Clear Sky Science · en
Trajectory of compensated metabolic dysfunction-associated steatohepatitis in a tertiary center with a large hispanic/latino population
Why this quiet liver disease matters
Many people live with serious liver scarring without realizing it. This study looks at a condition called metabolic dysfunction–associated steatohepatitis, or MASH, in people whose livers are badly scarred but who do not yet feel very sick. Because MASH is tightly linked to common problems like obesity and diabetes, understanding who gets worse, how fast, and why is crucial for preventing liver failure and saving lives—especially in communities that already face barriers to care.
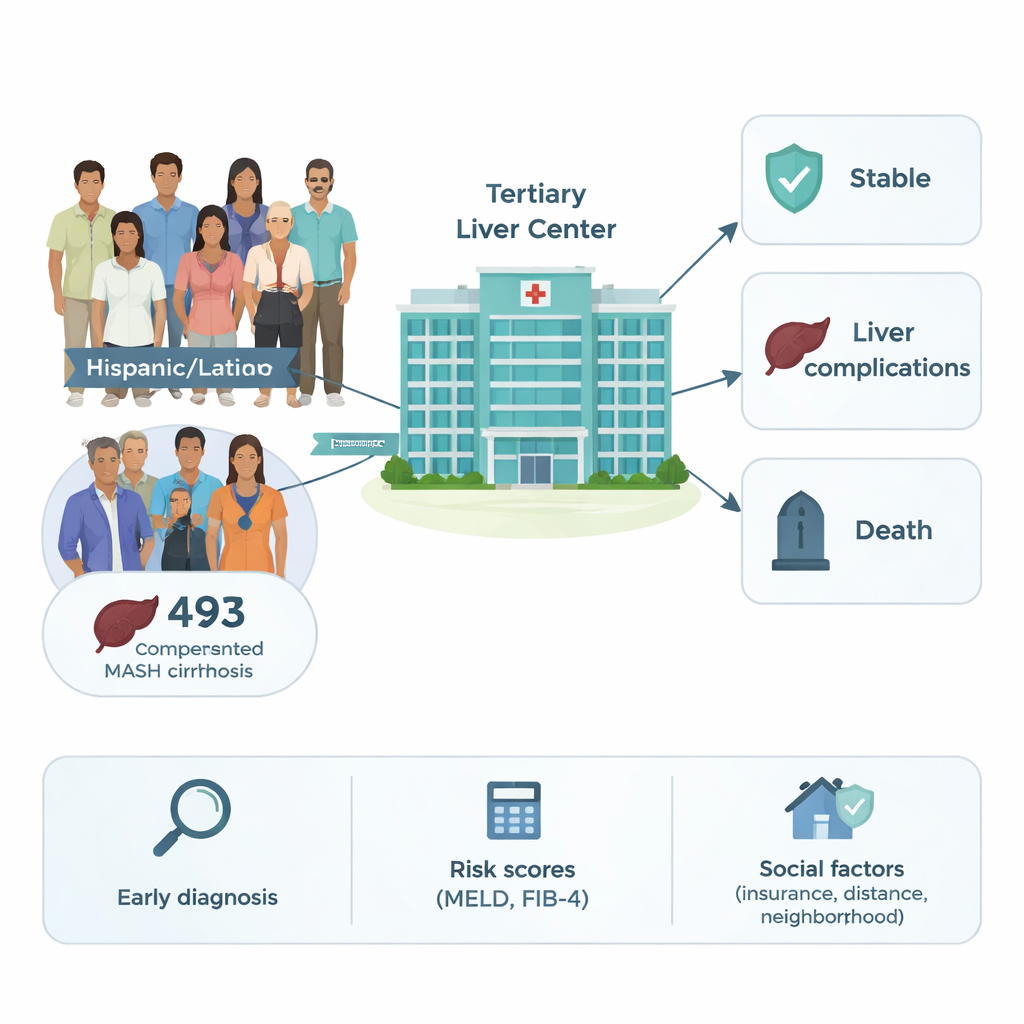
A closer look at patients before the crisis
Researchers at a major liver center in San Francisco analyzed electronic medical records from 2012 to 2024. They focused on 493 adults with “compensated” MASH cirrhosis—meaning their livers were badly scarred, but they had not yet developed dramatic complications like fluid in the belly or confusion. The typical patient was in their mid‑50s, most were women, and about one in three identified as Hispanic or Latino. Many lived with obesity, high blood pressure, high cholesterol, or diabetes, and over half relied on public insurance such as Medicare or Medicaid. This paints a picture of a middle‑aged, medically complex group already carrying a heavy health burden long before obvious liver failure appears.
What happened over time
Even though these patients initially had no major liver symptoms, a large share ran into serious trouble during follow‑up, which lasted a median of 3.4 years. Within five years, about 14% had died and roughly 20% had developed classic signs of liver breakdown, such as fluid buildup, internal bleeding from enlarged veins, or confusion caused by toxin buildup. Adding in other bad outcomes—like liver cancer, need for transplant, or big jumps in standard liver‑severity scores—about one in three patients experienced at least one major event. Their five‑year risk of death was nearly three times higher than what would be expected for people of similar age and sex in the general U.S. population.
Simple scores and blood tests tell a powerful story
The team used time‑to‑event statistical models to search for early warning signs in routine medical data. Two tools stood out: the MELD score and the FIB‑4 index, both based on common lab tests that reflect how damaged the liver is. Higher values on these scores at the first specialist visit strongly predicted later death, complications, and overall disease worsening. Older age and elevated alkaline phosphatase, another blood marker tied to bile flow and scarring, were also linked to a higher risk of death. Interestingly, people who entered the clinic more recently tended to fare somewhat better, hinting that growing awareness and improved care might already be making a difference.
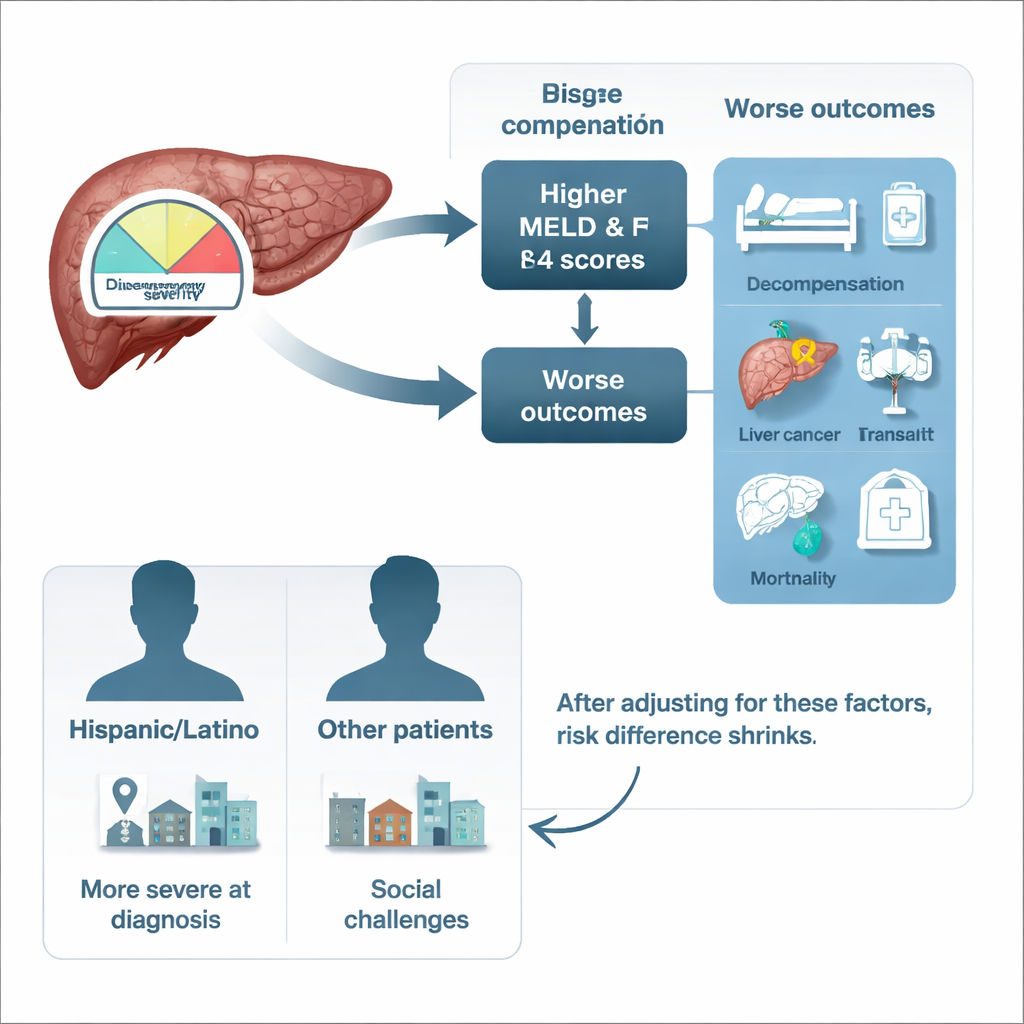
Why Hispanic and Latino patients faced higher risk
Because the clinic serves many Hispanic and Latino patients, the researchers looked closely at differences by ethnicity. Hispanic and Latino patients tended to live farther from the center, in more socially deprived neighborhoods, and were more likely to rely on Medicaid. They also arrived with more advanced liver damage, as reflected in higher MELD scores, and had higher crude rates of fluid buildup in the abdomen and death. However, when the scientists adjusted their models for disease severity and social factors—like neighborhood disadvantage, travel distance, and insurance type—most of the gap in outcomes narrowed. This suggests that where people live, how easily they can reach specialty care, and how late their disease is caught play major roles in the observed disparities.
What this means for patients and communities
To a layperson, the message is clear: by the time MASH cirrhosis causes obvious symptoms, the stakes are already high. This study shows that simple, widely available blood‑based scores can flag people at greatest risk well before they “look” sick, and that early detection plus close follow‑up could prevent a substantial number of bad outcomes. It also highlights that Hispanic and Latino patients are more likely to arrive late and sicker, largely because of social and access barriers rather than inherent biological differences. Improving screening in primary care, using automated tools in electronic records, and bringing liver assessment closer to high‑risk communities could shift the trajectory of this quiet but dangerous disease—especially for those who currently have the least access to timely care.
Citation: Ayati, A., Watanabe, A.H., Guillot, J. et al. Trajectory of compensated metabolic dysfunction-associated steatohepatitis in a tertiary center with a large hispanic/latino population. npj Gut Liver 3, 9 (2026). https://doi.org/10.1038/s44355-026-00057-z
Keywords: MASH cirrhosis, liver disease, health disparities, Hispanic Latino health, risk prediction