Clear Sky Science · en
State of the science and research opportunities on dietary patterns in endometriosis and uterine fibroids
Why Everyday Food Choices Matter for Uterus Health
Many people think of endometriosis and uterine fibroids as mysterious conditions that just “happen” to the uterus. This review article argues that what we eat every day may play a meaningful role in how often these conditions occur and how severe their symptoms become. Because endometriosis and fibroids affect tens of millions of women worldwide—often causing pain, heavy bleeding, fertility problems, and missed work—understanding the link between diet and uterine health matters for almost every family.
Common but Overlooked Uterus Conditions
Endometriosis occurs when tissue similar to the uterine lining grows outside the uterus, forming implants and lesions that can trigger chronic pain, inflammation, and fertility problems. At least one in ten women of reproductive age is affected, yet symptoms are often dismissed, leading to years-long delays in diagnosis and treatment. Uterine fibroids are benign muscle tumors that grow in the wall of the uterus; by age 50, they affect up to 70 percent of white women and more than 80 percent of Black women in the United States. Both conditions hit women from marginalized racial, ethnic, and low-income groups especially hard, reflecting deeper inequities in exposure to risk factors, access to specialists, and timely care.
How Diet Connects to Hormones and Inflammation
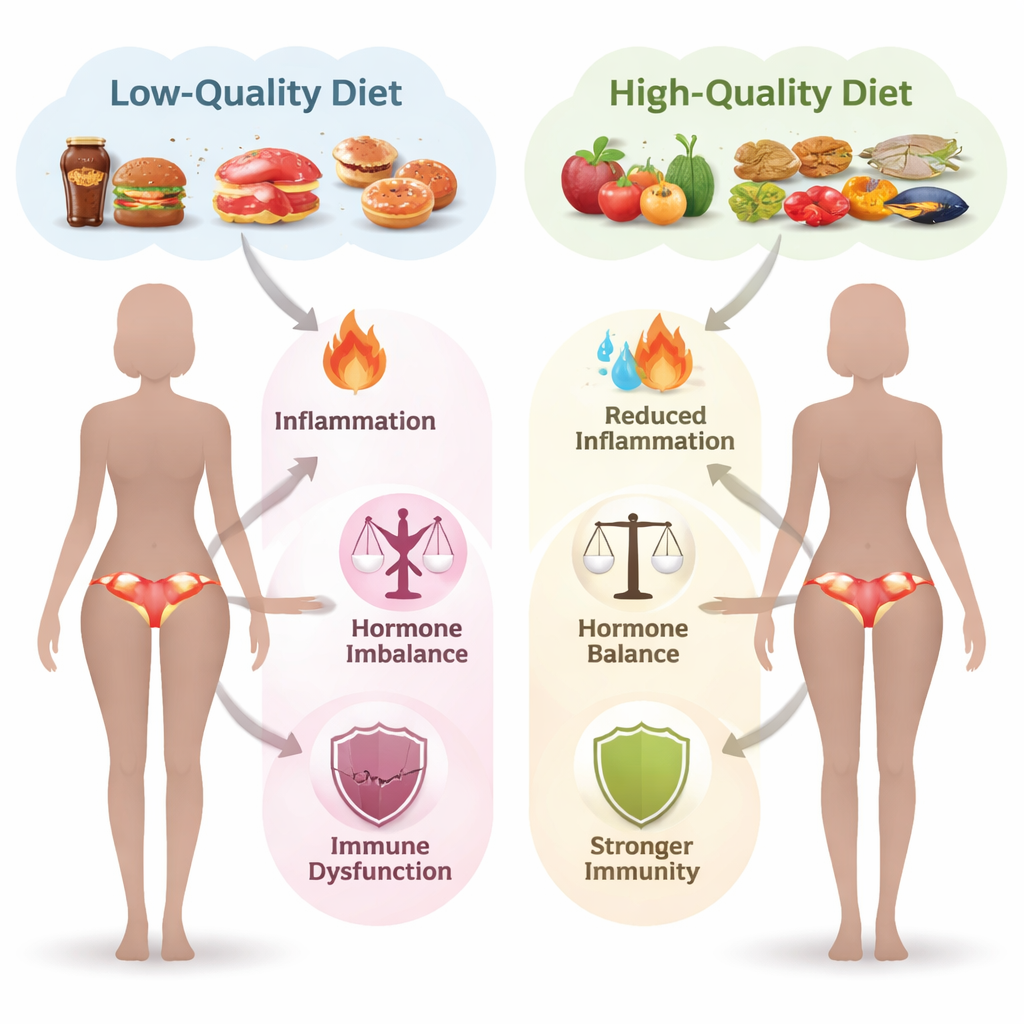
The authors explain that endometriosis and fibroids share three core biological drivers: immune system dysfunction, chronic inflammation, and sex hormone imbalance, especially the activity of the estrogen hormone estradiol. Low-quality diets heavy in red and processed meats, sugary drinks, refined grains, and ultra-processed snack foods tend to raise inflammation in the body and worsen metabolic problems like obesity and type 2 diabetes. These changes can increase circulating estrogens and create a body environment that favors growth of endometriosis lesions and fibroid tumors. In contrast, high-quality diets rich in fruits, vegetables, whole grains, healthy fats, and fiber support better hormone metabolism, help remove excess estrogen through the digestive tract, and can calm overactive immune responses.
What the Studies Show So Far
The review pulled together 11 studies on dietary patterns and endometriosis and just one on fibroids, underscoring how little research has been done. Overall, women whose eating patterns looked more like a “Western diet” or scored higher on a “pro-inflammatory” diet index had a higher chance of being diagnosed with endometriosis. On the other hand, women who scored higher on healthy eating indexes—such as the Harvard-style Alternative Healthy Eating Index or the MIND diet, which blends Mediterranean and blood-pressure-lowering DASH principles—tended to have lower odds of endometriosis. Several small intervention trials tested specific patterns, like a gluten‑free diet, a low‑FODMAP plan used for digestive complaints, and a Mediterranean diet. These studies suggest that changing what women eat can sometimes reduce pain, improve bowel symptoms, and modestly boost quality of life, although results were mixed and sample sizes were small.
Gaps, Limits, and Future Directions
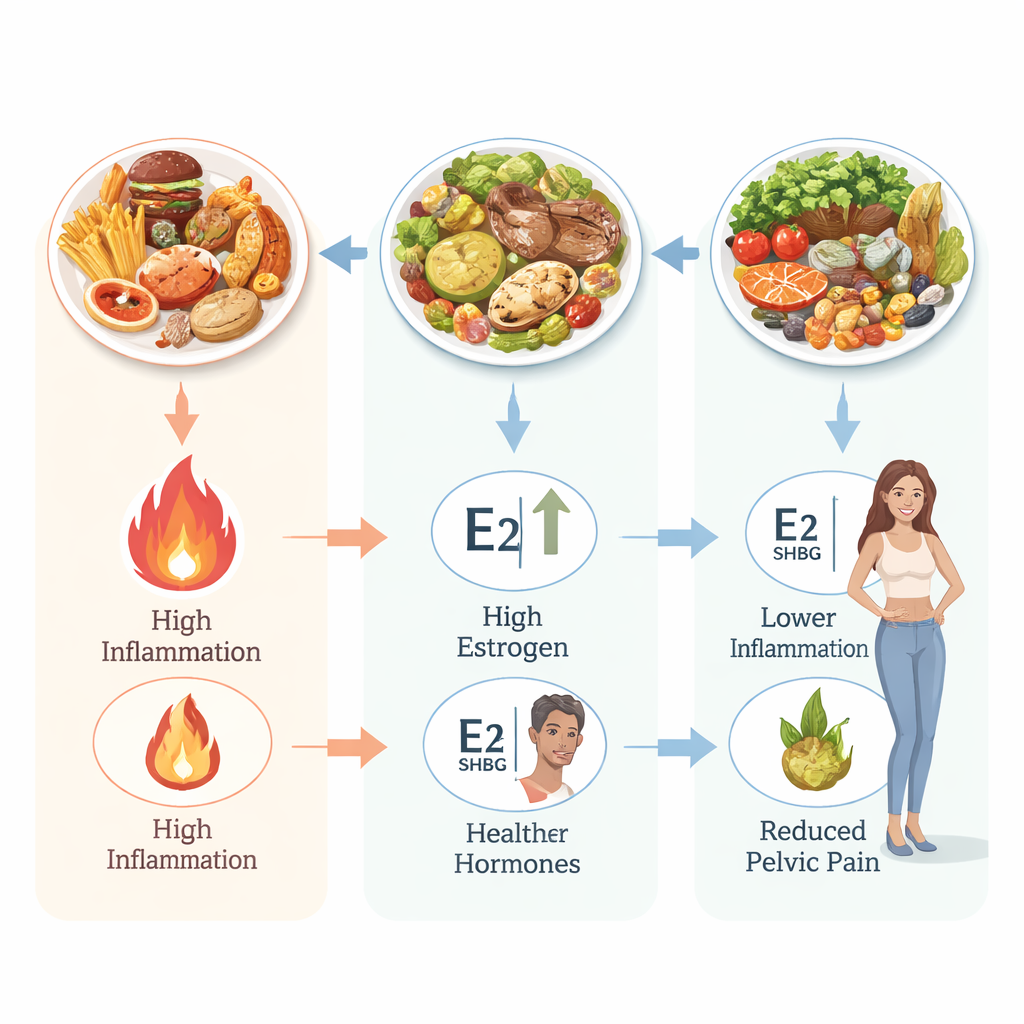
Evidence for fibroids is especially thin: only one large Taiwanese study looked at a self‑reported vegetarian diet and found no clear link with fibroid prevalence. The authors caution that “vegetarian” can still include many low‑quality processed foods, and that details on what participants actually ate were limited. Across all the studies, common problems included recall errors in food surveys, short follow‑up times, small or highly selected groups of participants, and few randomized controlled trials. Very few studies were designed to capture the experiences of racially and economically diverse women or to explore whether diet-based approaches feel realistic and acceptable in everyday life. The authors argue for future trials that are better designed, longer in duration, and intentionally inclusive, paired with interviews and focus groups to understand what women and their clinicians really want and can sustain.
What This Means for Everyday Life
For lay readers, the take‑home message is not that a single “miracle diet” can cure endometriosis or fibroids, but that overall eating patterns may nudge the odds and intensity of these conditions. Diets built around whole, minimally processed foods—plenty of plants, healthy fats, and fiber—appear to align with lower inflammation, more stable hormones, and in some cases less pain and better day‑to‑day functioning. At the same time, ultra‑processed foods and sugary, high‑fat options may fuel the biological pathways that let uterine lesions and tumors thrive. Because current research is still limited, women interested in trying dietary changes should work with health professionals, especially when symptoms are severe. With more rigorous and inclusive studies, food could become a more central, evidence‑based tool alongside medical and surgical care to support uterine health.
Citation: Fresco, T.M., Tussing-Humphreys, L.M., Kim, S.J. et al. State of the science and research opportunities on dietary patterns in endometriosis and uterine fibroids. npj Womens Health 4, 12 (2026). https://doi.org/10.1038/s44294-026-00133-y
Keywords: endometriosis, uterine fibroids, dietary patterns, inflammation, women's health