Clear Sky Science · en
Enhancing quality of antimicrobial prescribing through ‘Ask Eolas’ (language model): a user-testing and simulation evaluation
Why smart prescribing matters to everyone
Antibiotics have saved countless lives, but overuse and misuse are helping dangerous bacteria evolve into drug‑resistant “superbugs.” This silent crisis threatens routine surgery, cancer treatment, and even simple infections. The study behind this article tests a new artificial‑intelligence helper called Ask Eolas, designed to guide doctors toward safer, more accurate antibiotic choices. By seeing whether this tool cuts down on mistakes in realistic test cases, the researchers ask a question that affects all of us: can trustworthy AI help protect antibiotics for the future?
A digital assistant for everyday treatment decisions
Ask Eolas is built into a medical app already used in most hospitals in England to access local treatment guidelines. Instead of forcing clinicians to scroll through long documents or complex flowcharts, the new feature lets them type questions in plain language, such as the right drug and dose for a particular infection. Behind the scenes, Ask Eolas searches only the hospital’s own antibiotic rules and then writes a short, tailored answer, along with links back to the original guidance so users can check the source for themselves. In this way, it acts less like a black‑box robot and more like an efficient assistant that knows where everything is filed.
Testing the tool in realistic hospital scenarios
To find out whether Ask Eolas actually improves prescribing, the researchers ran a controlled simulation study with 45 clinicians, including consultants, junior doctors, pharmacists, and prescribing nurses. Participants were randomly assigned to one of three options: traditional PDF guidelines on the hospital intranet, the existing Eolas guideline app, or the new Ask Eolas AI feature. Each person worked through 45 antibiotic‑prescribing cases that ranged from straightforward infections to complex situations involving resistance patterns and multiple health problems. For each case, the team checked whether the final prescription exactly followed hospital rules on the right drug, route, dose, duration, and attention to local resistance data.
Fewer errors, clearer answers, calmer minds
The differences between tools were striking. Clinicians using Ask Eolas made no prescribing errors at all across the test cases, while those using the app or PDF guidelines had error‑free prescriptions only 60% and 47% of the time, respectively. Put another way, for every two clinicians who switched from PDFs to Ask Eolas, one extra patient would receive a completely correct prescription. Most mistakes with traditional tools were not wild misjudgments but subtle problems with dose or length of treatment—exactly the sort of details that can slip past tired staff scanning dense documents. Participants reported that Ask Eolas’ short, focused summaries, together with links to the original guideline sections, made it easier to trust and act on the advice.
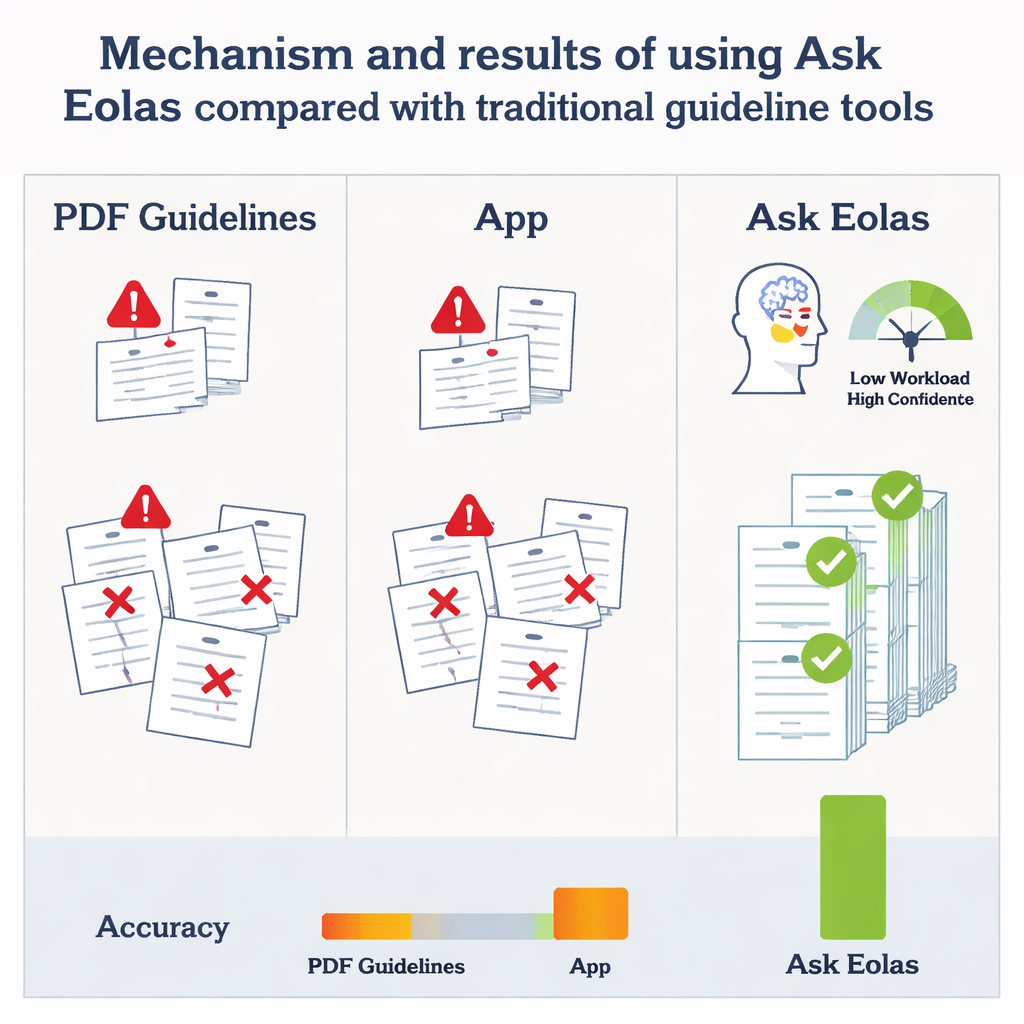
Designing AI that people actually want to use
Beyond accuracy, the study looked at how it feels to work with the tool. Using established questionnaires, clinicians said Ask Eolas was the easiest system to use, the one they would most like to use regularly, and the one that left them feeling most confident in their decisions. Measures of mental workload showed that the AI tool reduced time pressure, effort, and frustration compared with scrolling through PDFs or navigating a static app. Interviews revealed that users valued transparency—being able to see exactly which guideline passages the answer came from—and appreciated that the system adapted to individual patient details. Some downsides did appear, such as brief loading delays and differing tastes in how long replies should be, but these were seen as minor compared with the benefits.
From promising trial to real‑world practice
The authors caution that their evaluation took place in a safe, simulated environment rather than on busy hospital wards, and involved a relatively small number of participants at a single site. Real‑world pressures, varied hospitals, and live laboratory data could all change how the tool performs. To guide safe rollout, the team proposes a TRUST‑AI roadmap that stresses transparency, real‑time data links, user‑friendly design, strong safety safeguards, clear responsibility and audit trails, and smooth integration with electronic health records. Even with these caveats, the study offers early but encouraging evidence that carefully designed AI can help clinicians follow best‑practice antibiotic guidance more reliably, supporting both individual patients and the global fight against drug‑resistant infections.
Citation: Waldock, W.J., Gilchrist, M., Ashrafian, H. et al. Enhancing quality of antimicrobial prescribing through ‘Ask Eolas’ (language model): a user-testing and simulation evaluation. npj Antimicrob Resist 4, 16 (2026). https://doi.org/10.1038/s44259-026-00187-7
Keywords: antimicrobial resistance, antibiotic prescribing, clinical decision support, artificial intelligence in healthcare, large language models