Clear Sky Science · en
Pilot study of screening method for pancreatic cancer using lipidomic profiling of plasma or serum
Why this matters for you
Pancreatic cancer is notorious for being found too late, when treatment options are limited and survival chances are low. This study explores a simple blood test that looks at fat-like molecules in the blood to spot pancreatic cancer earlier and more accurately than current tools. If such a test can reliably flag the disease before symptoms appear, it could transform outcomes for people at risk and potentially save many lives.
A deadly cancer that hides in plain sight
Pancreatic ductal adenocarcinoma, the most common form of pancreatic cancer, is one of the deadliest cancers, with only about 13% of patients alive five years after diagnosis. The main reason is timing: tumors usually grow silently and are often discovered only when they have already spread. Today, doctors rely on imaging scans such as MRI, CT, and endoscopic ultrasound, as well as a blood marker called CA 19-9. These methods are expensive, sometimes invasive or uncomfortable, and importantly, they often miss early-stage disease. As a result, fewer than one in five patients are diagnosed when surgery has a real chance to cure them.
Reading the body’s fat fingerprints
Instead of hunting for a single cancer marker, the researchers focused on “lipidomics”—measuring many different lipids, the fat-like molecules that help build cell membranes and control cell signaling. Cancer cells rewire their metabolism, and that leaves a characteristic fingerprint in the mixture of lipids circulating in the blood. In this pilot study, blood samples (both plasma and serum) were prospectively collected from 488 adults in the Czech Republic: 177 people with pancreatic cancer, 218 healthy volunteers, and 93 individuals at high risk because of chronic pancreatitis, inherited syndromes, or strong family history. Using advanced mass spectrometry, the team quantified hundreds of lipid species and then used statistical models to see whether the overall lipid pattern could distinguish cancer from non-cancer.
How well the new blood test works
The researchers first examined how natural differences such as sex and the type of blood sample (plasma versus serum) affect lipid patterns. Men and women showed clear but manageable differences in certain lipid classes, so the team built separate models for each sex. Plasma and serum were largely similar, with plasma performing slightly better, so it became the preferred sample type. When they trained their models on lipid data from patients with pancreatic cancer and healthy controls, the test correctly separated the two groups with remarkable performance: in plasma, overall accuracy exceeded 95% in both training and independent validation sets. Sensitivity—the ability to detect cancer when it is present—was around 92–99%, while specificity—the ability to correctly label healthy people as cancer-free—was about 100% in the main analyses.
Early disease and high-risk individuals
Crucially, the lipid-based test worked just as well for early-stage tumors as for more advanced ones. This is where standard markers struggle most. CA 19-9, the current workhorse blood test, had sensitivities of only about 60–66% in the same group of patients, and another marker, CEA, performed even worse. By contrast, the lipid test maintained very high sensitivity across tumor stages, including small, potentially curable cancers and patients who naturally produce little CA 19-9. The team then applied their finalized models to the 93 high-risk individuals, whose pancreatic status was monitored using yearly MRI and/or endoscopic ultrasound. In this group, the lipid test correctly matched imaging-based findings in 96% of cases, with only a few borderline results and no known missed cancers during the follow-up period.
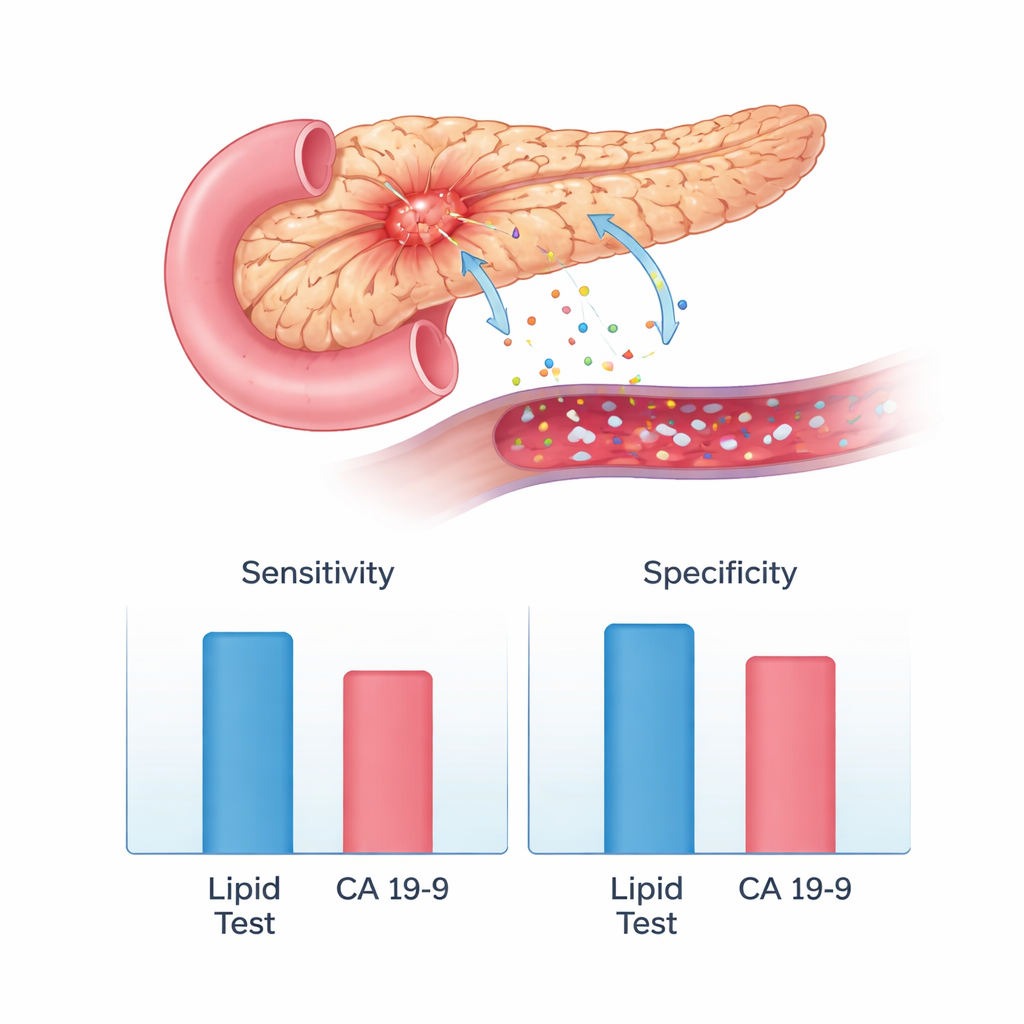
What this could mean for future screening
Because the test relies on a standard blood draw and automated analysis, it is noninvasive, high-throughput, and relatively inexpensive compared with imaging-based surveillance. Rather than depending on a single molecule, it reads a whole pattern of lipids, which seems more robust to natural biological variation. The study does note limits: it did not include people with other cancer types, so it is not yet clear how specific the pattern is for pancreatic cancer alone, and the number of high-risk individuals and length of follow-up were modest. Nonetheless, the striking accuracy, especially for early-stage disease and in people with low CA 19-9 levels, has prompted the launch of a larger multicenter clinical trial to confirm these findings.
A simple blood draw with life-saving potential
In plain terms, this work suggests that a carefully analyzed blood sample could one day act as a highly accurate early warning system for pancreatic cancer. By measuring a broad signature of lipid molecules rather than a single marker, the proposed test outperforms today’s standard blood assays and approaches the reliability of advanced imaging, while being gentler on patients and easier to repeat. If confirmed in larger studies, such a test could allow high-risk individuals to be screened more comfortably and frequently, catching dangerous tumors when they are still small, localized, and more likely to be cured.
Citation: Peterka, O., Jirásko, R., Dolečková, Z. et al. Pilot study of screening method for pancreatic cancer using lipidomic profiling of plasma or serum. Commun Med 6, 127 (2026). https://doi.org/10.1038/s43856-026-01445-5
Keywords: pancreatic cancer screening, blood-based biomarkers, lipidomics, early cancer detection, mass spectrometry