Clear Sky Science · en
Ischemic brain infarcts, white matter hyperintensities, and cognitive impairment are increased in patients with Atrial Fibrillation
When an Irregular Heartbeat Reaches the Brain
Atrial fibrillation—a common irregular heartbeat—often sounds like a problem confined to the chest. But this large Swiss study shows that it reaches far beyond the heart. Older adults with atrial fibrillation not only had more signs of damage on brain scans, they also performed worse on tests of memory and thinking than similar people without the arrhythmia. Surprisingly, most of this dip in brain function could not be explained by visible damage on MRI scans, suggesting that the abnormal rhythm itself may directly affect how the brain works.
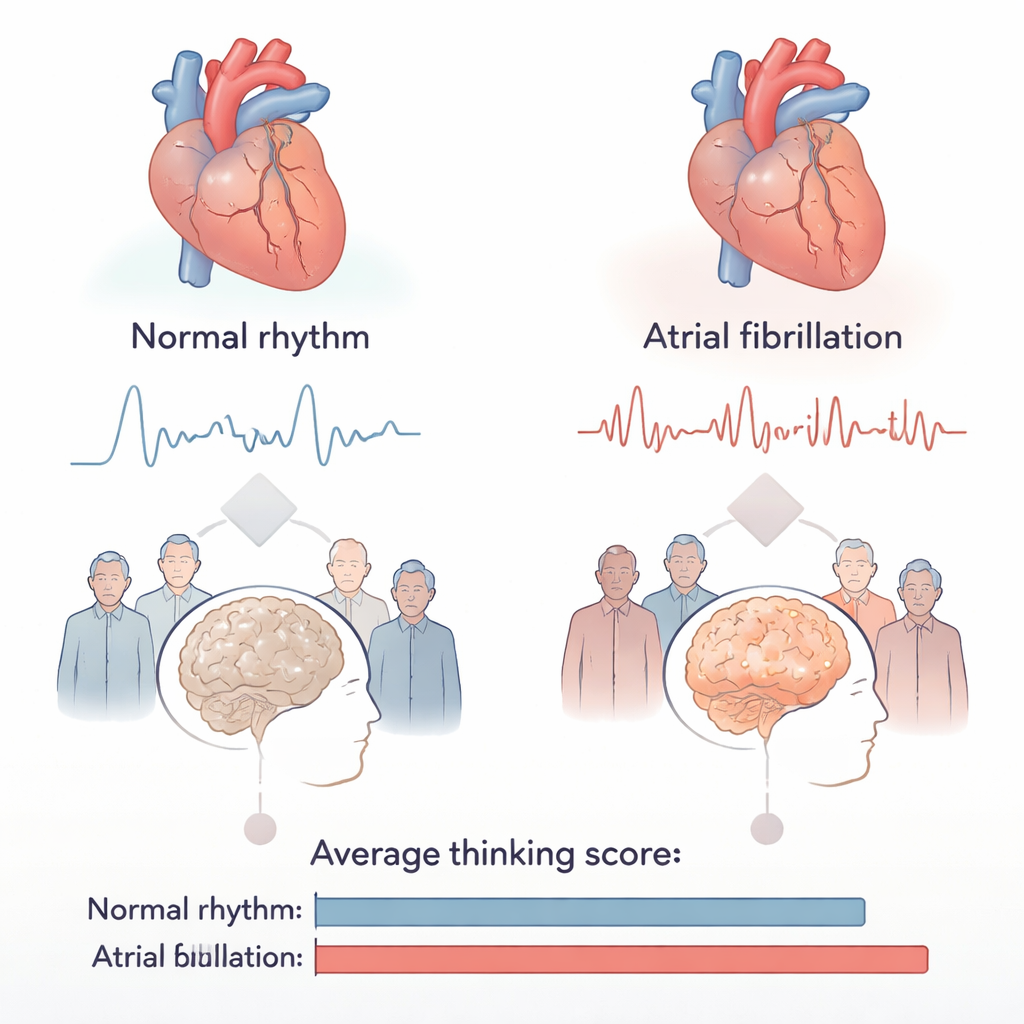
Who Was Studied and What Was Measured
Researchers followed more than 2,400 older adults in Switzerland, all at least 65 years old. About 1,480 had atrial fibrillation, and 959 had never been diagnosed with the condition and showed a normal rhythm on heart tests. The two groups were carefully matched in age and in common health problems such as high blood pressure, diabetes, and vascular disease. Everyone underwent detailed brain MRI scans and completed the Montreal Cognitive Assessment, a widely used 30‑point test of attention, memory, language, and problem solving. This setup allowed the team to separate the effects of atrial fibrillation from those of other shared risk factors.
Brain Scans Reveal Hidden Damage
The brain images told a clear story. Four in ten people with atrial fibrillation showed signs of ischemic brain infarcts—areas of tissue that had been starved of blood—compared with about one in four people without the arrhythmia. They also had more frequent patches of white matter hyperintensities, a type of scarring in the brain’s wiring that is commonly linked to small vessel disease and aging. These changes appeared even though most patients with atrial fibrillation were taking blood thinners to prevent clots. In contrast, tiny brain bleeds, called microbleeds, were not more common in the atrial fibrillation group, suggesting that the main added burden came from lack of blood flow rather than bleeding.
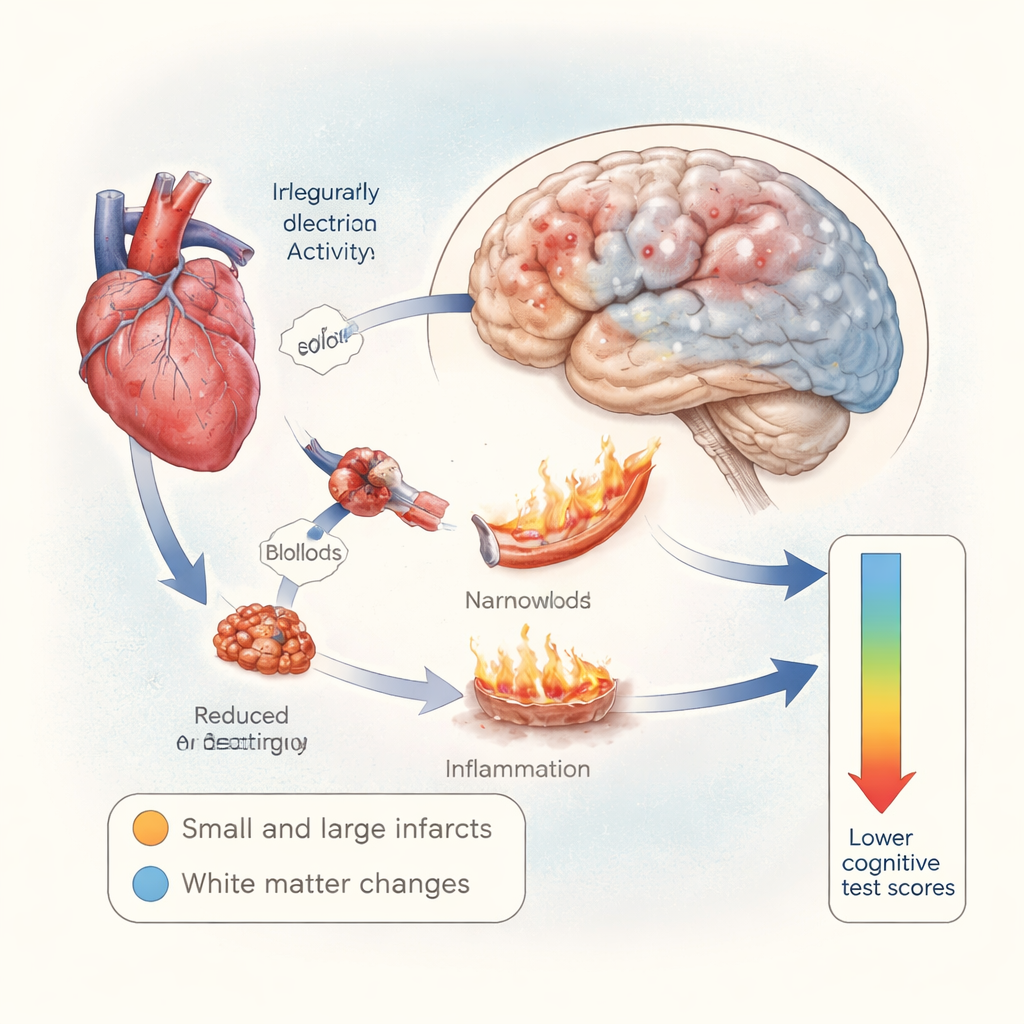
Thinking Skills and the Hidden Cost of AF
On the thinking test, people with atrial fibrillation scored on average about one point lower than their counterparts without the condition (25.3 versus 26.4 out of 30). While this may seem small, it is roughly similar to the gap typically seen between people almost a decade apart in age. Importantly, this difference showed up across age groups and remained even after adjusting for education, blood pressure, diabetes, and use of blood thinners. When the researchers looked only at participants whose brain scans showed no detectable lesions, those with atrial fibrillation still tended to score lower, hinting that something more than visible brain damage was at work.
Looking for the Path from Heart Rhythm to Mind
To probe this puzzle, the team used a statistical approach called mediation analysis. They asked how much of the link between atrial fibrillation and lower cognitive scores could be explained by the brain lesions seen on MRI. The answer was: very little. Overall, atrial fibrillation was associated with just over one point lower on the cognitive test. Of that, only a tiny fraction—at most about 0.06 points—could be traced to infarcts or white matter changes. The vast majority of the effect appeared to be direct, not channeled through these visible brain injuries. This suggests that irregular heart rhythm may harm thinking through other routes, such as unstable blood flow to the brain, inflammation, or disturbed waste‑clearing systems in brain tissue.
What This Means for Patients and Care
For patients, families, and clinicians, these findings underscore that atrial fibrillation is not just about preventing strokes. Even when major strokes are avoided and routine scans show only subtle changes, the condition still seems to be linked to slower or less efficient thinking. Protecting brain health in atrial fibrillation may therefore require more than standard blood‑thinning drugs. Future research will need to test whether better rhythm control, more stable blood pressure, or treatments targeting inflammation and brain circulation can help preserve memory and cognitive function in this growing patient population.
Citation: Krisai, P., Aeschbacher, S., Coslovsky, M. et al. Ischemic brain infarcts, white matter hyperintensities, and cognitive impairment are increased in patients with Atrial Fibrillation. Commun Med 6, 120 (2026). https://doi.org/10.1038/s43856-026-01389-w
Keywords: atrial fibrillation, brain infarcts, white matter changes, cognitive decline, elderly patients