Clear Sky Science · en
Advances in mechanical assessments of in vivo human lumbar spine tissues with noninvasive imaging techniques
Why Your Aching Back Needs More Than a Picture
Lower back pain is now the world’s leading cause of disability, yet most scans your doctor orders—like X‑rays or MRIs—mainly show what your spine looks like, not how it actually works. This review article explores a new frontier: imaging tools that measure how the discs and muscles in your lower back move, deform, and share load in real time. By revealing the spine’s mechanics rather than just its shape, these techniques could finally explain why so many people hurt even when their scans “look normal,” and help tailor treatments to how each person’s spine really behaves.
The Spine as a Living Mechanical System
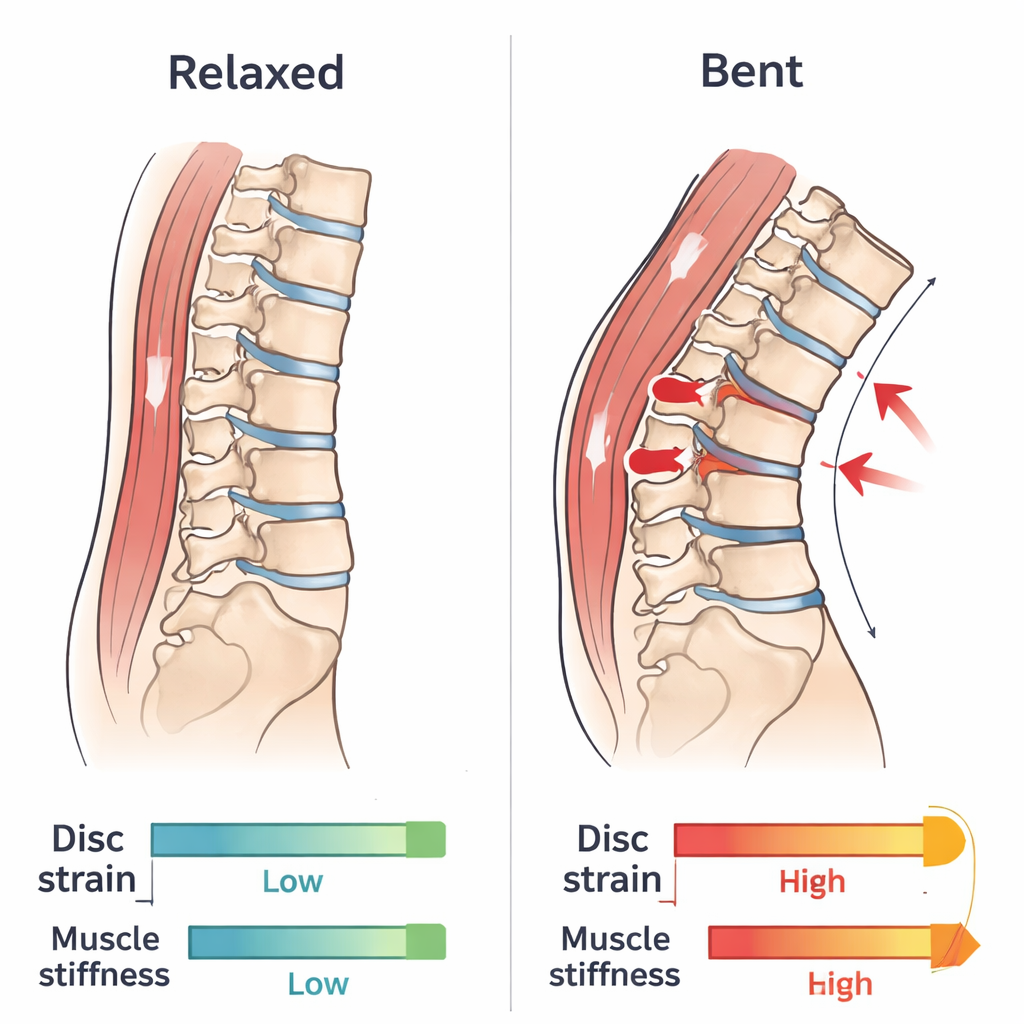
Your lumbar spine is far more than a stack of bones. Between each vertebra lies an intervertebral disc with a soft, gel-like center that attracts water and builds pressure, wrapped in tough, fibrous rings that resist bending and twisting. Thin cartilage plates connect the discs to bone, while a network of deep and superficial muscles—like the multifidus, erector spinae, and psoas—stabilize the spine and fine‑tune every movement. Low back pain rarely comes from the bones themselves. Instead, it usually reflects problems in these “passive” tissues (discs, joints, ligaments) and “active” tissues (muscles) that together keep the spine stable, flexible, and able to bear daily loads.
Why Standard Scans Miss Most Back Pain
Conventional imaging is excellent at spotting obvious issues like fractures, severe disc herniations, or tumors. It can also grade age‑related changes such as disc thinning or fatty streaks in muscles. But such changes are extremely common, even in people with no pain at all. As a result, most patients with chronic low back pain get labeled with “nonspecific mechanical back pain” because no clear structural cause is visible. The core problem is that anatomy alone does not capture mechanical function—how much a disc compresses during the day, how strain is shared across levels, or how stiff or weak key muscles have become. Without these mechanical clues, it is hard to distinguish normal aging from true disease or to pick the right treatment.
New Ways to Watch the Spine in Motion
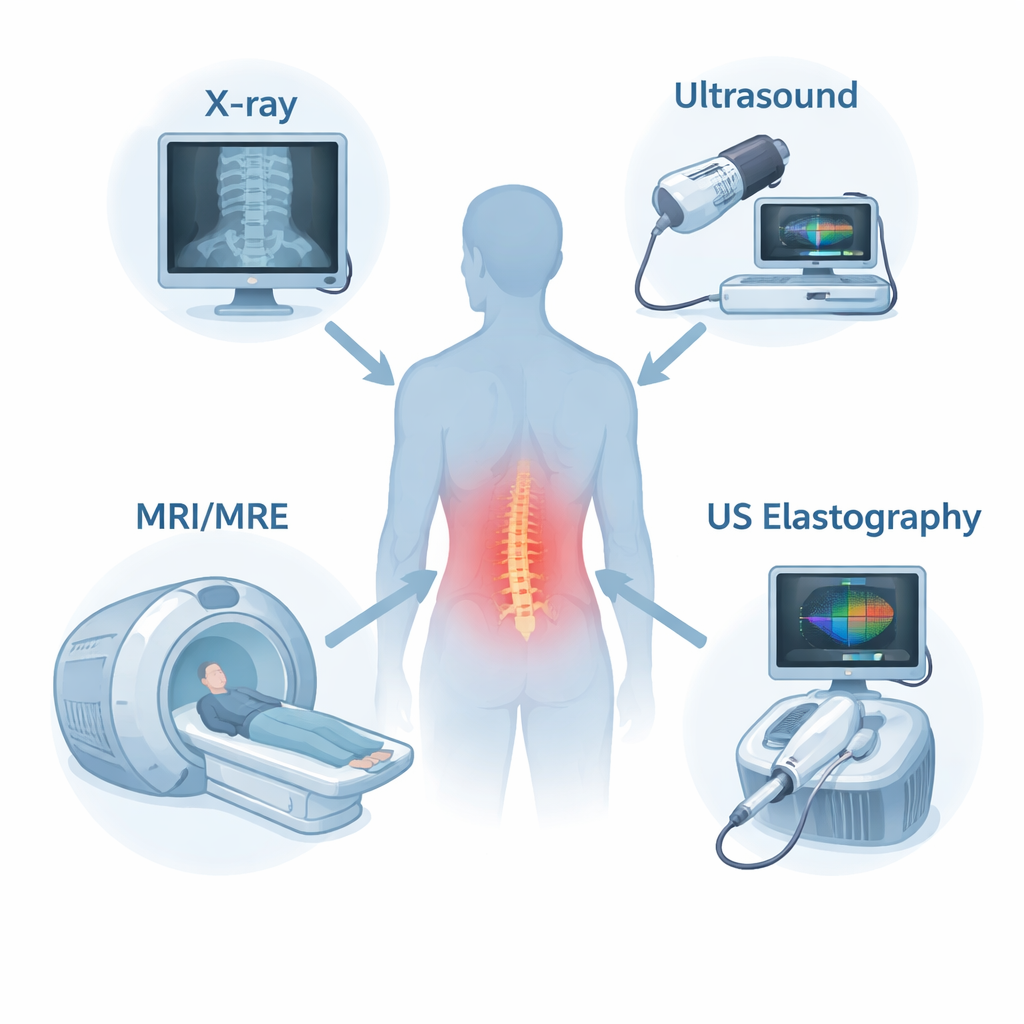
The review describes how several noninvasive imaging tools are being adapted to measure spinal mechanics in living people. Dynamic radiography and low‑dose 3D X‑ray systems can follow vertebrae as you bend or lift, revealing subtle shifts that may signal instability. Ultrasound can track the motion of the bony bumps you feel along your back and measure how back muscles thicken when they contract; its elastography versions go further by estimating muscle and disc stiffness from the speed of tiny shear waves. Magnetic resonance imaging (MRI) can now be performed during or after loading—such as standing, flexing, or walking on a treadmill—to map how discs deform and lose water over the day, while advanced sequences estimate tissue composition. Magnetic resonance elastography (MRE) uses vibrations inside an MRI scanner to create stiffness maps of deep discs and muscles, turning the scanner into a mechanical probe rather than just a camera.
From Promising Images to Practical Answers
Each technique brings trade‑offs. X‑ray methods are fast and good for bone mechanics but expose patients to radiation and show little muscle detail. Ultrasound and its elastography cousin are portable, safe, and good at capturing muscle behavior over time, but they struggle with deep structures and depend heavily on operator skill. MRI offers rich detail on both structure and function, yet studies often involve small groups of young, healthy volunteers and are technically demanding. MRE is already reliable for back muscles but still being refined for discs, where small size and high stiffness make measurements tricky. Across all methods, large differences between people, limited data on patients with significant symptoms, and varying protocols make it difficult to define what “normal” mechanics should look like at each spinal level and age.
How Mechanics Could Transform Back and Neck Care
The authors argue that the next big step is to turn these mechanical measurements into practical clinical tools. That will require collecting large, age‑ and sex‑specific reference datasets, studying people with different types of back and neck pain under realistic loading conditions, and following them over time to see which mechanical patterns predict worsening pain or recovery. Combining detailed maps of strain and stiffness with computational models and machine‑learning tools could allow doctors to pinpoint whether a patient’s pain stems mainly from overstressed discs, stiff or fatigued muscles, or abnormal motion at specific levels. For patients, this would mean moving from generic labels and trial‑and‑error therapies toward truly personalized, mechanism‑based diagnosis and treatment of spinal pain.
Citation: Elliott, D.M., Newman, H.R., Conner, M.N. et al. Advances in mechanical assessments of in vivo human lumbar spine tissues with noninvasive imaging techniques. npj Biomed. Innov. 3, 15 (2026). https://doi.org/10.1038/s44385-026-00070-0
Keywords: low back pain, spine mechanics, noninvasive imaging, intervertebral disc, muscle stiffness