Clear Sky Science · en
Leveraging artificial intelligence in eosinophilic esophagitis
Why This Matters for People Who Struggle to Swallow
Eosinophilic esophagitis, or EoE, is a mouthful to say and an even harder condition to live with. It is a chronic allergy‑driven disease of the esophagus—the tube that carries food from mouth to stomach—that can cause painful swallowing, food getting stuck, and long‑term scarring. This review article explores how artificial intelligence (AI) could change the way doctors find, diagnose, and treat EoE, potentially easing the burden on patients who now face repeated procedures and years of trial‑and‑error care.
Understanding a Hidden Digestive Trouble
EoE has become much more common over recent decades, especially in North America and Europe. Adults often feel as though food “hangs up” in the chest, while children may vomit, lose weight, or fail to grow as expected. Because these symptoms overlap with more familiar problems such as acid reflux, diagnosis is often delayed by more than two years. During that time, ongoing inflammation can stiffen and narrow the esophagus, raising the risk of food impactions and even tears. Current care relies on endoscopy (a flexible camera) and tiny biopsies to look for clusters of certain white blood cells. These tests are invasive, must be repeated, and do not always line up neatly with how sick a person feels.
How Smart Machines Can Lend a Hand
AI refers to computer systems that learn patterns from data and make predictions or decisions. In EoE, AI tools are being trained on many kinds of medical information: images from scopes, microscope slides of tissue, pressure and stretch measurements of the esophagus, genetic and blood‑based markers, and even written medical records. Some models can already sort out EoE from look‑alike conditions with very high accuracy, or flag patients with swallowing trouble who are especially likely to have the disease and should be sent for further testing. Others analyze how stiff the esophagus has become or how cells are arranged within a biopsy, revealing subtle disease patterns that human eyes might miss. 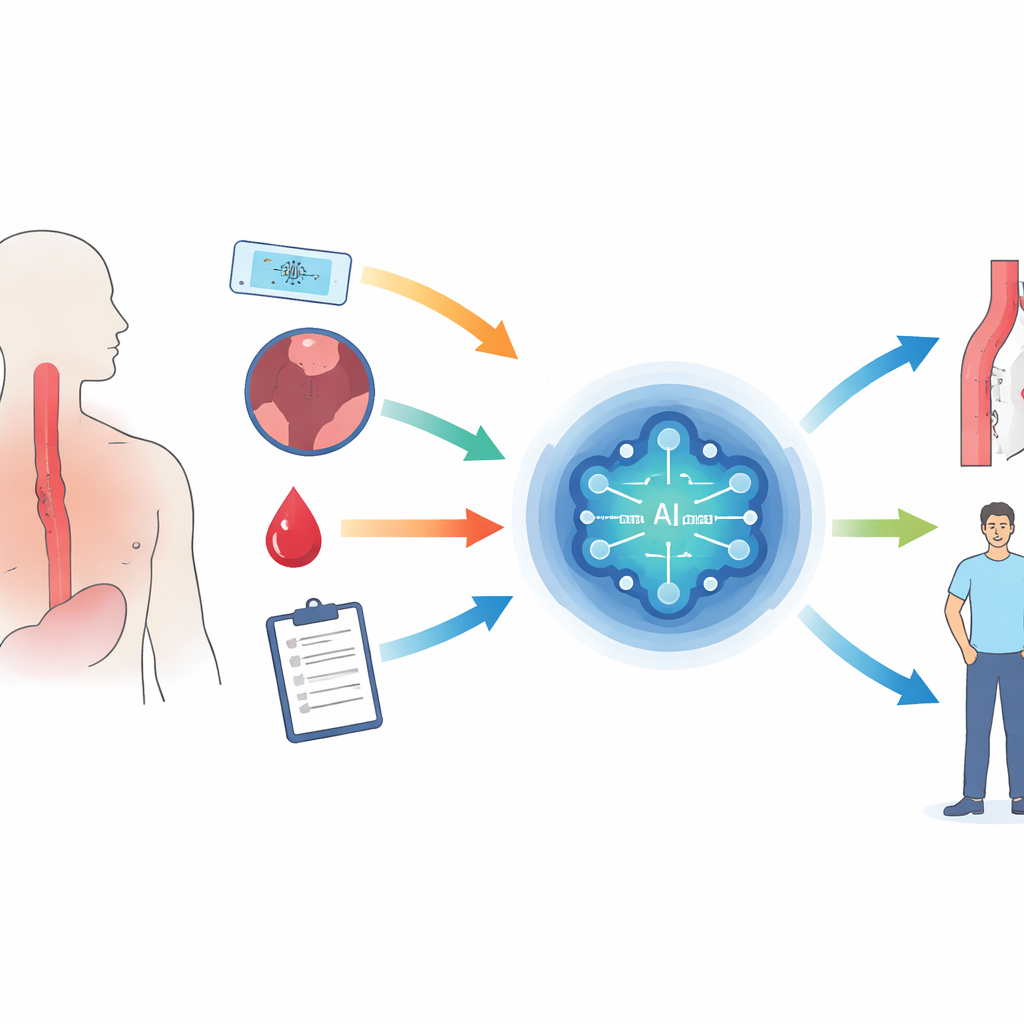
Sharper Images and Smarter Microscopes
Endoscopy and tissue analysis are at the heart of EoE diagnosis, and both stand to benefit from AI. Computer vision systems trained on thousands of scope images can automatically recognize rings, furrows, and white patches that point toward EoE, performing as well as seasoned specialists and better than trainees in some studies. In pathology, counting the key cells one by one is slow and subjective. New AI‑driven digital tools can scan entire biopsy slides, tally relevant cells, measure tissue damage, and even track other immune cells such as mast cells. These systems match expert pathologists in accuracy while offering consistent, repeatable results. Over time, they could provide instant, standardized reports that help doctors monitor disease activity and response to treatment more precisely.
Clues in the Blood, Genes, and Everyday Care
Researchers are also using AI to sift through complex biological signals and day‑to‑day clinical data. Machine learning models trained on gene expression and small regulatory molecules (microRNAs) have pinpointed patterns that clearly separate EoE from reflux and normal tissue, and may even reflect how well a patient is responding to steroid therapy. Similar approaches could one day turn a blood sample or a simple swab into a reliable test that tracks disease without repeated scopes. The review also examines AI chatbots and language models as tools for patient education. Early tests show that current general‑purpose systems can sound confident yet mix accurate statements with errors and confusing language, highlighting the need for careful tuning and medical oversight before such tools can safely support people living with EoE. 
Balancing Promise with Precautions
Despite the excitement, the authors stress that AI is not a magic fix. Many EoE studies rely on small, narrow patient groups, raising concerns about bias and limited real‑world reliability. Complex models can behave like “black boxes,” offering predictions without clear explanations, which complicates trust, accountability, and regulation. The review outlines the emerging rules for treating advanced algorithms as medical devices, emphasizing the need for large, diverse datasets, transparent testing, and ongoing monitoring. If these hurdles are met, AI could help transform EoE care from a slow, invasive, one‑size‑fits‑all process into a more precise, timely, and less burdensome journey—allowing patients to get the right diagnosis and the right treatment sooner, with fewer procedures and better long‑term outcomes.
Citation: Liberto, J.D., Snyder, D.L. & Codipilly, D.C. Leveraging artificial intelligence in eosinophilic esophagitis. npj Gut Liver 3, 13 (2026). https://doi.org/10.1038/s44355-025-00046-8
Keywords: eosinophilic esophagitis, artificial intelligence in medicine, endoscopy imaging, digital pathology, precision gastroenterology