Clear Sky Science · en
Advances in principles and technologies of non-mechanical blood pressure monitoring
Why Your Blood Pressure Gadget Is Getting Smarter
High blood pressure quietly raises the risk of heart attack, stroke, and kidney failure for more than a billion people worldwide. Yet many never know they have it, in part because checking blood pressure usually means finding a cuff, sitting still, and enduring an uncomfortable squeeze. This review article explores a new generation of "cuffless" technologies that promise gentler, more frequent, and more convenient blood pressure tracking—built into watches, rings, cameras, and even radar-like sensors.
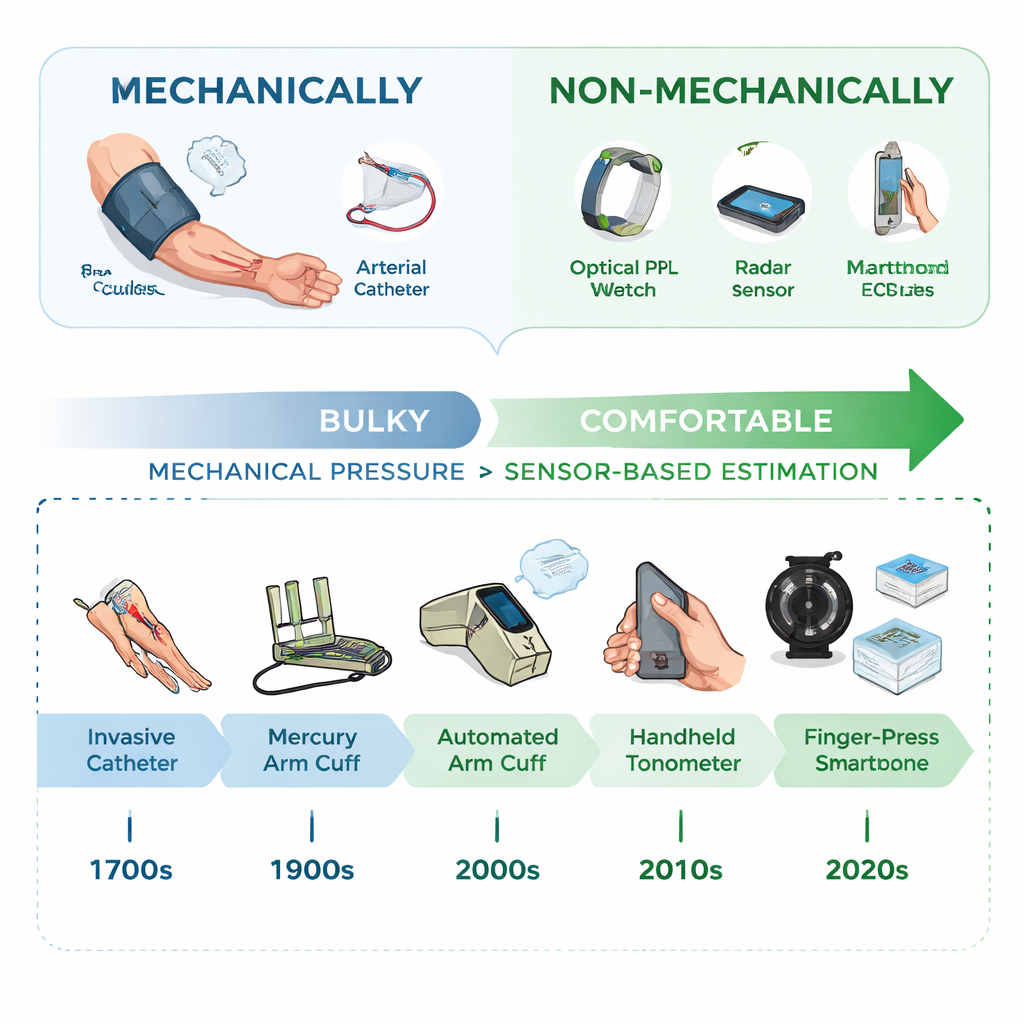
From Bulky Cuffs to Invisible Monitors
The story of blood pressure monitoring began with tubes placed directly into arteries in the 18th century, a method still used in intensive care units because of its accuracy. In the 1900s, doctors adopted arm cuffs and stethoscopes, and later automated cuff devices made home monitoring possible. But all of these are mechanical methods: they literally squeeze or press on an artery to feel its force, which can be painful, disruptive at night, and impractical for tracking quick changes during daily life. Recent years have seen a push toward more comfortable options that blend into everyday objects, allowing people to monitor blood pressure as they move, work, and sleep.
Measuring Pressure Without the Squeeze
The authors introduce a simple but powerful way to classify today’s devices: mechanical versus non-mechanical. Mechanical tools apply physical pressure and read it directly, like a traditional cuff. Non-mechanical tools, by contrast, never squeeze the artery. Instead, they watch the body for subtle signals that move in step with blood pressure—changes in blood vessel width, the speed of the pulse wave, or the shape of the pulse itself. Wearable and contactless devices can now track these signals using light (as in smartwatch pulse sensors), ultrasound patches, skin-mounted motion sensors, chest and wrist accelerometers, radar, or ordinary cameras that detect tiny color shifts in the face or hand. These signals are then translated into blood pressure numbers using mathematical formulas or machine-learning algorithms.
How Data and Algorithms Turn Pulses into Numbers
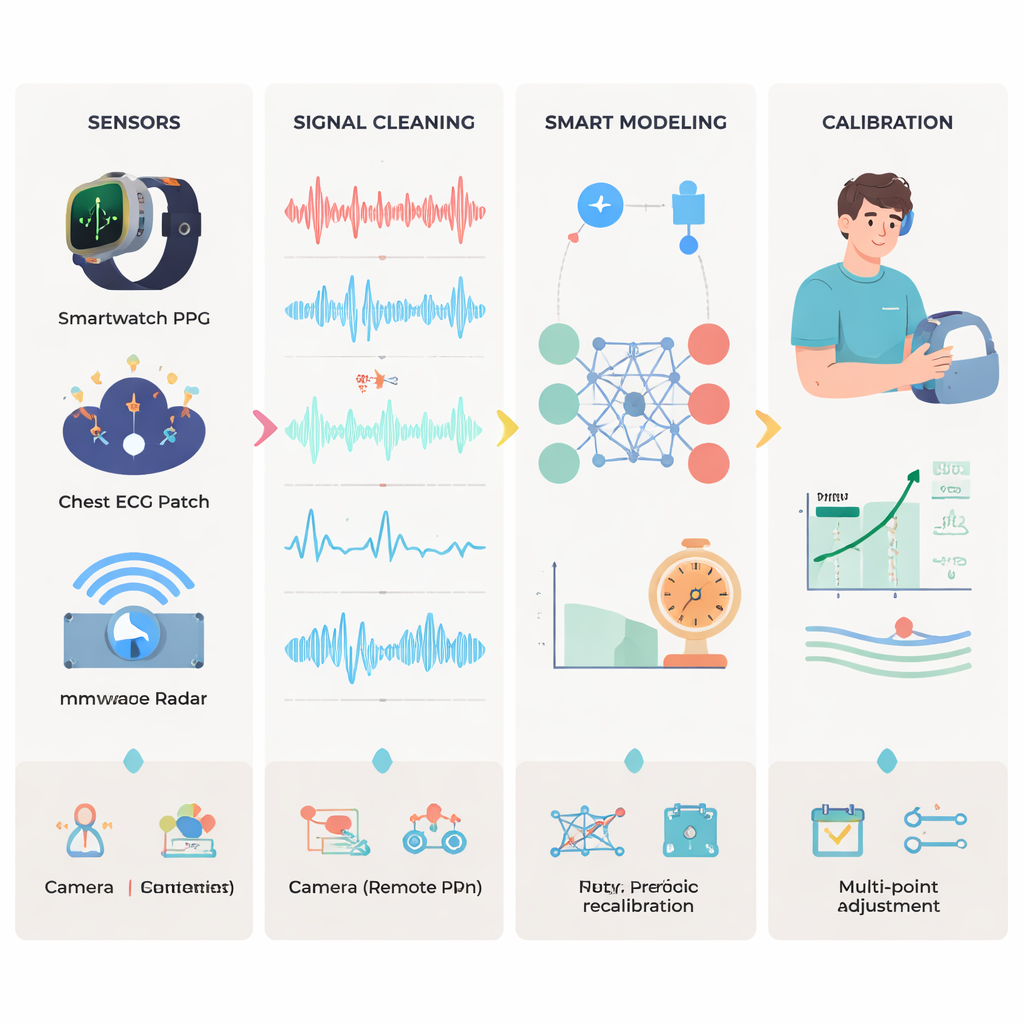
Non-mechanical monitoring follows a four-step pipeline. First, sensors capture raw biosignals such as optical pulse waves, electrical heart traces, or tiny body vibrations. Second, these signals are cleaned: obvious glitches are removed, noise is filtered out, and data from multiple devices are carefully time-aligned so that tiny timing differences—often just tens of milliseconds—can be trusted. Third, models estimate blood pressure from the cleaned signals. Early efforts relied on physics-based equations linking pulse speed or vessel size to pressure. Newer approaches use machine learning and deep learning to discover hidden patterns, including neural networks that analyze waveforms directly, attention mechanisms that focus on the most informative parts of each beat, and “physics-informed” networks that weave known cardiovascular laws into the training process. Finally, calibration ties everything back to reality by comparing the device’s estimates with a trusted reference, typically an arm cuff or an invasive line.
Challenges Before Doctors Can Fully Trust Cuffless Devices
Despite rapid progress, cuffless systems still face obstacles before they can be widely used in clinics. Their accuracy can drift as a person’s body or behavior changes—after exercise, during stress, or over months and years—so many products require regular re-calibration, which may be inconvenient and poorly understood by users. Existing international standards for testing blood pressure monitors were built for cuffs and do not fully capture the quirks of devices that depend on sensors, algorithms, and calibration history. The review highlights new efforts, such as European and IEEE protocols, that add tests for posture, movement, day–night changes, and long-term stability. The authors also point to gaps: many prototypes are only tested in small, controlled groups, and few studies explore how often calibration is really needed in everyday life.
Where Future Home Monitoring Is Headed
Looking ahead, the authors envision blood pressure tracking that is continuous, almost invisible, and tightly connected to broader health data. Future systems may fuse signals from multiple sensors with medical records and symptom descriptions using large-scale AI models, offering personalized, context-aware estimates rather than one-size-fits-all numbers. New sensor types—from terahertz waves to photoacoustic imaging—could make pulse measurements more precise and more tolerant of differences in skin tone or body shape. At the same time, better testing rules and disease-focused studies will be crucial to proving which technologies work best for specific groups, such as pregnant women, older adults, or people with nighttime hypertension. For patients and clinicians, the core promise is simple: more comfortable and reliable blood pressure monitoring that fits seamlessly into daily life, making it easier to detect problems early and keep hearts healthier for longer.
Citation: Zheng, Z., Hao, H., Huang, Y. et al. Advances in principles and technologies of non-mechanical blood pressure monitoring. npj Cardiovasc Health 3, 7 (2026). https://doi.org/10.1038/s44325-025-00102-5
Keywords: cuffless blood pressure, wearable sensors, hypertension monitoring, noninvasive cardiovascular, deep learning health