Clear Sky Science · en
Microglia cause HIV-induced transcriptional and metabolic changes in human neural organoids
Why brain changes in HIV still matter
Modern HIV medicines let many people live long, healthy lives, yet up to half still experience subtle problems with memory, attention, or mood. This study asks a pressing question: what is happening inside the brain, even when the virus is controlled, that might quietly harm nerve cells over time? Using tiny lab-grown "mini-brains" that mimic human brain tissue, the researchers zoom in on how HIV and the brain’s immune cells interact to disturb both inflammation and cellular energy use in ways that could underlie these lingering issues. 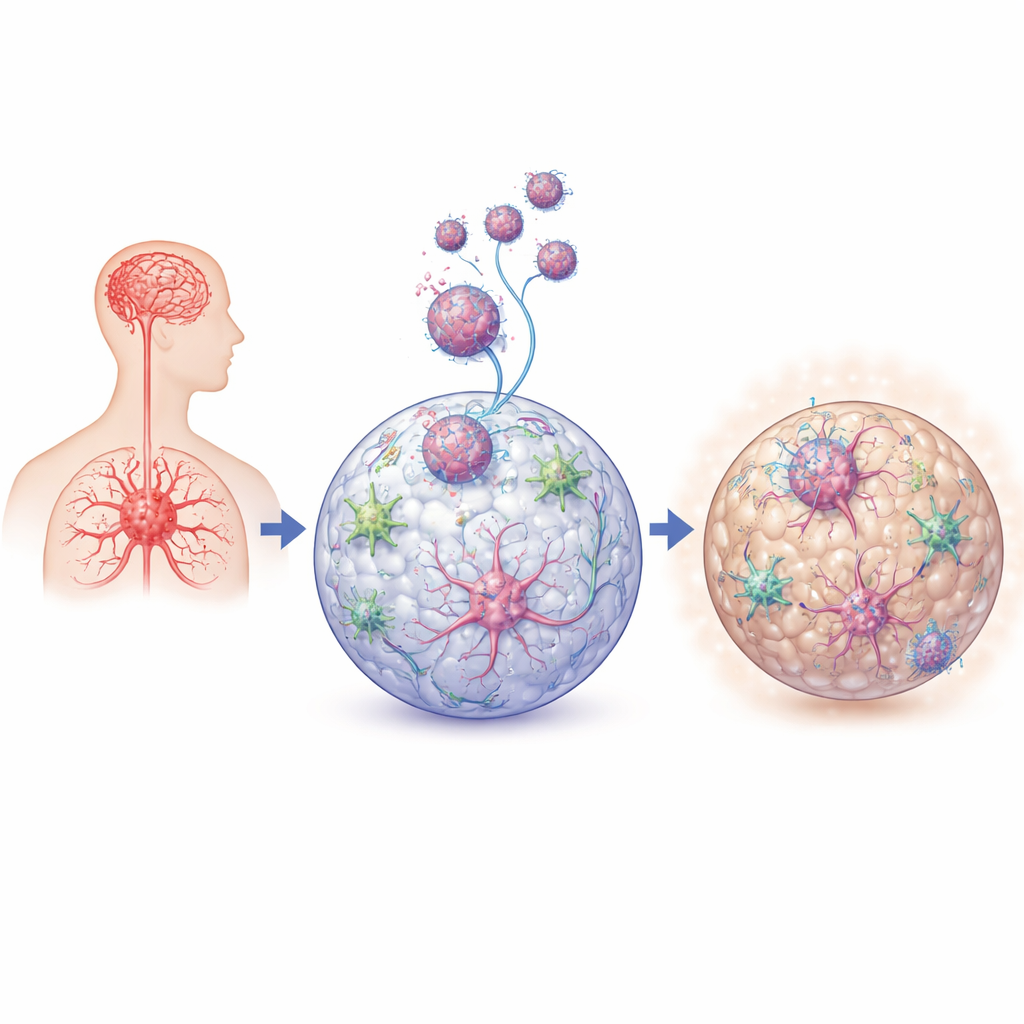
Mini-brains and the brain’s watchful sentinels
Instead of studying full human brains—which is rarely possible in living people—the team used three-dimensional neural organoids: pea-sized balls of human nerve tissue grown from stem cells. Into these organoids they added microglia, the brain’s resident immune sentinels, which patrol for threats and help maintain healthy connections between neurons. They then infected microglia with an HIV strain known to target brain cells and allowed these infected microglia to embed within the organoids. This setup created a controllable, human-based model of early HIV invasion into the brain’s environment, letting the scientists compare organoids with and without microglia, and with active or inactive virus.
Where the virus hides and who it touches
Microscope imaging and viral measurements showed that the virus replicated strongly inside microglia and that viral proteins spread to neighboring cells. Late-stage viral proteins were found not only in microglia but also in star-shaped support cells called astrocytes, while neurons themselves did not show clear signs of direct infection. Nonetheless, viral regulatory proteins appeared close to neurons, hinting that HIV can influence their behavior indirectly. Organoids that contained microglia had much higher levels of viral genetic material than those without, underscoring microglia’s role as a long-lived reservoir and amplifier of HIV within the brain.
Immune alarms and a new doorway for HIV
When the researchers examined which genes were turned on or off, they found that HIV triggered far more widespread changes when microglia were present. Hundreds of genes linked to inflammation and antiviral defense surged in activity, including pathways that control signaling molecules and the body’s interferon response. A notable finding was the strong increase in a receptor named CCR6, which can act as a secondary entry point for HIV and also shapes immune cell movement. Markers of astrocyte activation, often seen in brain inflammation, were elevated as well, while certain chemical messengers, such as the chemokine CCL13, rose in the surrounding fluid. Together, these shifts paint a picture of a brain tissue environment that becomes highly reactive and inflammatory once HIV-infected microglia are on the scene.
Fuel mix shifts inside stressed brain cells
Beyond gene activity, the team explored how HIV alters the chemistry of cell metabolism—the way cells handle their fuel and building blocks. Using computer models built from the gene data, they mapped which metabolic reactions sped up or slowed down in infected organoids. They discovered a distinctive "rewiring" of amino acid use and transport, especially for molecules like arginine, proline, tryptophan, and the energy-related compound alpha-ketoglutarate. Transport proteins that shuttle these substances between cellular compartments were more active in infected, microglia-containing organoids. The models suggested that cells were exporting some amino acids, redirecting others into alternative energy routes, and pushing more intermediates into mitochondria, as if the tissue were under metabolic stress and scrambling to meet high energy demands. Such changes can raise glutamate levels and disturb tryptophan breakdown—both linked to oxidative stress, disrupted communication between neurons, and mood and cognitive problems. 
What this means for people living with HIV
Overall, the study shows that HIV-infected microglia can reshape both immune signaling and energy handling in nearby brain cells, even in the absence of direct infection of neurons. This microglia-driven "immunometabolic" imbalance likely weakens the support system that neurons rely on, fostering chronic inflammation and subtle but progressive brain dysfunction. By pinpointing early molecular and metabolic changes—such as CCR6 upregulation and specific amino acid shifts—these organoid models may help identify future biomarkers to flag people at higher risk of HIV-related cognitive problems and guide therapies that protect not just against viral replication but also against the silent metabolic strain on the brain.
Citation: Capendale, P.E., Helgers, L.C., Ambikan, A.T. et al. Microglia cause HIV-induced transcriptional and metabolic changes in human neural organoids. Commun Biol 9, 436 (2026). https://doi.org/10.1038/s42003-026-09864-9
Keywords: HIV and the brain, neurocognitive disorders, microglia, brain organoids, brain metabolism