Clear Sky Science · en
Comprehensive characterization of nonlinear viscoelastic properties of arterial tissues using guided-wave optical coherence elastography
Why the stretchiness of arteries matters
Every heartbeat sends a pressure wave racing through your arteries, and the way those vessel walls stretch, rebound, and dissipate energy helps keep blood flowing smoothly. Subtle changes in this mechanical behavior are linked to high blood pressure, aneurysms, and other cardiovascular diseases. Yet most current medical tests see only a crude, average stiffness of the vessel, not how different layers of the wall behave or how their properties change with the rhythm of each beat. This study introduces an optical technique that can “listen” to tiny waves in the artery wall and use them to build a detailed mechanical profile of the vessel, layer by layer.
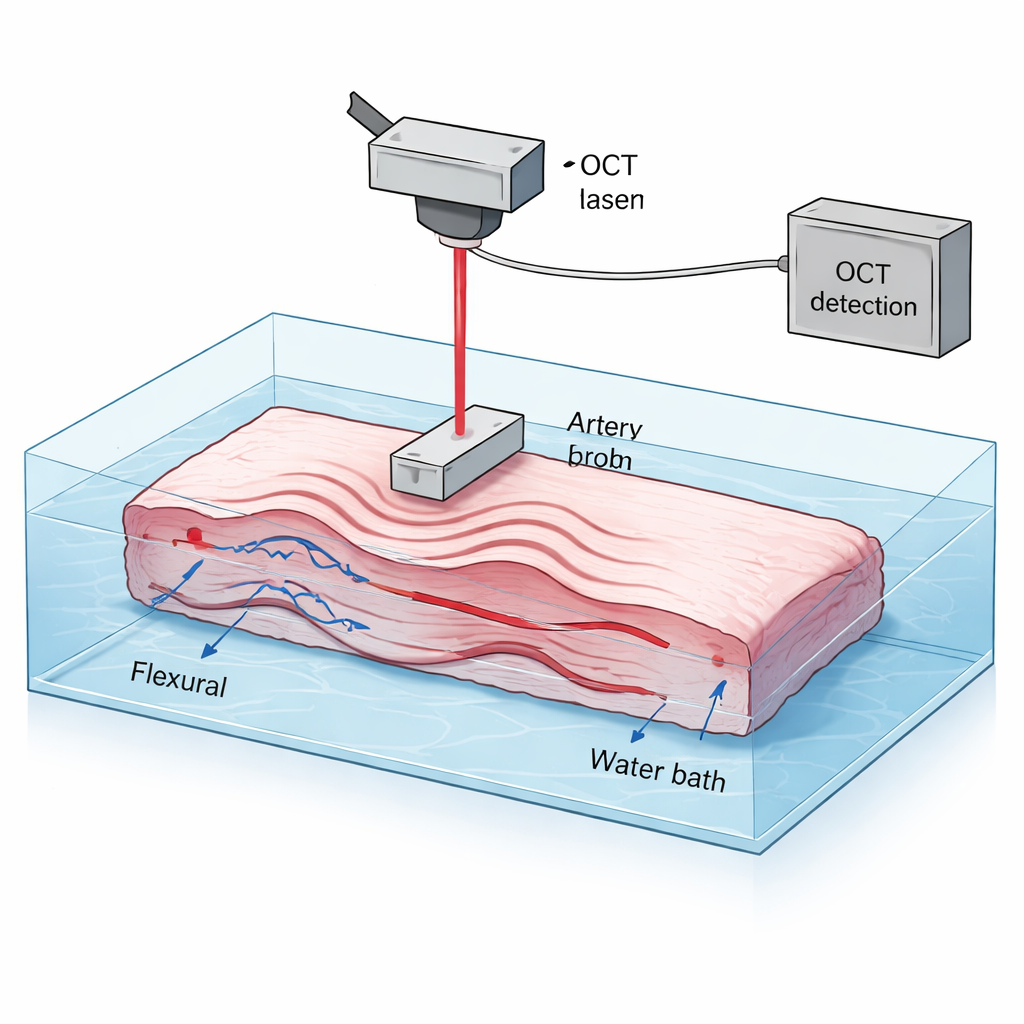
Listening to tiny waves in artery walls
The researchers used a method called optical coherence elastography, a cousin of high-resolution optical imaging. They took sections of pig aorta, gently stretched them in two directions, and used a small vibrating probe to launch microscopic ripples along the flattened artery wall. A scanning light beam measured how the surface moved in response. These guided waves travel in two main patterns: one dominated by bending motion, and another dominated by in-plane stretching. Because the waves move faster in stiffer material and their speed changes with frequency, analyzing these motions across a wide range of frequencies reveals how the tissue resists both shear (sliding) and stretch, much like tapping a drum skin at different pitches to infer its tension and structure.
Peeling apart layers and directions
Artery walls are not uniform: the inner media layer is rich in elastic fibers, while the outer adventitia is packed with wavy collagen fibers that straighten and bear load as the vessel stretches. Using mathematical models of wave propagation in layered materials, the team separated the mechanical contributions of these two layers and of two directions in the wall: around the vessel (circumferential) and along its length (axial). They found that both shear and tensile stiffness increase as the artery is stretched, and that the vessel is consistently stiffer around its circumference than along its length. At low stretch, the media is slightly stiffer, but as tension rises to levels similar to those in a beating heart, the adventitia rapidly becomes much stiffer than the media, highlighting how collagen fibers take over load-bearing under physiological pressure.
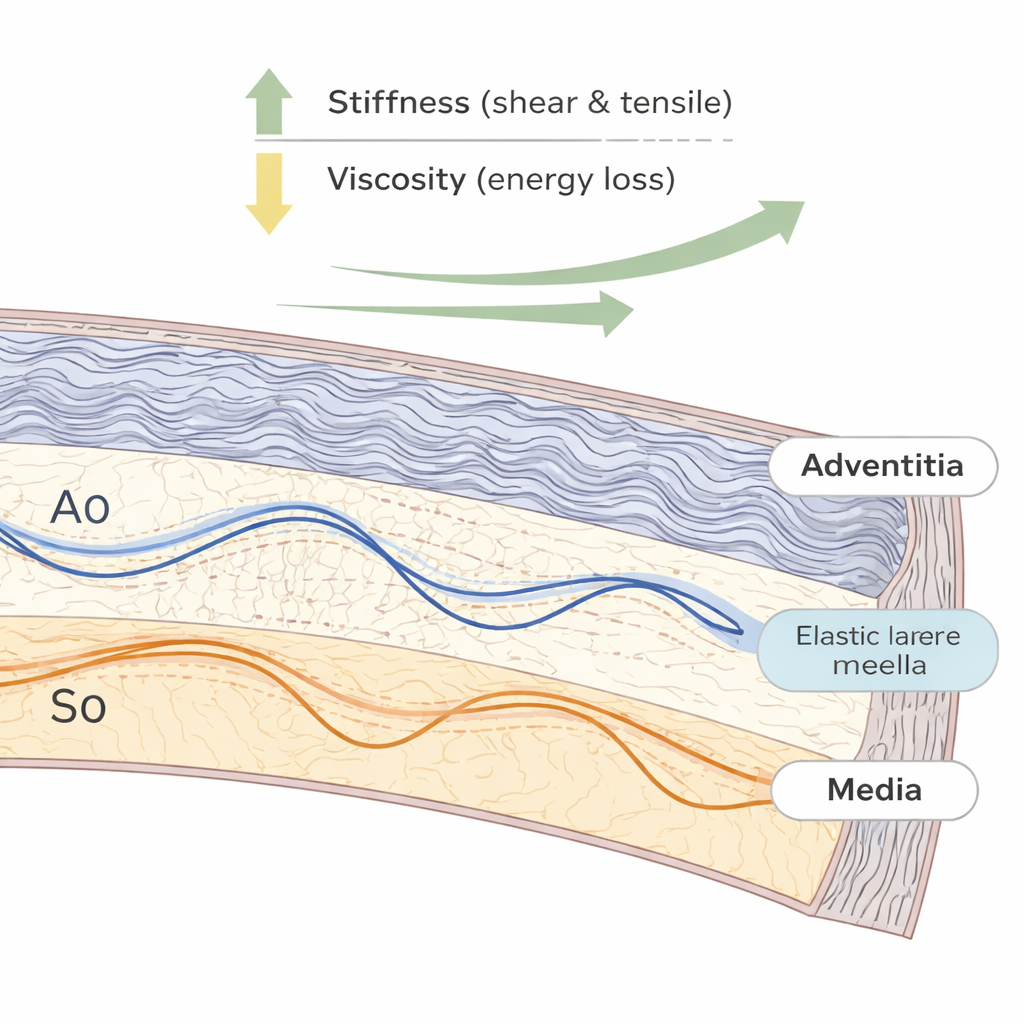
From springiness to energy loss
Real tissues are not just springy; they are also viscoelastic, meaning they temporarily store and dissipate energy with each cycle of loading. To capture this behavior, the authors used a fractional viscoelastic model that treats the wall as a combination of an elastic spring and a “spring-pot” element that captures sluggish, power-law-like response. Fitting this model to the measured wave speeds, they showed that as the artery is stretched, its effective viscosity and energy loss drop, while its elastic stiffness grows. In other words, a prestretched artery wall behaves more like an efficient spring and less like a damped shock absorber. Measurements of how quickly the waves fade as they travel confirmed this picture: higher stretch produced less attenuation, consistent with lower viscous losses.
What happens when collagen is removed
To probe which microscopic components generate these properties, the team chemically treated some artery samples to selectively degrade collagen while leaving the elastin network mostly intact. After treatment, the walls became thinner and much softer in both shear and stretch, confirming the key role of collagen in making arteries strong at higher strain. However, the viscous part of the response changed far less than the elastic stiffness. This suggests that at modest stretch levels, collagen is crucial for overall strength but is not the main source of viscoelastic damping; elastin and fluid-filled microstructures in the wall likely play outsized roles in how arteries dissipate energy over each heartbeat.
Why this matters for heart and vessel health
By combining ultrafine optical measurements with advanced wave and material models, this work delivers a rich, layer-by-layer map of how artery walls stiffen and lose viscosity as they are stretched. For a layperson, the takeaway is that healthy arteries behave like smart, multi-layer springs: collagen and elastin fibers share the load in a way that keeps the wall strong yet energy-efficient over many billions of heartbeats. The new optical method could eventually help doctors assess subtle changes in this balance—such as early stiffening of the outer layer or abnormal energy loss—before they become visible as full-blown vascular disease, opening doors to earlier diagnosis and more precisely targeted treatments.
Citation: Jiang, Y., Li, GY., Wang, R. et al. Comprehensive characterization of nonlinear viscoelastic properties of arterial tissues using guided-wave optical coherence elastography. Commun Phys 9, 66 (2026). https://doi.org/10.1038/s42005-026-02502-0
Keywords: arterial biomechanics, optical coherence elastography, vascular stiffness, viscoelastic tissue, collagen and elastin