Clear Sky Science · en
Large animal models for the assessment of snakebite envenoming therapies
Why Snakebites Still Matter
For many people, snakes are a rare worry. Yet in parts of Africa, Asia, and Latin America, a single bite can mean death, disability, or lifelong scars. More than 100,000 people die each year from snakebite, and many more lose limbs or suffer organ damage. This article looks at an underappreciated part of the solution: how we test new treatments before they ever reach a hospital. The authors argue that relying mostly on mice is not enough and explain why larger animals such as sheep and pigs are crucial for creating faster, safer, and more effective therapies for snakebite victims.
From Barnyard to Bedside
Today’s main treatment for snakebite is antivenom made from the blood of large animals, usually horses. These life‑saving medicines contain many different antibodies, but only some of them neutralize the harmful toxins in venom. They can be expensive, cause side effects, and are often hard to deliver in remote areas. New tools in biotechnology and chemistry are opening the door to next‑generation therapies: carefully designed antibody mixtures, tiny antibody fragments called nanobodies, custom‑built protein “minibinders,” and oral drugs that block venom enzymes. Most early tests of these ideas use mice, which are cheap and convenient. But mice are small, and their bodies process drugs differently from humans, making it hard to predict how a promising therapy will behave in real patients.
What Big Animals Can Tell Us
The review focuses on “large animal models” whose body size, blood volume, and circulation are closer to humans. Sheep and pigs stand out as especially useful. In sheep, researchers can place special tubes into the lymphatic system—the network of vessels that drains fluid and large molecules from tissues. This lets them track exactly how venom components move from the bite site into the bloodstream and how long they linger, which is vital for deciding when and how often to give treatment. Pigs, on the other hand, have skin, muscles, and wound‑healing patterns that closely resemble ours. Their thick skin and rich blood supply make them a powerful stand‑in for studying local tissue damage, such as the painful dead patches of skin and muscle that some venoms cause.
Following Venom and Medicine Through the Body
Snake venom is not a single substance but a cocktail of proteins of different sizes and actions. Small toxins slip quickly into nearby blood vessels, while larger ones often travel through the lymphatic system before reaching the circulation. Some toxins remain in a “depot” at the bite site, leaking out over many hours and causing symptoms to return even after treatment. Large animals allow repeated blood and lymph sampling from the same individual, so scientists can map how each toxin and each therapy rises and falls over time. The article explains how full‑size antibodies, their fragments, nanobodies, and small‑molecule drugs all behave differently in the body—some stay mainly in the bloodstream for days, others dive rapidly into tissues but are cleared within hours. Matching these patterns to venom behavior is key to making sure a therapy is present in the right place, at the right concentration, for long enough to neutralize toxins.
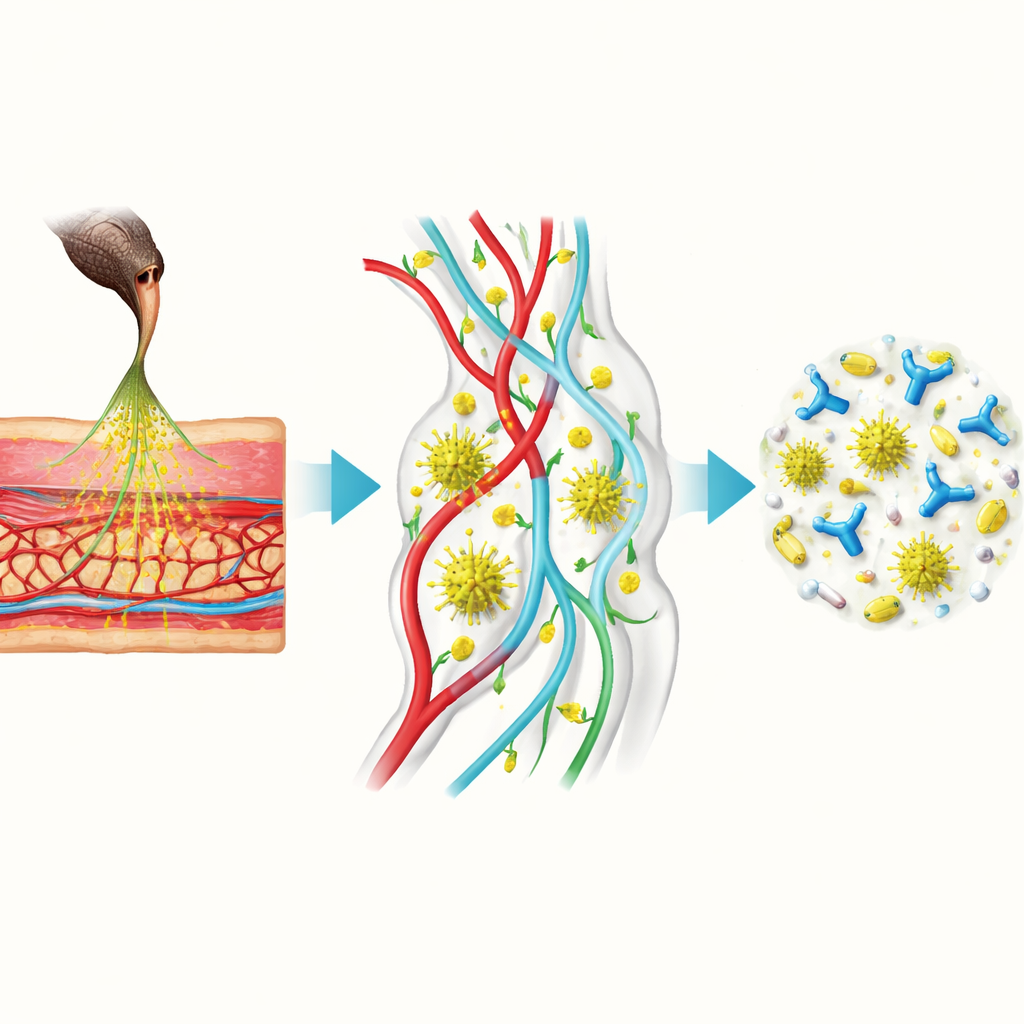
Building Better Models of Real Snakebites
Large animal studies are already yielding real‑world insights. In pigs, an oral drug called varespladib has reversed otherwise lethal bites from certain highly neurotoxic snakes, helping guide human trials now underway. Porcine models have also been used to test how pressure bandages, surgery to relieve swollen muscle compartments, and different routes of antivenom delivery affect outcomes. Still, such experiments are demanding: they need specialized veterinary teams, strict ethical oversight, and high costs. The authors suggest using mice for early screening, then moving only the most promising approaches into carefully designed large‑animal experiments that mirror human disease as closely as possible.
What This Means for Patients
The authors conclude that to truly improve snakebite care, we must understand both sides of the battle: how venom spreads and lingers in the body, and how our treatments move and act in response. Large animals, particularly sheep and pigs, offer a critical bridge between simple mouse tests and complex human illness. By standardizing how these studies are done, choosing clinically meaningful outcome measures, and linking results to detailed reports from human snakebite cases, researchers can speed the path from laboratory ideas to bedside reality. In the long run, this approach should help deliver more precise, affordable, and safer treatments to the people who need them most, wherever dangerous snakes and vulnerable communities intersect.
Citation: Benard-Valle, M., Ahmadi, S., Modahl, C.M. et al. Large animal models for the assessment of snakebite envenoming therapies. npj Drug Discov. 3, 12 (2026). https://doi.org/10.1038/s44386-026-00043-8
Keywords: snakebite envenoming, antivenom development, large animal models, sheep and pig research, venom pharmacokinetics