Clear Sky Science · en
Changes in temperature perception in transgender persons undergoing gender-affirming hormone therapy
Why feeling hot and cold is not the same for everyone
Most of us have argued about the thermostat: some people shiver while others feel perfectly fine. Scientists have long known that, on average, people assigned female at birth detect smaller changes in skin temperature than those assigned male at birth. But it has been unclear whether this difference is due mainly to hormones, genes, or other factors. This study takes advantage of gender-affirming hormone therapy in transgender people to watch, in real time, how shifts in sex hormones change the way the skin senses temperature.
Taking a closer look at temperature sensitivity
To explore this question, researchers in Germany followed four groups of adults over six months: transgender women (assigned male at birth, taking estrogen plus a testosterone blocker), transgender men (assigned female at birth, taking testosterone), and two control groups of cisgender women and men not receiving hormones. At three visits—before treatment, three months in, and six months in—the team measured how small a temperature change on the palm each person could notice, and when warm or cold sensations became painful. They also asked about everyday experiences of feeling hot or cold using a detailed questionnaire. 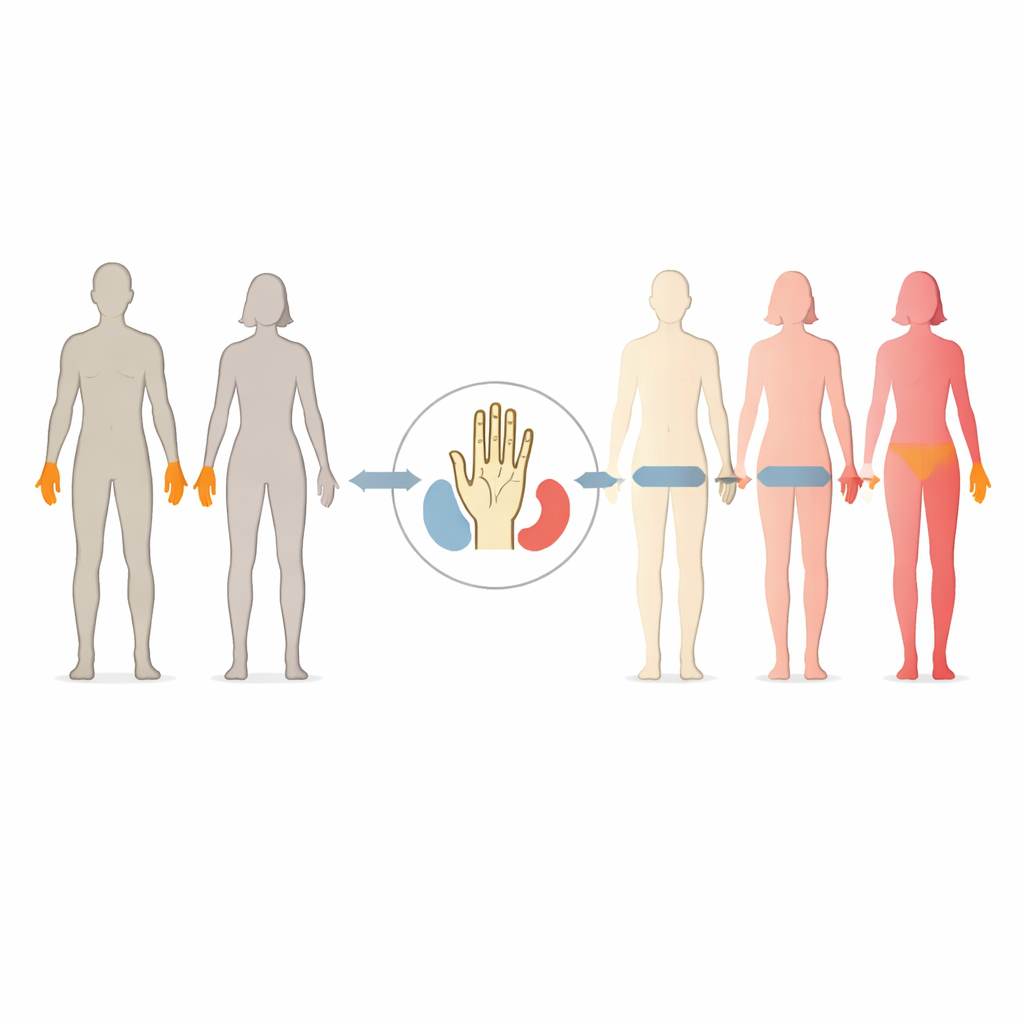
Measuring tiny changes on the skin
The researchers used a device that gently warmed or cooled a small metal plate resting on the palm. Starting from a neutral skin temperature, the plate slowly became cooler or warmer. Participants pressed a button the moment they sensed a change. The smaller the temperature shift needed, the more sensitive that person’s skin was to temperature. Separate tests quickly pushed the temperature to more extreme levels to find when warmth or cold started to hurt.
What differed at the start
Before any hormone therapy, the study confirmed earlier findings: people assigned female at birth—transgender men before treatment plus cisgender women—noticed both cooling and warming at smaller changes than people assigned male at birth—transgender women before treatment plus cisgender men. Importantly, these differences could not be explained by age, body size, body fat, or season. Yet the temperatures at which heat or cold became painful did not differ clearly between the two groups, suggesting that hormones and sex-related factors affect subtle temperature sensing more than pain from extreme temperatures. 
How hormone therapy changed temperature sensing
Over six months of estrogen plus a testosterone blocker, transgender women became more sensitive to temperature changes: they detected smaller shifts in both cooling and warming on the palm. This pattern moved their sensitivity closer to that typically seen in cisgender women. By contrast, transgender men receiving testosterone did not show clear changes in how they sensed temperature during the first six months, and neither cisgender men nor cisgender women changed over time. Pain thresholds for extreme heat and cold, and self-reported everyday feelings of being hot or cold, also stayed largely stable across all groups.
What this may mean for the body
The findings suggest that sex hormones help tune the body’s temperature sensors in the skin. Animal work points to possible roles for specific temperature-sensing proteins and hormone-sensitive brain circuits, but this human study cannot yet pinpoint where in the nervous system the change occurs. It also raises questions about whether skin structure, which softens and thins under estrogen therapy, contributes to increased sensitivity. Because the study followed a modest number of people for only six months, it remains unclear how large or long-lasting these changes will be.
Why these results matter to everyday life
In plain terms, when people with typically male hormone levels start estrogen-based gender-affirming therapy, their skin begins to notice smaller changes in temperature, more like that of people with typically female hormone levels. This shift did not make hot or cold more painful, nor did it dramatically change how people described their comfort in daily life—at least within the first half-year. The work offers an important step toward understanding how hormones shape basic body functions such as sensing warmth and cold, with implications not only for transgender health care but also for how all of us may cope with a warming and increasingly variable climate.
Citation: Zimmermann, P., Kaar, M., Bokeloh, T. et al. Changes in temperature perception in transgender persons undergoing gender-affirming hormone therapy. Commun Med 6, 146 (2026). https://doi.org/10.1038/s43856-026-01420-0
Keywords: temperature perception, gender-affirming hormone therapy, transgender health, sex hormones, thermal sensitivity