Clear Sky Science · en
Integrating digital solutions improves mental health management in cancer care
Why Your Phone Might Belong in the Cancer Clinic
Being told you have cancer is not only a medical shock; it is an emotional earthquake. Many people face anxiety, low mood, sleep problems, and fear of the future, yet in-person counseling is hard to access, especially during busy treatment schedules or in remote areas. This review article explores how everyday digital tools—smartphones, wearables, video visits, and even virtual reality—are being turned into powerful allies to protect mental health in cancer care.
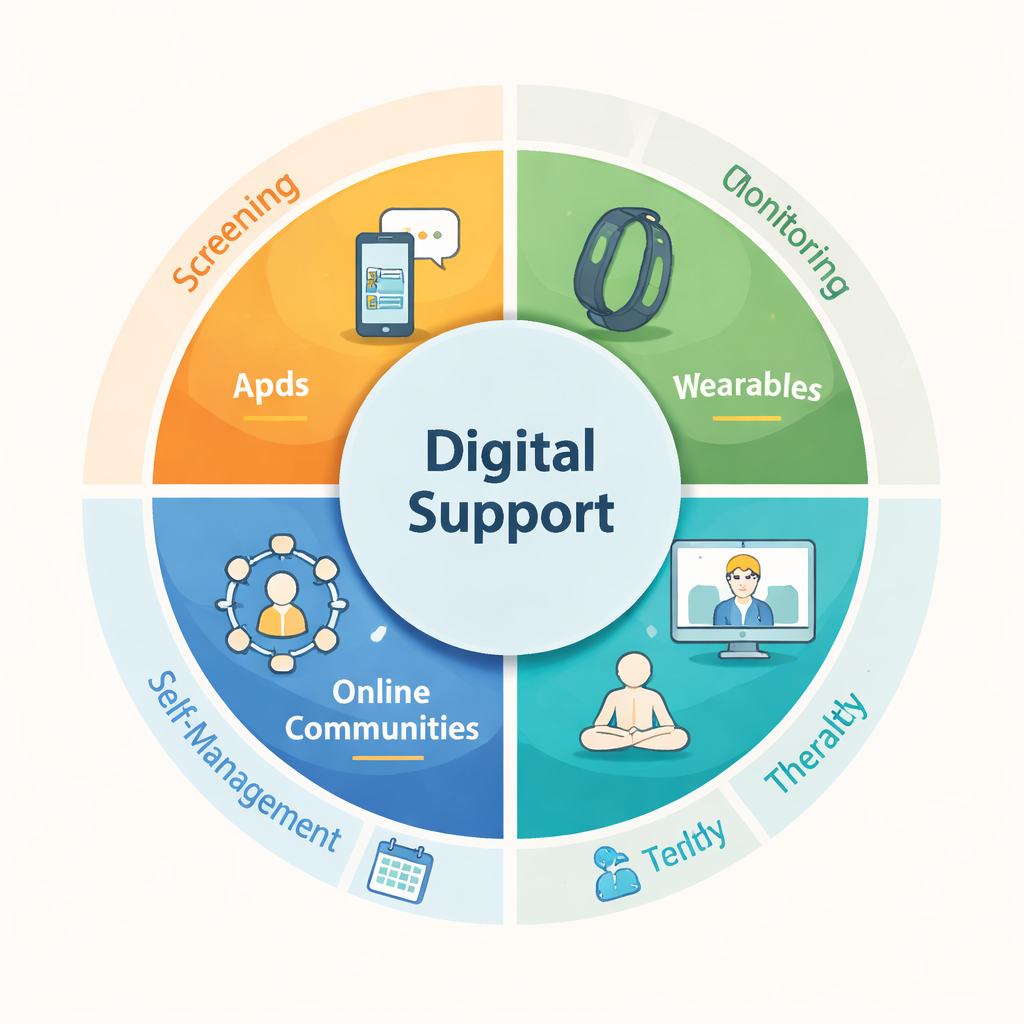
New Ways to Check In on How Patients Feel
Traditionally, doctors and nurses have relied on short clinic visits and paper questionnaires to ask about worries, mood, and sleep. Digital tools change this by allowing people to report their feelings from home through websites and mobile apps. Short check-ins sent to a phone several times a day can capture stress and mood in real time, rather than relying on distant memories. At the same time, fitness trackers and other wearables quietly collect information on steps, sleep, and heart rate. Because changes in activity often mirror changes in mood, these devices can give early warning that someone is struggling, even if they do not speak up directly.
From Information and Coaching to Real Therapy
Many cancer apps go beyond simple tracking to offer information and guided coping skills. Educational platforms explain diagnoses, treatments, and side effects in plain language, which helps reduce fear of the unknown. Others guide users through proven psychological methods like cognitive behavioral therapy—teaching people to spot unhelpful thoughts and replace them with more balanced ones—or mindfulness, which trains attention on the present moment to ease rumination. These programs can deliver short lessons, breathing exercises, and relaxation audio on demand, weaving emotional care into daily life instead of reserving it for rare clinic visits.
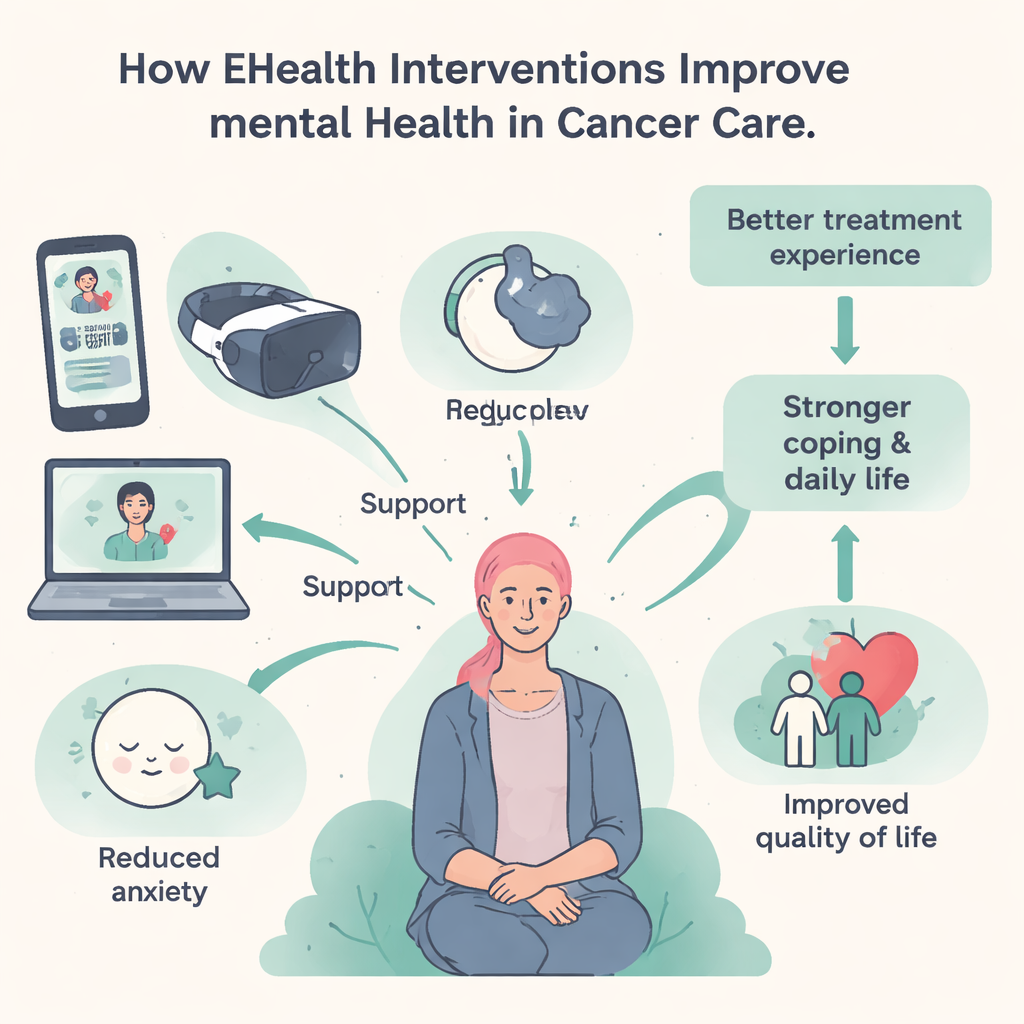
Video Visits, Virtual Worlds, and Online Communities
Telemedicine has opened the door for counseling sessions and follow-up visits by secure video, which is particularly useful for those who feel too tired to travel or live far from cancer centers. Receiving care from home can make it easier to talk about fears and pain. Virtual reality adds another layer: by immersing patients in calming scenes or engaging games, VR can distract from pain and reduce anxiety during difficult procedures or long infusions. Social media groups and online communities connect people who share a diagnosis, giving them a place to exchange tips, encouragement, and lived experience. For many, knowing that “someone else gets it” becomes an important lifeline.
What the Evidence Shows So Far
Across many types of cancer—including breast, lung, prostate, and gastrointestinal cancers—studies show that digital programs can modestly reduce anxiety, depression, stress, and pain, and can help people feel more in control of their illness. Some tools encourage physical activity, which is itself linked to better mood and energy. Others support self-management by helping patients track symptoms, side effects, and medication schedules, and by prompting timely contact with clinicians. These changes may improve quality of life and, by strengthening confidence and coping skills, can support better adherence to treatment. However, not all programs work equally well, and long-term benefits are still being studied.
Gaps, Risks, and the Road Ahead
The article also warns that digital care is not a magic fix. Older adults, people with limited internet access, or those unfamiliar with technology may be left behind, risking wider health gaps between rich and poor regions. Privacy and data security are major concerns, because mental health and cancer data are highly sensitive. Many apps on the market have not been carefully tested, and it can be hard for patients and clinicians to know which ones are trustworthy. The authors argue for better-designed clinical trials, stronger rules for data protection, and closer integration of digital tools with regular hospital systems so that information is not scattered across disconnected platforms.
What This Means for People Living with Cancer
Overall, the article concludes that digital health tools are reshaping how mental health is supported in cancer care. When chosen carefully and used alongside—not in place of—face-to-face care, apps, wearables, video visits, VR, and online communities can make help more constant, personal, and convenient. In the near future, advances in artificial intelligence and high-speed networks may allow even more tailored support, such as predicting who is at risk for emotional crises and offering just-in-time guidance. For patients and families, this means that a smartphone or wristband could become more than a gadget: it could be part of a continuous safety net for mind and mood during and after cancer treatment.
Citation: Lin, A., Zhang, Y., Jiang, A. et al. Integrating digital solutions improves mental health management in cancer care. Commun Med 6, 124 (2026). https://doi.org/10.1038/s43856-026-01448-2
Keywords: digital mental health, cancer survivorship, eHealth, telemedicine, mindfulness and CBT