Clear Sky Science · en
Leveraging multimodal machine learning for accurate risk identification of intimate partner violence
Why hidden warning signs matter
Violence in a romantic relationship is often kept secret, even from doctors who see the injuries it causes. Yet medical records quietly store years of clues: repeated emergency visits, certain injury patterns, and notes about pain or anxiety. This study asks whether computers can read those clues sooner and more reliably than today’s simple screening questions, so that women at risk of intimate partner violence can be offered help long before a crisis point.
Turning everyday care into an early warning system
The researchers drew on electronic medical records from two large U.S. hospitals, focusing on women who had either enrolled in a domestic abuse intervention program or carried medical diagnoses related to intimate partner violence. For each of these women, they selected similar patients of the same age range and broad background who had no documented abuse, creating a carefully matched comparison group. From 2017 onward, every encounter these patients had with the hospital system contributed data—diagnoses, medications, imaging studies, vital signs, emergency visits, and clinical notes such as radiology reports or social worker summaries.
Teaching computers to read numbers and narratives
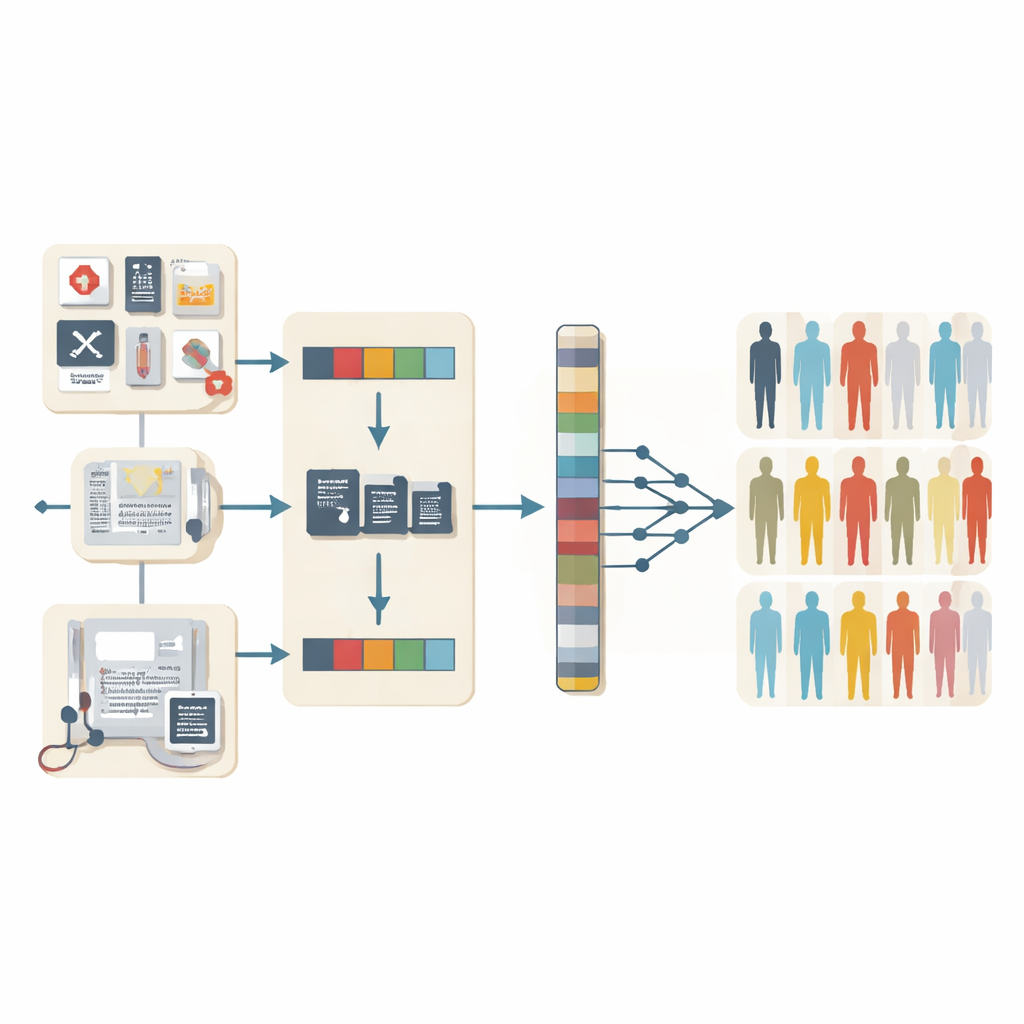
The team built three types of predictive models, each designed for a different level of data richness in real-world clinics. One model used only structured information, like diagnosis codes, prescription histories, and counts of specific imaging tests. A second model relied only on the free-text notes, which were converted into numerical representations using modern medical language models originally trained on millions of clinical sentences. The third, a “fusion” model, combined both sources: it distilled patterns from the tables and from the narratives, then fed the merged information into a machine-learning classifier. All models were trained to answer a daily question during each hospital contact: does this patient show signs that she may be experiencing intimate partner violence?
How well the risk signals worked
When tested on women not used during training, all three models were able to separate those with known abuse from their matched controls with high accuracy. Performance is summarized by a metric called AUC, where 1.0 is perfect and 0.5 is no better than chance. The tabular-only model reached an AUC of about 0.85, the notes-only model about 0.87, and the combined fusion model about 0.88. Crucially, these results held up when the models were applied to new groups: women who enrolled in the abuse program in later years, women at a second hospital in the same network, and women who had abuse-related diagnoses but never entered a specialized program. In all cases, the fusion model stayed above an AUC of 0.8, suggesting that blending numbers and text makes the system both accurate and stable across settings.
Seeing patterns years before women seek help
Beyond telling cases from controls, the models often recognized trouble long before women disclosed abuse to specialists. By comparing the first date on which the model flagged high risk with the date a woman entered the intervention program, the researchers found average “lead times” of more than three years, with many cases flagged over four or five years in advance. The combined model identified a larger share of future abuse cases early, while the tabular-only model sometimes gave slightly longer advance notice for those it did detect. An analysis of the structured features highlighted risk patterns that align with earlier clinical research: frequent emergency visits, certain upper-extremity imaging studies, high use of pain medications, mental health diagnoses, and signs of social hardship were all linked to higher predicted risk, whereas routine preventive screenings like mammograms tended to be associated with lower risk.
Using risk scores without taking away control
The authors stress that these tools are not meant to “diagnose” abuse or override a woman’s voice. Instead, they imagine the models running quietly in the background of electronic record systems, offering clinicians a private risk score that can prompt gentle, trauma-informed conversations and timely referrals to social and legal support. They also caution that the data reflect only women whose abuse was documented or who sought help, meaning that some groups remain underrepresented. Before broad deployment, hospitals will need to test performance in more general populations, monitor for bias, and design careful safeguards so that flagged scores lead to compassionate offers of help—not pressure or loss of autonomy. Used in this way, multimodal machine learning could turn everyday medical encounters into an earlier and more reliable gateway to safety for people facing violence at home.
Citation: Gu, J., Carballo, K.V., Ma, Y. et al. Leveraging multimodal machine learning for accurate risk identification of intimate partner violence. npj Womens Health 4, 15 (2026). https://doi.org/10.1038/s44294-025-00126-3
Keywords: intimate partner violence, electronic medical records, machine learning, multimodal data, early risk detection