Clear Sky Science · en
MRI of combination immunotherapy in an epithelial ovarian cancer preclinical model
Why This Matters for Women’s Health
Epithelial ovarian cancer is often discovered late and remains one of the deadliest cancers affecting people with ovaries. Many tumors come back even after surgery and chemotherapy, so researchers are urgently testing new ways to help the immune system fight this disease. This study explores a three-part experimental treatment and uses advanced MRI scans to watch, in real time, how immune cells move into ovarian tumors in mice. The work hints at how doctors might one day see whether an immunotherapy is working long before a scan shows the tumor has shrunk.
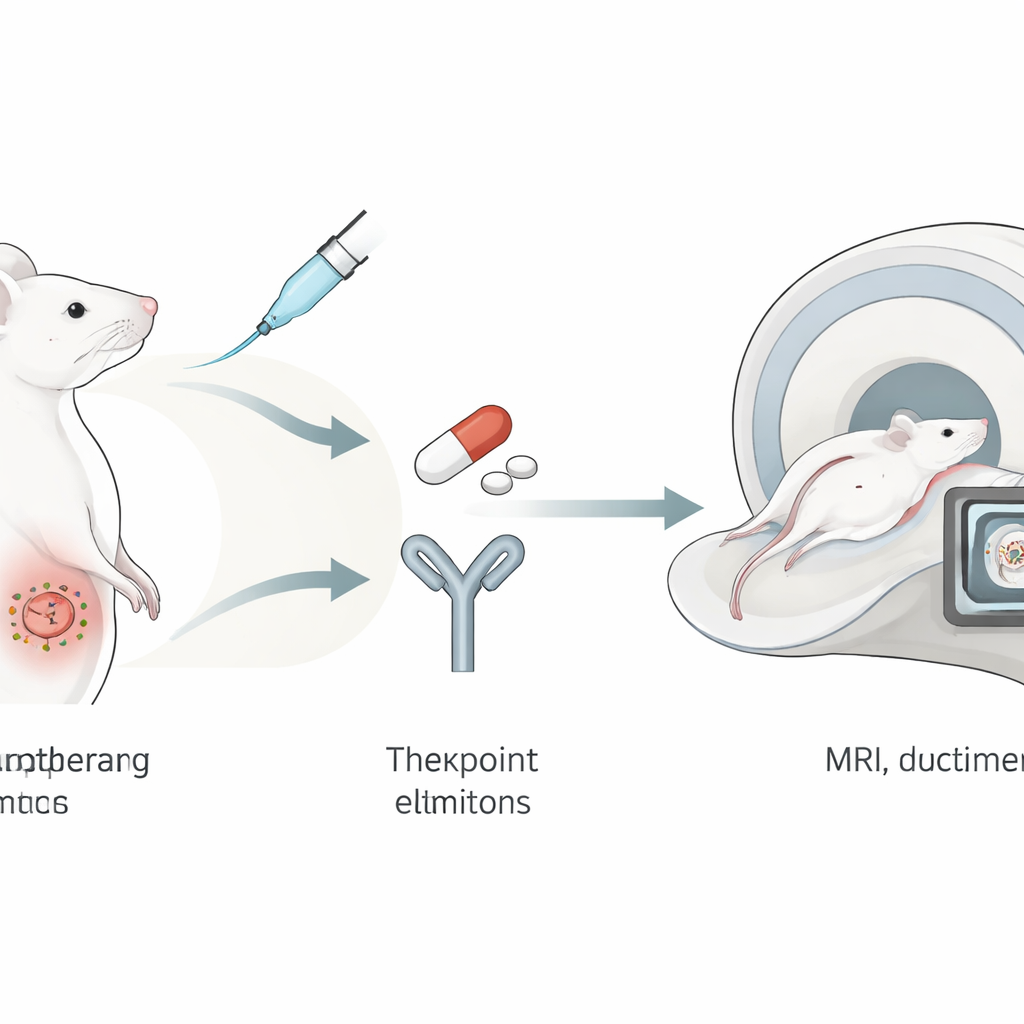
A Three-Drug Team Attack
The researchers tested a “triple therapy” in a mouse model designed to mimic human ovarian cancer. The first component was DPX-Survivac, a vaccine-like formulation that teaches immune cells to recognize survivin, a protein that helps cancer cells avoid self-destruction and is abundant in many tumors. The second was an immune checkpoint inhibitor that blocks PD-1, a molecular brake that tumors often use to switch off T cells. The third was an intermittent low dose of the chemotherapy drug cyclophosphamide, which can reduce suppressive immune cells that normally keep responses in check. Together, these agents were intended to free, train, and focus the immune system against ovarian tumors.
Watching Tumors Grow and Shrink
Because ovarian tumors grow deep inside the body, they are hard to monitor without imaging. In this study, the team used high-resolution MRI to measure tumor volume in each mouse several weeks after cancer cells were surgically implanted on the ovary. Across three scan dates, tumors in the treated mice stayed smaller than those in untreated animals, and by the final time point the difference in size and growth rate was statistically clear. While survival over the short study period did not differ, all animals had to be humanely euthanized at a fixed time for tissue analysis, so longer-term benefits could not be fully assessed. Nonetheless, the imaging results show that the triple therapy slowed the expansion of established ovarian tumors.
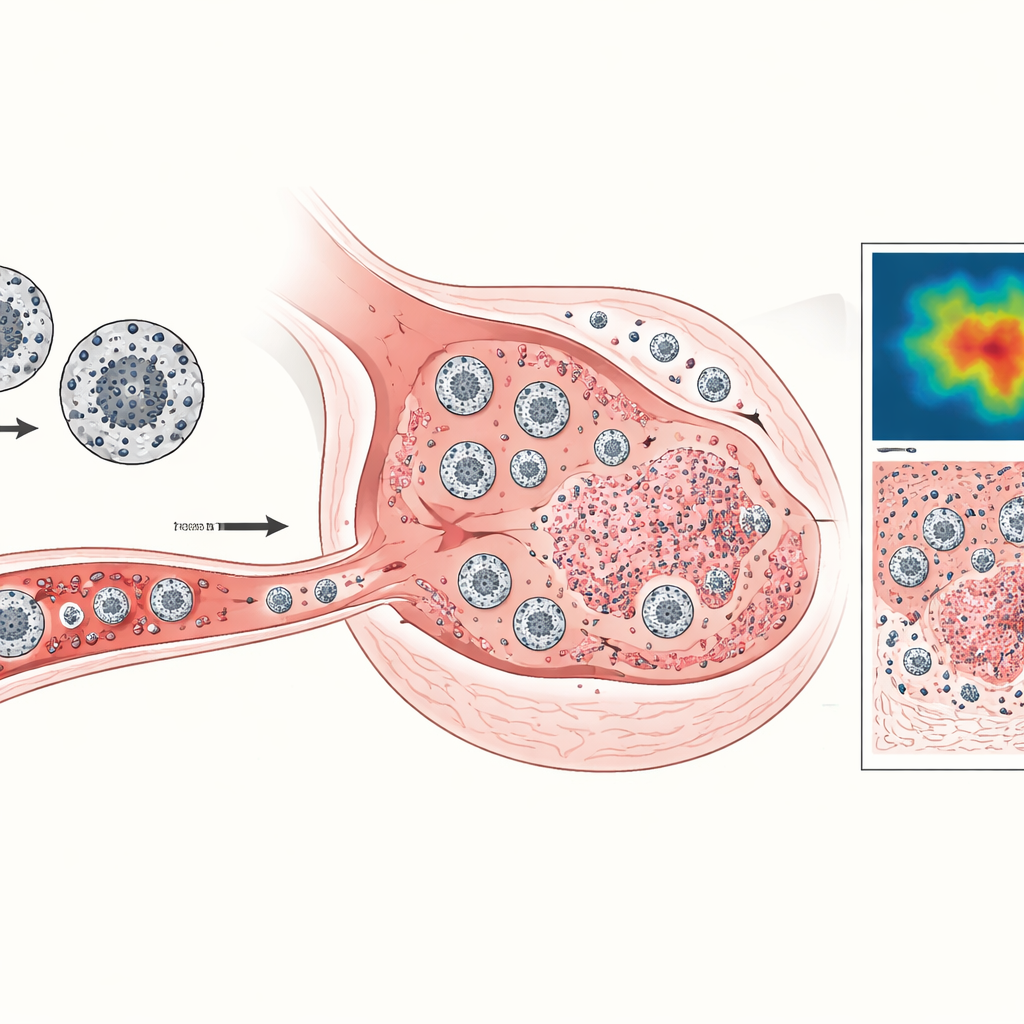
Tracking Immune Cells With Tiny Magnets
Beyond simply measuring tumor size, the scientists wanted to see whether helpful immune cells were actually reaching the cancer. They harvested two types of immune cells from donor mice: cytotoxic T lymphocytes, which can directly kill tumor cells, and a broader group of myeloid cells that can either support or suppress immune attacks. These cells were loaded with superparamagnetic iron-oxide nanoparticles—essentially tiny magnets—and infused into tumor-bearing mice. A specialized MRI method called TurboSPI then highlighted where iron-rich cells had gathered. By comparing the MRI signal with carefully calibrated standards, the team estimated how many labeled cells occupied each cubic millimeter of tumor or lymph node tissue at different times.
Immune Traffic in Tumors and Lymph Nodes
The imaging revealed that treated mice recruited substantially more iron-labeled killer T cells into their tumors than untreated mice, especially at later time points when tumors in the control group had grown rapidly and often contained almost no detectable T cells. Myeloid cells also appeared more frequently in tumors of treated animals, though their exact role—helpful or harmful—remains to be clarified. The team looked closely at groin lymph nodes, small immune hubs that drained either the tumor or the vaccine injection site. In treated mice, the node draining the DPX-Survivac vaccine consistently swelled more than the tumor-draining node, and this swelling was linked to smaller tumor sizes, suggesting strong immune activation in response to the vaccine. Flow-cytometry studies on tumor tissue and fluid in the abdomen supported the idea that treatment changed the balance of immune cells, reducing some suppressive or bystander populations and increasing the overall share of immune cells in the fluid where free-floating tumor cells can spread.
What This Could Mean for Future Care
Overall, the study shows that this three-part immunotherapy can slow ovarian tumor growth in mice and appears to do so by drawing more tumor-killing T cells into the cancer while stimulating immune activity in nearby lymph nodes. Just as important, it demonstrates that MRI can be used not only to size up tumors but also to track the journey of therapeutic immune cells throughout the body. If similar techniques can be adapted for people, doctors might one day use noninvasive scans to see early on whether a complex immunotherapy is rallying the right cells to the right place, helping them tailor treatments more precisely for patients with ovarian cancer.
Citation: Gosse, J.T., Skelton, C.S., Tremblay, ML. et al. MRI of combination immunotherapy in an epithelial ovarian cancer preclinical model. npj Imaging 4, 25 (2026). https://doi.org/10.1038/s44303-026-00157-8
Keywords: ovarian cancer, immunotherapy, MRI cell tracking, cancer vaccine, checkpoint inhibitor