Clear Sky Science · en
An international cohort study of breast cancer survival in young women
Why this research matters to young women
Breast cancer is often thought of as a disease of older women, but thousands of women in their 20s and 30s are diagnosed every year. This study asks a stark question: if a woman under 40 develops breast cancer, how much do her chances of surviving ten years depend on where in the world she lives? By pooling data on more than 36,000 young patients from six countries, the researchers show that survival can differ dramatically between nations—even when the cancers look similar on paper and receive broadly comparable treatments.
Young women, big impact
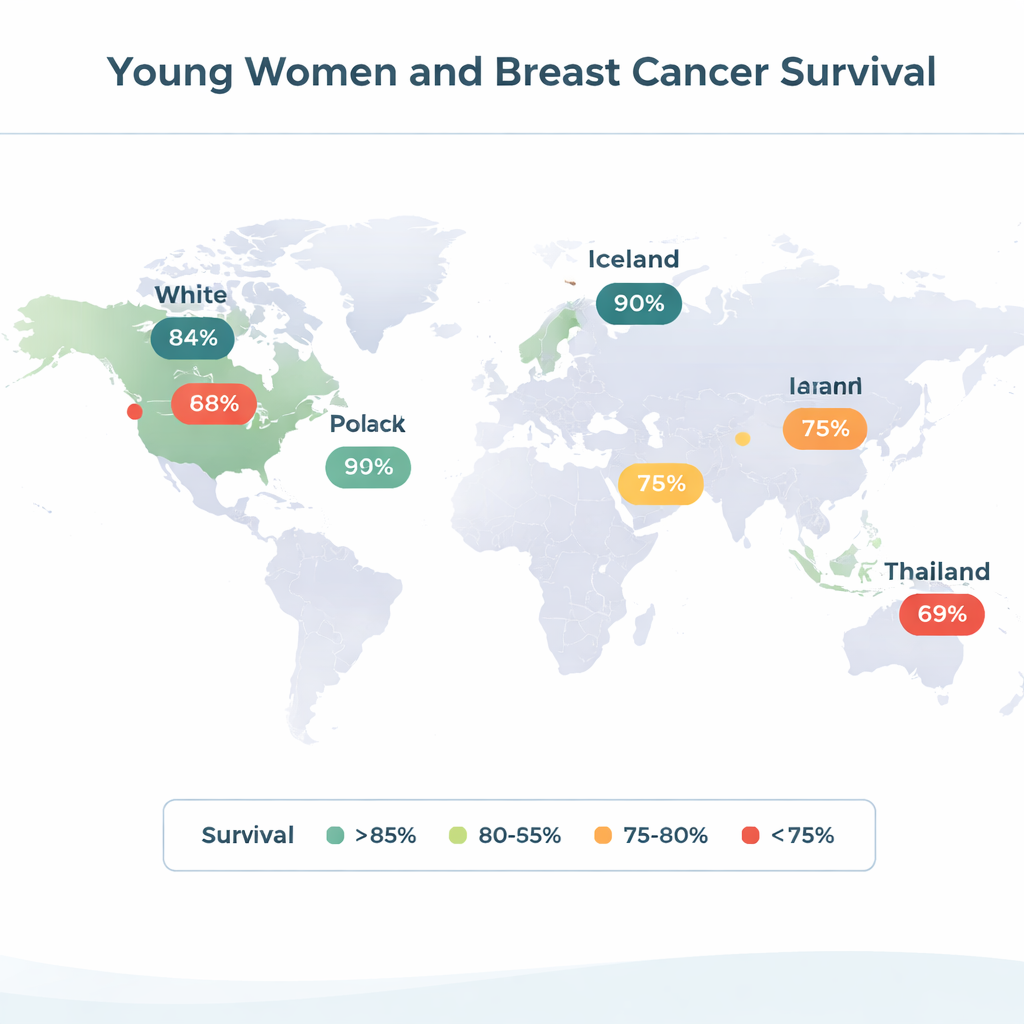
Breast cancer before age 40 is relatively rare, but its impact is outsized. These women often have more aggressive tumors, face difficult choices about fertility, early menopause, and long-term side effects, and lose more years of life when the disease is fatal. Because most national cancer statistics mix younger and older patients, it has been hard to see clearly which factors matter most for young women. To address this gap, researchers combined records from hospital databases and cancer registries in the United States, Canada, Poland, Iceland, Iran, and Thailand, focusing on women diagnosed between ages 20 and 39 from the late 1970s to 2020.
Tracking survival around the globe
The team analyzed 36,861 women and followed them for a median of just over eight years, long enough to estimate both five- and ten-year overall survival. They compared basic tumor features—such as size, spread to lymph nodes, and hormone-sensitivity—as well as treatments like chemotherapy, radiotherapy, and hormonal drugs. The headline finding is sobering: ten-year survival ranged from about 52% in Thailand to nearly 78% in Poland. White women in the U.S. and women in Iceland also did relatively well, while Canada, Thailand, and Black women in the U.S. had notably poorer outcomes. Even when women with incurable, stage IV disease were excluded, the ranking of countries changed little.
Looking past stage and treatment
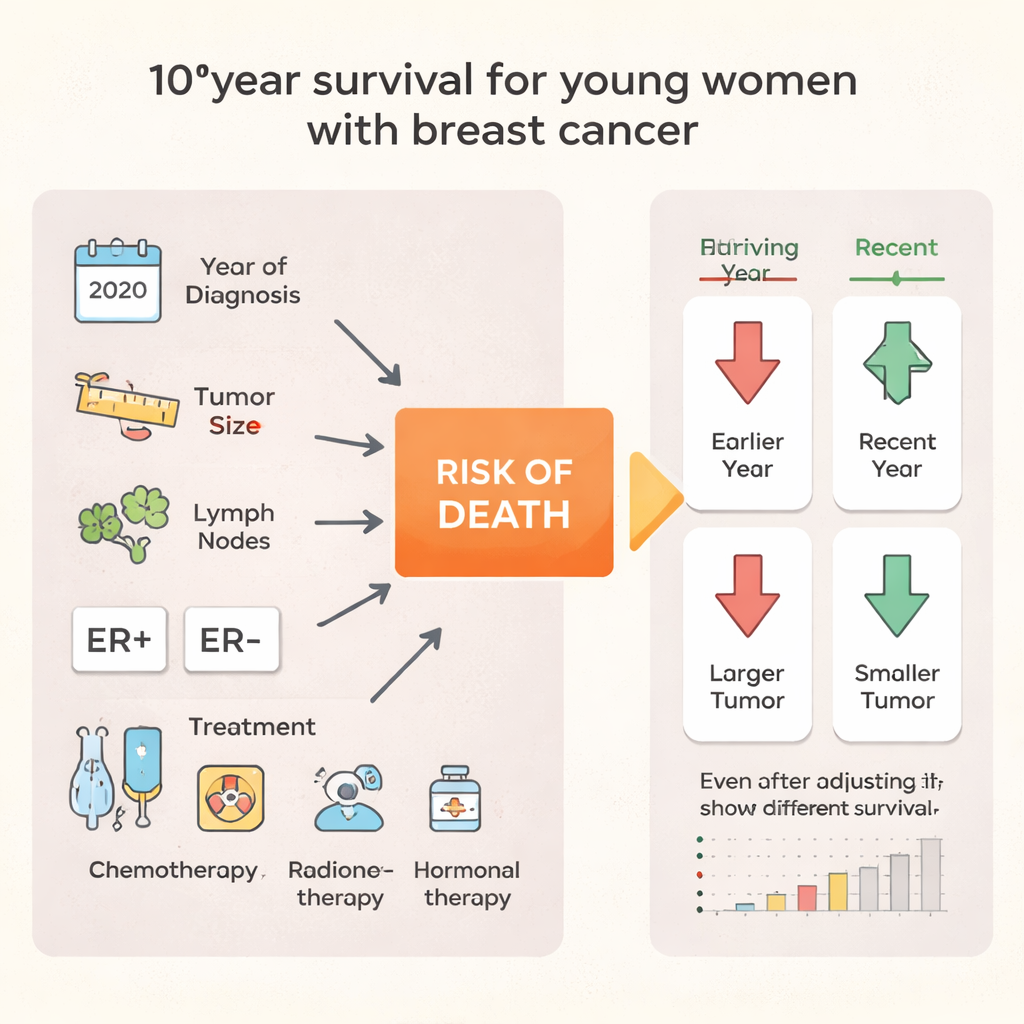
At first glance, it would be easy to assume that women fare worse in some countries because their cancers are caught later or because they receive less therapy. The study did find that the share of women diagnosed at the earliest stage varied widely—from about 12% in Thailand to 35% in Poland—and that chemotherapy and hormonal drug use differed by country. Yet, when the researchers used statistical models to adjust for year of diagnosis, tumor size, lymph node involvement, hormone receptor status, and whether women received chemotherapy and radiotherapy, a two-fold gap in death rates between centers remained. The disparity was even more striking for women with stage I disease, where survival after ten years varied by roughly four-fold between countries, despite these cancers being considered “early” and highly treatable.
Time trends and unequal progress
One bright spot is that outcomes have improved over the past few decades. Across all centers combined, ten-year survival rose from about 66% for women diagnosed in 1970–1995 to roughly 75% for those diagnosed in 2011–2015. This improvement occurred even though tumors tended to be slightly larger and more often stage IV in later years, suggesting that advances in systemic therapies and hormonal treatments are making a real difference. However, these gains have not been shared equally. In particular, Black women in the U.S. had substantially worse survival than White women, and that gap persisted even after accounting for tumor characteristics and recorded treatments—pointing to deeper issues such as differences in tumor biology, access to high-quality care, or treatment completion.
What this means for patients and policy
For a young woman facing breast cancer, this study carries a double message. First, modern treatment has improved survival over time, and many women with early-stage disease now live at least a decade after diagnosis. Second, where she lives—and potentially her ethnic background—still influences her odds in ways that current clinical measures cannot fully explain. The authors conclude that differences in screening, stage at presentation, and standard treatment patterns are not enough to account for the international gaps they observed. They argue that more detailed research into care quality, treatment adherence, newer drugs, and genetic and ethnic factors is urgently needed. Until then, the work underscores that closing the survival gap for young women with breast cancer will require more than simply applying existing guidelines—it will demand tailored strategies that ensure effective, equitable care across diverse health systems.
Citation: Sopik, V., Lubiński, J., Gronwald, J. et al. An international cohort study of breast cancer survival in young women. BJC Rep 4, 6 (2026). https://doi.org/10.1038/s44276-026-00207-z
Keywords: young women breast cancer, international survival disparities, early-onset cancer outcomes, breast cancer treatment patterns, global oncology