Clear Sky Science · en
Machine learning to infer neurocognitive testing scores among adolescents and young adults with congenital heart disease
Why this matters for growing up with a heart condition
More children born with serious heart defects are now living into adulthood than ever before. But many families discover that surviving heart surgery is only part of the story: some teens and young adults struggle with attention, learning, or memory. This study asks a practical question with big implications: can we use brain scans, genetic information, medical history, and family background together to estimate how a young person with congenital heart disease is doing in school-like thinking and problem solving, without having to rely on lengthy testing alone?
Looking at the whole picture, not just the heart
The researchers followed 89 adolescents and young adults with congenital heart disease, ages 8 to 30, from centers across the United States. Each participant completed standard paper-and-pencil tests that measured reading, vocabulary, problem solving, memory, processing speed, and overall IQ. Within about six months—often within just a couple of days—they also had detailed MRI scans of the brain and provided genetic samples. The team collected information about their heart diagnoses and surgeries, height and weight, and family socioeconomic background, including parents’ education and household income. The goal was to treat each young person not as “a heart case” but as a whole person whose brain, genes, health history, and environment all shape how they think and learn.
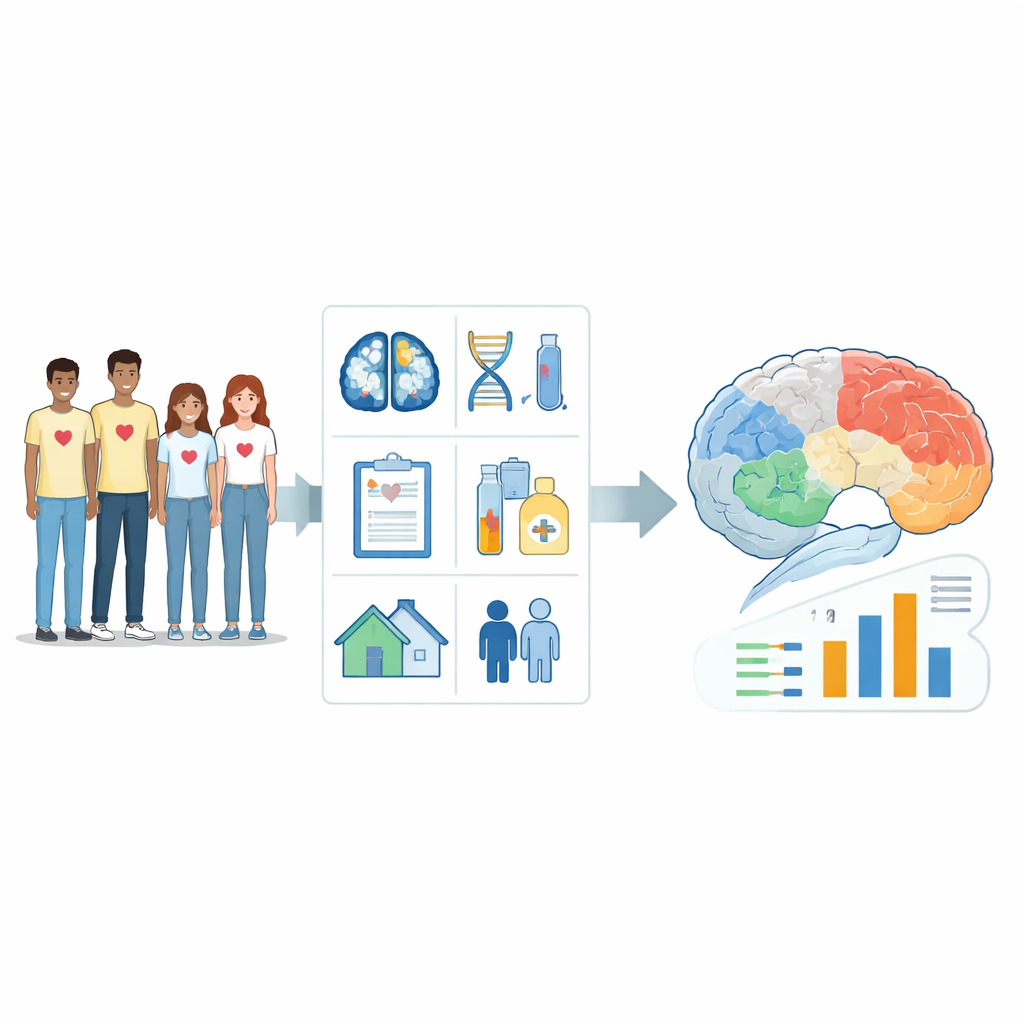
Teaching computers to estimate thinking skills
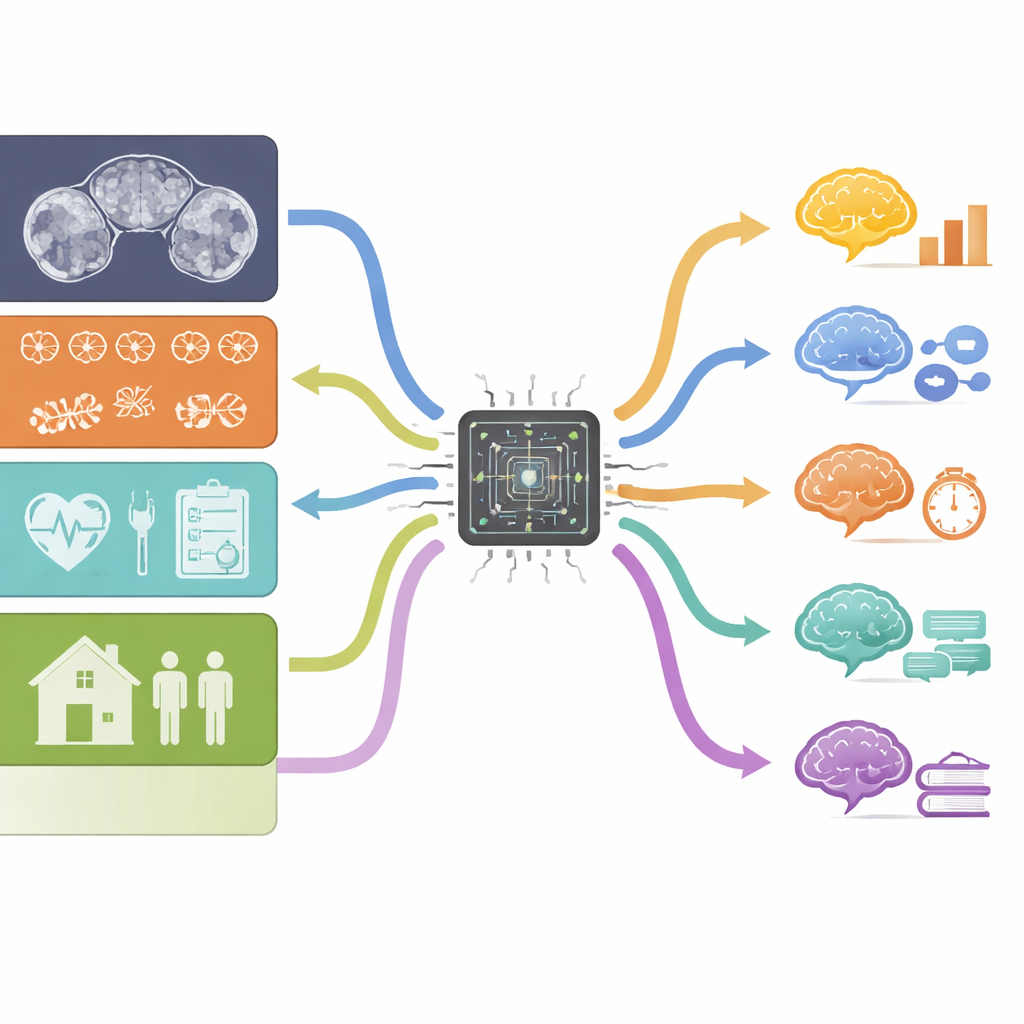
To make sense of this complex mix of information, the scientists used machine learning—computer methods that can find patterns in large sets of data. They fed in thousands of measurements from structural and diffusion MRI scans (which capture brain size, shape, and wiring), along with 17 non-imaging factors such as sex, number of heart surgeries, types of rare genetic variants, and parents’ education. For each of 15 different test scores across seven broad areas of thinking, they trained models to infer the score from these features. An advanced feature-selection method repeatedly added and removed candidate variables, keeping only those combinations that actually improved performance when tested on held-out participants. The team judged success by how closely the inferred scores matched real test scores and how large the typical error was in test-score points.
What the models could and could not see
The computer models were able to estimate most test scores better than chance, with correlations between actual and inferred scores ranging from modest to fairly strong. Full-scale IQ, working memory (remembering sequences of numbers), and processing speed (quick visual scanning and symbol matching) were among the easiest to infer. For example, the model’s estimates of digit span, a common memory test, tracked actual performance quite closely. In contrast, more specific skills like understanding sentences or solving block design puzzles were harder to predict. When the researchers combined results across tests, general intelligence came out as the most “inferable” ability, while perceptual reasoning—figuring out patterns in shapes and spaces—was the least.
How brain, genes, and environment each play a role
By examining which features the models relied on, the study paints a nuanced picture of what shapes cognition in this group. Brain measures from MRI appeared across all seven cognitive domains. Regions in the frontal and temporal lobes, and the white-matter highways connecting them, were especially important—areas long linked to language, memory, and problem solving. But non-brain factors also mattered. A father’s education level helped infer overall IQ and visual–spatial skills, hinting at the impact of home environment and learning opportunities. Features of heart disease itself, such as diagnosis type and number of surgeries, influenced verbal abilities. Certain rare genetic variants, particularly those that disrupt neurodevelopmental genes, tended to be associated with weaker reading, math, or vocabulary. Rather than a single cause, the picture that emerges is one of overlapping influences, where brain structure, medical history, genes, and socioeconomic context all nudge cognitive outcomes in different directions.
What this could mean for care and follow-up
For families and clinicians, the message is both reassuring and forward-looking. In this relatively small but carefully studied group, many young people with congenital heart disease had thinking skills in the average range. Yet the study shows that subtle differences in cognition can be meaningfully estimated from information already gathered in modern care, especially detailed brain scans. If confirmed in larger and more diverse groups, similar models could one day help doctors flag which children are at higher risk for school or memory difficulties, even before problems fully emerge. That, in turn, could guide earlier referrals for educational support, cognitive training, or family-based interventions—making brain health as central to follow-up as heart health itself.
Citation: Hussain, M.A., He, S., Adams, H.R. et al. Machine learning to infer neurocognitive testing scores among adolescents and young adults with congenital heart disease. Commun Med 6, 144 (2026). https://doi.org/10.1038/s43856-026-01417-9
Keywords: congenital heart disease, adolescent cognition, brain MRI, machine learning, neurodevelopment