Clear Sky Science · en
The acceptability and feasibility of a contextualised group-based maternal mental health intervention in Kenya
Why Mothers’ Minds Matter
Pregnancy is often portrayed as a joyful time, but for many women it also brings anxiety, sadness, and overwhelming stress. In countries with few mental health professionals, these struggles are frequently ignored, leaving both mothers and babies at risk. This study from rural western Kenya explores a simple idea with big promise: can trained community health workers lead small group sessions that help pregnant women manage emotional distress as part of routine maternity care?
Hidden Burden Behind the Baby Bump
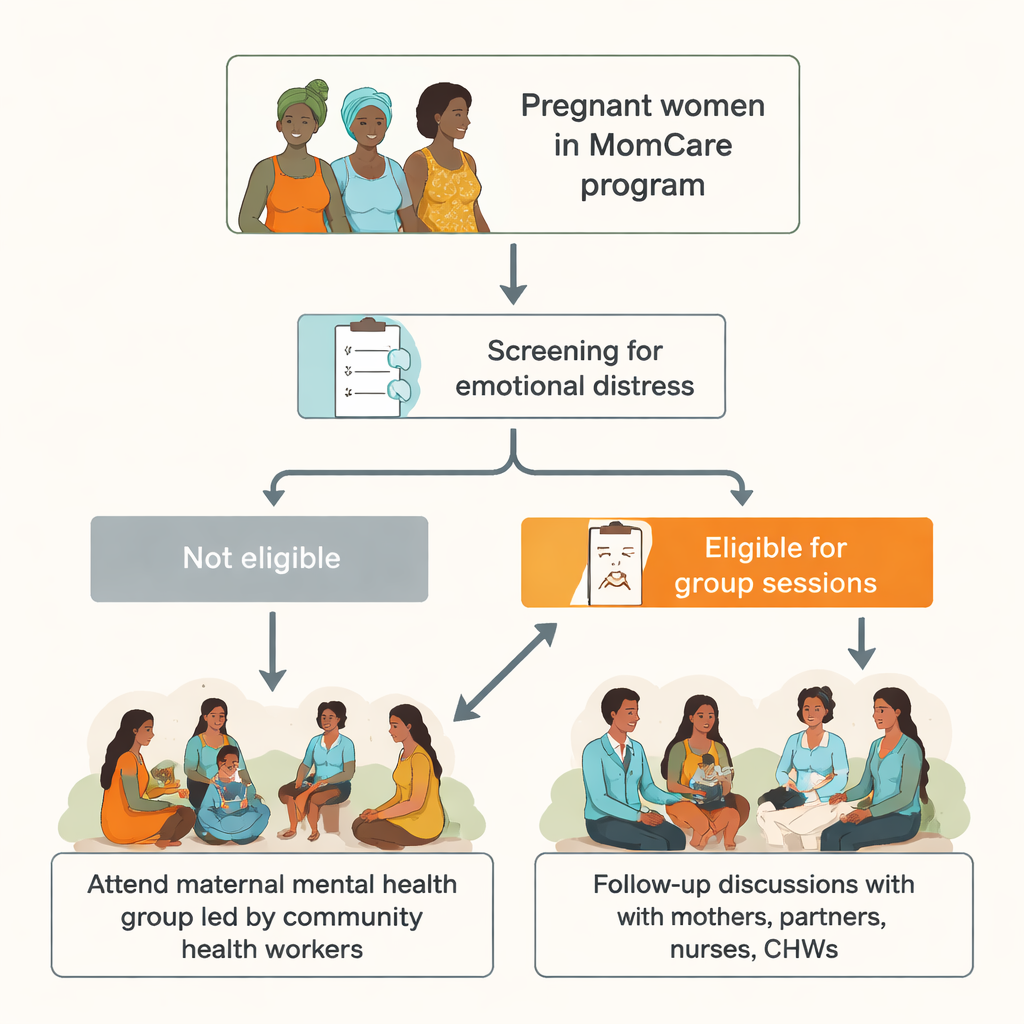
The researchers worked within MomCare, a program that supports low-income pregnant women attending public clinics in Kisumu County. Among 401 women who came for their first antenatal visit, more than one in three screened positive for signs of depression—higher than previous national estimates. Many described crying easily, feeling tense or resentful, worrying about money, fearing pregnancy complications, and lacking support from their partners. These emotional struggles are not just uncomfortable; left unaddressed, they can increase the risk of birth problems, suicide, and long-term difficulties for children.
A Group Approach Led by Neighbors
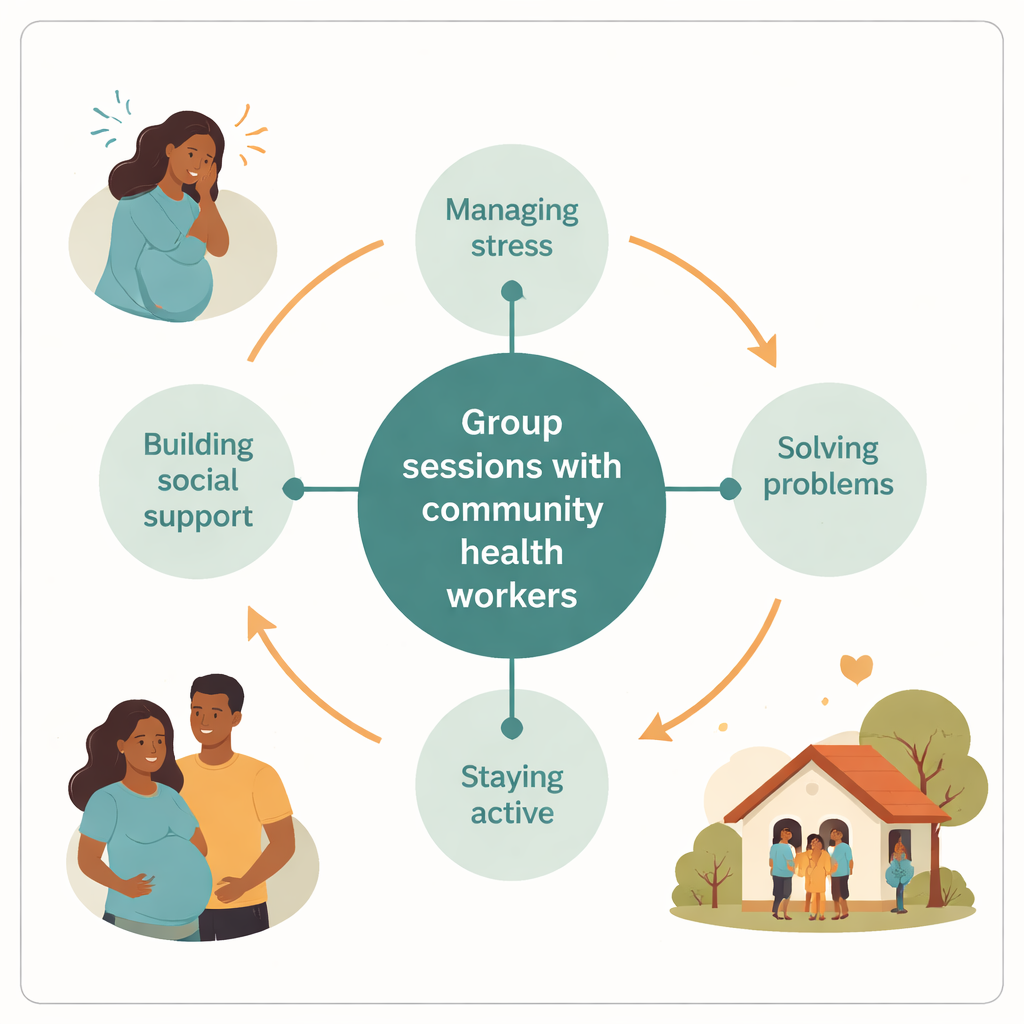
To respond, the team adapted a low-cost, five-session group course based on a World Health Organization method called Problem Management Plus. Instead of relying on scarce specialists, they trained local community health workers—people already known and trusted in the villages—to act as facilitators. Small groups of up to ten pregnant women met every two weeks at their clinic, usually on Saturdays to avoid clashes with work and household chores. Sessions focused on practical skills: recognising stress, solving everyday problems, staying active in meaningful tasks, and building supportive relationships. The language, stories, and even the drawings used in the materials were reshaped to match local ways of talking about distress.
What Participation Looked Like
Of the 143 women who screened positive and were invited, about 55 percent attended at least one session, and four in ten came to at least four of the five meetings. Attendance improved when the schedule was shifted to weekends, transport costs were reimbursed, and reminder calls were made. Women said they valued being able to bring their babies, though many wished for help with child care during discussions. Screening tools showed that those with more severe symptoms were actually less likely to attend all sessions—highlighting that the women most in need can also face the biggest barriers, such as low energy, long travel distances, or lack of partner support.
Voices from Mothers, Partners, and Health Workers
After the pilot, the team held group interviews with mothers, their partners, community health workers, and clinic nurses. Women reported feeling less alone and more hopeful once they heard that others faced similar worries. They described using new techniques—like pausing to breathe during arguments, choosing calmer words, and seeking help from friends or family—to ease tension at home. Partners noticed fewer quarrels and more open conversations, and several asked for their own classes to better understand what pregnant women go through. Community health workers felt proud of their new role and more confident talking about mental health, though they requested more training for handling sensitive topics such as violence. Nurses strongly supported the idea but felt sidelined, since they were involved mainly in initial screening and not in running the groups.
From Pilot Project to Everyday Care
Overall, the study found that a contextualised, group-based mental health program can fit well within routine antenatal care, even in places with deep stigma around mental illness. The approach was acceptable to women, their families, and health staff, and it was practically feasible when transport, timing, and good communication were addressed. While this pilot was not designed to prove long-term health benefits, early signs and participant stories suggest that such groups can ease distress, strengthen relationships, and help mothers feel more in control. For a lay reader, the takeaway is straightforward: with the right support and thoughtful adaptation, neighbors trained as community health workers can offer powerful, low-cost emotional support to pregnant women—improving not only their mental well-being, but also the start in life for their children.
Citation: De Sanctis, T., Katuwal, S., Waiyaiya, E. et al. The acceptability and feasibility of a contextualised group-based maternal mental health intervention in Kenya. npj Womens Health 4, 7 (2026). https://doi.org/10.1038/s44294-026-00127-w
Keywords: maternal mental health, perinatal depression, community health workers, group therapy, Kenya