Clear Sky Science · en
Predictive modeling of chronic foot ulcer outcomes using longitudinal photoacoustic imaging
Why stubborn foot wounds matter
For people with diabetes or poor circulation, a small sore on the foot can quietly turn into a chronic ulcer that refuses to heal. These wounds are painful, hard to treat, and a major reason for hospital stays and amputations. Doctors know that blood flow in the tiny vessels of the foot is key, but current tests give only rough clues about how well tissue is nourished with oxygen. This study introduces a new way to look under the skin—using light and sound—to track how blood vessels around foot ulcers change over time and to predict whether a wound is on the road to recovery or getting worse.
A new way to see blood flow
The researchers used a technique called photoacoustic imaging, which shines safe laser light into the foot and then “listens” with an ultrasound detector for the tiny sound waves created when blood absorbs that light. From these signals, a computer builds detailed three-dimensional pictures of blood vessels just beneath the skin. The team designed a scanner that images the top (dorsal) side of the foot, where many ischemic ulcers occur, and added a comfortable foot holder and adjustable mount so that each patient could be scanned in nearly the same way during repeat clinic visits. They also developed a method to digitally remove strong reflections from the skin surface so that deeper vessels stand out more clearly.
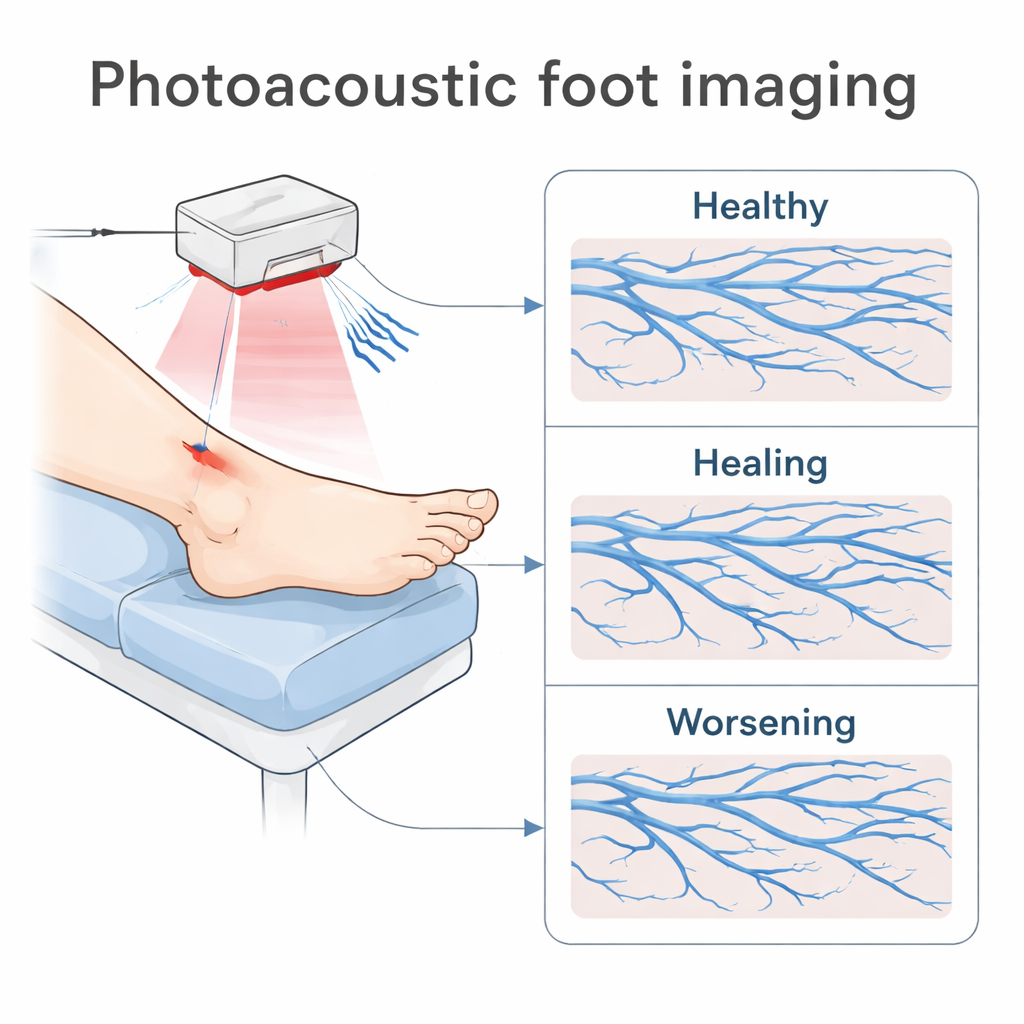
Turning images into trackable numbers
Instead of relying on visual impressions alone, the scientists converted each 3D image into a set of measurable “biomarkers” describing the brightness, texture, and shape of the vessels and surrounding tissue. In total they defined 45 such features, including how much of the region is filled with vessels, how sharp the vessel edges are, how tangled or orderly the vessel network appears, and how varied the signal is within vessels and tissue. Each patient—39 people with chronic foot ulcers and 24 volunteers without active disease—was scanned at least twice. For every person, the researchers focused on change over time by subtracting the first scan’s measurements from the second. This allowed them to see whether a given feature increased, decreased, or stayed stable within the same foot, reducing the impact of natural differences between individuals.
Teaching a computer to spot healing patterns
To find which features carried the most useful information, the team used a statistical method that automatically favors a small, focused set of predictors. From the original 45, it selected 12 key features that best distinguished three groups: ulcers that were healing, ulcers that were worsening, and healthy feet. These features reflected both how full the vascular bed was and how complex or irregular the vessel patterns were. The researchers then trained a machine-learning classifier to assign each subject to one of the three groups based solely on how their photoacoustic features changed between visits. Tested on unseen subjects, this system correctly labeled the outcome about four times out of five and showed strong separation between the three categories. Notably, the model never confused a worsening case with a healing one, an important safety consideration for clinical use.
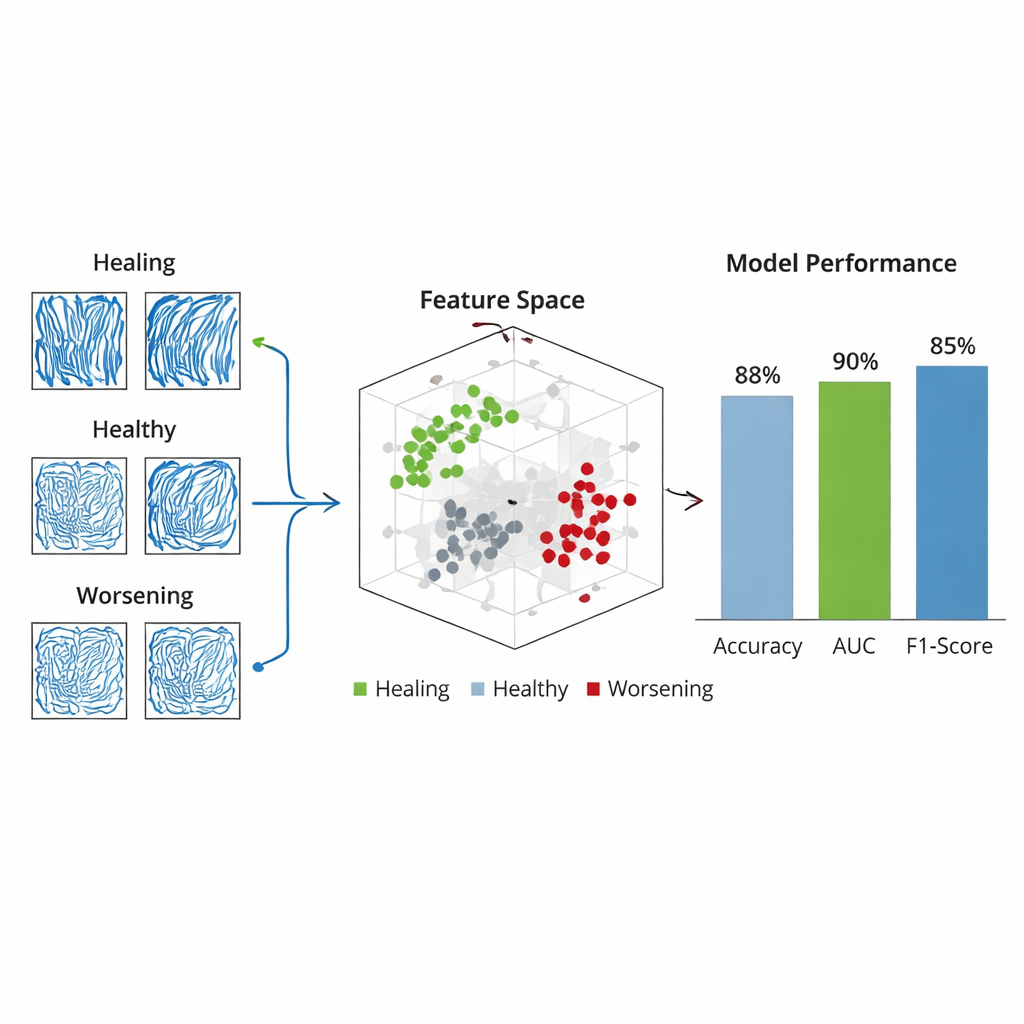
Connecting vessel changes to real-world healing
When the team looked more closely at individual features, the trends matched what doctors expect from wound biology. In people whose ulcers improved, the fraction of the region occupied by vessels generally rose, vessel edges became sharper, and local signal variation increased—signs of growing and remodeling blood networks. In those who worsened, vessel occupancy dropped, branches appeared more broken and sparse, and the overall pattern became more chaotic, consistent with progressive loss of blood supply. Healthy volunteers showed only small, random fluctuations over time, confirming that the system is stable when the underlying circulation does not change. Case studies of six representative subjects—two healthy, two healing, and two worsening—demonstrated that the model’s predictions aligned with physicians’ assessments based on standard tests and physical examination.
What this could mean for patients
In everyday practice, clinicians now rely heavily on visual inspection, ankle or toe blood-pressure ratios, and experience to judge whether a foot ulcer is getting better. These tools can miss early warning signs, especially in people with diabetes whose arteries are stiff or heavily calcified. This study shows that photoacoustic imaging can provide a noninvasive, repeatable, and quantitative view of how microvessels in the foot change over time. By turning rich 3D images into a small set of meaningful numbers, and combining them with machine learning, the approach offers an early indicator of whether a wound is healing or drifting toward trouble. While larger multi-center trials are still needed, this work lays the groundwork for personalized ulcer monitoring, better risk stratification, and more timely treatment decisions that could ultimately help patients keep their feet—and their independence.
Citation: Cheng, Y., Huang, C., Yu, Sl. et al. Predictive modeling of chronic foot ulcer outcomes using longitudinal photoacoustic imaging. npj Imaging 4, 12 (2026). https://doi.org/10.1038/s44303-026-00143-0
Keywords: chronic foot ulcers, photoacoustic imaging, diabetes complications, wound healing monitoring, vascular perfusion