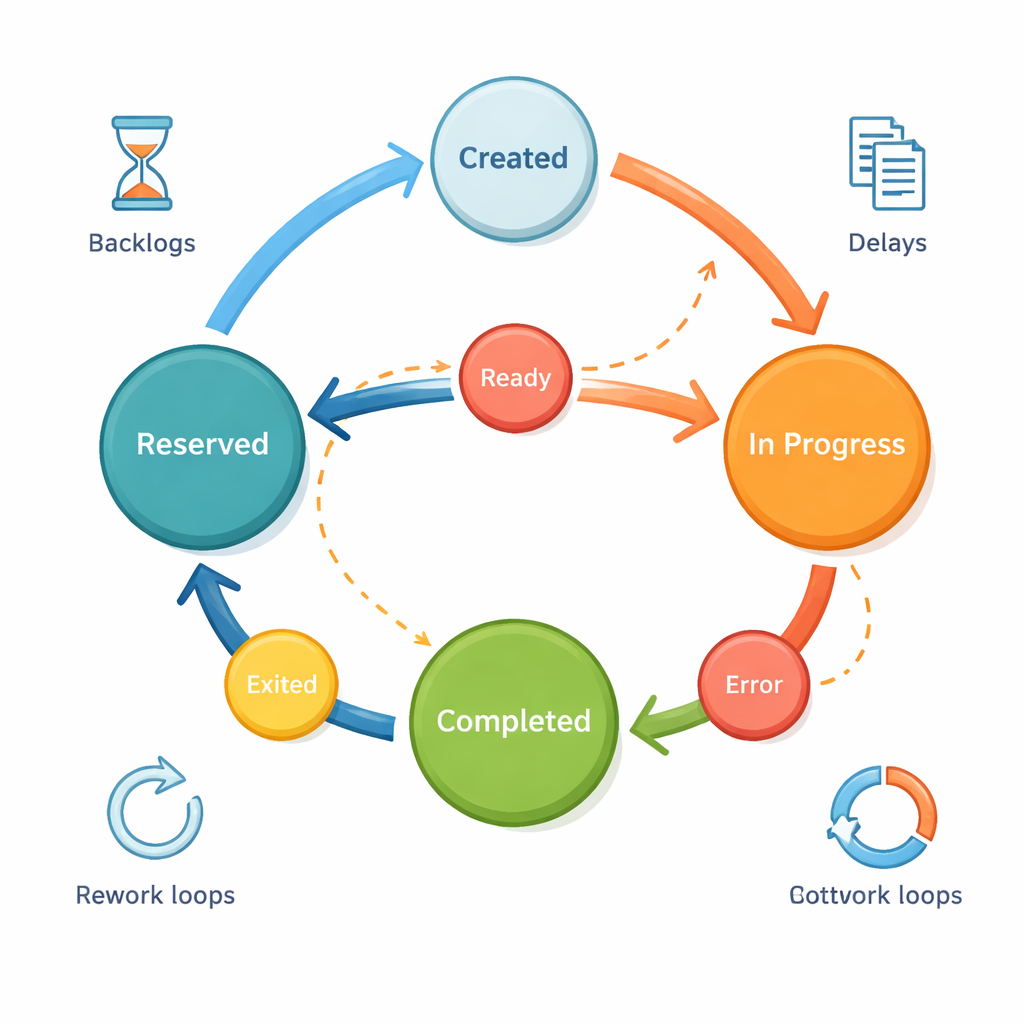
Following the Detours and Loops
The researchers also explored how small changes in routing rules ripple through the system. When they made it harder for orders to take a shortcut directly from Ready to Completed, more orders were forced to pass through Reserved and InProgress. This reduced overall throughput for a time and created longer, more tangled paths, with some orders looping back multiple times and spending far more time in the system. By visualizing the most common paths and counting how often orders “loop back” to earlier states, the model highlights where rework and repeated handling silently consume staff time. Network analysis of the digital routes showed that three states—Reserved, InProgress, and Completed—act as central hubs and potential bottlenecks where congestion is most likely to appear and where closer monitoring would pay off.
Using a Digital Twin to Keep Care Moving
For non‑specialists, the main takeaway is that the authors have built a kind of digital twin for EHR orders: a safe, data‑driven sandbox where leaders can rehearse changes before they touch patients. The study shows that this approach can realistically mirror how electronic orders move, where they jam up, and how policy tweaks or demand spikes might create hidden queues and delays. Hospitals could use such simulations to test new rules, plan for surges, watch key states for early signs of trouble, and reduce wasteful rework. In doing so, they can make the invisible plumbing of digital orders more reliable, helping ensure that behind‑the‑scenes technology keeps pace with the urgency of patient care.
Citation: Chen, Y., Niu, H., Omitaomu, O.A. et al. A simulation framework for evaluating electronic order workflows in integrated health records. npj Health Syst. 3, 14 (2026). https://doi.org/10.1038/s44401-026-00067-2
Keywords: electronic health records, workflow simulation, healthcare operations, digital twin, Veterans Health Administration